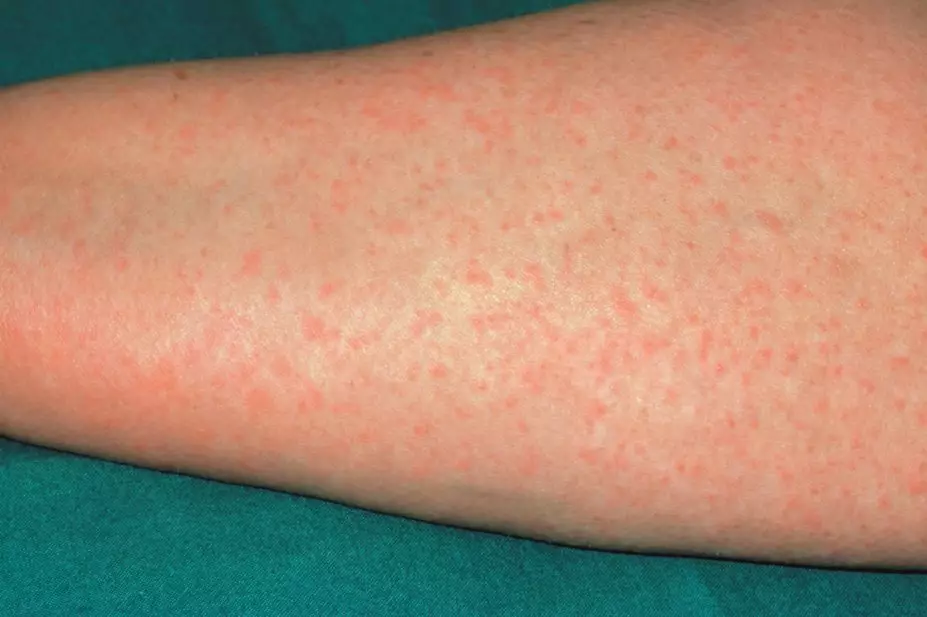
Dr P Marazzi / Science Photo Library
In this article you will learn:
- The incidence of true penicillin allergy
- The drugs to avoid in patients with penicillin allergy
- How to manage patients who experience a severe allergic reaction to an antibiotic
All forms of natural and semisynthetic penicillins, or drugs with a similar structure such as cephalosporins or carbapenems, can cause allergy. These drugs, which have a beta-lactam ring, are recognised as one of the most frequent causes of immediate and non-immediate drug reactions[1],[2],[3]
. Adverse reactions to penicillin have been reported in 0.2% per course of treatment in a large unselected cohort[4]
, and between 3.3–5% in a large drug surveillance programme[5],[6]
.
However, a significant number of patients labelled as ‘penicillin allergic’ are not truly allergic to the drug[7]
. As a result, these antibiotics can be withheld unnecessarily, which may subsequently affect their clinical outcomes, increase healthcare costs and contribute to the development of drug resistant bacteria.
The prevale
nce of penicillin hypersensitivity in the general population is unknown as no prospective studies evaluating sensitisation rates during treatm
ent have been undertaken to date[8]
. However, from data ext
racted from the electronic health medical records of patients who had at least one outpatient visit, the prevalence of ‘allergy’ in the general popula
tion appears to be around 9% for penicillins
and 1.3% for ceph
alosporins[9]
.
Th
e incidence of true penicillin allergy (a type I reaction which is immunoglobulin E [IgE] mediated) is <0.05% of the general po
pulation[10]
. True penicillin allergy can be fatal[11]
,
with a risk of anaphylaxis estimated in around 0.002% of treated patients[12]
. A UK study of drug-induced fatal anaphylaxis between 1992 and 1997 reported 12 deaths due to antibiotics[13],
[14]
. Up t
o 20
% of drug-related anaphylaxis deaths in Europe and up to 75% of deaths for all drug-related anaphylaxis in the USA are caused by pen
icill
in[15],
[16],[17]
.
Risk factors
Patients aged 20–49 years are at increased risk of anaphylaxis[9],[12]
, althou
gh the reasons are unknown. There is no evidence to suggest a hereditary link to anaphylaxis and therefore family history is irrelevant. The
latest data suggest ther
e is no link between atopic disease (e.g. patients with asthma, eczema or hay fever)
and increased risk of penicillin allergy
[8],[9]
, although
patients with atopic disease may experience more severe reactions.
As
many as 85% of patients who previously reacted to penicillin may not react upon second exposure if the time interval from the last exposur
e is prolonged
[9],
[18],[19]
.
A clinical history of penicillin allergy in the more distant past (>15 years) is associated with only a very low risk (0.4%) of reactions[20]
, and only 20–30% of patients positive on a penicillin skin test remain positive after ten years[21]
.
An allergic reaction is most co
mmonly
seen after parenteral administration
[10]
. Less comm
only, penicillin allergy reactions can occur days or weeks after exposure and may persist after treatment has stopped. Other conditions associated with penicillin allergy include serum sickness, drug-induced anaemia, drug reaction with eosinophilia and systemic symptoms (DRESS
) and nephritis
[10]
.
Assessment
The first step to assessing a possible penicillin allergy before a drug is prescribed is to take a detailed history (see ‘Questions to establish a penicillin allergy’)[7],[9]
.
Questions to establish a penicillin allergy
- What was the patient’s age at the time of the reaction?
- Does the patient recall the reaction, and if not, who informed them of it?
- How long after beginning penicillin did the reaction occur?
- What was the route of administration?
- What antibiotics has the patient reacted to in the past?
- What antibiotics has the patient taken and tolerated since the allergy diagnosis?
- What was the nature of the reaction?
- If a rash was present then: a. Describe the nature of the rash (e.g. pustular, urticarial), b. Could the rash be related to an underlying condition (e.g. viral)? c. How long after commencing the antibiotic did the rash appear?
- Why was the patient taking the antibiotic?
- Did this reaction result in hospitalisation?
- Did the reaction resolve on stopping the antibiotic? If so, what happened after stopping the drug?
- What other medications was the patient taking? Why and when were they prescribed?
- Has the patient taken antibiotics similar to penicillin (e.g. amoxicillin, cephalosporins) before or after the reaction? If so, did anything happen?
Histories can be unreliable and can result in over diagnosis of allergy. Some patients may have been too young to fully remember the reaction and patients who report a vague history of symptoms or gastrointestinal intolerance are probably not truly allergic to penicillins. Approximately 80–90% of patients reporting a penicillin allergy are negative when assessed by skin testing[7]
. This test can aid in determining a patient’s allergy status and identifying those at high risk of penicillin reactions[10],[22]
.
If a patient reports a rash after ingestion or administration of a medicine containing penicillin, its type can be used to guide whether a related drug (e.g. a cephalosporin or carbapenem) can be used safely. Rashes that involve hives (raised, intensely itchy spots that come and go over hours), or occur with other penicillin allergic symptoms (e.g. wheezing or swelling of the skin or throat)[7],[10]
suggest a true penicillin allergy. Rashes that are flat, non-itchy, develop over days and do not change in appearance are less likely to represent a dangerous allergy.
Treatment options
Patients who have experienced a type I allergic reaction with penicillins (e.g. urticaria, laryngeal oedema, bronchospasm, hypotension) should not be prescribed beta-lactam agents including penicillins, cephalosporins, carbapenems or monobactams[10],[23]
.
Cephalo
sporins and carbapenems can be used with caution in patients that do not have a history of a type I mediated allergic reaction. Cephalospor
in allergy is largely dependent on the generation of cephalosporin used
[23]
. First generation ceph
alosporins (e.g. cefazolin) were believed to have a cross-reactivity rate of aroun
d 10% in patients with a penicillin allergy
[23]
. However, at the tim
e of these early studies, cephalosporin formulations contained trace amounts
of penicillin[23],
[24],[25]
, so this figure is thought to b
e an overestimate. The true incidence of cross-sensitivity is unknown but there are data to suggest that it is much
lower
[25]
. Second and third gener
ation cephalosporins (e.g. cefuroxime, ceftriaxone, ceftazidime) have a lower propensity for cross reactivity, as they have different side chains to penicillin, which contribute to the decreased immunogenic
ity[26]
. However, alternatives should be used wherever possible (see below).
Carba
penems (e.g. merop
enem, imipenem, ertapenem, doripenem) have a cross reaction rate of 1–6%[27],
[28]
in pa
tients who have previously suffered IgE-mediated reactions to penicillins. A thorough clinical history should be taken before prescribing this class of drugs to a patient with known or suspected penicillin allergy.
Aztre
onam is a monob
actam that does not contain a bicyclic-ring structure[29]
similar to penicillins, cephalosporins and c
arba
penems. It can therefore be used safely in patients
w
ith a history of penicillin allergy
[23],[26],
[30]
, unless the patient is known to be a
llergic to ceftazidime, which has an identical side chain to
aztreonam[30],[31]
.
Tetracyclines (e.g. doxycycline), macrolides (e.g. clarithromycin), aminoglycosides (e.g. gentamicin), metronidazole, quinolones (e.g. ciprofloxacin) and glycopeptides (e.g. vancomycin) are all unrelated to penicillins and are safe to use in patients with penicillin allergy. However, patients with penicillin allergy a
re more likely to react to any class of drug
[10],
[32],[33]
.
Inadvertent administration
It is a medical emergency if inadvertent administration of penicillin in a patient with known penicillin allergy takes place. The offending drug should be stopped immediately. Anaphylaxis should be treated with adrenaline injection and emergency care to maintain blood pressure and support breathing[34]
. A second dose of adrenaline may be required in a small percentage of patients if there is insufficient response. More than two doses are rarely required[35]
.
Rashes or hi
ves can be treated with an antihistamine such as chlorpheniramine, although more severe reactions may require treatment with oral or injectable cor
ticosteroids. The severity of the reaction will determine the dose, duration and formulation of treatment.
F
ollowing emergency management, patients require close monitoring in hospital for 2–24 hours to ensure they do not develop biphasic anaphy
laxis[36],
[37],[38],[39]
. Biphasic anaphylaxis is the recurrence of symptoms within 1–72 hours with no further exposure t
o the alle
rgen
[35]
. The recurrence typically occurs within eight hours[37]
and is managed in the same manner as anaphylaxis[40]
.
The risk of inadvertent administration of a medicine known to cause allergy can be minimised by ensuring the patient knows about their condition, and that an accurate medical history is taken before the medicine is prescribed. In hospitals, all inpatients should have known adverse drug reactions included on all patient documents (e.g. drug charts, prescriptions, patient medication records and discharge summaries); this should inclu
de information on the nature of the reaction and when it occurred.
If inadvertent administration occurs, the incident should be reviewed to identify the reason and effective safety measures put in place to prevent re
currence[41]
. Combination prod
ucts should also be prescribed generically with their individual constituents to help staff identify when a prescribed medicine may be inappropriate.
Case studies
Case study 1: assessing history of allergy
Chloe Monroe is a 47-year-old female admitted to hospital for treatment of possible diverticulitis. Chloe’s notes state that she is allergic to penicillin; the nature of the reaction is gastrointestinal disturbance and diarrhoea. On further questioning, she says she gets an “upset stomach” and diarrhoea when taking oral penicillins and will not ingest these medicines. Chloe says she does not experience any itchiness, rash, swelling or other symptoms when taking penicillin. Does Chloe have a penicillin allergy?
Answer:
Chloe reports gastrointestinal disturbance. This is a known adverse drug reaction but is not a contraindication or true allergy. It is therefore likely that Chloe is intolerant of penicillins, but does not have a penicillin allergy and the medicines can be used safely if required.
Case study 2: treatment options in true allergy
Matthew Bonzer is a 30-year-old patient with a documented history of a penicillin allergy causing an itchy rash. He has been diagnosed with a bacterial respiratory tract infection. What treatment options can be considered?
Answer:
Matthew has previously experienced symptoms of an allergic reaction to penicillins, therefore a non-penicillin drug should be chosen to treat the infection. Clarithromycin is a macrolide antibiotic and is unrelated to penicillin, and the likelihood of the patient experiencing a reaction is low. He can therefore be started on clarithromycin to treat his respiratory tract infection.
Shilpa Jethwa MSc, MRPharmS, is a specialist pharmacist (antibiotics) at Northwick Park Hospital, London North West Healthcare NHS Trust.
Reading this article counts towards your CPD
You can use the following forms to record your learning and action points from this article from Pharmaceutical Journal Publications.
Your CPD module results are stored against your account here at The Pharmaceutical Journal. You must be registered and logged into the site to do this. To review your module results, go to the ‘My Account’ tab and then ‘My CPD’.
Any training, learning or development activities that you undertake for CPD can also be recorded as evidence as part of your RPS Faculty practice-based portfolio when preparing for Faculty membership. To start your RPS Faculty journey today, access the portfolio and tools at www.rpharms.com/Faculty
If your learning was planned in advance, please click:
If your learning was spontaneous, please click:
References
[1] Gomez MB, Torres MJ, Mayorga C et al . Immediate allergic reactions to betalactams: facts and controversies. Curr Opin Allergy Clin Immunol 2004;4:261–266.
[2] Torres MJ & Blanca M. The complex clinical picture of beta-lactam hypersensitivity: penicillins, cephalosporins, monobactams, carbapenems, and clavams. Med Clin North Am 2010; 94: 805–820.
[3] Pichichero ME & Zagursky R. Penicillin and cephalosporin allergy. Ann Allergy Asthma Immunol 2014; 112: 404–412.
[4] Apter AJ, Kinman JL, Bilker WB et al . Represcription of penicillin after allergic-like events. J Allergy Clin Immunol 2004; 113: 764–770 .
[5] Bigby M, Jick S, Jick H et al. Drug-induced cutaneous reactions. A report from the Boston Collaborative Drug Surveillance Program on 15,438 consecutive inpatients, 1975 to 1982. JAMA 1975; 1986: 3358–3363.
[6] Macy E & Poon K-YT. Self-reported antibiotic allergy incidence and prevalence: age and sex effects. Am J Med 2009;122:778 e1-7.
[7] Salkind A, Cuddy P & Foxworth J. Is this patient allergic to penicillin? An evidence-based analysis of the likelihood of penicillin allergy. JAMA 2001;285(19):2498–2505.
[8] Solensky R. Hypersensitivity reactions to beta-lactam antibiotics. Clin Rev Allergy Immunol 2003;24:201–220.
[9] Mirakian R, Leech SC, Krishna MT et al. Management of allergy to penicillins and other beta-lactams. Clinical & Experimental Allergy 2015;(45):300–327.
[10] Bhattacharya S. The facts about penicillin allergy: a review. J Adv Pharm Technol Res 2010;1(1):11–17.
[11] Saxon A, Beall GN, Rohr AS et al . Immediate hypersensitivity reactions to beta-lactam antibiotics. Ann Intern Med 1987;107:204–215 .
[12] Idsoe O, Guthe T, Willcox RR et al . Nature and extent of penicillin side-reactions, with particular ref erence to fatalities from anaphylactic shock . Bull World Health Organ Geneva, Switzerland 1968; 38:1 59–1 88.
[13] Pumphrey RS & Davis S . Under-reporting of antibiotic anaphylaxis may put patients at risk . Lancet 1999; 353: 1157–1158.
[14] Lee P & Shanson D. Results of a UK survey of fatal anaphylaxis after oral amoxicillin. J Antimicrob Chemother 2007;60:1172–1173.
[15] Neugut AI, Ghatak AT & Miller RL. Anaphylaxis in the United States: an investigation into its epidemiology . Arch Intern Med 2001; 161: 15– 21.
[16] Delage C & Irey NS . Anaphylactic deaths: a clinicopathologic study of 43 cases . J Forensic Sci 1972; 17: 525–5 40 .
[17] Lenler-Petersen P, Hansen D, Andersen M et al. Drug-related fatal anaphylactic shock in Denmark 1968 –1990. A study based on notifications to the Committee on Adverse Drug Reactions . J Clin Epidemiol 1995; 48: 1185–118 8 .
[18] Eisenberg M. Differences in sexual risk behaviors between college students with same-sex and opposite-sex experience: results from a national survey. Arch Sex Behav 2001;30:575–589.
[19] Wong T, Singh AE & De P. Primary syphilis: serological treatment response to doxycycline/tetracycline versus benzathine penicillin. Am J Med 2008;121:903–908.
[20] Holm A & Mosbech H. Challenge test results in patients with suspected penicillin allergy, but no specific IgE . Allergy Asthma Immunol Res 2011; 3: 118–122.
[21] Sullivan TJ , Wedner HJ , Shatz GS et al. Skin testing to detect penicillin allergy. J Allergy Clin Immunol 1981; 68: 171–180 .
[22] Phillips E, Louie M, Knowles SR et al. Cost-effectiveness analysis of six strategies for cardiovascular surgery prophylaxis in patients labeled penicillin allergic. Am J Health Syst Pharm 2000;57:339–345.
[23] James CW & Gurk-Turner C. Cross-reactivity of beta-lactam antibiotics. Proc (Bayl Univ Med Cent) 2001;14(1):106–107.
[24] Pederson-Bjergaard J. Cephthalothin in the treatment of penicillin sensitive patients. Acta Allergol 1967:22:299–306.
[25] Anne S & Reisman RE. Risk of administering cephalosporin antibiotics to patients with histories of penicillin allergy. Ann Allergy Asthma Immunol 1995;74:167–170.
[26] Shepherd GM. Allergy to beta-lactam antibiotics. Immunology and Allergy Clinics of North America 1991;11:611–633.
[27] Romano A, Gaeta F, Valluzzi RL et al. Absence of cross-reactivity to carbapenems in patients with delayed hyper sensitivity to penicilli ns. Allergy 2013;68(12):1618–1621.
[28] Frumin J & Gallagher JC. Allergic cross-sensitivity between penicillin, carbapenem, and monobactam antibiotics: what are the chances? Ann Pharmacother 2009;43(2):304–315.
[29] Kishiyama JL & Adelman DC. The cross-reactivity and immunology of betalactam antibiotics. Drug Saf 1994;10:318–327.
[30] Saxon A, Beall GN, Rohr AS et al. Immediate hypersensitivity reactions to beta-lactam antibiotics. Ann Intern Med 1987;107:204–215.
[31] Neftel KA & Cerny A. Beta-lactam antibiotics other than penicillins and cephalosporins. In: Dukes MNG, editor. Meyler’s Side Effects of Drugs. 12th ed. Amsterdam: Elsevier;1992;632–634.
[32] Madaan A & Li JT. Cephalosporin allergy. Immunol Allergy. Clin. North Am. 2004;24(3):463–476.
[33] Ulman K. AANP: certain cephalosporins may be safe for patients with penicillin allergies. Modern medicine 2007.
[34] Lockey RF, Bukantz SC & Bousquet J. Allergens and allergen immunotherapy. Informal Health Care 2004.
[35] Simons FE. World Allergy Organization survey on global availability of essentials for the assessment and management of anaphylaxis by allergy-immunology specialists in health care settings. Annals of Allergy, Asthma & Immunology 2010;104(5):405–412.
[36] Marx J. Rosen’s emergency medicine: concepts and clinical practice 7th edition (2010). Philadelphia, PA: Mosby/Elsevier; 1511–1528.
[37] Lee JK & Vadas P. Anaphylaxis: mechanisms and management. Clin Exp Allergy 2008;41(7):923–938.
[38] Lieberman P. Biphasic anaphylactic reactions. Ann Allergy Asthma Immunol 2005;95(3):217–226.
[39] Resuscitation Council (UK). Emergency treatment of anaphylactic reactions. Guidelines for healthcare providers. January 2008.
[40] Simons FE. Anaphylaxis: recent advances in assessment and treatment . Journal of Allergy and Clinical Immunology 2009;124(4):625–636.
[41] Irish Medication Safety Network. Briefing document: reducing preventable harm to patients with known drug allergies. 2012.



