
Simon Turner / Alamy Stock Photo
Mention the term ‘winter pressure’ to anyone who works for the NHS and you will get the inevitable response that the pressure is all year round. But it cannot be ignored that demand rises in the colder months and winter 2018/2019 looks set to be a particularly difficult one.
There has already been a 6% increase in emergency hospital admissions during October 2018 compared with the same month in 2017, and an even bigger increase in the number of patients waiting over four hours before admission (7%). Both figures are at the highest level since data collection began in October 2013 (see Figure). And, with all parts of primary and secondary care struggling under the strain, pharmacy is being hailed as part of the solution to take the pressure off hospital services and improve patient flow.
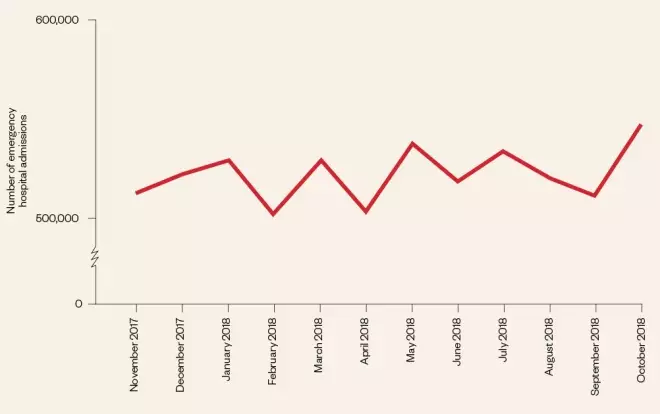
Figure: How pressure on the NHS is rising
Source: NHS Performance Statistics. NHS England, 8 November 2018. Available at: https://www.england.nhs.uk/statistics/wp-content/uploads/sites/2/2018/11/Combined-Performance-Summary-November-September-October-data-2018v2.pdf (accessed December 2018)
On 31 October 2018, NHS England published guidance on steps that hospitals should take to use pharmacists in helping to tackle winter pressures (see Box). Its recommendations included putting pharmacy professionals on hospital wards to manage medicines and help discharge patients; placing pharmacists in emergency departments to prescribe medicines before patients even reach the wards; and extending the working hours of pharmacy services so they are available to support hospital teams.
Box: How pharmacists could be used in hospitals
- Maximise whole pharmacy team to operate as a team across multiple wards, meeting in ‘daily huddles’ to identify priority areas for their input and attending board rounds on wards to identify patients prioritised for discharge;
- Place pharmacist prescribers in emergency departments to optimise the use of medicines on admission to acute care and ensure no delay in prescribing regular medicines before admission to a ward;
- Use pharmacists in the emergency department to support medicine reconciliation pre-discharge for acutely ill patients;
- Extend pharmacy service availability and consider support for discharge teams at weekends;
- Implement medicines housekeepers or volunteers to move medicines with the patient and consider satellite dispensaries and/or mobile dispensing units;
- Increase ready-prepared intravenous doses prepared in pharmacy.
Source: NHS England and NHS Improvement. Pharmacy and Medicines Optimisation: A Toolkit for Winter, October 2018
The control centre at Luton and Dunstable University Hospital in Bedfordshire shows patient flow in real-time detail and is often heralded as the gold standard of bed management. To carefully monitor what is happening in the hospital, a series of electronic systems are used to keep an eye on patient flow and pinpoint potential blockages in real time.
An important aspect of this system is that pharmacists are heavily involved at every stage and are able to ramp up their work at busy times.
The pharmacy prescription tracker is part of the ‘control centre’ suite of tools and once the trust hits a specific level of pressure, a member of the senior pharmacy team attends the bed meetings that are held four times per day. They can then feed down — on an individual patient-level basis if needed — what pharmacists can do to free up capacity. It is a carefully managed system that allows the pharmacy team to be actively aware throughout the day of wider hospital pressures and able to meet anticipated changes in demand.
Over the past few years, Luton and Dunstable University Hospital has finessed the system, adding extra prescribing pharmacists to the team who can prescribe electronically during a ward round; make better use of local dispensing satellites; and put a 7-day, 12-hour service in place. Of course, this system is not a tool for winter use only but it comes into its own when the hospital is at full capacity, prompting staff to implement extra measures to ensure discharges happen when they should.
Mary Evans, chief pharmacist at Luton and Dunstable University Hospital NHS Trust, says the control is “heightened” when they get into peak pressure time, with senior pharmacy staff attending all bed management meetings and taking an active part in decisions on how to keep things moving. “When it gets really pressured and the discharges don’t match up with potential attendances in the emergency department, we feed back to pharmacy teams in a much more detailed way about what is required.”
We should be doing these things all year round; winter is just a time to try to maximise the activities which add the greatest value at times of system pressure
A vital part of this process is arranging discharges as early as possible during the day and being aware of any additional possible complications with each discharge so hospital staff can keep on top of it. “We have evolved the system over the past four years. Every year we have slightly more prescribing pharmacists [in the hospital], and having a prescribing pharmacist [as part of] the ward round is relatively new,” Evans adds.
Sarah Lock, a pharmacist at Chesterfield Royal Hospital in Derbyshire, works year-round in the emergency department, but she is in no doubt that winter is the busiest time: “I focus on patients who look like they’re going to be admitted and complete their medicines reconciliation and I’m an independent prescriber so I can prescribe their regular medication,” she explains. “It can be very different in winter when you can have patients lined up in the corridors because there [are] no beds.”
Where possible, Lock also tries to see those patients who are not admitted but may require her input. After a fall, for example, a patient may require a review of their medicines to ensure it does not happen again.

Source: Courtesy of David Campbell
David Campbell, chief pharmacist at Northumbria Healthcare NHS Foundation Trust, says effectively managing patient flow is essential to coping with winter pressures
Keeping patients moving
David Campbell, chief pharmacist at Northumbria Healthcare NHS Foundation Trust, which runs a number of hospitals around Newcastle, says one of the essential aspects to coping with winter is safely and effectively managing patient flow. “In my view, we should be doing these things all year round; winter is just a time to try and maximise the activities which add the greatest value at times of system pressure.”
These measures include an integrated primary and secondary care pharmacy team that speeds up discharge, as well as helping to prevent admissions. Campbell adds that the trust’s model of extensive use of over-labelled drugs prevents discharge delays resulting from patients waiting for medicines.
“More than 70% of patients at Northumbria Specialist Emergency Care Hospital can be discharged at the time a decision is made, because the medicines are already in the patient’s bedside or available as over-labelled ward stock,” Campbell says.
He adds that the trust is continuing to find ways to take dispensing activities away from hospital pharmacies at times of ‘surge’ so the focus can be on inpatient and discharge medicines: “We are also exploring the use of electronic systems which would enable discharge prescriptions to be sent to usual community pharmacist for dispensing, which would also speed up discharge and support flow.”
During winter 2017/2018, the Northumbria Healthcare NHS Foundation Trust also provided clinical pharmacist support to the emergency department of Northumbria Specialist Emergency Care Hospital. More recently it employed a pharmacist who works as part of the NHS England-funded regional integrated urgent care network — a scheme designed to overcome fragmentation of out-of-hospital services and treat people closer to home — who works part time for NHS 111 and part time in the emergency department/urgent care.
Campbell explains that pharmacists also routinely support discharge by taking part in ward rounds when the system is under stress, and this kind of work is prioritised over other parts of the job.
Volunteer scheme
In Wye Valley, on the border of England and Wales, an award-winning scheme called Pharmacy Volunteers makes use of volunteers to support pharmacy teams with the delivery of 18,000 urgent medicines over 18 months to wards and departments in the County Hospital. Tony McConkey, clinical director of pharmacy and medicines optimisation at Wye Valley NHS Trust, says the volunteers are all trained in their delivery role and the safe handling of medicines, and security checked. Analysis of the service has shown that the average delivery time for urgent medicines is 5.4 minutes, while 35 hours have been saved per week. The majority of urgent medicine deliveries carried out by the volunteers are related to cancer services (40%), day-case surgery (10%) and the discharge lounge (8%).
We have been fortunate to secure a room in the new acute medical unit called the ‘Pharmacy hub’ and we will be running our pharmacy support from that from 21 December 2018
McConkey says: “We have been fortunate to secure a room in the new acute medical unit (AMU) called the ‘Pharmacy hub’ and we will be running our pharmacy support from that localised hub from 21 December 2018.”
He adds that there is currently a pharmacist, pharmacy technician and pharmacy assistant supporting the AMU and they are trialling pharmacy technician support in the emergency department. “We are developing a case for further pharmacist support into the emergency department off the back of this work. But it is early days.”
Primary care and community pharmacy
While hospital pharmacy teams across the UK are ramping up their efforts and trialling new systems to involve pharmacy in getting patients through hospital, or avoiding hospital admission altogether, the picture is less clear when it comes to primary care and community pharmacy.
While minor ailment schemes are being extended in Scotland and Northern Ireland, they are steadily being decommissioned across England, putting even more pressure on other NHS services during extraordinarily busy winter months.
In contrast, a winter minor ailments scheme was commissioned by NHS England in the Western Devon area for two winters — 2014/2015 and 2015/2016. Across Devon, a Pharmacy First minor ailments scheme that runs year-round still operates. It offers treatment for a number of conditions including urinary tract infections for women aged 16–65 years; impetigo; bacterial conjunctivitis in children aged 1–2 years; and infected nappy rash.

Source: Courtesy of Mark Stone
Mark Stone, project lead at Devon local pharmaceutical committee, is looking to expand a winter minor ailments scheme
Mark Stone, project lead at Devon local pharmaceutical committee (LPC), says he is looking to expand this service to cover winter ailments in time for the winter of 2018/2019.
In October 2018, Devon LPC introduced a service in collaboration with NHS Northern, Eastern and Western Devon Clinical Commissioning Group that uses funding from the Improving Access to General Practice programme — which extends evening and weekend opening hours in primary care — that encourages patients booking appointments with their pharmacist, rather than using an out-of-hours GP slot. First set up in October 2018, it is now being rolled out to Plymouth in time for winter demand.
Reducing GP pressures
In addition, the Digital Minor Illness Referral Service pilot, which aims to integrate community pharmacy into NHS 111 referral pathways for people suffering from minor conditions, has just been rolled out across more locations to help reduce pressure on other urgent care services as we head into winter.
Sanjay Ganvir, chair of Camden and Islington Local Pharmaceutical Committee, has been involved in getting it off the ground and is thrilled that 1,290 of 1,800 community pharmacies in London have signed up to the pilot, which is running from October 2018 to March 2019.
From a patient point of view, community pharmacy is the biggest walk-in centre in the entire NHS estate
Ganvir believes there are huge numbers of emergency department attendances and GP appointments that can be avoided by better use of pharmacy — and this is one really good way to join all those systems up. “The size of the prize [for the NHS] is massive here and, from a patient point of view, community pharmacy is the biggest walk-in centre in the entire NHS estate.”
He adds that the difference here is that rather than being just told to go to a pharmacy, the patient chooses one nearby that is taking part in the scheme, and their chosen pharmacy is sent details from the NHS 111 call so the patient does not have to go through it all again. Should it need escalating, the pharmacist is able to get direct access to out-of-hours services, the patient’s GP or an ambulance.
LloydsPharmacy also announced in November 2018 that it is offering a sore throat test-and-treat service in 600 of its stores with swabs to identify streptococcal infections to take pressure off GPs. LloydsPharmacy claimed that more than a third of people with a sore throat visit their GP when they would be much better placed seeking pharmacy advice. This follows an announcement in November 2018 from NHS Wales that it was launching an on-the-spot sore throat swab service in 48 community pharmacies to encourage patients to visit their pharmacist first for minor ailments.
The harshness of the forthcoming winter is obviously unknown, but there is consensus among health professionals that whatever the weather, this season will be one of the most testing ever for the health service. But pharmacists have shown what they can do to ease seasonal pressures, and the NHS is recognising this and encouraging the pharmacy profession to do more. This winter is likely to see pharmacists increase their role even further in helping the NHS run as smoothly as possible.
References


