Shutterstock.com
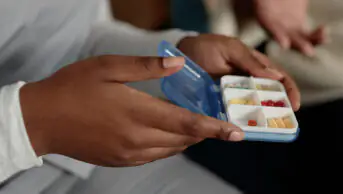
Patients with chronic obstructive pulmonary disease (COPD) are less likely to adhere to their medicines if they have depression, a new study shows.
In a cohort of 31,033 patients newly diagnosed with COPD, 20% were subsequently diagnosed with depression. The researchers found, overall, adherence to COPD medication was low, peaking at 57% in the first month post diagnosis and declining to 35% within six months. However, a diagnosis of depression was associated with a further decrease in adherence (odds ratio 0.93, 95% confidence interval 0.89–0.98). The average number of prescriptions collected per patient in a two-year period was 11.1 in the group without depression and 10.5 for those with depression (P<0.001).
COPD patients diagnosed with depression were more likely to have multiple other conditions, to be female, to have had a stay in a nursing home and to have had more severe COPD symptoms in the month of their depression diagnosis.
The data were collected from a sample of Medicare beneficiaries in the United States. Medicare is a government-run health insurance programme for people who are 65 years or older, and for younger people with certain disabilities or diseases.
Reporting their findings in Annals of the American Thoracic Society
[1]
(online, 22 June 2016), the study authors conclude that depression is undertreated and under-recognised in patients with COPD.
Anna Murphy, consultant respiratory pharmacist at University Hospitals of Leicester NHS Trust, says that although the published study was conducted in the United States, the findings are relevant to the UK. Depression is a recognised comorbidity of people with COPD, with previous studies estimating prevalence at between 17–44%. “All healthcare professionals supporting people with COPD should have awareness of anxiety and depression and refer or screen as appropriate,” says Murphy.
She points out that “it is interesting…that a higher percentage of beneficiaries with depression also had associated dementia, which has been also shown to reduce medication adherence rates, potentially affecting the validity of the results”.
However, adherence was sub-optimal even in patients without depression, which is, says Murphy, “a message to us all to ensure we discuss medicines use with patients, optimise inhaler technique and be aware of non-adherence affecting clinical outcomes”.
Mike McKevitt, head of patient services at the British Lung Foundation, says: “This paper highlights the impact of what we know anecdotally, that people who have become depressed find it harder to manage their condition.
“With COPD it is very important that people adhere to their treatment plans. Pulmonary Rehabilitation, support groups and talking to mental health professionals can all help to prevent depression and reduce anxiety with COPD,” he adds.
References
[1] Albrecht JS, Park Y, Hur P et al. Adherence to maintenance medications among older adults with chronic obstructive pulmonary disease: The role of depression. Annals of the American Thoracic Society 2016. doi: 10.1513/AnnalsATS.201602-136OC