This content was published in 2013. We do not recommend that you take any clinical decisions based on this information without first ensuring you have checked the latest guidance.
CELLULITIS is inflammation of loose connective tissue usually with a bacterial cause. It mostly refers to inflammation of subcutaneous layer of the skin. A related term “erysipelas” describes cellulitis that affects the more superficial components of the skin (ie, the dermis and upper subcutaneous tissue) [1]. Cellulitis commonly seen in community pharmacy often results from insect bites or stings. The condition usually responds to prompt treatment with antibiotics, but complications can arise. In 2010 there were 917 deaths as a result of cellulitis in England and Wales, mostly in elderly people [2]. In 2008–09 England and Wales saw 82,000 hospital admissions of people with cellulitis (1.6 per cent of emergency hospital admissions during this period).3 Mean length of stay was 7.2 days and the cost was £133m for beds alone [3].
Key points
- Cellulitis is a skin infection commonly resulting from a break in the skin. It is usually easily treated with antibiotics but it can be fatal.
- To identify urgent cases, ask patients whether they feel unwell or have fever or severe pain. Ask also whether they have any co-morbidities, such as peripheral vascular disease.
- Cellulitis affecting the eye area should be referred to an opthalmologist.
- Pharmacists can use counselling to support successful treatment and to prevent recurrence of infection.
Signs and symptoms
Cellulitis presents as a hot, red and sometimes painful, area of skin. This is usually unilateral. It often affects the lower leg and extends upwards. There may be an obvious entry point for infection, such as a recent wound, a venous ulcer or broken skin between the toes. The skin can blister, especially if it is oedematous. The more superficial infection erysipelas often affects the face and appears as a well defined, raised area. Systemic features, such as fever and malaise, may also be reported and patients can feel unwell. In the late stages, features of sepsis (eg, hypotension and tachycardia; see pp191–2) may be present.
Causes and risk factors
Cellulitis is predominantly caused by Gram-positive bacteria, the most common culprits being Streptococcus pyogenes and Staphylococcus aureus. However, patients with diabetes or penetrating injuries may also be infected with other anaerobic bacteria and immunosuppressed patients occasionally have fungal and Gram-negative infections. The most common risk factors for developing cellulitis are:
- Previous episodes of cellulitis at the same site
- An injury causing a break in the skin
- Leg ulceration
- Fungal infection in adjacent tissue (eg, athlete’s foot)
- A skin condition (eg, eczema)
Other contributing factors include lymphoedema (a chronic condition caused by disruption of the lymphatic system), obesity and leg oedema (eg, due to heart failure). Contrary to anecdotal reports and case series, diabetes, alcohol misuse, intravenous drug misuse and smoking are not risk factors [1,3]. It is important to note that some conditions, such as diabetes, obesity and arterial or venous insufficiency, can delay wound healing and response to antibiotic therapy so in practice keeping a closer eye on the appearance of the affected area and monitoring disease indicators is advisable.
There has been a decrease in childhood periorbital and orbital cellulitis (cellulitis that affects the eye), which may be due to the introduction of the Haemophilus influenzae type B vaccine [1].
Diagnosis
The diagnosis of cellulitis is largely clinical, with symptoms as described. Inflammatory markers such as raised white cell count and C reactive protein (CRP) can support a diagnosis but they are non-specific and a normal CRP does not rule out infection. It is important to rule out other conditions that can mimic cellulitis. For example, erythema alone may indicate an allergic reaction, particularly if associated with itching. Panel 1 describes other conditions that might be mistaken for cellulitis. Microbiological investigations are usually unhelpful in diagnosing cellulitis. Prospective studies have shown that true positive rates from cultures in those with suspected cellulitis are as low as 2–4 per cent [4]. Furthermore, a retrospective study has shown that blood cultures are neither clinically effective nor cost-effective, and should only be performed if a patient has significant systemic upset including temperature above 38C.3 Skin biopsies and aspirations should only be performed when the diagnosis is in doubt. Swabs should only be taken from open cellulitic wounds and caution is needed in identifying which organisms are causing the infection — some may be incidental. Testing for meticillin-resistant S aureus is important in patients who have recently been in hospital, who have had antibiotic treatment, who fail to respond to initial treatment or in whom the infection rapidly progresses.
Treatment
The Eron classification is widely used in the diagnosis and treatment of cellulitis. It guides whether oral or intravenous antibiotics are needed, and if hospital admission is indicated (see Panel 2). Class I patients can usually be managed with oral antibiotics in primary care. Class II patients are suitable for short-term (up to 48 hours) hospital admission and, when their condition is stable, discharged on IV antibiotics (where outpatient parenteral antimicrobial therapy is available; OPAT — see later) or on oral agents. Class III and Class IV patients require hospital admission until the infected area is clinically improving, the systemic signs of infection are resolving and any co-morbidities are stabilised. Patients with suspected necrotising infection require urgent surgical assessment and extensive debridement of the affected area. Before starting treatment, the affected area should be outlined with permanent marker, to monitor the spread of the infection, but this can be difficult in people with lymphoedema because the rash is often blotchy. There is generally a lack of evidence from placebo-controlled trials to support the effectiveness of antibiotics to treat cellulitis, but limited evidence from comparative trials indicates that the appropriate antibiotic will be successful in about 85 per cent of cases. Most cases of cellulitis are caused by beta-haemolytic Streptococci or S aureus, so empirical treatment should be active against these microorganisms. If blood cultures isolate specific pathogens, advice should be sought from a microbiologist. Clinical Knowledge Summaries (CKS), Clinical Resource Efficiency Support Team (CREST) and University College London Hospitals NHS Foundation Trust guidelines have been used as a basis for what follows.
PANEL 1: DIFFERENTIAL DIAGNOSES
- Stasis dermatitis (A type of eczema caused by venous insufficiency and, therefore, blood pooling. It is most commonly mistaken for cellulitis but can be distinguished by an absence of pain and fever. Stasis dermatitis is also often circumferential and bilateral.)
- Acute arthritis (Should be considered if a joint is involved and if there is increased pain on movement.)
- Deep vein thrombosis (Can be difficult to differentiate from cellulitis.
- Clues include significant calf swelling and tenderness without systemic upset.)
- Other, rarer, differential diagnoses include pyoderma gangrenosum(which gives rise to redness and ulceration of legs) and acute liposclerosis.
Primary care
Flucloxacillin is a narrow spectrum antibiotic with good diffusion into skin and soft tissues. It is classically used to treat infections with S aureus but at higher doses it is also active against S pyogenes and is, therefore, first-line monotherapy for Class I cellulitis. The dose is typically 500mg six-hourly po [4,7,8]. Erythromycin (500mg six hourly) 7 is suitable as an alternative to flucloxacillin, for example, for patients allergic to penicillin. CREST also recommends clarithromycin as an alternative to flucloxacillin. It has a similar spectrum of activity as erythromycin but is more convenient for patients, with its twice daily 500mg dosing [4,7].
Clindamycin is recommended in UCLH guidelines and by the Health Protection Agency to treat cellulitis in people who are allergic to penicillin. It may have an additional benefit because it suppresses toxin production by group A streptococci, Clostridium perfringens and S aureus in animal studies. However, CKS recommends seeking specialist advice before using clindamycin because it has a worse adverse effect profile than the macrolides. In addition, antibiotic-associated colitis occurs more frequently — in non-life threatening infection the development of diarrhoea should prompt discontinuation. Doxycycline is reserved for MRSA infection. It has excellent skin and soft tissue penetration but it is contraindicated in pregnancy and lactation. For all these antibiotics treatment duration is usually seven days but will depend on response. Although co-amoxiclav also exerts a bactericidal effect on streptococci and staphylococci it has a considerably broader spectrum of activity (including Gram-negative organisms and anaerobes) so is generally unnecessary for class I patients (but see later).
PANEL 2: ERON CLINICAL CLASSIFICATION SYSTEM3

Secondary care
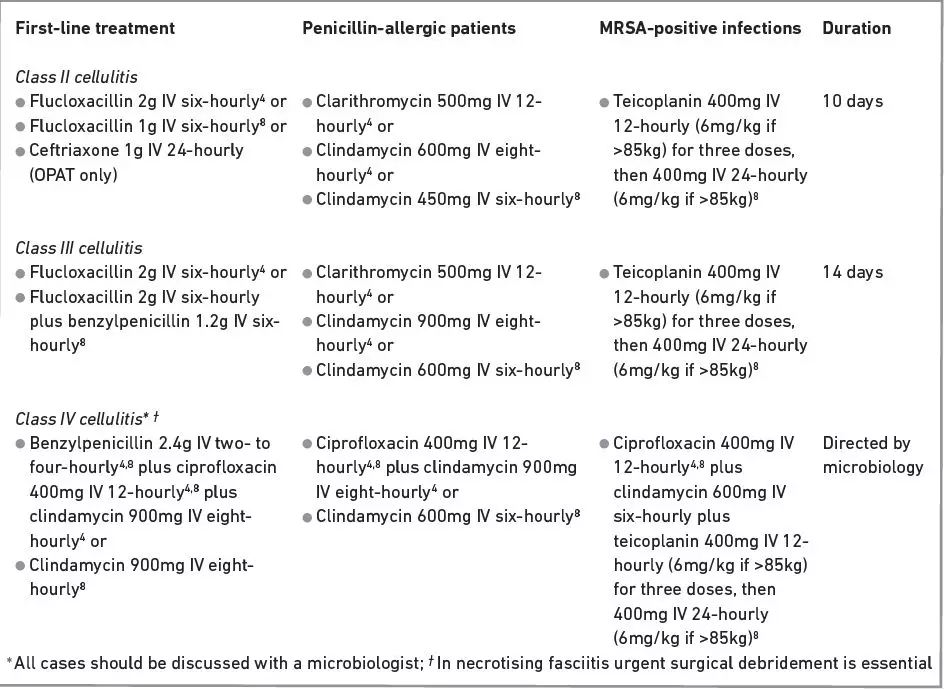
Practice traditionally combined the use of benzylpenicillin and flucloxacillin in the management of patients with cellulitis and admitted to hospital. The short half-life of benzylpenicillin necessitates administration at least every four hours and when combined with IV flucloxacillin, this results in 10 doses of an antimicrobial agent over 24 hours. In most cases this is not practical or necessary and at UCLH this regimen is restricted to use for patients in class III and above. Panel 4 summarises the standard antibiotics used for cellulitis in secondary care. Ciprofloxacin is licensed for infections of the skin and soft tissue caused by Gram-negative bacteria and has excellent tissue penetration. Although it has high oral bioavailability it should be used intravenously in severe infections and in combination with antibiotics that cover Gram positive bacteria.
Teicoplanin is a glycopeptide antibiotic indicated in potentially serious Gram-positive infections, including MRSA, which penetrates well into skin and soft tissue. It should be administered with caution to patients known to be hypersensitive to vancomycin because cross-hypersensitivity may occur, but a history of the drug eruption “red man syndrome” that can occur with vancomycin is not a contraindication. Teicoplanin is used much more at UCLH than elsewhere, due to local bacterial sensitivities. Vancomycin would be the normal option or, increasingly, linezolid in MRSA due to its good tissue penetration. Use of IV therapy for longer than three or four days does not correlate with better outcomes and guidelines recommend switching to oral antibiotics after three or four days of intravenous therapy. However information on the correct time to switch is limited to expert opinion and each case is different. Delay of discharge until complete resolution of fever and signs of inflammation is usually unnecessary [4]. Suggested criteria for oral switch and/or discharge include:
- Pyrexia settling
- Co-morbidities stable
- Less intense erythema
- Falling inflammatory markers
Suitable agents for oral switch therapy4, 8 are flucloxacillin (500mg–1g six-hourly), and clarithromycin (500mg 12- hourly) or clindamycin (300–600mg six-hourly) for patients allergic to penicillin. If an oral preparation of the parenteral drug is available this will usually be the most appropriate oral switch agent. The ideal treatment duration has not been extensively studied. Most cases of uncomplicated cellulitis can be successfully treated with one or two weeks of therapy.
PANEL 3: NECROTISING FASCIITIS
Necrotising fasciitis (NF) is a rapidly progressive infection of the deeper layers of the skin (ie, dermis, subcutaneous tissue), fascia (fibrous connective tissue in muscles and organs) or muscle. Presenting signs are often non-specific. They may resemble cellulitis although the skin may initially be spared. According to the Health Protection Agency, there are around 500 cases of NF per year in the UK and up to 50 per cent of sufferers die. Healthcare professionals should be alert to the clinical signs because it is essential to avoid delay in treatment. Pain is the major feature and often seems out of keeping with the early signs. Diagnosis is made on examination and confirmed by surgical exploration. Deep tissue necrosis leads to tense oedema, fever, overlying erythema with or without crepitus, bullae and cutaneous numbness. The patient usually has overwhelming sepsis and progression to organ failure is rapid. Spontaneous NF is usually caused by Streptococcus pyogenes but NF following a penetrating injury is often polymicrobial. Clinical Resource Efficiency Support Team guidelines list the following laboratory test results as useful in diagnosis: increased white cell count (>14×109/L), reduced sodium (<135mmol/L5), increased urea (>15mg/dl), C reactive protein >16mg/dl,6 CK>600u/L and blood culture. In addition, high lactate (lactate dehydrogenase >2mmol/L) is a marker of anaerobic metabolism. In cases of diagnostic difficulty, investigations that have been reported as being of use include frozen section tissue biopsy, X-ray (showing gas in the subcutaneous tissue), computed tomography and magnetic resonance imaging. However, surgical exploration should not be delayed by waiting for imaging. The best investigation is bedside review by a senior plastic surgeon.
OPAT
Previous standard practice was to admit all class II cellulitis patients to hospital. However many patients can be treated safely and effectively with outpatient parenteral antibiotic therapy (OPAT; see Panel 5) followed by transition to oral agents as the infection resolves. Ceftriaxone, used for the management of class II infections, is administered daily making it a suitable agent for OPAT. Its safety and efficacy are well established.
PANEL 4: ANTIBIOTICS USED FOR CELLULITIS IN SECONDARY CARE
Other treatment considerations
Treatment options can also be affected by the site and source of infection. For example, instead of using flucloxacillin for mild facial cellulitis that does not require hospital admission (ie, there is no intracranial involvement) the recommended first-line treatment is co-amoxiclav 500/125mg every eight hours po for seven to 10 days [4,7,8]. Another example is orbital or periorbital cellulitis, which have potential complications from decreased ocular motility, decreased visual acuity and cavernous sinus thrombosis. It is vital to distinguish the two. Orbital cellulitis should be suspected if there is any bulging of the eye, painful or limited eye movements, abnormal papillary reaction or visual disturbances. The usual causative organisms are S aureus, S pyogenes and H influenzae. Patients should be started on broad spectrum IV antibiotics and referred urgently to an ophthalmologist [11]. The College of Optometrists has developed useful clinical management guidelines. In atypical cellulitis the infection is caused by more unusual organisms. For example, if cellulitis results from salt water contamination, a likely causative organism is Vibrio vulnificus and the recommended treatment is doxycycline plus flucloxacillin. Bites by humans and cats or dogs may involve oral anaerobes and Pasteurella multocida, respectively, and the recommended treatment is co-amoxiclav (500/125mg eight-hourly for seven days).
Counselling
As well as supporting patients to get prompt and effective treatment, pharmacists can provide helpful advice. For example, where a leg is affected, it is important to keep it elevated for comfort and to relieve oedema. A bed cradle may be used to keep bedsheets off sore legs. The following actions can also be recommended:
- Take paracetamol or ibuprofen for pain and fever and drink adequate fluids to prevent dehydration
- Seek immediate advice if antibiotics are not tolerated, if the cellulitis becomes worse, or if systemic symptoms develop or worsen (such as high temperature or nausea and vomiting)
- Avoid compression garments
Note, also, that patients may experience an increase in erythema in the first 24 to 48 hours of treatment, probably related to toxin release. Further deterioration, however, should prompt consultation with a microbiologist and surgical team. Specialist wound management advice should be sought if there is skin blistering, broken skin, exudate or venous ulceration.
PANEL 5: OPAT
Expert opinion in CREST guidelines on the management of cellulitis is that certain people with cellulitis can be treated in the community with intravenous antibiotics followed by a course of oral antibiotics, provided there is an organised service in place to administer the treatment and monitor the patient. This includes people who are systemically ill with stable co-morbidities that are unlikely to complicate treatment, and people who are systemically well, but have one or more co-morbidities that may complicate or delay the resolution of cellulitis (eg, morbid obesity, peripheral vascular disease, diabetes mellitus or chronic venous insufficiency). At UCLH we refer patients to OPAT to facilitate discharge. CKS advises that local guidelines are followed in areas where an organised service exists. The benefits of OPAT include admission avoidance and reduced length of hospital stay, with resulting increases in inpatient capacity, significant cost savings, reduction in risk of healthcareassociated infection and improved patient choice and satisfaction [9]. In a UK study of OPAT episodes, 87 per cent of cases resulted in cure or improvement on completion of intravenous therapy. The readmission rate was 6.3 per cent and patient satisfaction was high. OPAT amounted to 41 per cent of equivalent inpatient costs for an infectious diseases unit, 47 per cent of equivalent inpatient costs using national average costs and 61 per cent of inpatient costs using minimum inpatient costs for each diagnosis [10].
Recurrence and prevention
Several studies suggest that a high proportion of cellulitis sufferers develop recurrent episodes, especially those with untreated predisposing factors. Venous insufficiency has been reported to be the commonest predisposing factor and lymphoedema is the most important risk factor in the development of recurrent cellulitis — each episode of cellulitis adds to the lymphatic damage. Opinion is divided on prophylaxis in patients with recurrent episodes. CREST guidelines recommend antibiotic prophylaxis for one to two years for patients with two or more previous episodes of cellulitis at the same site within a year. Case series have reported benefit from prophylaxis with low dose penicillin V or erythromycin in penicillin-allergic patients (both typically 250mg bd) or with intermittent IM depot penicillin. UCLH guidelines recommend 500mg penicillin od (or 1g if >75kg) with halving of the dose after a year or clarithromycin 250mg od (rather than erythromycin due to its improved tolerability). However early patient-initiated treatment rather than long-term prophylaxis may be preferable. Self-care advice can support prevention, for example, stressing the importance of good hygiene. Any of the following recommendations can be made:
- Treat any breaks in the skin promptly because they are a portal of entry for bacteria.
- Use emollients to prevent dry skin and cracking and eczema and, where appropriate, treat flares with steroid creams.
- Treat athlete’s foot (appropriate antifungal agents include clotrimazole 1 per cent cream for at least two weeks or oral griseofulvin or terbinafine, usually for six weeks depending on the site of infection).
- Wash hands frequently with soap and water or alcohol based hand gels, especially after touching infected skin or wound bandages.
- Bathe regularly.
- Keep any draining wounds covered with clean, dry bandages.
- Do not share personal items (eg, razors, towels or clothing before washing).
- Avoid shaving and other forms of hair removal that irritate skin.
- Wash clothing, sheets, and towels in hot water.
- Keep all personal sports clothing and equipment clean.
- Lose weight and exercise (for obese patients).
PRACTICE POINTS
Reading is only one way to
undertake CPD and the
regulator will expect to see
various approaches in a
pharmacist’s CPD portfolio.
- Train your pharmacy staff to
recognise cellulitis. - Is OPAT available in your
area? Find out. - Make sure you are up to
date with the recommended
management of athlete’s
foot.
The citation information is currently available. For more information please contact support@rcpharm.org