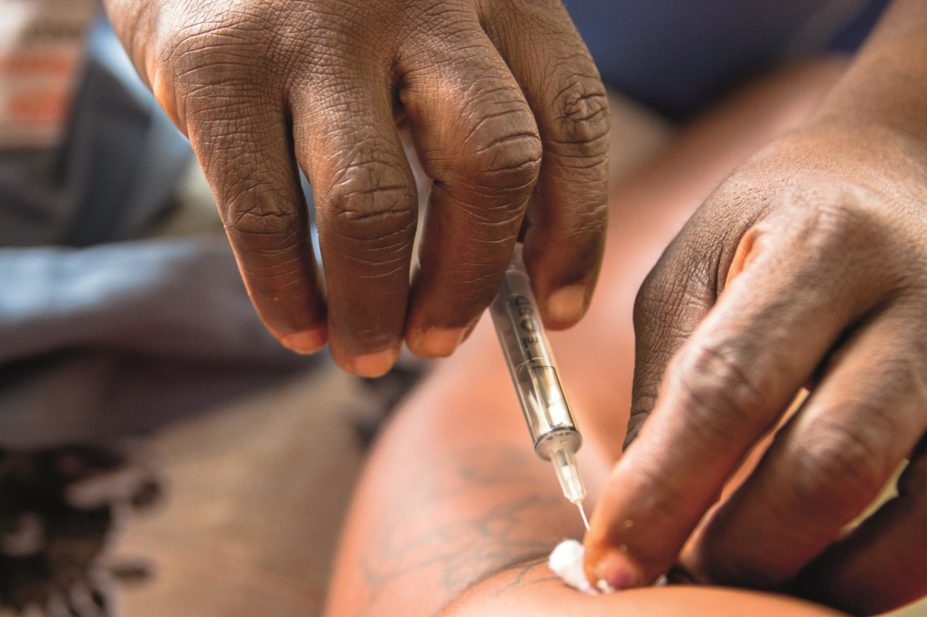
Marie Stopes International / Nana Kofi Acquah
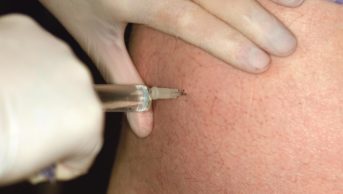
Depot medroxyprogesterone acetate (DMPA), a long acting birth control injection commonly known as Depo-Provera, is associated with a 40% increase in the risk of HIV infection in the women who receive it, a large meta-analysis[1]
has found
.
The injection protects against pregnancy for three months and is predominantly used in developing countries, particularly in resource-poor countries in sub-Saharan Africa that have a high incidence of HIV infection. It is used to a lesser extent in developed countries; in the UK it is most widely used by teenage girls.
Researchers from the University of California, Berkeley, identified published studies that had examined the effect of using the most commonly prescribed forms of hormonal contraception (combined oral contraceptives, progestogen-only pills, and the injectable contraceptives DMPA and norethisterone enanthate) on HIV risk.
Twelve studies, involving more than 39,500 women, had been published by June 2014 and met the exclusion criteria. All had been conducted in sub-Saharan Africa.
The team’s analysis of the studies’ findings, published in The Lancet Infectious Diseases, suggests that women using DMPA have a 40% greater chance of becoming infected with HIV compared with women using other contraceptive methods or no method at all (pooled hazard ratio [HR] 1.40, 95% confidence interval 1.16–1.69).
This increased risk seems to be greater in women who are sex workers, and therefore already at substantially greater risk of HIV, than in the general population. Eight of the studies looked at women in the general population and their results suggest that these women have a 31% increased risk of HIV when using DMPA (pooled HR 1·31, 95% CI 1·10–1·57).
Use of progestogen-only pills, combined oral contraceptives, or norethisterone enanthate did not seem to be associated with increased HIV risk.
The moderate elevation in risk observed “is not enough to justify a complete withdrawal of DMPA for women in the general population”, says lead author, Lauren Ralph, an epidemiologist at the University of California. “Banning DMPA would leave many women without immediate access to alternative, effective contraceptive options. This is likely to lead to more unintended pregnancies, and because childbirth remains life-threatening in many developing countries, could increase overall deaths among women.”
Whether or not use of hormonal contraceptives increases women’s risk of HIV infection has been debated for more than two decades. Worldwide around 41 million women use injectable contraceptives, including DMPA, compared with 103 million who take the oral contraceptive pill.
The latest advice from the World Health Organization in 2014 was that, while there was no need to restrict use of any hormonal contraceptives, women at high risk of HIV who are using progestogen-only injectables should be informed that some studies suggest that they “may be at increased risk of HIV acquisition”.
“Women using progestogen-only injectable contraception should be strongly advised to also always use condoms, male or female, and other HIV preventive measures,” it said.
“While modern contraceptive methods, especially long-acting reversible and permanent methods, offer the most effective protection against unintended pregnancies, barrier methods provide the best protection against STIs including HIV,” says Dhammika Perera, global medical director of Marie Stopes International, one of the organisations that provides DPMA to women in developing countries. It will continue to provide women with the option of injectable contraception, while counselling men and women that barrier methods, such as condoms, must be used in dual protection, he adds.
Limiting access to Depo-Provera, without users switching to an equally or more effective modern method such as implants or IUDs “will increase unintended pregnancies and the complications due to those unintended pregnancies”, and “will also increase HIV transmission since pregnancy itself may raise a woman’s risk of infection”, he says.
In the UK, the risk of HIV infection among the heterosexual population is low; in 2013, it is estimated that 1,500 people acquired HIV through heterosexual contact. The Faculty of Sexual and Reproductive Healthcare says there “is no reason to advise against use of DMPA even for women at ‘high risk’ of HIV infection” and also stresses the need for women at risk of HIV to use condoms.
In a statement, Pfizer, which produces Depo-Provera, said that the studies to date had been observational and that it was “not aware of any scientific evidence showing a causal association between use of hormonal contraceptives and an increase in HIV transmission rates”. It added that DPMA is an important treatment option for many women and emphasised that the only contraceptives that provide protection against HIV transmission are barrier methods.