Shutterstock.com
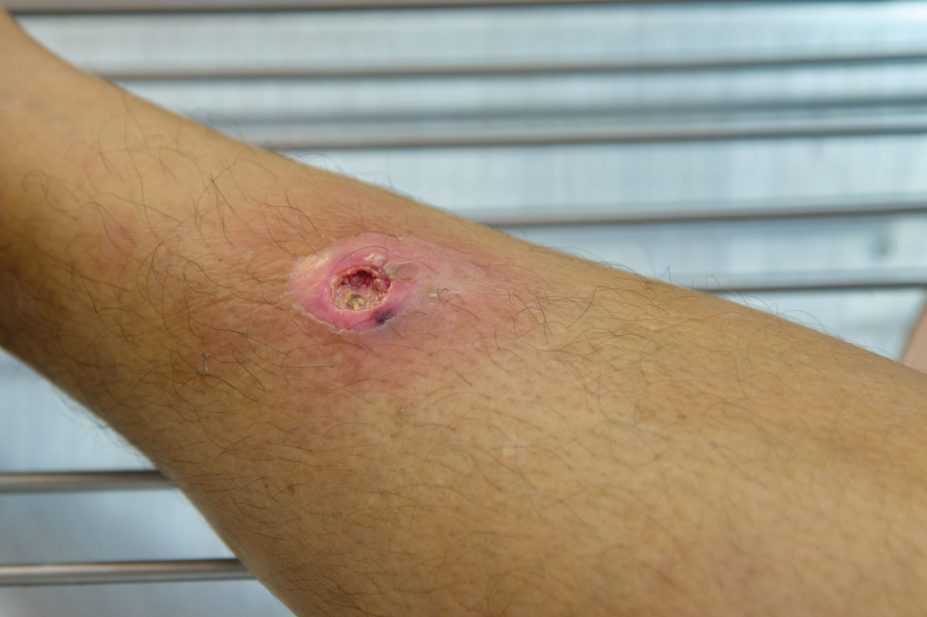
The role of antibiotics in treating small skin abscesses, including those infected with methicillin-resistant Staphylococcus aureus (MRSA), is currently unclear, with some clinicians opting to simply drain abscesses without antibiotics.
In a study published in The New England Journal of Medicine
[1]
(online, 29 June 2017), researchers randomly assigned 786 adults and children with a skin abscess 5cm or smaller in diameter to clindamycin, co-trimoxazole or placebo, following abscess incision and drainage. Half of all participants had abscesses owing to MRSA.
After 10 days, the cure rate was similar between the two antibiotic-treated groups (83.1% and 81.7%, respectively). Both of these were significantly higher than the cure rate in the placebo-treated group of 68.9%. The results were similar among patients with MRSA abscesses.
Antibiotic therapy seems to improve short-term outcomes, the study authors say, but the choice of clindamycin or co-trimoxazole should be based on a variety of factors, such as tolerability, cost and local antibiotic susceptibility patterns.
References
[1] Daum R, Miller L, Immergluck L et al. A placebo-controlled trial of antibiotics for smaller skin abscesses. N Engl J Med 2017; 376:2545-2455. doi: 10.1056/NEJMoa1607033