
Shutterstock.com
Lyme disease is a vector-borne zoonotic infection that is caused by different genospecies of Borrelia and transmitted by the bite of an infected tick[1]
. Ticks are found throughout the UK, although most do not carry the infection, and thrive in moist, humid conditions — particularly woodland and moorland, and some urban parks and gardens[2]
. If left untreated, Lyme disease can develop to late manifestations, affecting the joints, nervous system or the heart.
Healthcare professionals in highly endemic areas have a major role to play in raising awareness, particularly for people visiting from areas where Lyme disease is less common and so may be unaware of the risk. This article describes how pharmacists and their teams can recognise the signs and symptoms of Lyme disease, and provide advice about prevention and management.
Epidemiology
Lyme disease can occur anywhere in the UK; however, areas that have a higher risk include the south of England (including central London) and the Scottish Highlands[1]
. Peak incidence occurs in June, with a smaller peak in September, owing to increased tick activity during the early summer and autumn months when outdoor activities can place people at increased risk of tick exposure and, therefore, tick bites. Some cases occur following travel abroad, as Lyme disease is more commonly reported in Europe (particularly Eastern Europe), Asia, and parts of the United States and Canada[3]
.
The incidence of Lyme disease is steadily increasing; however, the reasons for this are complex and may include climate change, changes in land management and biodiversity, and human interaction with nature, as well as increased awareness of the infection resulting in more cases being reported[4]
. In 2017, 1,579 cases were recorded in England and Wales, an increase from 1,134 cases in 2016[3]
. The most recent data for Scotland show that 200 cases were recorded during 2015[5]
. However, these figures represent laboratory-confirmed cases and do not include data from clinically diagnosed cases, or those that may have been missed or misdiagnosed[6]
.
Risk factors
People of all ages and both sexes are equally susceptible to Lyme disease, although the highest rates occur in older adults aged 45–64 years[3]
. Particular “at risk” groups can include people who take part in recreational outdoor pursuits (e.g. walkers, off-road cyclists, anglers and horse riders), school-aged children, and occupational groups, such as countryside officers, conservation officers and other outdoor workers[2]
.
Signs and symptoms
An important early sign of Lyme disease, found in around two-thirds of cases, is a slowly expanding annular skin rash called erythema migrans (EM). This may occur 1–4 weeks after a tick bite (with a range of 3 days to 3 months) and can last for several weeks. There is often an area of central clearing that gives the rash a “bull’s eye” appearance (see Figure 1), although atypical rashes that are bruise-like or homogenously red also occur.

Figure 1: Erythema migrans rash
Source: Alamy
A slowly expanding, ring-shaped (or “bull’s eye”) rash called erythema migrans is an important early sign of Lyme disease and is found in around two-thirds of cases
An EM rash is usually not hot, itchy, scaly or painful, which may distinguish it from other common skin conditions such as cellulitis, ringworm and insect bites[1]
. A localised area of redness may occur as a reaction to a tick bite, but this usually resolves over 3–5 days and should be kept under review, rather than treated.
Patients who do not present with EM may be more difficult to diagnose and may receive a delayed or missed diagnosis[7]
. These patients may present with several of the following non-specific symptoms:
- Fatigue;
- Malaise;
- Headache;
- Neck pain or stiffness;
- Fever and sweats;
- Mild cognitive impairment, such as memory problems and difficulty concentrating (referred to as ‘brain fog’);
- Swollen glands;
- Fleeting muscle and joint pains;
- Paraesthesia.
The National Institute for Health and Care Excellence (NICE) guideline recommends that if there is a high clinical suspicion of Lyme disease in people without EM, the test for Lyme disease should be offered and treatment with antibiotics should be considered while waiting for the test results[1]
.
Pharmacists and healthcare professionals may be alerted to the possibility of Lyme disease by questioning the patient about:
- The likelihood of tick exposure (e.g. exposure to highly endemic areas, recreational/occupational activities, seasonal factors);
- History of the tick bite (these may go unnoticed);
- EM;
- Flu-like symptoms, especially following tick exposure, a tick bite or EM;
- Other focal symptoms and signs consistent with Lyme disease, including:
- Neurological symptoms (e.g. facial palsy, unexplained radiculitis [nerve root inflammation]);
- Joint pain and swelling;
- Meningitis, carditis and uveitis (although these are rare symptoms);
- Chronic skin rashes.
Focal symptoms and signs may begin to appear in the first few weeks and months following infection and indicate that the infection has spread from the skin with organ involvement. In the UK and Europe, disseminated Lyme disease tends to cause neurological problems, whereas in the United States, a Lyme arthritis, usually involving a single large joint such as the knee or elbow, is more common[8]
.
Diagnosis
Patients with erythema migrans
An important recommendation in the NICE guideline is that Lyme disease should be diagnosed clinically without laboratory testing in patients with EM[1]
; EM is specific for Lyme disease and prompt treatment will prevent disease progression.
Patients without erythema migrans
However, NICE recommends using a combination of clinical presentation and laboratory testing to guide diagnosis and treatment in patients without EM.
Lyme serology testing (see Box 1) relies on detecting a measurable antibody response to the bacteria, which may be limited in the early stages of infection. Patients with impaired immunity (e.g. those taking immunosuppressants) may also have a false-negative result. The advice from NICE is not to rule out a diagnosis of Lyme disease if there is high clinical suspicion, despite negative test results. False-positive results may occur as a results of previous infection or a cross-reaction.
Box 1: Lyme serology testing
In the UK, Lyme serology testing involves two stages:
- Stage 1: An enzyme immunoassay or an enzyme-linked immunosorbent assay (commonly known as ELISA) aimed at detecting antibodies to Borrelia spp.;
- Stage 2: A second tier immunoblot to confirm that any antibodies present are specific to Borrelia spp.
The National Institute for Health and Care Excellence has produced an algorithm showing recommendations for testing of Lyme disease[9]
. Tests should be carried out at laboratories that are accredited by the UK Accreditation Service, use validated tests and participate in a formal external quality assurance programme.
Histological examination of tissues (e.g. synovial fluid aspirate, synovial membrane, skin biopsies and lumbar puncture with cerebrospinal fluid analysis) may also be needed to confirm diagnosis. Polymerase chain reaction testing aimed at direct detection of Borrelia DNA in tissues may be requested via the Lyme reference laboratory, but has limited sensitivity owing to the low numbers of bacteria in tissues samples[10]
.
Differentials
Symptoms of Lyme disease may overlap with a range of other conditions, including other infectious diseases and tick-borne diseases, as well as a range of non-infectious neurological and auto-immune conditions. This includes but is not limited to[11]
:
- Multiple sclerosis;
- Bell’s palsy;
- Stroke;
- Parkinson’s disease;
- Guillain-Barré syndrome;
- Systemic lupus erythematosus;
- Sarcoidosis.
The relapsing remitting pattern of pain and fatigue may also resemble chronic fatigue syndrome[12]
.
Management
Antibiotic treatment
Treatment with antibiotics should be prescribed according to symptom presentation and a second course of an alternative antibiotic should be considered for patients with ongoing symptoms[1]
. If symptoms continue following two completed courses of antibiotics, healthcare professionals should discuss this with the appropriate national Lyme reference laboratory or refer the patient to a specialist.
However, it is important to note that NICE recommendations for antibiotic treatment have been chosen at the higher ranges of formulary doses and duration to reduce the risk of insufficient treatment. A Jarisch–Herxheimer reaction may occur between 1–12 hours after antibiotics are initiated, but can also occur later and last for a few hours or up to two days. Symptoms include a worsening of fever, chills, muscle pains and headache. If this occurs, patients should be advised to continue with antibiotic treatment and consult their doctor[1]
.
People aged 12 years and over
Patients who are diagnosed with Lyme disease without focal symptoms should be prescribed oral doxycycline 100mg twice per day or 200mg once per day for 21 days as first-line treatment[1]
. For Lyme disease with focal symptoms, refer to Table 1 in the NICE guidance.
Children aged under 12 years
Children with Lyme disease, but no focal symptoms, who are aged 9–12 years and weigh less than 45kg should be prescribed oral doxycycline 5mg/kg in two divided doses on day one, followed by 2.5mg/kg daily in one or two divided doses for a total of 21 days as first-line treatment. For severe infections, this can be increased to 5mg/kg daily for 21 days[1]
.
Children under 9 years of age (who are 33kg and under) with Lyme disease, but without focal symptoms, should be prescribed oral amoxicillin 30mg/kg three times per day for 21 days[1]
.
For children with Lyme disease who have focal symptoms, refer to Table 2 in the NICE guidance (see Box 2).
The NICE committee acknowledged that although doxycycline is not licensed in the UK for children aged under 12 years — and is contraindicated in this age group because of side effects (such as teeth staining) — use in children aged 9 years and over is now accepted specialist practice. The committee agreed that doxycycline is the most effective treatment for Lyme disease and that the risk of dental problems in children is low when it is used for short-term treatment (28 days or less)[1]
,[13]
.
Pregnant women
Women who are pregnant should be treated with antibiotics that are appropriate for the stage of pregnancy in accordance with the British National Formulary
[14]
. Women who contract Lyme disease during pregnancy are unlikely to pass the infection on to their baby if they complete the full course of recommended antibiotics. However, if there are concerns about the baby, this should be discussed with a paediatric infectious disease specialist[1]
.
Ongoing treatment
It may take time for some patients to recover but their symptoms should gradually improve in the months after antibiotic treatment (see Box 2). However, patients whose diagnosis and treatment is delayed, and those with evidence of central nervous system involvement, may experience debilitating ongoing symptoms[15],[16]
. The cause of these symptoms is not fully understood and may include tissue damage, post-infectious immune dysfunction and persistence of bacteria or bacterial debris[16]
.
NICE recommends offering regular clinical review and reassessment to patients with ongoing symptoms, including patients with no confirmed diagnosis. Symptoms related to Lyme disease that may need assessment and management, with reference to relevant NICE guidelines, include:
- Chronic pain;
- Depression and anxiety;
- Fatigue;
- Sleep disturbance.
Prophylactic treatment
The NICE guideline does not cover prophylactic treatment and there is no vaccine currently licensed for use in humans.
Prophylactic treatment following a tick bite with a single dose of antibiotics (e.g. doxycycline) is used in the United States but is not recommended in Europe because the risk of Lyme disease following a single tick bite is low[17],[18]
.
Box 2: Case study
A seven-year-old boy was seen by his GP a week after returning from a camping holiday in the Scottish Highlands. He had a 5cm annular rash at the back of his neck but was otherwise well. His mother had not noticed a tick bite.
The GP diagnosed erythema migrans and prescribed a seven-day course of amoxicillin at the lower end of the British National Formulary dose range. Two weeks later, the child developed a facial palsy, headache and was lethargic.
The GP contacted a paediatric neurologist who arranged for admission and diagnosed Lyme neuroborreliosis, confirmed by Lyme serology and lumbar puncture. The child was showing signs of meningitis and was therefore treated with intravenous ceftriaxone 80mg/kg daily for 21 days. Recovery happened slowly over a six-month period.
Role of the pharmacist
Pharmacists and other healthcare professionals, particularly those in high-risk geographical areas, can provide advice about ticks, tick bites and the risk of Lyme disease[1]
,[2]
,[19]
, including:
- Prevention
- Advice on the areas where ticks are usually found (i.e. woodland and moorland);
- How people can avoid tick bites by covering exposed skin (i.e. wearing trousers rather than shorts), keeping to defined paths when outdoors and using insect repellents containing DEET or permethrin;
- Checking for ticks
- How people can check themselves and their children for ticks after possible exposure;
- How to properly brush down clothing before going inside;
- Tick removal
- The importance of prompt tick removal — the longer an infected tick remains attached to the skin, the higher the risk of Lyme disease transmission;
- How to remove ticks correctly — especially if the pharmacy stocks tick removal tools, such as tick cards or tick hooks (see Box 3 and Figure 2);
- How to clean the bite site with antiseptic and watch for signs of a rash;
- Reassurance
- People may ask whether all tick bites cause Lyme disease:
- Advise that not all ticks are infected;
- Advise that the infection rate varies from 0–15%
[20]
.
- People may ask whether all tick bites cause Lyme disease:
Box 3: How to remove ticks correctly
When dealing with a tick, the main aims are to remove the tick promptly, to remove all parts of the tick’s head and body, and to prevent it from releasing additional saliva or regurgitating its stomach contents into the bite wound. The risk of infection increases the longer a tick remains attached to the skin.
Do:
- Use an approved tick removal tool (available from Lyme Disease Action or many vets and pet shops), and follow the instructions provided. There are two common types of removal tools available — the hook and the loop — that are designed to be twisted to facilitate removal (see Figure 2). These tools will grip the head of the tick without squashing the body;
- Use alternative methods if the tick removal tools are not available:
- With pointed tweezers (not blunt eyebrow tweezers) grasp the tick as close to the skin as possible. Without squeezing the tick’s body, pull the tick out without twisting (it is difficult to twist tweezers without separating the tick’s head from its body). There may be considerable resistance;
- If no tools are available, use a fine thread (e.g. cotton or dental floss). Tie a single loop of thread around the tick’s mouthparts, as close to the skin as possible, then pull upwards and outwards without twisting;
- Start by cleansing the tweezers/tool with antiseptic. After tick removal, cleanse the bite site and the tool with antiseptic;
- Wash hands thoroughly afterwards;
- Keep the tick in a sealed container in case a doctor asks for evidence (label it with date and location). Public Health England is also currently running a tick surveillance scheme to record tick distributions on a national scale (ticks can be posted to them as per instructions on their website).
Do not:
- Squeeze the body of the tick, as this may cause the head and body to separate, leaving the head embedded in the skin;
- Use your fingernails to remove a tick. Infection can occur via any breaks in the skin (e.g. close to the fingernail);
- Crush the tick’s body, as this may cause it to regurgitate its infected stomach contents into the bite wound;
- Try to burn the tick off, apply petroleum jelly, nail polish or any other chemical. Any of these methods can cause discomfort to the tick, resulting in regurgitation, or saliva release.
Source: Lyme Disease Action
[20]
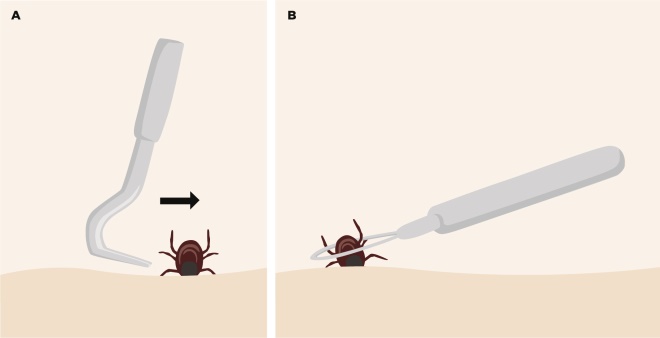
Figure 2: How to safely remove a tick
Source: JL/ The Pharmaceutical Journal
Two common tick removal tools. A) The hook. Approach the tick from the side until it is held by the hook and lift the hook very lightly and turn it to remove the tick. B) The loop. Release the lasso and carefully pass the loop over the tick against the skin. Tighten the loop, rotate and pull the tick out vertically.
Pharmacists should be vigilant for patients presenting with EM over the summer months and for patients with flu-like symptoms at a time when seasonal flu is receding. Such patients should be advised to seek medical help as soon as possible.
Patients with Lyme disease may seek help from the pharmacist for neurological symptoms, joint pain and swelling, multiple rashes, and cardiac or ophthalmic complications, although this is less common. The NICE guideline recommends a discussion with an appropriate specialist for any adult presenting in this way and an emergency referral if there is evidence of central nervous system involvement, cardiac involvement or uveitis. Diagnosis and management of Lyme disease in all people aged under 18 years should be discussed with a specialist, unless they have a single EM lesion and no other symptoms[1]
.
Useful resources
- The National Institute for Health and Care Excellence (NICE) guideline for the diagnosis and treatment of Lyme disease gives advice on awareness, testing, diagnosis, treatment and specialist referral;
-
The NICE resource with images of erythema migran
; - Public Health England’s (PHE’s) Lyme disease guidance, data and analysis;
- PHE’s ‘Tick awareness toolkit’;
- Lyme Disease Action— a national charity providing evidence-based information on an NHS Information Standard-accredited website. Leaflets and posters about ticks and Lyme disease may be supplied free of charge.
References
[1] National Institute for Health and Care Excellence. Lyme disease. NICE guideline [NG95]. 2018. Available at: https://www.nice.org.uk/guidance/ng95 (accessed October 2018)
[2] Public Health England. ‘Be tick aware’ — toolkit for raising awareness of the potential risk posed by ticks and tick-borne disease in England. 2018. Available at: https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/694157/PHE_Tick_Awareness_Toolkit.PDF (accessed October 2018)
[3] Public Health England. Lyme disease epidemiology and surveillance. 2018. Available at: https://www.gov.uk/government/publications/lyme-borreliosis-epidemiology/lyme-borreliosis-epidemiology-and-surveillance (accessed October 2018)
[4] Medlock JM & Leach SA. Effect of climate change on vector-borne disease risk in the UK. Lancet Infect Dis 2015;15(6):721–730. doi: 10.1016/S1473-3099(15)70091-5
[5] Health Protection Scotland & NHS National Services Scotland. Lyme disease, Scotland: annual totals as at 28 July 2016. 2016. Available at: http://www.hps.scot.nhs.uk/resourcedocument.aspx?id=5469 (accessed October 2018)
[6] Evans R, Mavin S, Holden S et al. Lack of accurate information on the prevalence of Lyme disease in the UK. BMJ 2014;348:g2037. doi.org/10.1136/bmj.g2037
[7] Aucott JN, Morrison C, Munoz B et al. Diagnostic challenges of early Lyme disease: lessons from a community case series. BMC Infect Dis 2009;9:79. doi: 10.1186/1471-2334-9-79
[8] Stanek G, Wormser GP, Gray J & Strle F. Lyme borreliosis. Lancet 2012;379(9814):461–473. doi: 10.1016/S0140-6736(11)60103-7
[9] National Institute for Health and Care Excellence. Lyme disease: laboratory investigations and diagnosis chart. 2018. Available at: https://www.nice.org.uk/guidance/ng95/resources/visual-summary-pdf-4792272301 (accessed October 2018)
[10] Dessau RB, van Dam AP, Fingerle V et al. To test or not to test? Laboratory support for the diagnosis of Lyme borreliosis: a position paper of ESGBOR, the ESCMID study group for Lyme borreliosis. Clin Microbiol Infect 2018;24(2):118–124. doi: 10.1016/j.cmi.2017.08.025
[11] Mygland A, Ljøstad U, Fingerle V et al. EFNS guidelines on the diagnosis and management of European Lyme neuroborreliosis. Eur J Neurol 2010;17(1):8–e4. doi: 10.1111/j.1468-1331.2009.02862.x
[12] Treib J, Grauer MT, Haass A et al. Chronic fatigue syndrome in patients with Lyme borreliosis. Eur Neurol 2000;43(2):107–109. doi: 10.1159/000008144
[13] Cross R, Ling C, Day NPJ et al. Revisiting doxycycline in pregnancy and early childhood — time to rebuild its reputation? Expert Opin Drug Saf 2016;15(3):367–382. doi: 10.1517/14740338.2016.1133584
[14] Pharmaceutical Press. British National Formulary 76. 2018. Available at: https://bnf.nice.org.uk/ (accessed October 2018)
[15] Eikeland R, Mygland Ã…, Herlofson K & Ljøstad U. European neuroborreliosis: quality of life 30 months after treatment. Acta Neurol Scand 2011;124(5):349–354. doi: 10.1111/j.1600-0404.2010.01482.x
[16] Rebman AW, Bechtold KT, Yang T et al. The clinical, symptom, and quality-of-life characterization of a well-defined group of patients with posttreatment lyme disease syndrome. Front Med 2017;4:224. doi: 10.3389/fmed.2017.00224
[17] Wormser GP, Dattwyler RJ, Shapiro ED et al. The clinical assessment, treatment, and prevention of Lyme disease, human granulocytic anaplasmosis, and babesiosis: clinical practice guidelines by the Infectious Diseases Society of America. Clin Infect Dis 2006;43(9):1089–1134. doi: 10.1086/508667
[18] Tijsse-Klasen E, Jacobs JJ, Swart A et al. Small risk of developing symptomatic tick-borne diseases following a tick bite in The Netherlands. Parasit Vectors 2011;4(1):17. doi: 10.1186/1756-3305-4-17
[19] Piesman J, Mather TN, Sinsky RJ & Spielman A. Duration of tick attachment and Borrelia burgdorferi transmission. J Clin Microbiol 1987;25(3):557–558. PMID: 3571459
[20] Lyme Disease Action. 2017. Available at: https://www.lymediseaseaction.org.uk (accessed October 2018)


