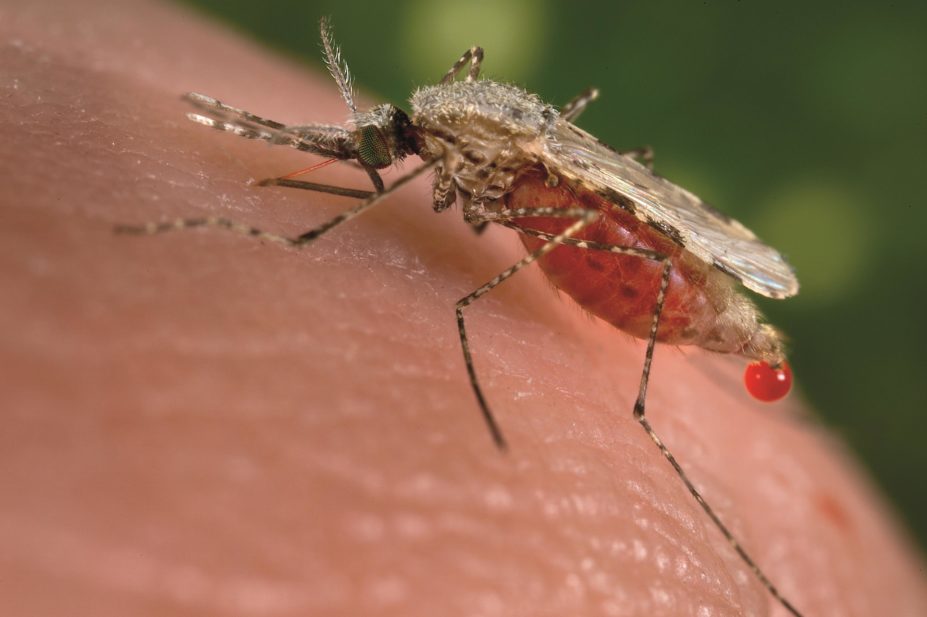
Jim Gathany / Centers for Disease Control and Prevention’s Public Health Image Library
Although malaria is currently completely treatable and preventable, paradoxically it still represents an area of unmet need. There has been significant progress in the fight against malaria, said Susan Charman, professor of pharmaceutics at Monash University at the 74th International Pharmaceutical Federation Congress in Bangkok. An estimated 3.3 billion lives have been saved since the year 2000 as a result of the widespread deployment of artemisinin-based combination therapies (ACTs), together with indoor spraying to kill mosquitoes and the use of insecticide treated bed nets.
Artemisinin derivatives used in ACTs represent extremely potent, rapid-acting, affordable treatments for malaria but recently resistance to these essential drugs has emerged in South East Asia. Multi-drug resistant forms of the Plasmodium falciparum parasite have already rendered once useful agents such as chloroquine and sulfadoxine-pyrimethamine ineffective in many parts of the world. In addition, there are compliance issues with ACTs which have to be taken once or twice daily for three days. Thus, there is an acute need for novel antimalarial agents. The Medicines for Malaria Venture (MMV), a non-profit public-private partnership, formed in 1999, has established the largest portfolio of antimalarial drugs in development ever, with the aim of bridging this gap.
Charman gave a snapshot of several antimalarial agents in the MMV portfolio at different stages of development. The drugs were discovered using a variety of approaches. The discovery and lead optimisation programme which led to the development of the new drug P218 was guided by rational design and X-ray crystallography. These techniques enabled improvements to be made to bioavailability, binding and selectivity of initial experimental compounds. In addition, side chains that were implicated in the development of resistance were identified and altered. The result was P218, a next generation dihydrofolate reductase inhibitor, which has potent activity against resistant parasite strains. The compound is currently undergoing preclinical toxicological studies in preparation for phase I studies in 2015.
In a collaborative project between the Universities of Texas, Washington, and Monash, as well as GlaxoSmithKline, the National Institutes of Health and MMV, high throughput screening of 220,000 compounds was used to identify inhibitors of the enzyme dihydrooroate dehydrogenase. This enzyme is involved in the synthesis of pyrimidines, essential to survival of the parasite. A potent lead compound emerged, however, it was highly metabolised and had poor pharmacokinetics. Lead optimisation generated DSM265: a compound with a long half-life coupled with potent and selective inhibition of parasite dihydroorotate dehydrogenase. Phase I studies in volunteers indicated that it has good safety and pharmacokinetic profiles. Phase II studies in patients are due in 2015.
Artemisinin and its derivatives all share a unique peroxide pharmacophore, which is essential for their rapid action and potent antimalarial activity. However, artemisinin-based compounds have an extremely short half-life. Charman described how medicinal chemistry, using a novel ozonolysis reaction, led to the discovery of OZ439, known as artefenomel. This is the first long half-life, synthetic peroxide and is an innovative compound since it has the potential to provide a single-dose treatment for uncomplicated malaria, thereby improving compliance. The drug is currently in phase II studies.
Collaborative partnerships
A common theme that emerged was that partnership working between academia, the (bio)pharmaceutical industry and other stakeholders can be an effective means of encouraging the development of drugs for unmet needs. The aim of these partnerships is to tackle the declining research productivity, declining number of innovative medicines and to get safe and effective medical products to patients faster and more efficiently, using partnerships that traditionally may not have been in place for drug development. Such initiatives include MMV, as well as the European Innovative Medicines Initiative, and the Global Fund to fight AIDS, Tuberculosis and Malaria.“Partnerships are key to encouraging innovation in drug discovery and development,”concluded McKinnon.
