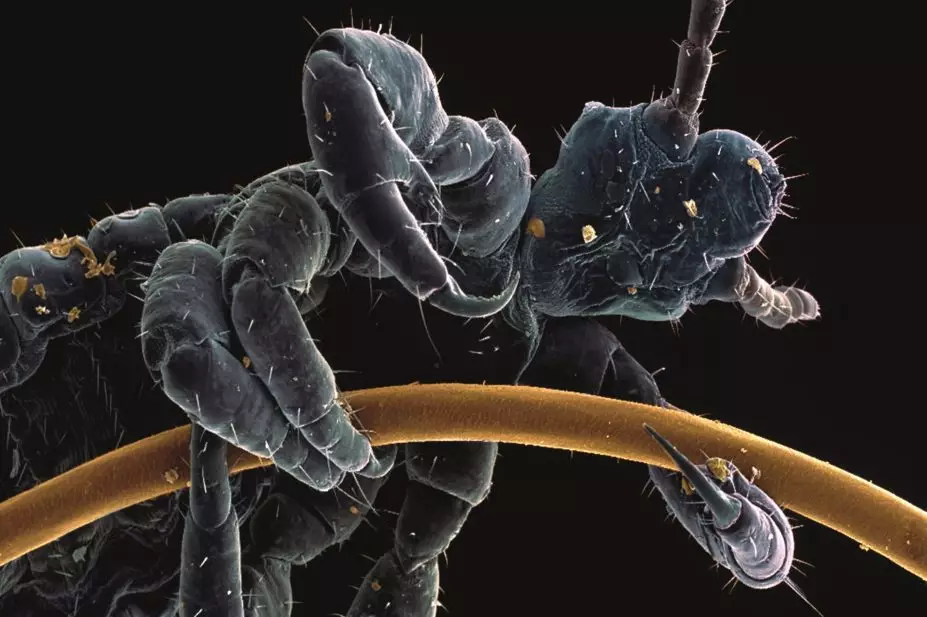
Steve Gschmeissner / Science Photo Library
Despite greater awareness of head lice today, little has changed in the overall burden of this infestation in the community in the past 50 years[1]
. However, it is difficult to know how many cases there currently are in the UK and whether the incidence of cases has increased during this time because the data collected by school inspections up until the mid-1980s were often only estimates[2]
. Based on observations made while collecting lice from schools in Cambridgeshire, the overall prevalence has not changed since the Medical Entomology Centre was engaged by the Community Paediatrician for Cambridge to conduct surveys of insecticide resistance in the mid-1990s, when an average of around 8% of schoolchildren were found to be infested at any one time (unpublished data). The main difference today is that most children seem to have fewer lice than their counterparts had when failing neurotoxic insecticide products were the main treatment options, and it is now harder to collect sufficient numbers of lice for laboratory testing when making school visits than three to four years ago (unpublished data).
Recent data suggest that the spread and prevalence of insecticide resistance in head lice in the United States is caused by knock down resistance (kdr) -type mutations[3]
. However, treatments available to the public in the United States rely almost entirely on pyrethroid insecticide-based products. In the UK, on the other hand, insecticides have almost disappeared; there are very small market shares for both 1% permethrin creme rinse (Lyclear creme rinse) and 0.5% malathion (Derbac-M liquid), which are both severely affected by resistance and should no longer be recommended[4],[5],[6], (as stated in the British National Formulary)[7]
. However, these facts and differences have not stopped misleading reports from appearing in the media[8],[9]
.
This article aims to provide an update on head lice, their identification and the various treatment options available, after considering resistance. Specific counselling advice around treatment failure is also discussed.
Signs and identification of lice
Head lice, Pediculus humanus capitis, have three development stages (egg, nymph and adult) that range from around 0.5mm up to 3mm in length. The full life cylce, including development and reproductive stages, can be found in ‘ Figure 1: Life cycle of the head louse.’ Identification of an infestation can only be made by finding one or more live lice, usually whitish or grey-brown in colour, on a person’s head or scalp. There are no clear symptoms and field studies have found that as many people without lice itch as those with lice, although in some cases itching is persistent and continuous[10],[11]
. Limited evidence suggests that wet combing with conditioner may be the most sensitive diagnostic method, however combing dry hair with a suitable plastic detection comb is quicker and nearly as good a technique for finding lice[12]
.
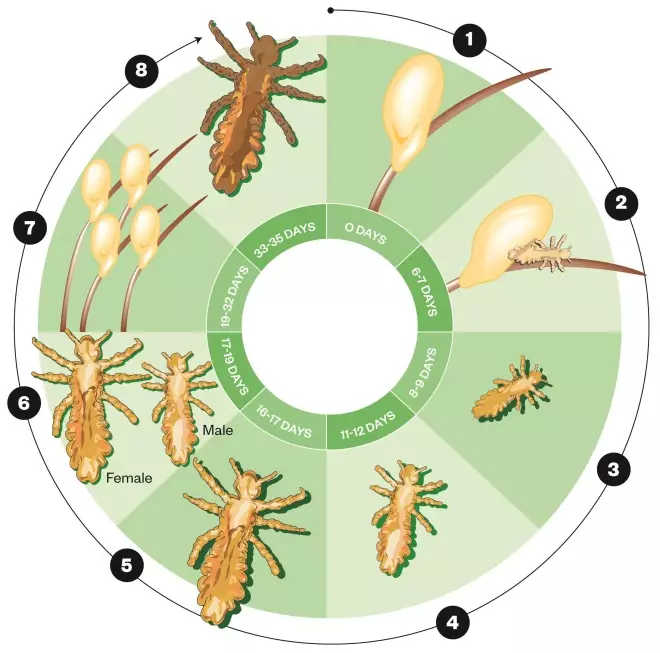
Figure 1: Life cycle of the head louse
The life cycle of the head louse has three stages: egg (nit), nymph and adult. Stages of the lifecycle:
1) Egg (nit) is laid on the hair shaft.
2) Nymph emerges from eggs laid on day 0.
3) Nymph moults for the first time.
4) Second moult.
5) Third moult.
6) Adult male and female lice mate.
7) Female lays first eggs two days after mating and can lay four to eight eggs per day for the next 16 days.
8) Louse dies.
Treatment options
When resistance made insecticide treatments ineffective, the only alternative was the physical removal of lice, such as the “bug busting” method of wet combing with conditioner[13]
. This was found to be more effective than insecticides, with a success rate of up to 57%[4]
. However, it was not appropriate for all households and personal observations during school visits and clinical trials in Cambridgeshire, parts of Suffolk, Bedfordshire, Essex and Hertfordshire found increasingly heavy infestations of hundreds, or even thousands, of lice on some children in the late 1990s (data on file).
Consequently, when physically acting silicone (Hedrin 4% lotion, Thornton & Ross) and silicone/oil mixtures (Full Marks solution, RB) were released in 2005 and 2006, they swiftly became market leaders over the next 12 months. These were more effective than other contemporary options[14],[15]
but were difficult to apply consistently and hard to wash off. These treatments work by forming a water barrier coating that occludes the spiracles (see image 1) and prevents lice from excreting water, causing osmotic stress in vital organs and gut rupture[16]
.
Self-selection, physically acting class I medical devices are now the first choice treatments for most households, with several different products based on silicones, mineral oils, lipid esters, surfactants, or oil-surfactant co-polymers (which aim to make oils more washable) available. Increasing viscosity improves manageability but many patients still find it difficult to apply them thoroughly and consistently. However, there is currently little published evidence of their efficacy. Of the oil-based medical devices available in the UK, only Hedrin Once liquid and spray gels (Thornton & Ross) and Nyda (Pohl Boskamp), which can be washed off after 10–15 minutes, have published clinical investigations[17],[18]
.
Simple shampoo detergents no longer work against lice because the lice encounter them too often and the detergents are too diluted in use. However, some surfactant wetters (e.g. 1,2-octanediol) can dissolve the waterproofing cuticle lipid of the louse so the lice dehydrate[19]
. This process is slow – treatment requires eight hours to overnight using 5% 1,2-octandiol (Hedrin Treat & Go, Thornton & Ross) – but it washes out easily and leaves no oily residues. Despite being easier to apply, there is a greater risk of under use, which means lice do not get adequately coated. This type of product is less effective against eggs and requires a second treatment after a week. Octanediol is not a repellent but it can help prevent lice establishing if they come into contact with treated hair using 1% in a detangler conditioner spray (Hedrin Protect & Go, Thornton & Ross). People who use it regularly are significantly less likely to acquire an active infestation[20]
.
Various other products claim to either kill lice or prevent them; there are theories that because a product contains oil or silicone it will block the louse respiratory spiracles (irrespective of the product’s formulation) or because the product contains a registered biocide it will repel lice (since repellents used to deter flying insects will also repel lice). However, clinical evidence to support these theories are lacking.
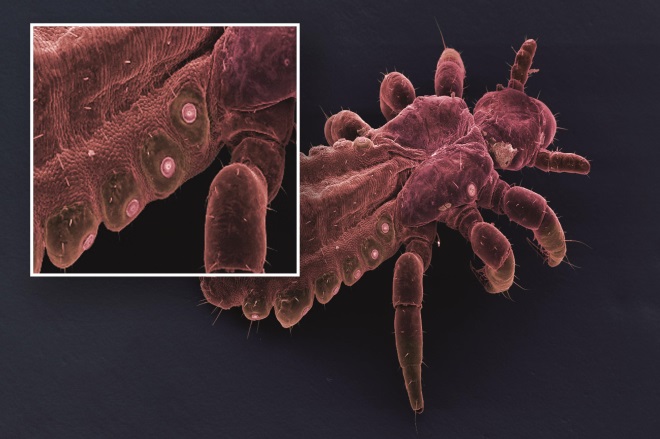
Image: Head louse spiracles
Source: Science Photo Library
Physically acting silicone and silicone/oil mixtures work by forming a water barrier coating that occludes the spiracles (round external respiratory openings, inset) and prevents lice from excreting water, causing osmotic stress in vital organs and gut rupture
Lifestyle and home remedies
Alternative treatments include products that have essential oils or plant extracts, however, there is no clinical evidence of their efficacy. Furthermore, these products do not need to meet the safety or manufacturing standards used for approved drugs. Similarly, there are products marketed as “homeopathic” louse killers that have a small quantity of sodium chloride added to them but there is no evidence of their efficacy[21]
.
Advice for treatment failures and patient counselling
When treating head lice, a plastic detection comb can be used to spread the product evenly; this also removes lice trapped in the fluid. A few days after treatment, a detection comb should be used to ensure no lice were missed or survived treatment. None of the aforementioned products demonstrate complete efficacy and, for inexperienced users, the relative effectiveness inevitably declines. Pharmacists and healthcare professionals may regularly be asked by patients for advice after treatment failure and they should ensure that the following points are included in patient counselling (bearing in mind the information in ‘Box 1: Key treatment points’):
- Ensure the product used has evidence regarding its ability to treat head lice;
- Confirm that sufficient product was purchased to adequately treat the person(s) (e.g. girls with long, thick hair may require more than one bottle of a product for a single application);
- Confirm that the product was applied thoroughly and spread through the hair with a comb to ensure all sections (down to scalp level) were adequately coated;:
- Currently, only the instructions for Hedrin 4% lotion, Derbac-M liquid, Lyclear shampoo and Hedrin Treat & Go state that a second treatment is required;
- Other treatments state that a single application should be sufficient, but if lice persist or are found after seven days, a further treatment should be given.
Confirm a second application of product has been given, where required, and within the recommended time frame;
No treatment failure is desirable, however, some products may be more suited to a household than others. Changing the type of product to another with a different mode of action may be adequate to solve the problem, but in most areas there is no provision for referral for further assistance, except perhaps in the case of at-risk families, where support may be available through social care services.
If a patient has experienced repeated treatment failures, it should first be established that they are dealing with a real and continuing head lice infestation. All products may exacerbate itch symptoms through irritation or drying of the scalp, leading to unwarranted further applications of treatment in the mistaken belief that lice persist. However, if persistent lice are confirmed through detection of live lice, the possibility of repeated reinfestation, either from within the household or from close contacts, should be considered and investigated before further treatment efforts are carried out.
In all cases, even after an apparently successful treatment, a follow-up check with the detection comb should be made at least seven days after the last application. This timing is important for two reasons:
- In some clinical studies, the final check-up was conducted only 24–48 hours after the final treatment application[17]
. This is not a sufficient length of time if any eggs survived; - A retrospective examination of data from around 20 clinical studies found that in a small proportion of thoroughly treated individuals, a few louse eggs hatched up to 13 days after the first treatment, which was six days longer than previously believed[22]
.
Although there have been suggestions that lice can infest household items (e.g. bedding, hats, sofas, etc.), lice do not survive away from their host[23]
and therefore any actions on the environment (e.g. spraying pesticides around the home or freezing teddy bears) are unnecessary.
Box 1: Key treatment points
- Both 1% permethrin creme rinse (Lyclear creme rinse) and 0.5% malathion (Derbac-M liquid) are both severely affected by resistance and should no longer be recommended;
- Self-selection, physically acting class I medical devices are the first choice treatments for most households, with several different products based on silicones, mineral oils, lipid esters, surfactants, or oil-surfactant co-polymers (which aim to make oils more washable) available;
- There are no clear guidelines on optimum time frame of an application. Every product is different, with several modes of action available across the category. This is further confused because some manufacturers have changed their claims in relation to timing and efficacy over the past few years, mostly without reference to clinical evidence data;
- As a general rule, synthetic oil based products can be used with shorter application times because, if they are effective, the coating effect on the lice occurs almost immediately, whereas aqueous formulations generally deliver their effect more slowly through emulsification of lipids or some similar mechanism.
Future treatment options
Newer products that aim to aid diagnosis are currently available in Europe, including gels that dye louse eggs to make them easier to see (e.g. Apaisyl Détect Lentes, Merck Médication Familiale). A new product that loosens old eggshells from hair and makes removing them easier has also just been launched (Hedrin Stubborn Egg Loosener lotion, Thornton & Ross).
However, there is a need for more novel treatment products that are easier to use and are more effective in killing head lice. This will help people manage lice more efficiently but, in the meantime, increased vigilance to stop lice establishing will make treatment easier.
Additional resources
Reading this article counts towards your CPD
You can use the following forms to record your learning and action points from this article from Pharmaceutical Journal Publications.
Your CPD module results are stored against your account here at The Pharmaceutical Journal. You must be registered and logged into the site to do this. To review your module results, go to the ‘My Account’ tab and then ‘My CPD’.
Any training, learning or development activities that you undertake for CPD can also be recorded as evidence as part of your RPS Faculty practice-based portfolio when preparing for Faculty membership. To start your RPS Faculty journey today, access the portfolio and tools at www.rpharms.com/Faculty
If your learning was planned in advance, please click:
If your learning was spontaneous, please click:
References
[1] Burgess IF. Current approaches to head louse treatment – a global update. Self Care [In press] 2016;7(2):41–60.
[2] Burgess IF. Human lice and their management. Adv Parasitol 1995;36:271–342.
[3] Gellatly KJ, Krim S, Palenchar DJ et al. Expansion of the knockdown resistance frequency map for human head lice (Phthiraptera: Pediculidae) in the United States using quantitative sequencing. J Med Entomol 2016;53(3):653–659. doi: 10.1093/jme/tjw023
[4] Hill N, Moor G, Cameron MM et al. Single blind, randomised, comparative study of the Bug Buster kit and over the counter pediculicide treatments against head lice in the United Kingdom. The BMJ 2005;331:384–387. doi: 10.1136/bmj.38537.468623.E0
[5] Downs AM, Stafford KA, Harvey I et al. Evidence for double resistance to permethrin and malathion in head lice. Br J Dermatol 1999;141:508–511. doi: 10.1046/j.1365-2133.1999.03046.x
[6] Burgess IF, Brown CM & Nair P. Comparison of phenothrin mousse, phenothrin lotion, and wet-combing for treatment of head louse infestation in the UK: a pragmatic randomised, controlled, assessor blind trial. F100Res 2014;3:158. doi: 10.12688/f1000research.2026.1
[7] National Institute for Health and Care Excellence. British National Formulary, 13.10.4, Parasiticidal preparations: Head lice. Available at: https://www.evidence.nhs.uk/formulary/bnf/current/13-skin/1310-anti-infective-skin-preparations/13104-parasiticidal-preparations/permethrin (accessed August 2016)
[8] Boyle D. ‘Indestructible’ head lice now resistant to over-the-counter remedies, researchers warn. Daily Telegraph 3 August 2016. Available at: http://www.telegraph.co.uk/news/2016/08/03/indestructible-head-lice-now-resistant-to-over-the-counter-remed/ (accessed August 2016)
[9] De Graaf. Does your child have nits? Watch out! Head lice are becoming indestructible as they are now ‘resistant to 98% of over-the-counter remedies’. Mail Online 3 August 2016. Available at: http://www.dailymail.co.uk/health/article-3721744/Does-child-nits-Watch-Head-lice-indestructible-resistant-98-counter-remedies.html (accessed August 2016)
[10] Mumcuoglu KY, Klaus S, Kafka D et al. Clinical observations related to head lice infestation. J Am Acad Dermatol 1991;25:248–251. doi: 10.1016/0190-9622(91)70190-d
[11] Courtiade C, Labrèze C, Fontan I et al. [Pediculosis of the scalp: study by questionnaire in four groups of school students of Bordeaux in 1990-1991] (in French) Annales de Dermatologie et de Vénéréologie 1993;120:363–368.
[12] Larsen KS, Consultant entomologist; Vander Stichele RH, Family physician. Personal Communications. 10/11 September 2015.
[13] Community Hygiene Concern. Welcome to bug busting. Available at: http://www.chc.org/index.cfm (accessed July 2016)
[14] Burgess IF, Lee PN & Matlock G. Randomised, controlled, assessor blind trial comparing 4% dimeticone lotion with 0.5% malathion liquid for head louse infestation. PLoS ONE 2007;2(11):e1127. doi: 10.1371/journal.pone.0001127
[15] Burgess IF, Lee PN & Brown CM. Randomised, controlled, parallel group clinical trials to evaluate the efficacy of isopropyl myristate/cyclomethicone solution against head lice. The Pharmaceutical Journal 2008;280:371–375. Available at: http://www.pharmaceutical-journal.com/research/research-article/randomised-controlled-parallel-group-clinical-trials-to-evaluate-the-efficacy-of-isopropyl-myristate/cyclomethicone-solution/10967949.article (accessed July 2016)
[16] Burgess IF. The mode of action of dimeticone 4% lotion against head lice, Pediculus capitis. BMC Pharmacol 2009;9:3. doi: 10.1186/1471-2210-9-3
[17] Heukelbach J, Pilger D, Oliveira FA et al. A highly efficacious pediculicide based on dimeticone: randomized observer blinded comparative trial. BMC Infect Dis 2008;8:115. doi: 10.1186/1471-2334-8-115
[18] Burgess IF & Burgess NA. Dimeticone 4% liquid gel found to kill all lice and eggs with a single 15 minute application. BMC Res Notes 2011;4:15. doi: 10.1186/1756-0500-4-15
[19] Burgess IF, Lee PN, Kay K et al. 1,2-octanediol, a novel surfactant, for treating head louse infestation: identification of activity, formulation, and randomised, controlled trials. PLoS ONE 2012;7(4):e35419. doi: 10.1371/journal.pone.0035419
[20] Burgess IF, Brunton ER, French R et al. Prevention of head louse infestation: a randomized, double-blind, cross-over study of a novel concept product, 1% 1,2-octanediol spray versus placebo. BMJ Open 2014;4:e004634. doi: 10.1136/bmjopen-2013-004634
[21] Burgess IF. Lice, damned li…, and regulatory confusion? Outlooks on Pest Management 2014;25:352–355. doi: 10.1564/v25_dec_02
[22] Burgess IF. How long do louse eggs take to hatch: one possible answer to an age-old riddle? Med Vet Entomol 2014;28:119–124. doi: 10.1111/mve.12026
[23] Canyon DV & Speare R. Indirect transmission of head lice via inanimate objects. The Open Dermatology Journal 2010;4:72–76. doi: 10.2174/1874372201004010072


