Shutterstock.com
- Advise patients to wash their hands well before applying eye treatment. Eyes are susceptible to infection so hand washing is particularly important;
- Ensure that patients do not touch the tip of the bottle to their eye. This is particularly important if patients are using multi-dose treatments, to help prevent infection;
- With most treatments, there is no need to use additional treatment if the normal dose is missed. If patients forget to use the product, they can use it at the next available opportunity, without using twice the amount;
- Advise patients not to drive if their vision is impaired by using the treatment. Suggest that patients test a new product before they have to drive — the blurring will usually clear after a few minutes;
- Advise patients applying multiple products to leave around 10 minutes between each application. Carmellose eye drops are usually recommended last, to help the drops stay in contact with the eye for as long as possible;
- Recommend that patients keep using eye treatments, particularly artificial tears, even if symptoms improve. This helps to prevent symptoms of dry eye disease returning;
- Recommend that patients keep eye treatments in a cool, dry place away from heat and light. This will help to ensure the treatment remains effective;
- Ensure that patients put the cap back on the treatment after use. This helps to prevent the product becoming contaminated.
Eye drops
- Recommend that patients use only one drop at a time. A second drop should be used only if the first drop misses the eye;
- Advise patients to close their eyes after applying the drops. Pressing gently on the nose at the corner of eye can help eye drops to stay in the eye for longer;
- Ensure that patients check the expiry date on their eye drops. Even multidose products usually expire between four and six weeks after being opened. This helps to reduce the risk of infection;
- Advise patients using single-dose formulations to use them immediately after opening. These formulations contain no preservatives and must be used straight away.
Eye gels
- Ensure that patients hold the tube vertically when applying gel. As with other treatments, advise patients not to touch their eye with the tip of the tube.
Eye creams and ointments
- Ensure patients know how to correctly apply more viscous substances, such as creams and gels. Eye creams and ointments should be applied in a thin line across the inside of the bottom lid;
- Advise patients to close their eyes then blink slowly after applying treatment. This will help to distribute the treatment over the surface of the eye;
- Suggest that patients use a mirror or ask for help if they struggle to apply treatment alone. Applying creams and ointments can be challenging, particularly for people with dexterity problems, such as those with rheumatoid arthritis. Some formulations, such as liposomal sprays, can be easier to apply.
- Advise patients that creams and ointments are usually most appropriate for overnight use. Except in more severe cases, creams and ointments are usually reserved for overnight use, because of potential side effects including blurred vision and irritation.
Example: Supporting a patient in applying their eye drops
You have just recommended some eye drops for a patient, but they have not used drops before.
Pharmacy technician: Would you like some advice about how to apply those drops?
Patient: Yes please, that would be really helpful.
Pharmacy technician: Ok, no problem. This is a multi-dose bottle so, once you open it, it will last six weeks and then you have to throw any remaining drops away. First, you’ll need to wash your hands and then unscrew the cap and keep it safe. You will need to put it back on after use, to help keep the drops sterile. Then, you need to tilt your head backwards. Hold the bottle of drops upside down in one hand, and use the other hand to pull your lower lid down gently, creating a pocket. Does that make sense so far?
Patient: Yes, that makes sense, thank you.
Pharmacy technician: Great. Once you are in that position, gently squeeze the bottle, releasing one drop into the pocket you have made. Repeat the process for the other eye. Then, make sure you put the cap back on and store the bottle in a cool, dry place. You can use the drops as often as you need to, up to about six times a day.
Patient: Great, thank you for all your help.
Liposomal sprays
- Advise patients that liposomal sprays can be used without removing make-up or contact lenses. Liposomal sprays are applied to closed eyes from a distance of around 10cm;
- Advise patients that liposomal sprays can last for up to six months after being opened. Patients should always check the expiry date on OTC eye treatments;
- Liposomal sprays may be useful in circumstances where patients have reduced dexterity. For example, it can be helpful if patients struggle with rheumatic problems in their hands or if they have neck or back problems — most treatments require the patient to lean back for application;
- Recommend that patients spray once or twice over closed eyes, from a distance of around 10cm. Patients should then open their eyes and blink a few times to spread the spray over the eyes.
How do liposomal sprays work?
Source: RB
Liposomal sprays contain soy lecithin, a phospholipid, which is enclosed within tiny microscopic spheres, called vesicles. Soy lecithin is an emulsifier, or ‘stabiliser’, which helps the water and oil layers of the eye to work together.
The tear film lipid layer (see ‘The structure of the tear film’, p6) is made up of two parts: a thick outer neutral layer in contact with the air, and a thinner layer made up mainly of phospholipids. If this layer is absent or not visible, there is likely to be a higher rate of tear film evaporation.
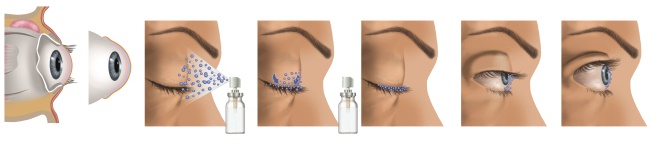
Liposomal sprays are formulated to help stabilise the tear film and increase the thickness of the lipid layer. They are applied to closed eyes, and eyes should be kept closed after application. This is designed to allow the phospholipids to settle, warm up and migrate to the edge of the eyelid. When the patient blinks, the lipids are distributed across the eye.
This is designed to mimic the natural action of the meibomian glands, which secrete lipids onto the edge of the eyelids. Blinking puts pressure on the glands, which leads to a small amount of oil mixing with the tear film. When the eyes are opened, some of the lipids form the lipid layer.
Example: Recommending a liposomal spray to a patient
Ms Smythe approaches the medicines counter. You recognise her because she sometimes collects medicines for her elderly mother.
Ms Smythe: Good afternoon. My mother’s optician recommended some artificial tears for her dry eyes, which I picked up for her last week. She has been trying to use the drops and they do help, especially when I or my brother are there to put them in for her. However, my mother has arthritis in her hands and really struggles to squeeze the bottle to put the drops in herself.
Pharmacy technician: Ok, I understand that must be difficult for her. We actually stock these liposomal sprays, which can be a useful alternative to eye drops. They are easier to apply — your mother would need to hold the spray about 10cm away from her eyes, which should be closed, and press the spray. She will then need to keep her eyes closed for a few seconds, open them and blink a couple of times. Do you think she would be able to operate the spray?
Ms Smythe: That looks like it will be much easier for her, thank you. I will get some of these and see how she gets on.



