
MikeDotta / Shutterstock.com
Vaccine development needs to be incentivised and those already available need to be administered more widely to help reduce the use of antibiotics, according to the latest report by the Review on Antimicrobial Resistance (AMR).
The report says that while it is essential to develop new antibiotics, there is no guarantee that enough will be discovered to tackle the threat of antimicrobial resistance in the long term, so other approaches to the prevention and treatment of infections are needed.
In the short term, the use of existing vaccines needs to be increased, both in humans and in animals. The use of many vaccines needs to be rolled out to low-income countries, and high and middle-income countries lacking universal coverage for large portions of the population need to address this, the report says.

Source: AMR
Universal coverage with a pneumococcal conjugate vaccine could largely prevent 800,000 deaths each year, says Jim O’Neill, chair of the Antimicrobial Resistance review
“Universal coverage with a pneumococcal conjugate vaccine, something that is already used in many parts of the world, could largely prevent the 800,000 yearly deaths of children under five caused by Streptococcus pneumoniae,” says Lord O’Neill, chair of the review. “It could also prevent over 11 million days of antibiotic use in these children, reducing the chance of resistance developing.” Similarly, diarrhoeal disease is a major cause of child mortality in developing countries and a driver of antibiotic use, both of which could be significantly improved by wider use of the rotavirus vaccine, the report says.
The AMR report says that researchers working in a variety of disciplines need to be incentivised to look for the solutions that will reduce dependence on antibiotics. It points out that there are no vaccines in use for the three “urgent” resistance threats highlighted by the US Centers for Disease Control and Prevention (CDC) – carbapenemase-producing bacteria (including Klebsiella and Escherichia coli), gonorrhoea and Clostridium difficile – and few candidates in clinical trials. The AMR has already recommended that a US$2bn five-year global innovation fund should be set up, but it adds that further sustained funding from philanthropic organisations, the public sector and companies will be needed.
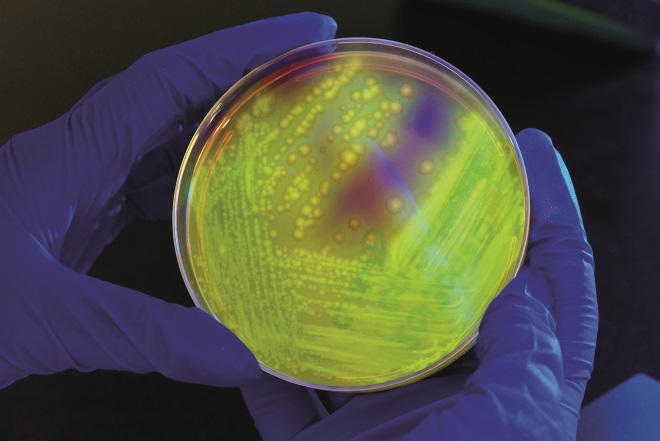
Source: James Gathany / CDC
There are no vaccines in use for three “urgent” resistance threats: carbapenemase-producing bacteria, gonorrhoea and Clostridium difficile (pictured)
Specific measures to reward vaccine developers need to be considered where research and development is not an attractive proposition, the report adds. Possible interventions have already been set out for the development of new antibiotics and diagnostics, and include advance market commitments and market entry rewards.
Jeremy Farrar, director of the Wellcome Trust, says its own analysis on the use of vaccines and other antibiotic alternatives supports the AMR report. “They will be an important way we can reduce – but not replace – our need for antibiotics.”

Source: World Economic Forum
Seth Berkley, pictured, chief executive of Gavi, the Vaccine Alliance, says: “It is exciting to see such a powerful argument on the important roles vaccines play.”
Seth Berkley, chief executive of Gavi, the Vaccine Alliance, says: “It is exciting to see such a powerful argument on the important roles vaccines play, not just in preventing diseases and therefore reducing antibiotic usage, but also in directly reducing antimicrobial resistance.”
Also commenting on the report, Jayne Lawrence, chief scientist at the Royal Pharmaceutical Society, says Lord O’Neill is right to call for alternatives to antibiotics, including vaccines.“ However, there are serious challenges to producing vaccines,” she says, adding that other approaches are needed.
“For example, treatments that are less likely to increase the likelihood of drug resistant infections such as the use of bacteriophages — viruses that infect and kill bacteria but not human cells — are attractive, as is the use of anti-viral drugs and immune-based therapies including monoclonal antibodies or white cells.”
Lawrence also points out that new approaches to the genetic modification of bacteria are also under consideration – treatments that “silence” the genes in bacteria that cause the illness or “switch off” the resistance genes in bacteria that stop antibiotics working.
“The development of these gene-specific so-called ‘antisense’ antibiotics, that directly affect the genetic make-up of bacteria, offer potential in the future battle against drug-resistant bacterial infections,” she says.
The AMR, which was set up by prime minister David Cameron, is due to make its final recommendations in May 2016, setting out a package of actions to tackle drug-resistant infections globally.


