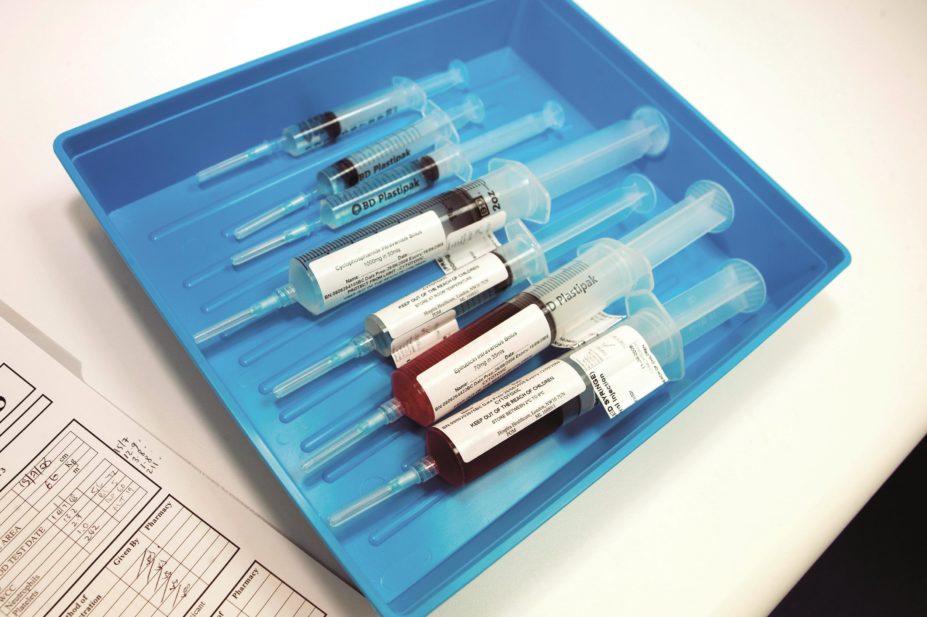
Alan Holden / Alamy Stock Photo
The National Institute for Health and Care Excellence (NICE) has revealed that, where there is insufficient evidence to support routine use, it will no longer recommend the use of a cancer drug as part of a clinical trial. Instead, the drug will be placed on the Cancer Drugs Fund (CDF) list.
“There won’t be an ‘only-in-research’ category as well as the CDF as far as I am aware,” Gillian Leng, deputy chief executive of NICE, told Westminster Health Forum’s keynote seminar, ‘Next steps for NICE, priorities for the pharmaceutical industry, and the Accelerated Access Review’, in London on 14 January 2016.
Under NICE’s proposals for the CDF, unveiled in November 2015, there will be three directions a decision on a cancer drug can take: if the appraisal committee considers a drug cost effective it will be approved for routine commissioning; if considered not cost effective it will be rejected; and if there is not enough evidence for a cost-effectiveness decision to be made, the drug will be placed in the CDF. Drugs in the CDF will be funded for a certain number of patients and data collected for two years. The drug will then be taken out of the fund and either recommended for routine NHS use or not.
“The real issue with the ‘only-in-research’ recommendations is that no one took up the research,” Meindert Boysen, programme director of technology appraisals at NICE, added at the seminar. “The Cancer Drugs Fund allows that research to be done.” Currently, around 5% of NICE’s recommendations are made on an ‘only-in-research’ basis.
Boysen added that data collection through systems such as the systemic anti-cancer therapy dataset (SACT) were now in place for the benefit of patients. SACT collates data from patients receiving cancer chemotherapy in or funded by the NHS in England.
However, Deborah Flanagan, associate director of market access and reimbursement at Gilead Sciences, warned: “We still don’t really have great data from SACT.”

Courtesy of Karl Claxton
Proposals are a major threat to evidence-based medicine, according to Karl Claxton, an economist at the University of York
Karl Claxton, an economist at the University of York, added that NICE’s proposals would incentivise manufacturers to provide as little evidence as possible at launch and to price their products as high as possible.
“All manufacturers can expect the [CDF] budget to be exceeded and you don’t want to be the one taking the biggest haircut,” he said. “The only way you can ensure that is to make sure your prices are as high as possible and that you get the lion’s share of what funds are available.”
But, Claxton emphasised, “the real threat of these proposals is the faith in what is called ‘real-world’ data. In the case of the CDF what that actually means is drug registries – observational data with no controls”.
He added that using ‘real-world’ data meant ignoring the basic principles of clinical epidemiology. “We are ignoring Nobel prizewinning research on how to analyse observational data,” he said. “These proposals are a major threat to evidence-based medicine and a bigger threat to patient outcomes in the long run. We will not know what works and what doesn’t work and we will never have the opportunity to find out by doing decent experimental research once these products are in widespread use,” he added.
Asked whether the CDF could be rolled out to other categories of medicines, Leng said that while she did not have “a crystal ball”, she hinted that it might make sense.
“We all know that the [CDF] has been criticised over the years because of its focus on cancer and the inequities that raises, so it could be potentially rolled out [to other categories of medicine],” she said.
Claxton said hat every new drug approved for use on the NHS was detrimental to the overall care that the NHS could offer. This was because NICE tends to recommend technologies with a cost per quality adjusted life year (QALY) of above £30,000 whereas other NHS care costs £13,000 per QALY[1]
.
“When NICE approves a new technology it does more harm than good – the ratio of harm to benefit is at least 3:1,” he claimed. “The CDF has been a real lesson. In terms of the ratio of harm to benefit we are looking at at least 5:1.”
References
[1] Claxton K, Martin S, Soares M, et al. Methods for the estimation of the NICE cost effectiveness threshold. Health Technol Assess J February 2015. doi:10.3310/hta19140.


