Mariona Ribó
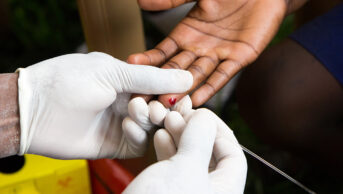
Safeguarding patients against the risk of bleeding and the management of polypharmacy are vital roles for pharmacists when dealing with patients taking new oral anticoagulants (NOACs), according to speakers at a satellite symposium that took place during the 20th annual congress of the European Association of Hospital Pharmacists in Hamburg on 25–27 March 2015.
“This is a place where pharmacists can help physicians, especially with concomitant medication,” said Peter Verhamme, of the Centre for Molecular and Vascular Biology at the University of Leuven, Belgium.
The risk of bleeding and the lack of an antidote can be a barrier to the use of NOACs.
Vitamin K antagonists (VKAs) are associated with bleeding complications in 4–7% of patients, with a case fatality rate of 20%. Intracranial bleeding is a particular problem with VKAs, explained Verhamme. Risk assessment, using the HAS-BLED score, enables clinicians to reduce the risk, he added.
Pooled results from studies that compared NOACs with VKAs for the prevention of stroke in patients with non-valvular atrial fibrillation (AF) showed that the overall risk of bleeding was reduced with NOACs. The risk of intracranial bleeding was markedly reduced but the risk of gastrointestinal bleeding was increased.
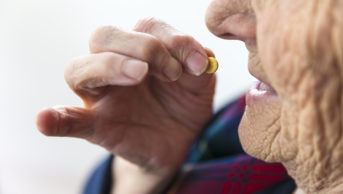
One explanation for this observation could be that patients with AF tend to be frail and are sensitive to the effects of anticoagulants. Frail patients have a three-fold greater risk of bleeding with enoxaparin plus VKA treatment than with rivaroxaban and are therefore likely to benefit most from treatment with NOACs, he noted. In future, as more elderly patients are treated with NOACs, the absolute numbers of patients who experience bleeding is likely to increase, he warned.
An audience poll showed that fewer than 40% of symposium attendees had hospital-wide policies for the management of bleeding with NOACs in their hospitals. Verhamme advised the audience members to go back to their hospitals and campaign for such a policy. “Not all doctors are specialists in anticoagulation and you should help them,” he said.
The management of bleeding involves assessing the patient and checking the time of the last dose because in 24 hours the pharmacodynamic effects of NOACs will be over. Concomitant antiplatelet agents or non-steroidal anti-inflammatory drugs will increase the risk of bleeding, he emphasised.
For minor bleeds, the main message is not to stop taking the anticoagulant. “In these patients we prioritise stroke prevention over nuisance bleeds,” he said. It is also important to review concomitant medication in case changes can be made, he added.
For major bleeds, fluid resuscitation is essential and it may be necessary to give a transfusion of packed cells or platelets, or administer tranexamic acid if the bleed is trauma-related.
For life-threatening bleeds, prothrombin complex concentrate (PCC), activated prothrombin complex concentrate (aPCC) or activated Factor VII can be given.
Reversal agents for NOACS are currently being investigated. These include idarucizumab, a reversal agent for dabigatran etextilate, andexanet alfa, a decoy Factor X that neutralises anti-Factor Xa activity and aripazine, a reversal agent for all NOACs.