Jack Xander
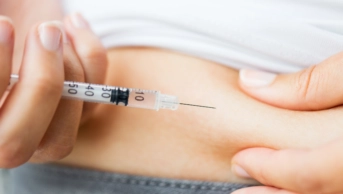
When a pharmacist hands over a medicine to a patient, they might assume the patient will take it as instructed, but a surprising number do not. In fact, it is thought that only around half of medicines for long-term conditions are taken as prescribed in developed countries, and there is little evidence of any improvement in adherence rates over the past 50 years[1]
.
In 2002, a Cochrane Review concluded that effective ways to help people follow medical treatments could have far larger effects on health than any treatment[2]
. Highly sophisticated medicines that can cost billions of pounds to develop, delivered with painstaking medical advice and support, will not be effective if patients fail to take them in the right way, either intentionally or not.
The overall cost of wasted medicines to the NHS in England each year is estimated to be around £300m[3]
. But this figure does not take into account the countless visits to the doctor, further tests and sometimes hospital admissions and other medical costs incurred when a patient does not take their medicines. A doctor who assumes their patient is adherent may increase the dose or add in additional therapies when they do not see the desired effect, further adding to medicines costs.
When people fail to take their medicines as prescribed, it does not just place a burden on the healthcare system; without getting the full benefit from their medicines, patients’ quality-of-life suffers and the risk of morbidity and mortality increases.
Several pharmaceutical companies are looking to develop ways to improve how patients take their medicines. London-based behaviour-change consultancy Spoonful of Sugar, which spun out of University College London in 2011, focuses entirely on changing patient behaviour, and the vast majority of its clients are pharmaceutical companies. As well as trying to understand why particular behaviours occur, the company also develops programmes to change those behaviours.
Spoonful of Sugar’s chief executive officer Tom Kenny, a former GP, says there is an important aspect to non-adherence that often goes unrecognised — it may lead prescribers to doubt the efficacy of the medicines. “Every clinician ‘knows’ that medicines in the real world are less effective than they are in clinical trials,” says Kenny. “They put a lot of that down to biased sample sizes and hand-picked patients but actually a lot of it is that there is an adherence problem.”
Every clinician ’knows’ that medicines in the real world are less effective than they are in clinical trials; they put a lot of that down to biased sample sizes and hand-picked patients but actually a lot of it is that there is an adherence problem
With adherence still such a problem, it is important that interventions to improve it are validated and effective, and that healthcare professionals know how to match patients to these interventions, including the deluge of apps that are coming to market.
Forget me not
People fail to adhere to their medicines for many different reasons but, according to a survey published by pharmacy automation company Omnicell in 2015, the most common is that they simply forget[4]
. The survey found that two-thirds of people forget to take their medicines, while a quarter do not take them because of unpleasant side effects. A further 20% said they felt well so believed their medicines were unnecessary.
Failing to recognise the need for medicines can be a particular issue for patients with long-term conditions, where there are long periods when patients feel well. For example, in epilepsy, where the medicines tend to have quite unpleasant side effects, patients will sometimes reduce or stop taking them during seizure-free periods.
Debi Bhattacharya, a senior lecturer in pharmacy practice at the University of East Anglia, says that there are three main components to adherence: does the patient have access to the medication? Do they have the cognitive and physical ability to take it? And do they have the motivation to take it?

Source: Courtesy of Debi Bhattacharya
Debi Bhattacharya, a senior lecturer in pharmacy practice at the University of East Anglia, says that much of the existing workforce did not receive training in advanced consultation skills
“I think the third element, where we are talking about the psychosocial impact of medicines and how to positively influence that, is where the real challenge is for all healthcare professionals,” says Bhattacharya.
I think the third element [to adherence], where we are talking about the psychosocial impact of medicines and how to positively influence that, is where the real challenge is for all healthcare professionals
She notes that healthcare professionals, by and large, know how to address the former two aspects. For pharmacists, this includes initiatives such as home delivery services, reducing regimen complexity and providing compliance aids.
However, when it comes to patients’ motivation to take their medicines, things become more complex. Bhattacharya says that patients are likely to be forthcoming about discussing barriers to access and cognitive or physical ability, but less willing to discuss intentional non-adherence.
One of the challenges for pharmacists is knowing what conversations to have with patients to elicit information about their levels of adherence.
Bhattacharya, who graduated as a pharmacist in 1999, says that much of the existing workforce did not receive training in this type of consultation. “We were not trained to have a consultation where we are trying to elicit [information] about the barriers to taking a medicine, the patient’s thoughts and feelings, and then linking that to appropriate behaviour-change interventions.”
She says that this should improve as more cohorts come through the new degree system, which includes consultation skills training. “There is recognition that the future pharmacist has a patient-facing role and therefore needs significant consultation skills training,” says Bhattacharya. However, she says that the opportunity for undergraduate students to fully develop these skills is limited by the lack of patient-contact time that results from funding constraints. And behaviour-change techniques, such as motivational interviewing and implementation interventions, are not taught at undergraduate level.
There is recognition that the future pharmacist has a patient-facing role and therefore needs significant consultation skills training
She notes that some of this gap is being addressed through the introduction of the Pharmacy Integration Fund in England and pharmacist prescribing training, which includes advanced consultation skills. At the University of East Anglia, these concepts are introduced in its postgraduate diploma and prescribing course.
“Most prescribing courses will provide training in consultation skills technique so this is all upskilling the workforce to at least be able to have these patient-centred consultations,” she says.
Heidi Wright, practice and policy lead for England at the Royal Pharmaceutical Society, suggests that pharmacists make use of general health coaching as well as training on shared decision-making.

Source: MAG / The Pharmaceutical Journal
Heidi Wright, practice and policy lead for England at the Royal Pharmaceutical Society, suggests that pharmacists make use of general health coaching as well as training on shared decision-making
“The Centre for Pharmacy Postgraduate Education has done a very good consultation skills training course, which is available for all pharmacists and technicians,” says Wright. Training doesn’t have to be specific for pharmacists, she adds. “There’s a lot out there on health coaching and how to have more person-centred, shared decision-making consultations.”
Quest continues
When it comes to interventions to improve adherence, a Cochrane review published in 2014 makes for gloomy reading. “Methods of improving medication adherence for chronic health problems tested to date are mostly complex and not very effective, so that the full benefits of treatment cannot be realised,” it says, adding that the quest for effective and practical interventions to promote medicines adherence and improve clinical outcomes must continue[1].
“We don’t have a gold standard [intervention],” says Bhattacharya. She and her colleagues have developed the ‘Identification of medication adherence barriers questionnaire (IMAB-Q)’, which aims to assist pharmacists and other healthcare professionals to identify a patient’s reasons for non-adherence and link them to interventions. They have validated it using a sample of 600 patients in nine community pharmacies in Suffolk and Norfolk[5]
.
However, when Bhattacharya did some work with nurses and pharmacists to train them on delivering behavioural change interventions, they found it difficult to translate the information gathered on barriers to adherence into selecting the most appropriate intervention.
The team is now working on how to link up the domains of the IMAB-Q to the appropriate interventions in a user-friendly way.
“Pharmacists will have clear guidance in terms of what they should be doing to fix those barriers [to adherence].
Pharmacists will have clear guidance in terms of what they should be doing to fix those barriers [to adherence]
“But there will be lots of flexibility so that it can be patient centred — there will be several correct answers and it will be up to the pharmacist and the patient to work through together and decide which solution is most appropriate,” says Bhattacharya.
The IMAB-Q was developed using the theoretical domains framework, a validated integrative framework intended to act as a vehicle for applying theoretical approaches to interventions for behavioural change[6]
.
Unfortunately, much of the research into adherence interventions has not been based on psychological and behaviour-change principles, says Bhattacharya. She also argues that interventions need to be complex if they are to address the different dimensions of non-adherence.
“Doing a medication review, that’s one thing; providing a text message, that’s one thing; providing a compliance aid, that’s one thing,” she says. “None of these are complex interventions. A complex intervention is having the option of doing all of those things depending upon the patient’s need.”
For Bhattacharya, the focus for research now should not be on developing new interventions but on working out how to match patients to the interventions already available. She says that one of the reasons individual interventions tend to have small effect sizes in trials is that they will only be effective in the subset of participants whose reason for non-adherence is targeted by the intervention being studied.
For example, if somebody proposed studying an app that reminds people to take their medicines or of the correct technique, it would not help people whose difficulty is accessing the medicines or having negative beliefs around their medicines.
Kenny agrees that for interventions to work they have to be built upon first principles.

Source: Courtesy of Tom Kenny
Tom Kenny, a former GP and chief executive officer of Spoonful of Sugar, says that when it comes to digital interventions, the most successful are those designed to be delivered both digitally and by a healthcare professional
“If you build a programme based on the construct from first principles you will have something that is successful, and it will be more successful than a lot of the programmes that are currently in existence,” he says.
“You can do better than that though, by understanding how to refine it based on the context.
“This could include tailoring the programme to specific conditions, the healthcare professional who will deliver the intervention or the method of delivery, such as via an app or with printed materials.”
Automatic friends
The use of apps and digital technology for healthcare, and specifically for adherence, is a relatively recent development, but one that looks set to expand in the coming years.
NHS England is trialling a digital apps library to help patients choose those that are safe and have value.
Examples of apps already in the library are myCOPD, which enables people living with chronic obstructive pulmonary disease to monitor their symptoms, track their medicines use and get coaching on correct inhaler technique; and Squeezy CF, which reminds people with cystic fibrosis to do pelvic floor exercises. Squeezy CF users can also record when they have done the exercises and the app can be tailored to an exercise programme set by their own physiotherapist.
Mona Johnson, senior clinical lead for the NHS Digital programme for apps and wearables, explains that NHS England decides the types of apps that should be prioritised. When an app falls within their scope, NHS Digital will assess it.

Source: NHS Digital
Mona Johnson, senior clinical lead for the NHS Digital programme for apps and wearables, says that healthcare professionals can use patient data as a springboard to have richer conversations with patients about their experience of health and care delivery
The assessment process focuses on safety and technical assurance, considering whether a patient’s data would be vulnerable and how the developer will use data collected by the app in future. Apps deemed to be medical devices are referred to the Medicines and Healthcare products Regulatory Agency and those considered medical services must be registered with the Care Quality Commission, the independent regulator of all health and social care services in England. Any apps that make clinical effectiveness claims must also go through a clinical assurance process.
“Because there are hundreds and hundreds of apps that are coming online every day, it is really difficult for clinicians and patients to understand which of those apps are the ones they should be using,” says Johnson, who also works as a GP.
Because there are hundreds and hundreds of apps that are coming online every day, it is really difficult for clinicians and patients to understand which of those apps are the ones they should be using
“The work that we are doing in the app program is helping people to understand how to be smart consumers.”
Digital partnerships
Johnson believes that technology can be used to empower patients to look after their health and can also be harnessed by healthcare professionals to facilitate improved adherence.
Healthcare professionals can use patient data “as a springboard to have richer conversations with patients about their experience of health and care delivery”, she says, adding that there may be a time when all patients share their real-time health data with healthcare professionals.
“It might mean that there is a totally new kind of role that is created for different sorts of health or care professionals that is more about coaching and facilitating, rather than the paternalistic relationship that’s traditionally been held between healthcare professionals and patients,” she says.
It might mean that there is a totally new kind of role that is created for different sorts of health or care professionals that is more about coaching and facilitating, rather than the paternalistic relationship that’s traditionally been held between healthcare professionals and patients
Kenny agrees that, when it comes to digital interventions, by far the most successful are the ones where the programme is designed to be delivered both digitally and by a healthcare professional.
“This makes them so much more powerful because the communication from within the app and from the healthcare professionals are aligned and joined up.”
Wright also emphasises the importance of the human touch in improving adherence. “You need to spend time with people to help them understand [the reasons for taking their medicines]. You might tell them something when they are in hospital or being discharged, [but] there is so much going on at that point that they do not remember,” she explains.
“People want care; they want that human interaction,” says Kenny, adding: “There is good evidence that pharmacists, if they’re trained up in some simple techniques, can be really effective at improving adherence for patients.”
Reading this article counts towards your CPD
You can use the following forms to record your learning and action points from this article from Pharmaceutical Journal Publications.
Your CPD module results are stored against your account here at The Pharmaceutical Journal. You must be registered and logged into the site to do this. To review your module results, go to the ‘My Account’ tab and then ‘My CPD’.
Any training, learning or development activities that you undertake for CPD can also be recorded as evidence as part of your RPS Faculty practice-based portfolio when preparing for Faculty membership. To start your RPS Faculty journey today, access the portfolio and tools at www.rpharms.com/Faculty
If your learning was planned in advance, please click:
If your learning was spontaneous, please click:
References
[1] Nieuwlaat R, Wilczynski N, Navarro T et al. Interventions for enhancing medication adherence. Cochrane Database Syst Rev 2014; issue 11. Art. No: CD000011. doi:10.1002/14651858.CD000011.pub4
[2] Haynes R, McDonald H, Garg A et al. Interventions for helping patients to follow prescriptions for medications. Cochrane Database Syst Rev 2002, Issue 2. Art. No.: CD000011. doi: 10.1002/14651858.CD000011
[3] Hazell B & Robson R. Pharmaceutical waste reduction in the NHS. 18 June 2015. Available at: https://www.england.nhs.uk/wp-content/uploads/2015/06/pharmaceutical-waste-reduction.pdf (accessed February 2018).
[4] Hagan P. The true cost of medication non-adherence. 2015. Available at: http://www.letstakecareofit.com/wp-content/uploads/2015/10/The-True-Cost-of-Medication-Non-Adherence-Report.pdf (accessed February 2018).
[5] Brown TJ, Twigg M, Taylor M et al. Final Report for the IMAB - Q Study: Validation and Feasibility Testing of a Novel Questionnaire to Identify Barriers to Medication Adherence. Available at: http://pharmacyresearchuk.org/wp-content/uploads/2017/01/IMAB-Q-validation-and-feasibility-testing-full-report.pdf (accessed February 2018).
[6] Phillips C, Marshall A, Chaves N et al. Experiences of using the Theoretical Domains Framework across diverse clinical environments: a qualitative study. J Multidiscip Healthcare 2015; 8: 139–146. doi: 10.2147/JMDH.S78458