Shutterstock
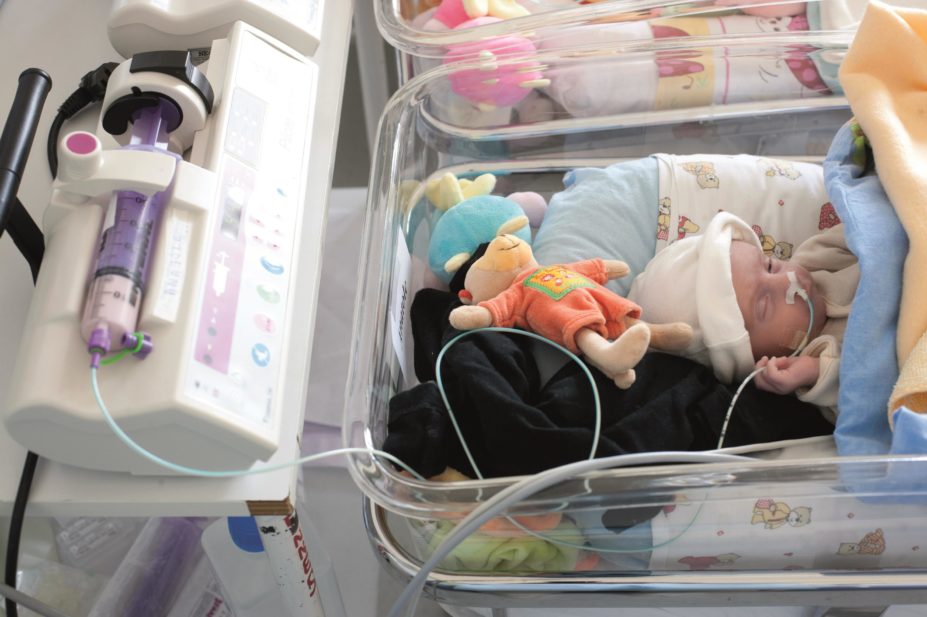
Adverse drug reactions (ADRs) are severely underreported in infants aged under two years, researchers have revealed, sparking a potential need for new ADR reporting systems.
The team, from the University of Liverpool, analysed ADRs reported through the Medicines and Healthcare products Regulatory Agency’s (MHRA) Yellow Card system involving children aged under two years between 2001 and 2010 with the aim of describing their content.
The ADR reports, which are collected by the MHRA to determine any potential safety signals, show that, with the exception of vaccinations, the number of received reports for this age group was very low and did not correlate with subsequent safety information provided by the MHRA.
The data show 3,496 suspected ADRs reported during the ten-year period – 2,673 of which were for vaccines. Only 97 reports related to neonates (babies aged under 28 days), the researchers found.
Reporting their findings in the British Journal of Clinical Pharmacology (online, 6 September 2016)[1]
, the researchers say: “Underreporting is a problem for all spontaneous ADR reporting schemes, with estimates of the frequency of underreporting are approximately 95%.”
The Yellow Card reports relate to medicine taken by the infants themselves as well as by parents at the time of conception, during pregnancy or while breastfeeding.
Medicines most commonly reported included fluoxetine taken during pregnancy or breastfeeding, swine flu vaccine given to babies under 28 days old, oseltamivir given to infants aged under two years and the meningococcal vaccine.
While the number of reports do not tally with clinical concerns raised by the MHRA, the researchers point out that reports related to drugs taken during pregnancy correlated best with MHRA guidance.
The team highlights one report of an infant who died following a BCG tuberculosis (TB) vaccination after its mother took infliximab during pregnancy, an anti-TNF drug, known to increase the risk of TB.
Subsequently, national guidance is now being updated to recommend that infants born to mothers who have taken anti-TNF agents are not given live vaccines, such as the TB vaccination, for up to seven months.
Other shortcomings identified following the analysis of the Yellow Card reports include that the age of children was given in years and gestational age was only mentioned in 1% of cases.
The researchers say efforts to boost the number of reports in this group of patients is needed, as well as new systems introduced to gather extra data.
Lead author Dan Hawcutt, a senior lecturer in paediatric clinical oncology at the University of Liverpool, points out that the Yellow Card scheme, which was set up 50 years ago in response to the thalidomide disaster, has helped improve the safety of drugs and continues to be valuable, but this may not be enough in newborn babies and infants.
“There are several alternative strategies. Active surveillance has been tried in Canada and variants of this could be used [in the UK].”
He adds that the use of sentinel sites may be the most promising option. “This is where large units with a critical mass of expertise in this area actively look for particular adverse drug reactions,” he explains.
Overall, the researchers found that doctors reported the largest number of Yellow Cards (1,445), followed by nurses (1,086), parents/carers (173) and pharmacists (138).
A spokesperson for the MHRA, which regulates pharmaceuticals and medical devices, says the Yellow Card scheme has a proven track record in identifying safety concerns, including important paediatric safety issues.
The MHRA also acknowledges that there is a variable level of underreporting and sustained effort is required to promote awareness of the scheme and encourage reporting of suspected side effects.
“We have taken forward a number of initiatives to publicise the importance of reporting side effects in children to the scheme… information on the importance of reporting paediatric ADRs is published on our website, for example,” the spokesperson explains.
“We recognise that identifying side effects in children can be difficult and the parents or carers are in the best position to identify symptoms in their child. In partnership with paediatric organisations, we promote the use of Yellow Card Scheme for parents and carers to report suspected side effects,” the MHRA spokesperson adds.
Neena Modi, president of the Royal College of Paediatrics and Child Health, comments: “This report confirms the suspicions of many clinicians that infants and [newborns] would benefit from focused attention upon their needs, in this instance adverse drug reporting.
“The existence in the UK of strong collaboration between neonatologists and paediatricians, wide use of electronic patient records and a national neonatal database holding population data could be harnessed to meet these challenges,” she adds.
References
[1] Hawcutt D, Russell N-J, Maqsood H et al. Spontaneous adverse drug reaction reports for neonates and infants in the UK 2001—2010: content and utility analysis. British Journal of Clinical Pharmacology 2016. doi: 10.1111/bcp.13067