Eric Bazuaye
I am a neurology-based botulinum toxin type A (Botox) injecting pharmacist and an independent prescriber at Hull University Teaching Hospitals NHS Trust. As far as I know, my role is the first of its kind in the UK.
I became involved with the neurology botulinum toxin clinic in 2019, after it was determined that a clinical pharmacist supporting the consultant to assess and administer treatment would provide added value to the service.
08:30 — start
In addition to attending the botulinum toxin clinic, this morning I also provide a patient-centred clinical pharmacy service on one of the surgical wards.
Today, I review the appropriateness of medications charted for patients on a general surgical ward who have been admitted for issues such as bowel obstructions or perforations.
13:30
The neurology botulinum toxin clinic is held at Hull University Teaching Hospitals NHS Trust once a week, on a Tuesday afternoon. Today, we have 64 patients booked in, who will be seen by a team comprising one consultant neurologist, two registrars and myself. I usually see 13 patients per clinic.
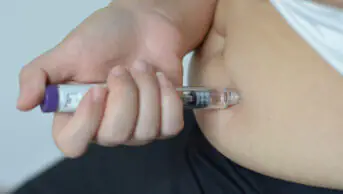
I start by ensuring that the clinic room has the required botulinum toxin, sodium chloride 0.9% solution for reconstitution, equipment for injection, and relevant paperwork to document what is discussed and actioned in patient notes.
When injected into dystonic muscles, botulinum toxin acts by inhibiting the release of acetylcholine into the neuromuscular junction, resulting in partial chemical denervation and muscle relaxation
As an independent prescriber and a trained pharmacist botulinum toxin injector, I am involved in the assessment, preparation and administration of botulinum toxin to known patients with all types of dystonia — a neurological disorder caused by damage or degeneration of the brain resulting in involuntary movements.
The mechanism of clinical efficacy of botulinum toxin in dystonia is not completely understood. However, when injected into dystonic muscles, it acts by inhibiting the release of acetylcholine into the neuromuscular junction, resulting in partial chemical denervation and muscle relaxation.
To be trained to work in the neurology clinic, I spent three months of practical supervision with the consultant neurologist in 2019. During this period, I learned about the muscular structure/anatomy of areas affected by dystonia; movement disorder in dystonia; how botulinum toxin injections are used to reduce the excess muscle activity caused by dystonia; and areas of the face which are safe to inject.
The training also included guidance on assessing patients and administering repeat injections independently for cervical dystonia (involuntary contractions of the neck muscle, also known as torticollis), blepharospasm (abnormal contraction of the eyelid muscles), hypersalivation (excessive production of saliva) and spasticity (a state of increased muscle tone with increased tendon reflexes).
14:00
The consultant neurologist and I have an appointment with a new patient who has been referred by their GP with suspected cervical dystonia.
For new patients in the dystonia clinic, the consultant neurologist usually makes the initial assessment and diagnosis before discussion with, or referral to, myself. Today there is enough time for me to attend the initial assessment with the neurologist and hold a joint clinic, so that I can gain experience and improve my clinical reasoning.
Botulinum toxin treatment is well tolerated and the National Institute for Health and Care Excellence recommended therapy for dystonia
The patient states that their head tends to turn to the right, with it being more prominent when looking down. The patient explains that touching their face or neck helps reduce this feature of cervical dystonia. The patient does not have any associated tremor or pain and their vision, speech, swallowing, hearing, balance, coordination, dexterity, bowel and bladder function are all normal. This information helps exclude other potential neurological diagnoses.
The patient does not take any prescribed medicines, doesn’t smoke, and consumes an average of 21 units of alcohol per week. They can drive without difficulty.
On examination by the consultant neurologist, they have a typical torticollis, a dystonia characterised by involuntary contractions of the cervical musculature that leads to abnormal movements and postures of the head. In this case, the condition causes their head to involuntarily turn to the right with no other significant features.
The neurologist recommends intramuscular botulinum toxin treatment, which is well tolerated and the National Institute for Health and Care Excellence recommended therapy for dystonia.
The consultant explains the side effects to the patient (e.g. swallowing issues, dry mouth, local pain and potential for antibody formation, which may lead to a higher dose in the future) and outlines the benefit of symptom improvement to the patient. They consequently consent to initiating botulinum toxin treatment.
Since the patient has hypertrophy (an increase in size) of the left sternomastoid muscle, I start with an injection of 25 units of botulinum toxin in the left sternomastoid muscle and 50 units in the right splenius capitis muscle. We schedule a standard review in clinic in three months; however, if the benefit of the botulinum toxin wears off before then, we can change the frequency of the repeat injection appointments to every two months.
15:00
I see my second patient, who comes in for a repeat injection, independently from the consultant. Prior to meeting with them, I review their case notes to understand the type of dystonia I am treating. Their record shows that they have been diagnosed with cervical dystonia. They have a long history of muscle tension, stiffness, pain in the neck and shoulder, and balance issues.
As I meet the patient in the waiting area, I observe them walk with their head tilted towards the right. During the consultation, I check how their previous injection went. They confirm that the treatment is working; however, they explain that it has been more than three months since their last injection and they feel that the botulinum toxin effect is wearing off. They tell me that they have been prescribed etoricoxib, amitriptyline and diazepam in the past for their cervical dystonia, but could not tolerate them owing to side effects. They say that botulinum toxin controls their symptoms very well.
I assess the patient to determine whether they are suitable for a further injection. Owing to their right-sided rotatocollis (neck rotation) and laterocollis (head tilt), I administer 25 units in the right trapezius, 25 units in each splenius capitis and 25 units in the right sternocleidomastoid muscle. I give them the opportunity to ask questions, book another appointment in three months and then document our consultation and dose administered in their notes.
15:30
The next patient has a previous diagnosis of left blepharospasm and is attending the clinic for a repeat injection. During the consultation, they tell me that they do not feel that their previous dose was strong enough and believe an increased dose of botulinum toxin would be beneficial. Following discussion with the consultant neurologist, I was instructed to increase the dose of botulinum toxin by five units. I administer ten units superomedially (above the eye toward the midline of the face), ten units superolaterally (above the eye away from the midline) and ten units laterally (on the side away from the midline) around the left eye, again documenting our consultation and dose administered in the patient notes.
16:00
I review another patient presenting for a repeat botulinum toxin injection, but this time for hypersalivation associated with Parkinson’s disease. We discuss their condition and previous treatment, and the patient confirms that the injection is helping their symptoms with no side effects. They would like to continue having treatment. I administer 25 units of botulinum toxin in each parotid gland and book another appointment for them in two months’ time.
16:30
My final patient of the day is receiving a repeat botulinum toxin injection for spasticity. They have a learning disability and their mum is their main carer, who confirms that the injections are beneficial. As per the patient’s clinic note, I administer 50 units of botulinum toxin in the left bicep, 50 units in the left brachioradialis and 50 units in the left common flexor origin. I organise for the patient to be seen again in two months time.
17:00 — finish
To conclude the session, I generate clinic letters for all the patients that I have seen, detailing the units of botulinum toxin administered, the areas injected, next clinic appointment and any other relevant information that would be shared with their GP and is available electronically for other healthcare providers.
Currently, I am working alongside the neurology team to further develop the efficiency of the clinic. Since starting to work independently, I have managed to release medical staff for other critical work and I am taking the lead in supporting the long-term plan of moving the clinic to predominantly non-medical injectors, thus reducing the number of registrars needed at the clinic.
Box: Are you interested in a similar role?
- My role is banded as NHS Agenda for Change Band 7;
- To my knowledge, there are no professional groups/societies associated with this role so I would recommend undertaking medical aesthetics training. As a medically-trained aesthetics pharmacist, I have an in-depth knowledge of facial anatomy and skin function. I completed my foundation and advanced Botox and dermal fillers training course through Derma Medical in 2018;
- Undertake further education to upskill yourself. A clinical pharmacy diploma and independent prescriber qualification are desirable;
- Be prepared and confident to branch out of your comfort zone by expressing interest in shadowing neurology botulinum toxin injectors;
- Look out for internal emails requesting clinical support in unusual areas and ask to get involved.