BSIP SA / Alamy
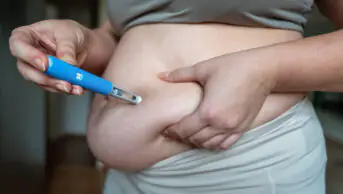
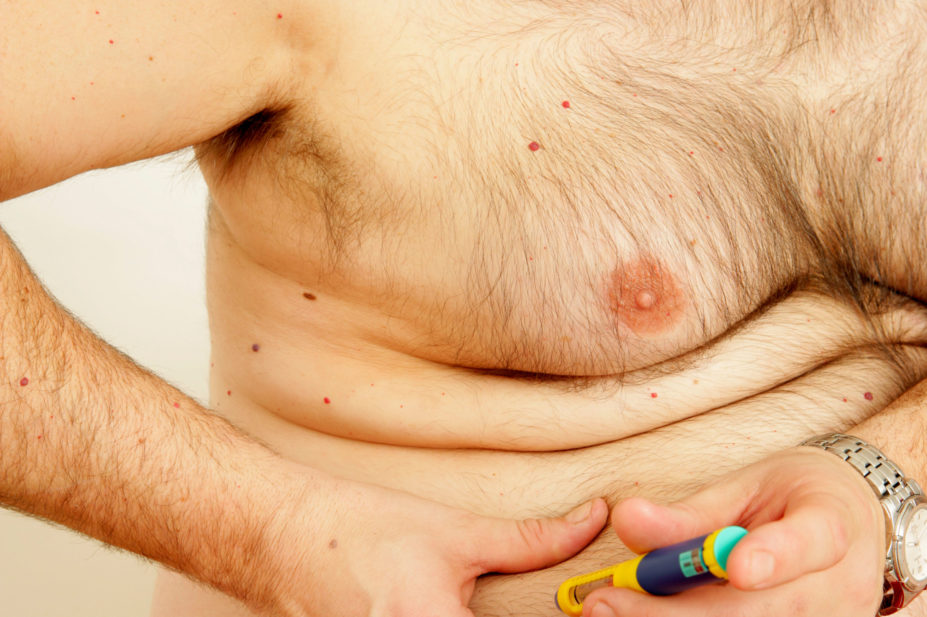
The US Food and Drug Administration (FDA) has approved liraglutide, an injectable drug best known as an antidiabetes agent, to treat obesity in combination with lifestyle changes such as a reduced-calorie diet and exercise.
Adult patients must have a body mass index (BMI) of 30 or greater, which indicates obesity, or a BMI of 27 or greater and at least one weight-related condition such as hypertension, type 2 diabetes, or high cholesterol, the FDA said.
The glucagon-like peptide-1 (GLP-1) receptor agonist will be marketed by Novo Nordisk as Saxenda and is the second obesity treatment to be approved in the United States in 2014 after the combination drug Contrave (naltrexone/bupropion) got the green light in September 2014. The diabetes formulation of liraglutide is marketed as Victoza.
Three clinical trials involving around 4,800 obese and overweight patients were assessed by the FDA in making its decision. All patients received counselling regarding lifestyle changes that consisted of a reduced-calorie diet and regular physical activity.
In one trial — of people without diabetes — participants sustained an average weight loss of 4.5% from baseline compared to placebo at one year, while patients in another trial, this time with patients who had type 2 diabetes, had an average weight loss of 3.7% at one year.
The FDA says patients should be assessed after 16 weeks to determine whether treatment is working and discontinued if a patient has not lost at least 4% of their baseline body weight.
In terms of product safety, Saxenda will have a “boxed” warning about tumours seen in an animal model. Tumours of the thyroid gland have been noted in rodent studies but it is unknown whether the drug causes thyroid C-cell tumours, including a type of thyroid cancer called medullary thyroid carcinoma, in humans. The product’s label will also include serious side effects such as pancreatitis, gallbladder disease, renal impairment, and suicidal thoughts. The most common side effects seen in trials were nausea, constipation, vomiting, hypoglycaemia and decreased appetite. Novo Nordisk has been tasked with a number of follow-on studies, including assessing Saxenda’s potential risk on breast cancer and its cardiovascular safety.
Novo Nordisk, which plans to launch Saxenda in the United States in the first half of 2015, explains that it regulates appetite and lowers body weight through decreased food intake. “As with other GLP-1 receptor agonists, liraglutide stimulates insulin secretion and reduces glucagon secretion in a glucose dependent manner.”
An application to license the product is currently under review by the European Medicines Agency (EMA).
Targeting obesity is a major public health issue in the United States with more than one-third of adults obese. Currently, drug therapies for weight management are limited.
Pharmaceuticals designed to treat obesity can often become embroiled in controversy and several products have been removed from the market in the past over safety concerns. The latest product to cause a stir is Orexigen Therapeutics’s Mysimba (known as Contrave in the United States), an oral combination product containing naltrexone plus bupropion. The EMA approved Mysimba on 18 December 2014.
Prescrire, a drug bulletin based in France, contends that the EMA should reverse its decision to license naltrexone plus bupropion. “A weight loss of a few kilograms achieved through drug therapy cannot in itself justify exposing obese or simply overweight patients to a disproportionate risk of adverse drug reactions, especially since the weight lost is very often regained within months of discontinuing treatment.”
Health authorities should learn the lessons from past mistakes, notably those related to appetite suppressants subsequently withdrawn from the EU market for disproportionate and serious adverse drug reactions such as sibutramine (Sibutral), benfluorex (Mediator) and rimonabant (Acomplia), it says.
“Member states opposing the recommendation still can and should require arbitration by the European Commission and convene a standing Committee meeting. The EU Commission, as last gatekeeper, also has the possibility of deciding not to follow the [EMA’s] recommendation,” it says.