Shutterstock.com
Providing long-acting reversible contraceptives (LARCs) free to teenagers substantially reduces rates of unwanted pregnancy, birth and abortion, according to a US study.
The research, published in The New England Journal of Medicine
[1]
, shows that pregnancy, birth and abortion rates among study participants aged 15–19 years were reduced by 79%, 79% and 77%, respectively, when compared with nationally observed rates in the United States.
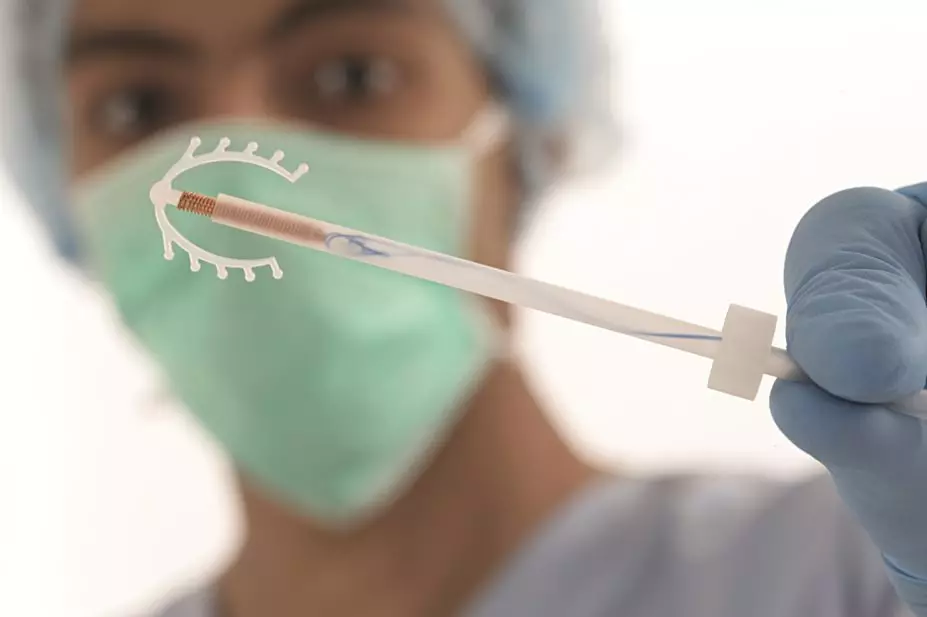
More than 9,000 women aged 14–45 years were enrolled in a contraceptive project in the St Louis area of Missouri, which was designed to promote the use of LARCs — intrauterine devices and implants — in order to reduce unintended pregnancies. Of the participants, 1,404 were aged 15–19 years.
Participants received standardised counselling on available LARC methods, including information on their relative effectiveness and their potential side effects, risks and benefits. After counselling, 72% of the teenage girls chose to use a LARC and they were monitored for 2–3 years during the study period from 2008 to 2013.
The researchers found the teenagers continued to use LARC methods for longer than short-acting methods. Two thirds were still using their LARC method after 24 months compared with only one third using a non-LARC method.
“Although the rate of LARC use among teens aged 15–19 years in the United States has increased from less than 1% in 2002 to almost 5% in 2009, our study suggests that it is possible to achieve a much greater rate of use,” the researchers say.
Hilary Pannack, chief executive officer of the UK teenage pregnancy charity Straight Talking, said that similar methods had been tried in Britain and that teenage pregnancy rates had fallen. However, she could not say that the reduction was connected to LARC use. Pannack also expressed concern that such methods could potentially “have pushed up the rates of sexually transmitted infections, which are already too high”.
According to Straight Talking, there is no “one quick fix” to bring down the rates of teenage pregnancy.
“Certainly, good, safe contraception and education will stop some risky behaviour but we also need to be telling young people the consequences of unprotected sex … and helping them to have self respect — and that means the boys as well as the girls,” Pannack said.
Debbie Mennim, head of nursing at Brook, the UK young people’s sexual health charity, agreed that LARCs were highly effective in reducing unplanned pregnancy but that it was empowering young people to make informed decisions about their contraceptive options, including but not limited to LARCs, that led to greatly improved health and well-being outcomes.
“Young people’s right to choose freely the method of contraception which works best for them must always be preserved,” she said.
Pharmacists should use every opportunity to give advice to young women to ensure that they are aware of the full range of contraception options, advises Jane Bass, a spokesperson on woman’s health for the Royal Pharmaceutical Society.
“Many [teenagers] are unaware of LARCs and so do not request one when asking for contraception,” she says. “The counselling given in this study, describing contraceptive methods from the most to the least effective, persuaded the majority of participants to use a LARC.”
The National Institute for Health and Care Excellence (NICE) guidance on LARCs encourages the use of intrauterine devices (IUD), the progesterone-containing intrauterine system (IUS) and implants for adolescents, but Depo-Provera (medroxyprogesterone acetate) should only be used in this group if other methods cannot, Bass added.
Kate Guthrie, a fellow of the Faculty of Sexual and Reproductive Healthcare at the Royal College of Obstetricians and Gynaecologists, described the study as remarkable. “It’s evidence that LARC is as good as NICE says it is,” she said.