Fever is common in children and is a symptom seen in many conditions, including COVID-19[1],[2]
. Potential therapy concerns, alongside a general anxiety from parents when medicating children, may lead to fever being untreated or mismanaged[3]
.
This resource outlines guideline-based recommendations for the management of children and young people with fever, including the appropriate use of over-the-counter (OTC) analgesics and should be used to support pharmacists and their teams in providing effective counselling to parents or carers of children with fever.
Understanding fever
The Figure on page 1 of the learning resource (available to download here) provides an overview of fever, including its causes and symptoms in children[4],[5],[6],[7],[8],[9],[10],[11]
.


Initial assessment and when to refer
The National Institute for Health and Care Excellence (NICE) ‘traffic light’ system for identifying risk of serious illness in those aged under 5 years may be used and considered for all children to help determine the risk of serious illness[5]
(see quick reference version
here and for more detailed information see here).
Management
Ensure the parent or carer is fully involved in decisions on how to best treat the child’s fever and associated symptoms. This will help improve compliance with the dosage regime, which can be up to four times a day[12]
.
Antipyretic agents should not be recommended with the sole aim of reducing body temperature in children with fever
[5]
.
As per the NICE CKS, explain to the patient that:
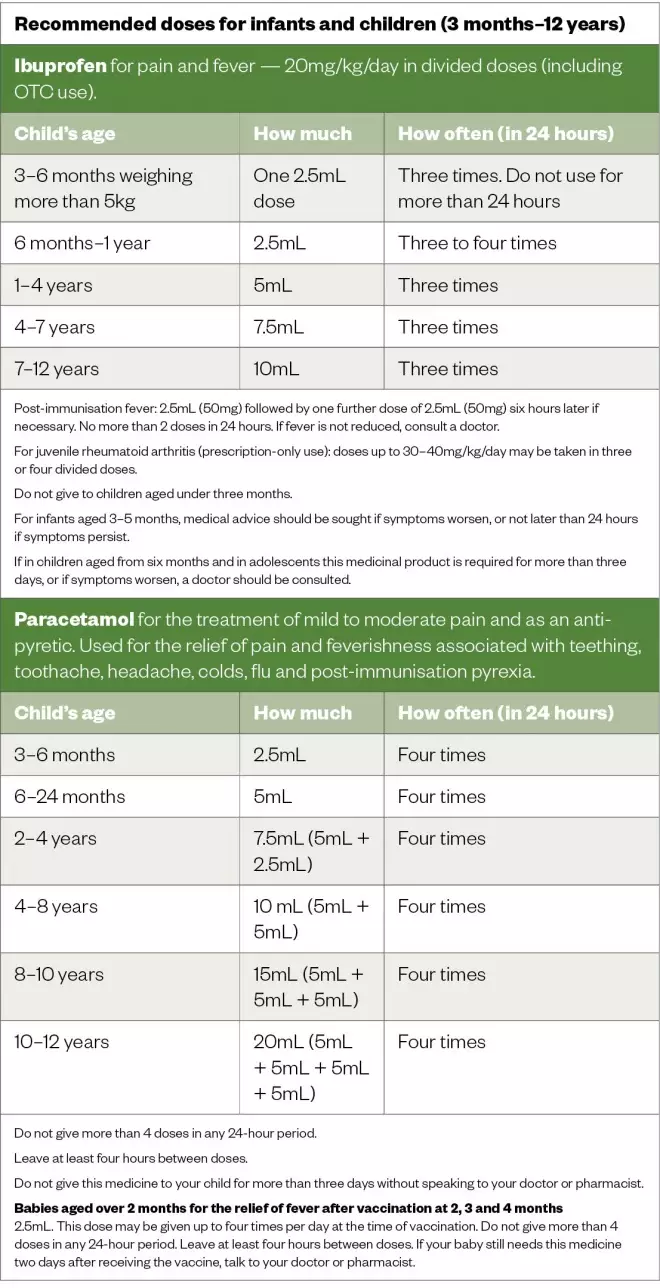
- Either ibuprofen or paracetamol may be used to manage fever, but should only be used when the patient is symptomatic;
- If one analgesic is ineffective, then the other may be trialled;
- Ibuprofen and paracetamol can be used together if fever symptoms are present before the next scheduled dose of either medicine;
- Aspirin should not be used
[4],[12]
[13],[14]
.
During the COVID-19 pandemic, parents may be concerned that their child’s symptoms should not be treated until a diagnosis has been made. It is important that pharmacists and their teams reassure parents that it is safe to give either ibuprofen or paracetamol to patients with COVID-19 (see Box)[15],[16]
.
Box: Managing COVID-19 fever
The Medicines and Healthcare products Regulatory Agency and Commission of Human Medicines (CHM) Expert Working Group concluded that there is currently insufficient evidence to establish a link between use of ibuprofen, or other NSAIDs, and susceptibility to contracting COVID-19 or the worsening of its symptoms. The CHM advise that people can take paracetamol or ibuprofen when self-medicating for symptoms of COVID-19 and should follow NHS advice[15],[16]
.
Pharmacy advice
It is important to explain the importance of non-pharmacological actions to parents or carers as part of a management strategy, including:
- Encouraging increased fluid intake, as fever will make the child sweat more;
- An awareness of signs of dehydration (e.g. reduced urine output);
- Dressing the child appropriately (i.e. do not underdress or over-wrap);
- Checking the child regularly, even through the night, to determine severity[5]
.
Explain to parents that the use of tepid sponging is not recommended and there may be a need to keep the child out of nursery/school until they have recovered[5]
. Some parents may be concerned that ibuprofen can cause gastrointestinal disturbances; reassure them that the formulation is safe for children and does not lead to gastrointestinal side effects[17]
.
Download the learning resource here.
RB-M-20087
Date of preparation: November 2020
Safety, mechanism of action and efficacy of over-the-counter pain relief
These video summaries aim to help pharmacists and pharmacy teams make evidence-based product recommendations when consulting with patients about OTC pain relief:
- Safety of over-the-counter pain relief
- Mechanism of action of over-the-counter pain relief
- Efficacy of over-the-counter pain relief
Promotional content from Reckitt
References
[1] NHS. High temperature (fever) in children. 2017. Available at: https://www.nhs.uk/conditions/fever-in-children/ (accessed November 2020)
[2] NHS. Check if you or your child has coronavirus symptoms. 2020. Available at: https://www.nhs.uk/conditions/coronavirus-covid-19/symptoms/ (accessed November 2020)
[3] Mukattash TL, Alghzawi, NY, Farha RKA et al. An audit on parental attitudes towards medicines used in children. Saudi Pharmaceutical Journal 2018;26(1):133–137. doi: 10.1016/j.jsps.2017.10.001
[4] The National Institute for Health and Care Excellence. Feverish children – management. Clinical Knowledge Summary. 2017. Available at: https://cks.nice.org.uk/topics/feverish-children-management/ (accessed November 2020)
[5] The National Institute for Health and Care Excellence. Fever in under 5s: assessment and initial management. NICE guideline [NG143]. 2019. Available at: https://www.nice.org.uk/guidance/ng143/chapter/Recommendations#thermometers-and-the-detection-of-fever (accessed November 2020)
[6] NHS Inform. Fever in children. 2020. Available at: https://www.nhsinform.scot/illnesses-and-conditions/infections-and-poisoning/fever-in-children (accessed November 2020)
[7] Rutter P. Community pharmacy: symptoms, diagnosis and treatment. 4th ed. Elsevier, 2017. 400 p.
[8] NHS. Chicken pox. 2020. Available at: https://www.nhs.uk/conditions/chickenpox/ (accessed November 2020)
[9] Dowdall M & Stewart K. Differential diagnosis: cold, flu or COVID-19? Pharm J 2020; online. doi: 10.1211/PJ.2020.20208379
[10] NHS. Meningitis. 2019. Available at: https://www.nhs.uk/conditions/meningitis/symptoms/ (accessed November 2020)
[11] NHS. Glandular Fever. 2017. Available at: https://www.nhs.uk/conditions/glandular-fever/ (accessed November 2020)
[12] Electronic medicines compendium. Paracetamol 120mg/5ml Oral Suspension. Available at: https://www.medicines.org.uk/emc/product/9274/smpc#gref (accessed November 2020)
[13] Electronic medicines compendium. Ibuprofen 100mg/5ml Oral Suspension. Available at: https://www.medicines.org.uk/emc/product/4560/smpc#gref (accessed November 2020)
[14] NHS. Ibuprofen for children. Available at: https://www.nhs.uk/medicines/ibuprofen-for-children/ (accessed November 2020)
[15] Medicines and Healthcare products Regulatory Agency Central alerting system. Ibuprofen and coronavirus (COVID-19). 2020. Available at: https://www.cas.mhra.gov.uk/ViewandAcknowledgment/ViewAlert.aspx?AlertID=103025 (accessed November 2020)
[16] NHS. How to treat coronavirus symptoms at home. 2020. Available at: https://www.nhs.uk/conditions/coronavirus-covid-19/self-isolation-and-treatment/how-to-treat-symptoms-at-home/ (accessed November 2020)
[17] Kanabar DJ. A clinical and safety review of paracetamol and ibuprofen in children. Inflammopharmacology 2017;25(1):1–9. doi: 10.1007/s10787-016-0302-3