Developed as an alternative to smoking and vaping, oral nicotine pouches are now increasingly popular among young people, likely including those who have never smoked previously. Here, The Pharmaceutical Journal has compiled the latest information about oral nicotine pouches, including regulation, risks and what pharmacists need to know.
- What are oral nicotine pouches?
- Who uses oral nicotine pouches?
- Are oral nicotine pouches used by non-smokers?
- Are oral nicotine pouches less harmful than smoking?
- What are the health impacts of nicotine?
- How are oral nicotine pouches regulated?
- Do oral nicotine pouches interact with medications?
- What should pharmacists be advising patients about oral onicotine pouch use?
- Useful resources
What are oral nicotine pouches?
Oral nicotine pouches are small permeable pouches containing nicotine that are placed between the lip and the gum. Nicotine is then absorbed into the bloodstream through the gum and mouth lining.
They are sometimes referred to as ‘white snus’ and differ from ‘brown snus’, in that they do not contain tobacco. Tobacco snus has a long history of use in Scandinavia but has been banned in other EU countries and the UK since 1992. Oral nicotine pouches were developed in Scandinavia in the early 2000s and began gaining popularity in the UK between 2018 and 20191.
There is currently very little legislation applied to oral nicotine pouches, but the Tobacco and Vapes Bill, which is undergoing discussion in UK parliament, could change that2.
Read on to find out who is using oral nicotine pouches, how the risks compare to smoking and how they affect the body.
Who uses oral nicotine pouches?
Oral nicotine pouch use is on the rise, particularly among young men. Data published in October 2025 suggest that an estimated 1.6% of adults in England used oral nicotine pouches, equating to around 777,000 people, while 14.2% used vapes and 15% smoked cigarettes3,4. See Figure 1 for a full breakdown of oral nicotine pouch use in England since 20135.
Figure 1: Acceleration of oral nicotine pouch use in England since 2013
The number of people using oral nicotine pouches is disproportionately much higher among those aged 16–24 years and 25–34 years, peaking at 7.5% and 3.8% in July 2025, respectively. This age group generally has lower rates of tobacco cigarette use than other demographics but higher rates of vaping and pouch use4. See Figure 2 for a breakdown of oral nicotine pouch use in England, by age5.
Figure 2: Prevalence of oral nicotine pouch use in England, by age
However, respiratory pharmacist Darush Attar-Zadeh thinks it is likely children aged younger than 16 years have tried pouches. “It doesn’t seem to be that high in that group yet, but we’ve got to watch out for that,” he says.
Are oral nicotine pouches used by non-smokers?
Oral nicotine pouches can be used in places where smoking or vaping is not allowed; such as at work, on public transport or in pubs, bars and nightclubs. Many pouch users are likely to be current or former smokers, although there are little data on this and many pouch brands market their products to existing smokers or vapers6.
However, Attar-Zadeh says the increasing popularity of oral nicotine pouches among young people in England might suggest increasing usage among non-smokers.
He suggests that popularity among young people might be influenced by widespread oral nicotine pouch use among Premier League football players and other public figures7.
According to a 2024 survey by Loughborough University into snus use among 679 English professional footballers, 18% of male players (n=113) and 22% (n=11) of female players used snus8. The majority used oral nicotine pouches rather than tobacco-containing snus (52% of men [n=62] and 55% of women [n=6] using snus).
Just under half (42%; n=263) of male players and 39% (n=20) of female players surveyed had used snus at least once in the past. Most respondents in both samples said they did not use snus or oral nicotine pouches as an alternative to smoking, but reported that they found snus use relaxing8.
Are oral nicotine pouches less harmful than smoking?
“Tobacco constituents are very dangerous, and they’re responsible for many tumour formations all over the place — it’s not just lung cancer, every organ can be caught by cancer development,” says Thomas Muenzel, senior professor and environmental cardiologist at Johannes Gutenberg University Mainz, Germany.
As a result, “there is some harm reduction” observed in adults when switching from cigarettes to oral nicotine pouches, he explains.
“If you have coronary artery disease and you switch from tobacco to e-cigarettes, we have less cardiovascular events.”
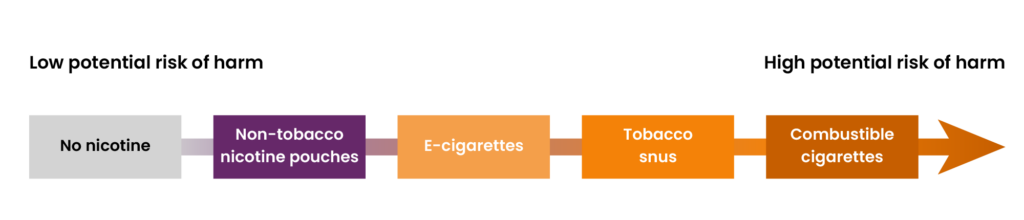
In a 2024 evidence review, the Royal College of Physicians listed oral nicotine pouches as a less harmful alternative to smoking tobacco — second only to medical nicotine replacement therapies9. This was supported by a 2022 systematic review, which suggested that non-tobacco nicotine pouches have a relatively low risk of cancer compared to other nicotine products (see Figure 3)10.
Figure 3: Potential risk of harm from nicotine and tobacco products
Oral nicotine pouches deliver nicotine without tobacco and other chemicals found in cigarettes, which are known to cause harm. However, a 2024 US review of non-industry studies revealed that some harmful chemicals were found in oral nicotine pouches11. However, they were found at lower levels than those typically found in cigarettes and tobacco snus, and in such small quantities that they could not be easily quantified.
The exception to this was formaldehyde, which was consistently found in all oral nicotine pouches at levels comparable to tobacco snus, except for two products that had concentrations three to four times higher than tobacco snus11.
What are the health impacts of nicotine?
The long-term health impacts of nicotine itself are less clear, particularly because it is often studied as a component in tobacco cigarettes.
The specific effects of long-term nicotine use are less well-known
‘E-cigarettes and harm reduction: An evidence review’, Royal College of Physicians
“Given the lack of experimental evidence and observational evidence free from confounding, the specific effects of long-term nicotine use are less well-known,” the Royal College of Physicians review acknowledged10.
In 2025, a report published by the Karolinska Institutet in Sweden said: “Research on the health effects of white snus is almost non-existent and urgently needed.”12
However, data from nicotine-only products, such as e-cigarettes or nicotine replacement therapy, as well as a pharmacological understanding of nicotine itself, can give some idea of the impact of nicotine pouches on the body.
Nicotine acts upon nicotinic acetylcholine receptors (nAChRs) in the central and peripheral nervous system. When AChRs are stimulated, neurotransmitters such as dopamine are released in the brain, producing rewarding psychoactive effects that make nicotine a highly addictive substance. It also increases systolic blood pressure and, to a lesser extent, diastolic blood pressure13. Even medical nicotine replacement therapy has been shown to lead to palpitations and arrhythmia during 3–24 weeks of use14.
Some people have reported positive effects associated with nicotine use, such as increasing focus and short-term memory, and it is reported to improve cognitive function in Alzheimer’s disease, Parkinson’s disease and schizophrenia15–17. But emerging data suggest the harm associated with nicotine in patients with mental health conditions outweighs any potential benefit18. It has also been reported that acute nicotine exposure in adolescents may have long-term effects on the maturation of the prefrontal cortex that could impair cognition19,20.
Some countries, such as France and Belgium, have banned or restricted oral nicotine pouch use, citing their appeal to young people, increasing cases of intoxication linked to oral nicotine pouch use and concerns that they might act as a “stepping stone” to smoking21,22. But, in Sweden, a culture of snus usage is a crucial reason for its low smoking rate — at 5.3%, it is the lowest in Europe and close to the ‘smoke-free’ standard of 5%. However, while rates of lung cancer have declined over time in Sweden, overall cancer incidence is increasing23.
Oral nicotine pouch use has been reported to cause local oral soft tissue abnormalities and alteration of sensation and taste24. Also, there have been several bacteria linked to periodontal diseases found in the saliva of oral nicotine pouch and other tobacco product users25.
Muenzel stresses the nervous system and cardiovascular impacts of nicotine, coupled with its highly addictive nature, should be cause for concern, particularly if patients are going to be using nicotine over the long term. While long-term data are not yet available, Muenzel suggests that biomarkers such as elevated blood pressure should be taken as early indicators of longer-term harm.
You’re getting addicted. This is the problem. It has to be handled like a drug
Thomas Muenzel, senior professor and environmental cardiologist at Johannes Gutenberg University Mainz, Germany
“[Nicotine] activates the sympathetic nervous system, so you get an increase in blood pressure and heart rate,” he adds — the opposite of what people with cardiovascular disease need. And the activation of stress hormones by nicotine could precipitate acute myocardial infarctions and stroke in cardiovascular disease patients.
Muenzel also explains that nicotine can also cause endothelial dysfunction and vascular dysfunction, parameters that indicate increased risk of coronary artery disease, or cardiovascular events in the next 10 to 20 years.
“It takes 10, 20, 30 years when you have a cardiovascular risk factor to develop full-blown disease,” he says. “So people are asking me, ‘if you are 30 years old and you want to use pouches, what is the problem?’ You’re getting addicted. This is the problem. It has to be handled like a drug.”
How are oral nicotine pouches regulated?
Currently, oral nicotine pouches are not regulated as a drug, but as a consumer product. There are no age restrictions related to the sale of oral nicotine pouches in the UK, although most brands and retailers say they impose an 18+ limit (see Figure 46,26–28). There is also no standardisation or regulation around the nicotine concentration contained in the pouch, or around flavourings.
Figure 4: Age policies for popular UK oral nicotine pouch brands
This lack of regulation could change. The Tobacco and Vapes Bill, which was passing through UK parliament at the time of press, could for the first time set age, flavour and advertising restrictions on non-medical nicotine products, such as oral nicotine pouches (see Box)2.
Box: How the Tobacco and Vapes Bill defines nicotine products2
The bill defines nicotine products as:
- A device which is intended to enable nicotine to be delivered into the human body;
- An item which is intended to form part of such a device;
- Nicotine, or any substance containing nicotine, which is intended to be delivered into the human body;
- An item containing nicotine or a substance containing nicotine.
Restrictions on tobacco products and vapes are covered elsewhere in the bill.
But Juan Rafael, a spokesperson for Considerate Pouchers — a campaign group that represents adult oral nicotine pouch users worldwide — says that while he agrees pouches should not be sold to children, he is worried the bill currently being debated could go too far and stop current smokers choosing an alternative that would be less harmful to them and those around them.
If we over-medicalise them, we make it harder for a 20-year smoker to walk into a shop and make a life-saving switch
Juan Rafael, a spokesperson for Considerate Pouchers
“We are not advocating for no laws, no regulation. We’re advocating for common sense regulation that’s based in risk and not fear,” he explains.
“Pouches are accessible, they’re varied and they’re appealing. I feel if we over-medicalise them, we make it harder for a 20-year smoker to walk into a shop and make a life-saving switch.”
Flavours and over-the counter access are crucial to maintaining consumer access, Rafael adds. He believes they should be available at pharmacies as well as other retailers.
Do nicotine pouches interact with medications?
Although oral nicotine pouches are not thought to interact with any medications, the process of smoking cessation should require greater caution with medication.
“If a person is smoking and they’re using the pouches [to try to] quit smoking, it’s not the pouches that interact with the medication. It’s the actual stopping smoking itself that can mean that you have to monitor some medications closely,” says Attar-Zadeh.
According to the National Institute for Health and Care Excellence (NICE), smoking cigarettes increases the metabolism of some medicines by stimulating the hepatic enzyme CYP1A2. When smoking is stopped, even if other nicotine products are in use, the dose of these drugs may need to be reduced and the person monitored regularly for adverse effects. This includes aminophylline, theophylline, chlorpromazine, clozapine, erlotinib, flecainide, methadone, olanzapine, riociguat and warfarin29.
Reducing nicotine may also result in caffeine toxicity, with symptoms such as feeling jittery, says Attar-Zadeh.
He also advises pharmacists treating patients in hospital to ask about oral nicotine pouch use and to consider additional pharmacotherapies, such as a nicotine patch alongside pouch use for the duration of hospital stay to avoid nicotine withdrawal.
“Most of the time people are dual users, which means they smoke and use pouches… The way to look at it is pretty much somebody using an unlicensed version of nicotine replacement therapy. Less than 6mg [the amount of nicotine contained in most pouches] is not very strong, so it could be that if they are smoking a lot, and maybe using less than 6mg of pouch, then that person needs additional pharmacotherapies … and behavioural support is going to be key alongside that,” Attar-Zadeh explains.
“What you don’t want is for an inpatient to experience nicotine withdrawal, because that’s very cruel for a person to experience.”
What should pharmacists be advising patients?
Attar-Zadeh advises that oral nicotine pouches should be avoided in pregnancy, kept out of the reach of children and pharmacists should look for independent research on products manufactured by tobacco companies.
But his advice on pouch use would vary depending on whether the person he is speaking to is already a smoker or user of tobacco products.
“The ultimate goal for smokers is to help them stop smoking and eventually stop nicotine too. And for those who have never smoked, obviously including children and young people, ideally don’t start [consuming nicotine or tobacco] in the first place,” he says.
Useful resources
- 1.The History of Nicotine Pouches: When Were Nicotine Pouches Invented? Zyn. August 2025. Accessed March 2026. https://www.zyn.com/gb/en/blog/when-were-nicotine-pouches-invented.html
- 2.Tobacco and Vapes Bill. UK Parliament. March 2026. Accessed March 2026. https://bills.parliament.uk/bills/3879
- 3.Estimates of the population for the UK, England, Wales, Scotland and Northern Ireland. Office for National Statistics. September 2025. Accessed March 2026. https://www.ons.gov.uk/peoplepopulationandcommunity/populationandmigration/populationestimates/datasets/populationestimatesforukenglandandwalesscotlandandnorthernireland
- 4.Fidler JA, Shahab L, West O, et al. “The smoking toolkit study”: a national study of smoking and smoking cessation in England. BMC Public Health. 2011;11(1). doi:10.1186/1471-2458-11-479
- 5.Resources Relating to Smoking in England. Smoking in England. February 2026. Accessed March 2026. https://www.smokinginengland.info/resources/sts-documents
- 6.Nordic Spirit. Nordic Spirit. Accessed March 2026. https://nordicspirit.co.uk/
- 7.Taylor D. How English football got hooked on snus: ‘Players don’t understand the threat of it.’ NY Times. March 2023. Accessed March 2026. https://www.nytimes.com/athletic/4347316/2023/03/30/premier-league-snus-players-addiction/
- 8.Read D, Cope E, Taylor L. Snus Use in English Professional Football. Loughborough University. 2024. Accessed March 2026. https://www.lboro.ac.uk/media/media/london/images/news/2024/snus-use-in-english-professional-football.pdf
- 9.E-cigarettes and harm reduction: An evidence review. Royal College of Physicians. April 2024. Accessed March 2026. https://www.rcp.ac.uk/media/n5skyz1t/e-cigarettes-and-harm-reduction_full-report_updated_0.pdf
- 10.Murkett R, Rugh M, Ding B. Nicotine products relative risk assessment: an updated systematic review and meta-analysis. F1000Res. 2022;9:1225. doi:10.12688/f1000research.26762.2
- 11.Travis N, Warner KE, Goniewicz ML, et al. The Potential Impact of Oral Nicotine Pouches on Public Health: A Scoping Review. Nicotine and Tobacco Research. 2024;27(4):598-610. doi:10.1093/ntr/ntae131
- 12.Health effects of new nicotine and tobacco products: A review of the scientific evidence. Institutet för miljömedicin – IMM. February 2025. Accessed March 2026. https://ki.se/media/272685/download
- 13.Gogineni HP, Sachs DPL, Brunzell DH. Neurobiology and Mechanisms of Nicotine Addiction. Respiratory Medicine. Published online 2023:45-74. doi:10.1007/978-3-031-24914-3_3
- 14.Benowitz NL, Hukkanen J, Jacob P III. Nicotine Chemistry, Metabolism, Kinetics and Biomarkers. Handbook of Experimental Pharmacology. Published online 2009:29-60. doi:10.1007/978-3-540-69248-5_2
- 15.Heishman SJ, Kleykamp BA, Singleton EG. Meta-analysis of the acute effects of nicotine and smoking on human performance. Psychopharmacology. 2010;210(4):453-469. doi:10.1007/s00213-010-1848-1
- 16.Alhowail A. Molecular insights into the benefits of nicotine on memory and cognition (Review). Mol Med Rep. 2021;23(6). doi:10.3892/mmr.2021.12037
- 17.Barr RS, Culhane MA, Jubelt LE, et al. The Effects of Transdermal Nicotine on Cognition in Nonsmokers with Schizophrenia and Nonpsychiatric Controls. Neuropsychopharmacol. 2007;33(3):480-490. doi:10.1038/sj.npp.1301423
- 18.Kanniah G, Kumar R. A selective literature review exploring the role of the nicotinic system in schizophrenia. Gen Psych. 2023;36(2):e100756. doi:10.1136/gpsych-2022-100756
- 19.Leslie FM. Unique, long-term effects of nicotine on adolescent brain. Pharmacology Biochemistry and Behavior. 2020;197:173010. doi:10.1016/j.pbb.2020.173010
- 20.Goriounova NA, Mansvelder HD. Short- and Long-Term Consequences of Nicotine Exposure during Adolescence for Prefrontal Cortex Neuronal Network Function. Cold Spring Harbor Perspectives in Medicine. 2012;2(12):a012120-a012120. doi:10.1101/cshperspect.a012120
- 21.Galvin G. France has just banned nicotine pouch sales. Where else in Europe are they restricted? EuroNews. February 2025. Accessed February 2026. https://www.euronews.com/health/2025/02/28/france-has-just-banned-nicotine-pouch-sales-where-else-in-europe-are-they-restricted
- 22.The Brussels Times with Belga. Belgium’s Health Minister wants nicotine pouches banned. The Brussels Times. January 2023. Accessed March 2026. https://www.brusselstimes.com/359085/belgiums-health-minister-wants-nicotine-pouches-banned
- 23.Statistics on cancer incidence 2024. Socialstyrelsen. November 2025. Accessed March 2026. https://www.socialstyrelsen.se/publikationer/statistics-on-cancer-incidence-2024-2025-11-9875/
- 24.Davda L. Oral nicotine pouches: A scoping review. Dental Health. May 2025. Accessed March 2026. https://www.bsdht.org.uk/wp-content/uploads/2025/05/Oral-nicotine-pouches.pdf
- 25.Miluna-Meldere S, Vanka SA, Skadins I, Kroica J, Sperga M, Rostoka D. Oral mucosal changes caused by nicotine pouches: case series. Diagn Pathol. 2024;19(1). doi:10.1186/s13000-024-01549-3
- 26.Zyn. Zyn. Accessed March 2026. https://www.zyn.com/gb/en/home.html
- 27.Velo. Velo. Accessed March 2026. https://www.velo.com/gb/en
- 28.LOOP Nicotine Pouches. LOOP. Accessed March 2026. https://loopnicotinepouches.com
- 29.Which drugs are affected by stopping smoking? National Institute for Health and Care Excellence. January 2026. Accessed March 2026. https://cks.nice.org.uk/topics/smoking-cessation/prescribing-information/drugs-affected-by-smoking-cessation/