Courtesy of the Office of Lord Jim O’Neill
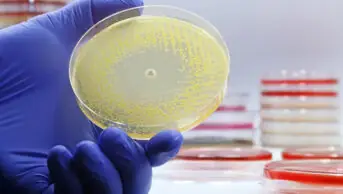
Diagnostics are central to tackling antimicrobial resistance (AMR), agreed expert witnesses giving evidence to the House of Commons health and social care committee inquiry into progress on tackling the problem.
Lord Jim O’Neill, economist and former treasury minister, said that although there has been “lots of talking”, very little progress had been made in the area of diagnostics. O’Neill was appointed in 2014 by then prime minister, David Cameron, to lead an independent review into how to drive the development of new antibiotics.
“When I am asked what is the single most important intervention that would make a huge difference? It would be diagnostics — I think about it in terms of supply and demand,” he told MPs on 4 September 2018.
“We can get all the new drugs we want, but that will only work for a while until they become resistant — we need to permanently reduce the demand — particularly the inappropriate demand.”
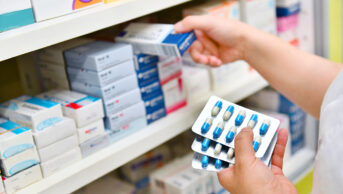
Luciana Berger, Labour Party MP and committee member, asked the panel whether commissioning diagnostic testing in community pharmacies would be achievable and, if so, what resources would be required to ensure delivery.
O’Neill referred to a July 2016 trial of a ‘test and treat’ service for group A Streptococcus in Boots pharmacies in parts of London and Leicestershire. “I gather that’s no longer taking place because the cost per unit is too high relative to getting a pill, but from the early results I saw in terms of how many people stopped going to waste a doctors time, the results were highly encouraging,” he said.
“This is exactly why I believe it should be embedded at the core of every part of healthcare provision.”
Dame Sally Davies, chief medical officer for England, said that she agreed with O’Neill on the importance of diagnostics in tackling AMR.
“Better diagnosis is clearly part of the answer; whether it’s a lab test or an algorithm, I want to see much more use of diagnostics,” she told the committee.
But she said that there may be some doubt over the role of pharmacists in using algorithms as a diagnostic tool.
“Algorithms are pretty effective in general practice, but you might not want a pharmacist doing it — although I don’t see why a good pharmacist, a well-trained one, shouldn’t.”
O’Neill said that with the announcement of additional government funding for the health budget it would be the “perfect time” to devote “a lot of that” to diagnostics.
He said that the time and cost savings that could be made with state-of-the-art diagnostics would be “enormous”.
“My suggestion is that there should be a thorough survey or analysis done of what could be the system wide benefits of introducing state of the art diagnostics.”
He referred to his 2016 AMR review, which stated that, “by 2020, all antibiotic prescriptions will need to be informed by up-to-date surveillance information and a rapid diagnostic test wherever one exists”.
Davies also said that money needed to be spent on preventing infection by way of hand-washing and vaccines, as well as education, and that Public Health England planned to repeat its awareness campaign on antibiotics in autumn 2018.
But she added that “one of the more scary bits” of the threat of AMR was the development of new antimicrobials.
“We don’t pay enough for antibiotics that they’re looked after carefully and that also means we’re not getting new ones through,” she said.
“Pharmaceutical companies have been working with the Department [of Health and Social Care] — and there is now a proposal for a pilot of two early antibiotics to see if we can manage one of these — but this will need some resource, so we come back to resourcing being important.
“You won’t solve this from the [Department of Health and Social Care’s] budget — this is a wicked problem that is cross-sectoral and it will have to be solved with treasury funding, and no country can do it on its own.”