Shutterstock.com
The chief executive of a national charity has welcomed a commitment by G20 health ministers to tackle antibiotic usage and begin implementing national action plans by the end of 2018.
At a meeting, held on 19 and 20 May 2017 in Berlin, representatives from 20 of the world’s leading economies and the European Union signed a declaration on global health that will feed into the G20 leaders’ summit being held later this year.
Colin Garner, chief executive of the charity Antibiotic Research UK and a former pharmacist, says it is encouraging to see a coordinated response to the threat of antimicrobial resistance. But, he says, it will remain to be seen whether it translates into action.
“I suppose the question is about delivery, and how that will be made to happen, and also whether there’s going to be new money set aside in some way to tackle antibiotic resistance because it certainly needs tackling,” says Garner.
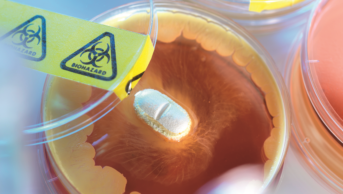
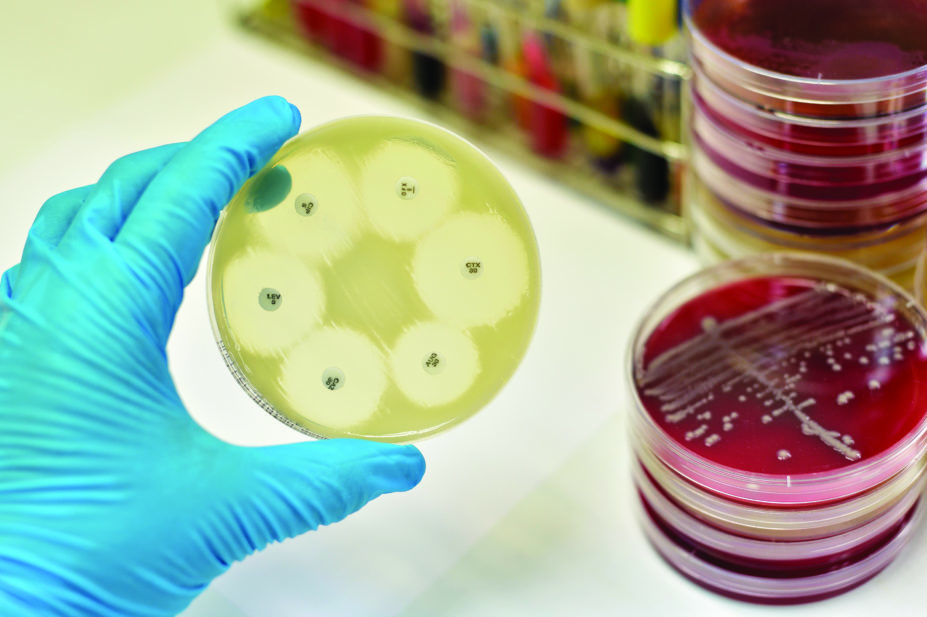
Reducing antibiotic use is key, he adds. “A lot more control needs to be introduced to prevent widespread abuse of antibiotic usage, because the more antibiotics are used, the more that you’re going to drive resistance.”

Source: Courtesy of Antibiotic Research UK
Colin Garner, chief executive of the charity Antibiotic Research UK and a former pharmacist, says it is encouraging to see a coordinated response to the threat of antimicrobial resistance.
The countries have pledged to “lead by example” on tackling antimicrobial resistance by putting into place national action plans by the end of 2018, as called for in the World Health Organization (WHO) Global Action Plan. The declaration also states that they will improve antimicrobial resistance surveillance and antibiotic usage, including a drive towards obligatory antibiotic prescribing.
The declaration also states countries will take action to reinvigorate and incentivise research and development on antimicrobial agents and encourage better coordination of existing initiatives.
Globally, the sale of antibiotics over the counter is widespread and a 2015 WHO survey found that most countries had no action plan in place to address antibiotic resistance.
As well as exploring ways to combat antimicrobial resistance, the meeting looked at ways to improve global health crisis management and better support vulnerable countries in strengthening their national health systems.
The presidency of the G20, which represent two-thirds of the world population, is currently held by Germany where the leaders’ summit will take place in Hamburg in July 2017.
In further efforts to tackle antimicrobial resistance this week, the European Medicines Agency recommended changes to the prescribing information for the antibiotic vancomycin.
It comes as part of a review by the Committee for Medicinal Products for Human Use (CHMP) of the product information for old antibacterial agents.
CHMP says that current data do not support the use of the vancomycin for the treatment of staphylococcal enterocolitis or to decontaminate the gastrointestinal tract in patients with a weakened immune system.
It also advises changes to the way infusion dosages of the antibiotic are calculated, stating these should be based on the patient’s age and weight. This was based on evidence that the previously recommended doses often resulted in suboptimal serum levels of the antibiotic.
The recommendations support the use of vancomycin infusion for treating serious infections caused by certain bacteria including MRSA (methicillin-resistant Staphylococcus aureus) and orally for Clostridium difficile infections. They also still include vancomycin for the prevention of bacterial endocarditis in patients undergoing surgery and to treat infections in patients undergoing peritoneal dialysis.
Delayed antibiotic prescriptions for uncomplicated LRTI do not increase hospital admission rates
Also, a study published in the BMJ
[1]
on 22 May 2017, revealed that giving patients a delayed antibiotic prescription for uncomplicated lower respiratory tract infection (LRTI) was not associated with an increased risk of 30-day hospital admission or death compared with immediate prescription.
The prospective cohort study involved 28,883 people treated at GP surgeries in the UK. After 30 days, the rate of hospital admission or death was 0.3% for those who received no antibiotic and 0.4% for those who received a delayed prescription (median advised delay three days), compared with 0.9% in those who received immediate antibiotic prescription.
And, while patients who received an immediate prescription were just as likely to return for consultation on new, worsening or non-resolving symptoms as those who received no prescription, the rate of reconsultation was reduced by 36% for those who received a delayed prescription.
The researchers say the findings should provide reassurance to prescribers who will sometimes err on the side of caution when it comes to antibiotic prescribing because of concerns about complications and medicolegal consequences.
References
[1] Little P, Stuart B, Smith S et al. Antibiotic prescription strategies and adverse outcome for uncomplicated lower respiratory tract infections: prospective cough complication cohort (3C) study. BMJ 2017; 357: j2148. doi: 10.1136/bmj.j2148