Sherry Young/Dreamstime
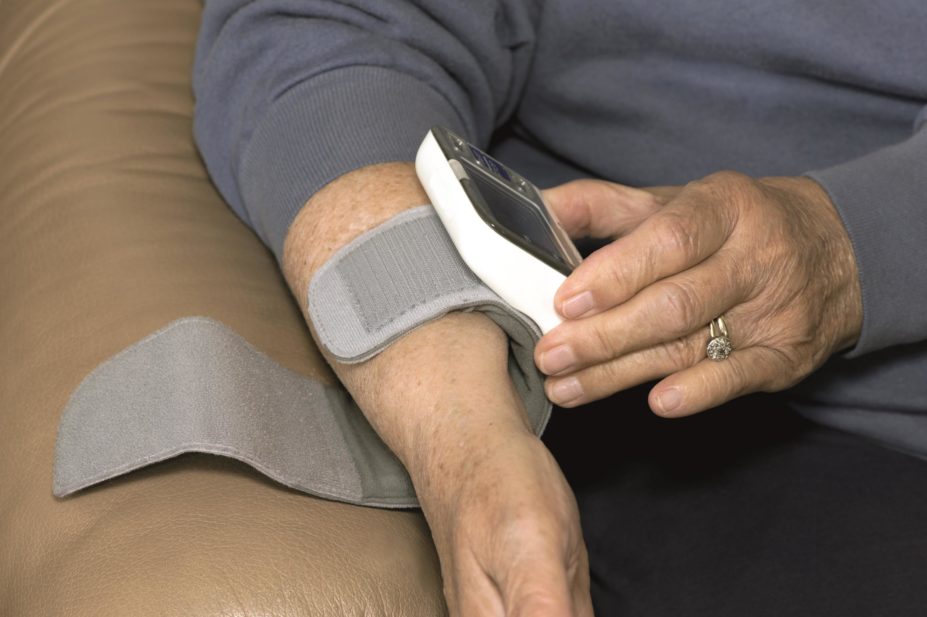
Blood pressure devices designed for use at home can give inaccurate readings for as many as 15% of users, a retrospective study suggests.
The units, used by patients with hypertension to help guide diagnosis and treatment, may fall short for in 5% to 15% of cases, depending on the threshold for accuracy needed, the research, to be presented during the American Society of Nephrology Kidney Week
[1]
on 11–16 November 2014, reveals.
The genesis for the study came in 2010 from Hypertension Canada, a not-for-profit organisation “representing expertise in the field of hypertension”, which receives pharmaceutical industry funding.
It ran the Canadian Hypertension Education Programme (CHEP) which strongly advocated that patients being treated for hypertension measure their own blood pressure in addition to a doctors’ monitoring. This meant patients needed to purchase their own monitors, which range in price from $CAD50 to $CAD100, a cost not typically covered by Canada’s universal healthcare system.
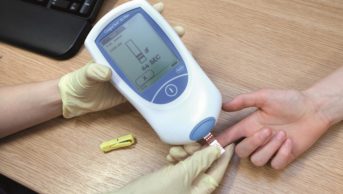
CHEP’s advice was well received, says Swapnil Hiremath, a nephrologist at Ottawa Hospital and the lead author of the study. However, says Hiremath, physicians started to hear comments from their patients that blood pressure readings taken in the doctor’s office differed from readings at home. To ensure that patients were using correct monitoring techniques — including having arms and legs in the correct positions — Ottowa Hospital created the Nephrology Blood Pressure Assessment Clinic (NBPAC) in the summer of 2011. At the clinic, a nurse provided lifestyle education and blood pressure-taking techniques to patients who brought in their own devices. Patients received two readings, one using their home-use device and the other using a clinical machine with a validated mercury sphygmomanometer.
Hiremath became aware of the alarming discrepancies in the measurements, including those from well-known brands. In spring 2014, his team analysed data from 210 patients who attended NBPAC. At the clinic, patients had their blood pressure taken with the clinic’s validated device and also with the home device each patient brought in.
Hiremath and his team used the readings from the clinic’s device as the baseline figure. For systolic blood pressure taken with the patient’s own device, the researchers found that 30% of the patient’s home devices showed variations greater than five millimetres on either side of the baseline number, and 8% showed variations greater than 10 millimetres. For diastolic blood pressure taken with the patient’s home device, 32% of the home devices showed variations greater than five millimetres on either side of the baseline number, and 9% showed variations greater than 10 millimetres.
Hiremath chose the away-from-baseline variations of greater-than-five millimetres and greater-than-10 millimetres according to how far away from baseline the measurements were. “We were surprised that, according to our figures, as many as one in ten home devices may be unreliable,” he says.
“These variations could give patients the idea their blood pressure was either being better controlled or more poorly controlled than it actually was,” says Hiremath. “Because there is the potential for overtreatment and undertreatment of hypertension, physicians, including cardiologists and family doctors, as well as nephrologists, need accurate numbers.”
Although the study’s goal was to point out measurement discrepancies, Hiremath says that the problem was compounded by consumers’ trust in the reliability of devices they buy. “People typically overestimate the technology in a machine, believing that it’s going to be accurate,” he says.
To improve the situation, NBPAC issues patients with a letter stating that their specific device gives inaccurate readings. Patients whose new monitors are faulty can take the letter to their pharmacy which may exchange the product. If the device is older, Hiremath adds, at least the patient’s healthcare provider has a baseline of discrepancy that can be taken into account and of which the patient is now aware.
Hiremath believes it may be unrealistic for retail pharmacists to devise their own informal, in-store classes to teach consumers how to use these devices correctly. However, at the very least, his research team encourages all patients with home blood pressure monitors get them validated with their health care providers at least once.
References
[1] Swapnil Hiremath, et al. Are Home Blood Pressure Monitors Accurate Compared to Validated Devices? [Presentation SA-PO187]. American Society of Nephrology Kidney Week 2014, November 11-16. (http://www.asn-online.org/abstracts/)