Shutterstock.com
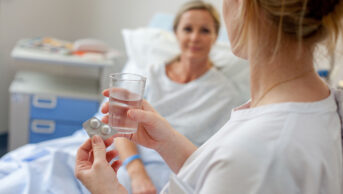
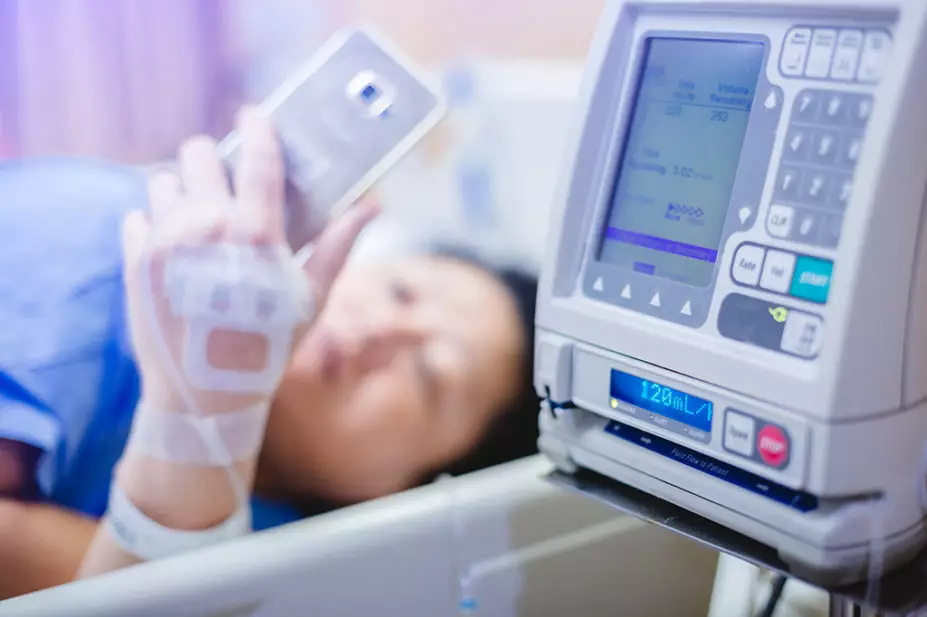
The use of intravenous (IV) infusion devices pre-programmed with safety alerts could save hundreds of lives each year, but they are often not available or the software is overridden, researchers have concluded in a new study.
In the first study of its kind in English hospitals, pharmacy researchers from the University of Manchester reviewed data from two large NHS trusts with smart IV pumps and found the devices may have averted 110 deaths over the course of one year by alerting staff to potentially dangerous drug dose errors.
Published in BMJ Open Quality on 12 July 2022, the study found that less than half of the infusions (338,263 of 745,170 infusions; 45%) carried out at the trusts over one year were administered using a Dose Error Reduction Software (DERS) system. In the other infusions, the system was not used or over-ridden.
Around 20–30 NHS hospitals currently use ‘smart pumps’ with DERS installed. DERS devices are pre-programmed with drug libraries, drug concentrations and dosing rates and limits to mitigate programming and delivery errors, and have been recommended as an intervention to reduce administration errors.
The study authors concluded: “Where DERS is used, the prevalence of potentially harmful medication adverse events is roughly the same as those estimates from systematic reviews where one in ten IV medication errors may be associated with a potential for harm.”
Adam Sutherland, lead researcher on the study and a paediatric pharmacist at Royal Manchester Children’s Hospital, said previous research had shown that “the programming of devices isn’t configured to the way people work in practice”.
“If it isn’t doing what you want it to do, you’re going to bypass the device. That goes some way to explain why they are not used.”
He added that another issue was lack of staff training in their use, and inconsistency in the way that smart pumps are configured, which meant users found them confusing.
The devices need to be configured by the hospital when they arrive — a job often delegated to the pharmacy department, as was the case for Sutherland’s team. “Our organisation purchased a suite of smart pumps last year and turned round to pharmacy department and said ‘you can sort out the programming, can’t you?’”
However, setting up the systems is time-consuming and challenging, partly because of a lack of standardised parameters. The situation is likely to become more acute, Sutherland said, because IV infusion systems in most hospitals will be replaced with smart pumps over the next few years.
“We have got some time now to get our house in order as the NHS, to think about how those pumps will be introduced,” he said.
He added that there was “no reason” why devices could not be pre-programmed with standardised configurations to be used “out of the box”, needing only minor localised changes, but this would require the manufacturers working with pharmacists and other experts to agree standardisation (see box).
The BMJ Open Quality study found that, where DERS was used, it triggered 18 alerts for every 1,000 infusions (17.9/1,000, 95% confidence interval 17.5 to 18.4). However, most of these alerts were for small deviations and could be down to rounding errors (4,652 of 6,067 alerts; 77%). Of the remaining 1,415 alerts considered by experts, 747 were judged to be likely to lead to little or no harm. That left 668 alerts for errors that could cause moderate or severe harm. The researchers estimate that 110 of these could have caused disability or death if they had not been picked up — a rate of 0.2% of DERS infusions administered.
While rates of dangerous infusion errors are low, “my position as a researcher and a pharmacist is, you can’t justify having smart pumps and not using them”, said Sutherland.
“Busy hospitals administer a million infusions a year. If you are using smart pumps, you are going to prevent a lot of potential errors.”
The drugs most likely to be associated with potentially dangerous errors were anticoagulants (24.16 alerts for every 1,000 administrations), antiarrhythmic drugs (21.8 per 1,000 administrations) and antiepileptics (20.86 per 1,000 administrations). Paediatric and medical departments were most likely to trigger potentially harmful alerts.
Box: Recommendations for health systems implementing smart pumps to improve intravenous safety
- Standardise infusion concentrations to facilitate ‘ready to administer’ formulations of frequently-used medications and standardised programming of infusion devices;
- Develop and implement drug libraries based on understanding of their real-world use;
- Develop standardised outcomes and metrics to interpret data from infusion devices;
- Involve all stakeholders in these developments and work with manufacturers and users on device design.