Shutterstock.com
Development of the visual system begins prenatally and continues after birth. However, owing to how personal and subjective a person’s sight is, children may not realise they have a vision problem. Sight problems in infants can cause developmental delays, therefore, early detection and management are essential in ensuring children have the opportunity to develop the visual abilities they need to learn. Pharmacists and healthcare professionals should be aware of the stages of vision development, as well as common eye conditions that present in childhood, in order to best support, advise and refer patients when necessary.
Stages of vision development
Infancy (birth to 3 years)
A baby’s vision improves rapidly over the first few months of their life[1]
, with the ability to judge distance (depth perception) developing at around five months of age. By two years of age, a child’s hand-eye coordination and depth perception should be well developed[1]
.
Preschool (age 3–5 years)
Development of accommodative facility (ability of the eye/s to focus on stimuli at various distances and in different sequences in a given period of time), vergence ability (movement of both eyes in opposite directions to obtain or maintain single binocular vision) and eye movements continues until the child is around five years of age. Toys, games and playtime activities help this by stimulating the process of vision development. Children should have a thorough, in-person optometric eye examination at 3–5 years of age to ensure that their vision is developing properly and there is no evidence of eye disease before they begin school.
School age (age 6–18 years)
Vision changes can occur without a child or parent noticing them. To reduce the risk of this happening, children aged 6–18 years should receive an eye examination every two years, or more frequently if specific problems or risk factors exist or if recommended by an ophthalmologist
[2]
. The most common vision problem is nearsightedness (myopia); however, some children have other forms of refractive error, such as farsightedness and astigmatism. Problems with eye focusing (the ability to quickly and accurately maintain clear vision as the distance from objects changes), tracking (the ability to keep the eyes on target when looking from one object to another) and coordination may affect school and sports performance (see Box 1)[3]
.
Box 1:
Signs that may indicate vision problems in a school-age child
Parents should be advised to look out for the following signs in their child:
- Frequent eye rubbing or blinking;
- Short attention span;
- Avoidance of reading and other close-distance activities;
- Frequent headaches;
- Covering one eye;
- Tilting the head to one side;
- Holding reading materials close to their face;
- An eye turning in or out;
- Seeing double;
- Losing place when reading;
- Difficulty remembering what he or she read.
Common eye conditions
Refractive errors
Myopia (nearsightedness) occurs when the eyeball is too long, relative to the focusing power of the cornea and lens of the eye. This causes light to focus at a point in front of the retina, rather than directly on its surface. Myopia generally develops in children during their early school years and increases in severity as they get older. The age at onset is typically 7–16 years. Children may complain of headaches or need to sit closer to the whiteboard at school if they are struggling to read it.
Hyperopia or hypermetropia
(farsightedness) is when people can see distant objects very well, but have difficulty focusing on objects that are up close. Children may experience headaches and squint in order to see more clearly, and may experience difficulty reading.
Astigmatism results in blurred vision for both near and far objects because light fails to come to a single focus on the retina. Instead, multiple focus points occur in front of the retina or behind the retina, or both. Astigmatism up to 2.00 dioptres (a unit of measurement of the optical power of a lens or curved mirror; D) is common in children aged under three years. Studies show that 30–50% of infants aged under 12 months have astigmatism (≥1.00D), which declines over the first few years of life, and becomes stable by around 2.5–3 years of age. An individual with astigmatism will usually also be nearsighted or farsighted[4]
. Children may experience headaches, tired eyes and blurred vision[4]
.
Anisometropia is where the two eyes have significantly different refractive powers. Anisometropia of ≥1.00D is considered clinically significant. There is a low prevalence (4%) of anisometropia in children aged under six years; however, it has been shown to increase to nearly 6% at 12–15 years of age[5],[6]
.
Refractive errors can easily be corrected with glasses or contact lenses. Parents with children who are complaining of these symptoms should be referred to an optometrist for assessment and treatment.
Strabismus
Squint, or strabismus, is a common condition affecting around 2.1% of the population[7]
. Although strabismus can develop at any age, it usually develops during childhood. Infantile esotropia (an inward turning of one or both eyes; see Figure 1) has an onset prior to six months of age. Accommodative esotropia typically has an onset of 2–3 years of age, but can develop before 6 months of age. Young children with constant unilateral strabismus (where the misalignment always affects the same eye) often develop amblyopia and impaired stereopsis (impaired depth perception). Early identification and treatment may prevent amblyopia (lazy eye) and preserve stereopsis. Treatment options include patching (wearing an eye patch over the stronger eye), glasses and surgery to correct the muscle around the eye.
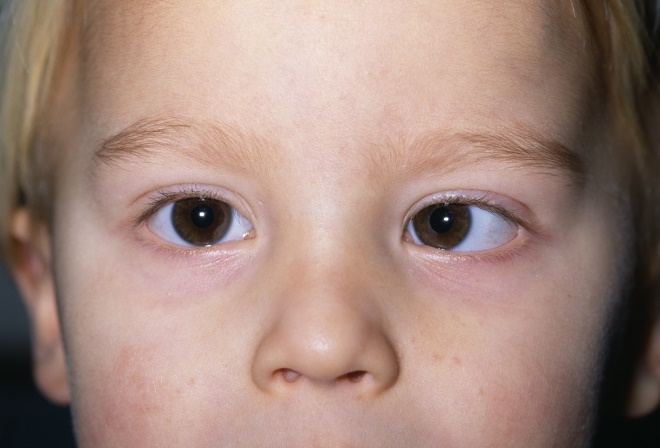
Figure 1: Strabismus
Source: Dr P. Marazzi / Science Photo Library
Infantile estropia, an inward turning of one or both eyes, has an onset prior to six months of age.
Amblyopia
Also known as lazy eye, amblyopia is a vision development disorder where an eye fails to achieve normal visual acuity, even with prescription glasses or contact lenses[8]
. The prevalence of amblyopia is estimated at 1 in 50 children[9]
. Although it is a treatable condition in both children and adults, the potential for successful treatment is better when it is diagnosed and treated early, generally during the infantile and preschool years when the visual system demonstrates greatest plasticity[8]
. Treatment includes patching, which may be required for several hours each day or even all day, and may continue for weeks or months. Patches often need to be worn with glasses[9]
.
Infective conjunctivitis
Redness and inflammation of the conjunctiva (the thin layer of tissue that covers the front of the eye) is indicative of the common condition conjunctivitis[10]
. It can be caused by viruses (e.g. common cold) or, less often, by bacteria (most commonly staphylococcal or streptococcal bacteria). Viral conjunctivitis tends to cause a watery, red eye and can last for 2–3 weeks, whereas bacterial conjunctivitis is more likely to cause a red eye with a sticky yellow discharge (see Figure 2). Conjunctivitis can affect one eye or both eyes[9]
, is often self-limiting and can be managed through self-care (see Box 2); however, some parents may notice that their child has a cold, sore throat or feels unwell at the same time.
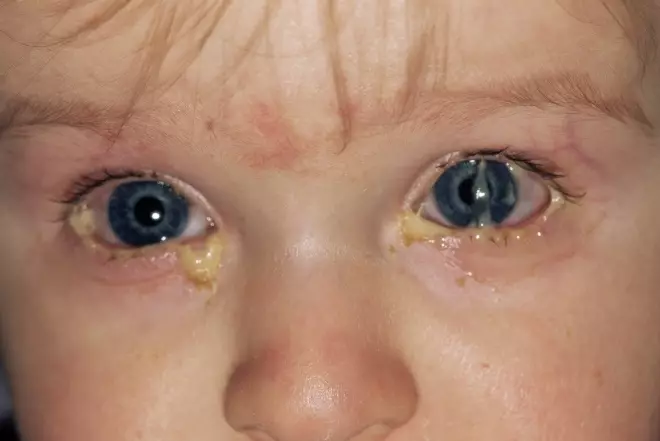
Figure 2: Bacterial conjunctivitis
Source: Dr P. Marazzi / Science Photo Library
Conjunctivitis is a common condition that causes redness and inflammation of the conjunctiva, and can be either viral or bacterial in nature.
Box 2: Self-care for infective conjunctivitis
Pharmacists and healthcare professionals should advise parents of the following to help them manage their child’s infective conjunctivitis:
- Gently clean away any sticky discharge from the eyelids and lashes using cotton wool soaked in cooled, boiled water;
- Remove contact lenses — if the patient wears contact lenses, advise them to take them out and refrain from wearing any contact lenses until all symptoms of the infection have gone. Patients must not re-use old lenses, even after the infection has gone, as they could be a potential source of reinfection; instead, used lenses should be discarded and new lenses, solutions and cases used after an infection;
- Use lubricant eye drops — these are available over-the-counter and may help ease any soreness and stickiness in the eyes. Patients should always follow the manufacturer’s instructions;
- Wash hands regularly — viral and bacterial conjunctivitis are contagious and can spread very easily.
If symptoms have not cleared up after two weeks, patients should be referred to their GP.
Source: NHS Inform. Conjunctivitis. 2018. Available at: https://www.nhsinform.scot/illnesses-and-conditions/eyes/conjunctivitis#treatment (accessed December 2018)
Patients may require antibiotics for bacterial conjunctivitis that is particularly severe (or has lasted for longer than two weeks). Chloramphenicol eye drops are usually the first-line treatment and are available without a prescription, but need to be used as per the patient information leaflet to get the best results. If chloramphenicol is not suitable, fusidic acid eye drops may be prescribed. This is often better for children as they do not need to be taken as frequently.
Babies up to one month of age with red eyes, swollen eyelids and a watery or sticky discharge from the eyes may have ophthalmia neonatorum. This is a severe infection that occurs in babies who are exposed to a sexually transmitted infection when passing through the birth canal. As this can lead to permanent eye damage, babies who display these symptoms must be referred to an eye specialist immediately for treatment[11]
.
Allergic eye disease
Children with allergic eye disease tend to have symptoms of sneezing, congestion and a runny nose, as well as itchy, red or watery eyes and swollen eyelids (see Figure 3). The pattern of symptoms will depend on the cause, for example patients allergic to grass will experience symptoms during the spring and summer, whereas those allergic to animal fur will have symptoms throughout the year. Children with mild symptoms can be managed with self-care advice (see Box 3).
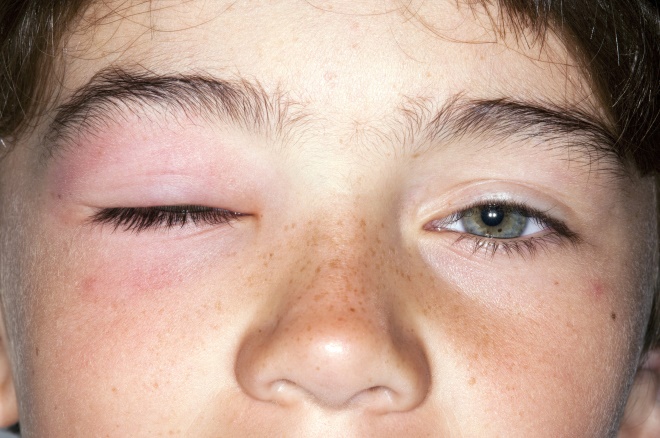
Figure 3: Allergic eye disease
Source: Dr P. Marazzi / Science Photo Library
Symptoms of allergic eye disease often include sneezing, congestion and a runny nose, swollen eyelids and itchy, red or watery eyes.
Box 3: Self-care advice for allergic eye disease
Pharmacists and healthcare professionals should advise parents of the following to help them manage the symptoms of their child’s allergy:
- Avoid the allergen — limit the exposure to common allergens the patient is sensitive to (e.g. if the patient has hay fever, they can reduce exposure to outdoor pollen and grasses by keeping house and car windows closed during days with high pollen counts);
- Remove contact lenses — avoid the build-up of allergens and other debris on lenses until signs and symptoms have gone;
- Place a cool compress over the eyes — wetting a flannel with cool water and placing it over the eyes could help to ease symptoms;
- Use over-the-counter eye drops — these should help relieve relatively mild symptoms.
Source: NHS Inform. Conjunctivitis. 2018. Available at: https://www.nhsinform.scot/illnesses-and-conditions/eyes/conjunctivitis#treatment (accessed December 2018)
If the allergy symptoms are relatively severe, or if over-the-counter eye drops are ineffective at providing relief, patients should be referred to their GP.
Retinoblastoma
A rare type of eye cancer, retinoblastoma, can affect young children (usually under five years of age)[12]
. If diagnosed early, retinoblastoma can often be successfully treated; children treated for retinoblastoma who are diagnosed at an early stage have a survival rate of more than 95%[13]
.
This disease can either affect one or both eyes. If it affects both eyes, it is usually diagnosed before the child is aged one year. If it affects one eye, it tends to be diagnosed later, usually at 2–3 years of age.
Signs and symptoms of retinoblastoma include[13]
:
- A squint;
- A change in the colour of the iris — in one eye or sometimes only in one area of the eye;
- A red or inflamed eye, even if the child does not complain of any pain;
- Poor vision — a child may not focus on faces or objects, or they may not be able to control their eye movements (this is more common when both eyes are affected); they may say that they cannot see as well as they used to;
- An unusual white reflection in the pupil — this may be apparent in photos where only the healthy eye appears red from the flash, or it may be noticed in a dark or artificially lit room (see Figure 4).

Figure 4: Retinoblastoma
Source: Shutterstock.com
Retinoblastoma may be noticed as a ‘white eye glow’, either in photographs or in an artificially lit room.
In accordance with the National Institute for Health and Care Excellence guideline ‘Suspected cancer: recognition and referral’, children with an absent red reflex should receive an urgent referral to an ophthalmologist (for an appointment within two weeks) for retinoblastoma[14]
.
Role of the pharmacist
Most babies begin life with healthy eyes and will develop their visual abilities without difficulty. However, eye health and vision problems can occasionally develop and may be difficult to notice. Pharmacists and healthcare professionals can advise patients and dispel common misconceptions around children’s vision, such as that children can only have their sight tested once they can read or that the child’s school or nursery will arrange their sight examination. They can also help advise parents on ‘red flags’ for eye and vision problems in their children. These include:
- Excessive tearing — this may indicate blocked tear ducts;
- Red or encrusted eye lids — this could be a sign of an eye infection;
- Constant eye turning — this may signal a problem with eye muscle control;
- Extreme sensitivity to light — this may indicate an elevated pressure in the eye;
- Appearance of a white pupil — this may indicate the presence of a retinoblastoma.
If babies or children have any of these symptoms, they should be referred immediately to their GP, paediatrician or optometrist.
References
[1] American Optometric Association. Infant vision: birth to 24 months of age. 2008. Available at: https://www.aoa.org/patients-and-public/good-vision-throughout-life/childrens-vision/infant-vision-birth-to-24-months-of-age#1 (accessed December 2018)
[2] NHS. Eye tests for children. 2018. Available at: https://www.nhs.uk/conditions/eye-tests-in-children/ (accessed December 2018)
[3] American Optometric Association. School-aged vision: 6 to 18 years of age. 2008. Available at: https://www.aoa.org/patients-and-public/good-vision-throughout-life/childrens-vision/school-aged-vision-6-to-18-years-of-age (accessed December 2018)
[4] Moorfields Eye Hospital. Children’s astigmatism. 2011. Available at: https://www.moorfields.nhs.uk/content/childrens-astigmatism (accessed December 2018)
[5] Abrahamsson M & Sjöstrand J. Natural history of infantile anisometropia. Br J Ophthalmol 1996;80(10):860–863. doi: 10.1136/bjo.80.10.860
[6] Afsari S, Rose KA, Gole GA et al. Prevalence of anisometropia and its association with refractive error and amblyopia in preschool children. Br J Ophthalmol 2013;97(9):1095–1099. doi: 10.1136/bjophthalmol-2012-302637
[7] The Royal College of Ophthalmologists. Guidelines for the management of strabismus in childhood. 2012. Available at: https://www.rcophth.ac.uk/wp-content/uploads/2014/12/2012-SCI-250-Guidelines-for-Management-of-Strabismus-in-Childhood-2012.pdf (accessed December 2018)
[8] Wallace DK, Repka MX, Lee KA et al; on behalf of the American Academy of Pediatric Ophthalmology/Strabismus Preferred Practice Pattern Pediatric Ophthalmology Panel. Amblyopia Preferred Practice Pattern®. Ophthalmology 2018;125(1):105–142. doi: 10.1016/j.ophtha.2017.10.008
[9] NHS Choices. Lazy eye (amblyopia). 2016. Available at: https://www.nhs.uk/conditions/lazy-eye/ (accessed December 2018)
[10] NHS Inform. Conjunctivitis. 2018. Available at: https://www.nhsinform.scot/illnesses-and-conditions/eyes/conjunctivitis#introduction (accessed December 2018)
[11] The College of Optometrists. Ophthalmia neonatorum. 2018. Available at: https://www.college-optometrists.org/guidance/clinical-management-guidelines/ophthalmia-neonatorum.html (accessed December 2018)
[12] Cancer Research UK. About retinoblastoma. 2017. Available at: https://www.cancerresearchuk.org/about-cancer/childrens-cancer/eye-cancer-retinoblastoma/about (accessed December 2018)
[13] NHS Choices. Retinoblastoma (eye cancer in children). 2016. Available at: https://www.nhs.uk/conditions/retinoblastoma/ (accessed December 2018)
[14] National Institute for Health and Care Excellence. Suspected cancer: recognition and referral. NICE guideline [NG12]. 2017. Available at: https://www.nice.org.uk/guidance/ng12 (accessed December 2018)



