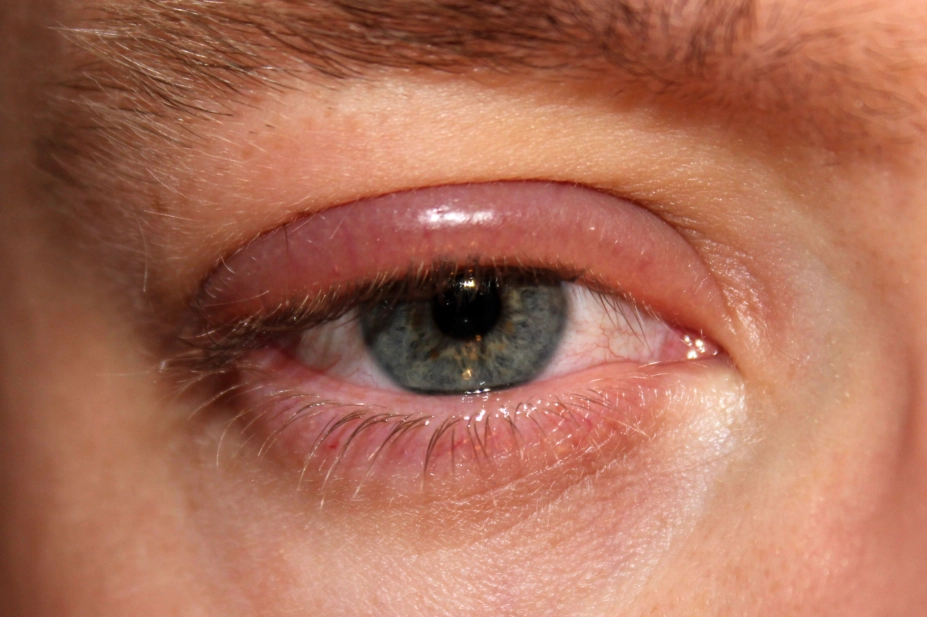
clubtable / Wikimedia Commons
Blepharitis is inflammation of the eyelid margins, which become red and swollen.
Traditional treatment for blepharitis suggests improving eyelid hygiene with the use of diluted baby shampoo. However, there is no specific guidance about how much to dilute the baby shampoo, and some patients may have an allergic reaction. Additional research also suggests that baby shampoo causes eye irritation compared with wipes, so should not be recommended to manage blepharitis. A suitable homemade solution for cleaning eyelids involves boiling a pint of water, allowing it to cool to a warm temperature and adding a teaspoon of bicarbonate of soda. This can then be used to soak cotton wool balls and cleanse the lid[1]
.
- Advise patients with blepharitis to maintain good lid hygiene. There are a wide variety of lid hygiene products available, including wipes, solutions and gels. Initially, patients should be advised to clean their eyelids twice daily. This can then be reduced as their condition improves;
- Recommend a warm compress. A warmed wet towel or eyelid-warming mask can help to improve gland function. This is usually recommended for 10 minutes twice daily, but manufacturers’ instructions for eyelid-warming masks may vary. Heat bags and eyelid-warming masks are not all as effective as one another — not all achieve the 40°C inside the eyelid required to melt the meibum. Advise patients that care should be taken not to use a hot towel, owing to the risk of scalding;
- Advise patients to perform a lid massage after a warm compress. Gently massaging the eyelid, starting at the outer corner and working towards the edge of the lid, can also help to improve gland function. This can help to push the melted oil out of the glands. Initially, this may feel a little like the patient has soap in their eyes, but should improve as the patient repeats the process;
- Suggest an anti-dandruff shampoo, if appropriate. In some patients, blepharitis is caused by seborrheic dermatitis or dandruff, which can be reduced using specialist shampoos;
- Ensure that patients are aware that continued treatment is important. Even if the patient’s condition improves, continued management is important to ensure that any improvement is maintained;
- Suggest omega-3 supplements for patients with blepharitis. Several formulations of omega-3 supplements, specifically for dry eye, are now commercially available.
If lid hygiene is ineffective, especially if there are signs of staphylococcal infection, then chloramphenicol eye ointment or drops can be prescribed for application twice daily for six weeks, although it is not available over the counter for this indication. Other antibiotic ointments or drops, including erythromycin and bacitracin, may also be prescribed. Patients will usually use these medicines for approximately four to six weeks.
- Advise patients using antibiotic drops or ointment to avoid wearing contact lenses. The drops may build up behind the contact lenses and cause irritation. The contact lenses may also be damaged by the medicines.
Low-dose oral tetracyclines and doxycyclines, which are types of antibiotic, may also be effective in meibomian gland dysfunction and blepharitis management. These medicines, which are often prescribed for patients who also have rosacea, can help to decrease the number of bacteria that can break down the tear film, as well as increase the fluidity of the oil so it flows from the glands more easily.
- Advise patients that these tablets should not be given if they have kidney problems. These antibiotics can exacerbate renal failure;
- Ensure patients are not pregnant or breastfeeding if they are taking low-dose antibiotics. These medicines can affect unborn and developing babies;
- Advise patients taking low-dose antibiotics to avoid prolonged exposure to the sun or using sunbeds. These medicines can make patients more sensitive to the effects of the sun;
- Inform patients that they may experience stomach problems when taking these medicines. Side effects are rare but can include diarrhoea and vomiting.
Example: Advising a patient taking low-dose antibiotics for blepharitis
Mr Rogers approaches the pharmacy counter with a prescription for tetracycline from his GP.
Mr Rogers: Hello again. I’ve come to collect my prescription. My GP has suggested some tablets to help with my blepharitis.
Pharmacy technician: Hi, Mr Rogers. You haven’t taken these tablets before, no?
Mr Rogers: No, I haven’t taken them before.
Pharmacy technician: Ok, it is best to avoid sun exposure as much as possible when you are taking them, because they can make you more sensitive to the sun. It is also possible, but unlikely, that you will experience some stomach discomfort, including diarrhoea or vomiting. Do you have any kidney problems at all?
Mr Rogers: No, I don’t have any other health problems at all, except a little dermatitis occasionally.
Pharmacy technician: Ok, that’s fine. I’ll just check to see if we have these tablets in stock and get them ready for you, if you’d like to take a seat.
Mr Rogers: I will do, thanks for all the information.
References
[1] NHS Choices. Blepharitis. Available at: www.nhs.uk/Conditions/Blepharitis/Pages/Treatment.aspx (accessed December 2017)



