RPS
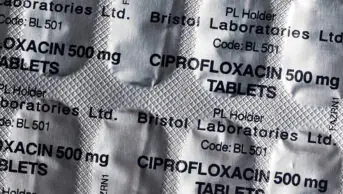
Policy makers, educators and doctors need to stop advocating “complete the course” when it comes to antibiotics, UK experts have urged, saying that the “deeply embedded” link between stopping antibiotic treatment early and antibiotic resistance is not supported by hard evidence.
An analysis in the British Medical Journal by UK experts in infectious diseases, microbiology and health psychology, who are working to tackle antimicrobial resistance, recommends that, outside hospital, where repeated testing is not feasible, patients should be advised to stop antibiotic treatment as soon as they feel better.
The analysis highlighted that when a patient takes antibiotics, antibiotic sensitive species and strains present among commensal flora on their skin or gut or in the environment are replaced by resistant species and strains ready to cause infection in the future[1]
. The longer the antibiotic exposure these bacteria are subjected to, the greater the pressure to select for antibiotic resistance.
And it concluded that: “for the opportunist pathogens for which antimicrobial resistance poses the greatest threat, no clinical trials have shown increased risk of resistance among patients taking shorter treatments”.
Kieran Hand, consultant anti-infectives pharmacist at Southampton General Hospital and a spokesperson for the Royal Pharmaceutical Society (RPS) on antimicrobial topics, described the article as a welcome opening of the debate in the UK on the relationship between antibiotic course length, and efficacy and resistance.
“The authors have sown the seed of suspicion that the ‘finish the course’ mantra does not stand up to scientific scrutiny but they have quite rightly pointed out that further research is needed before an alternative message such as ‘stop when you feel better’ can be confidently advocated,” he said.
“The focus of this article is on patient behaviour but health professionals in hospitals must be reassured that if a diagnosis of infection is excluded based on the results of diagnostic tests, then it is also not necessary to finish the course of antibiotics and the prescription should be cancelled.”
Phil Howard, consultant antimicrobial pharmacist at Leeds Teaching Hospitals NHS Trust and also an RPS spokesperson, said that clear information needed to be given to ensure that patients were not left confused about their recommended course of treatment.
“Any implementation in a change of national guidance needs to be explicit on the information given to patients by pharmacists dispensing antibiotic prescriptions, but more importantly to ensure that any leftover antibiotics are returned to a pharmacy for destruction, and not re-used for new infections by the patient or others,” he said.
Nicholas Reid, Public Health Wales’s all-Wales consultant antimicrobial pharmacist, questioned how it was possible to define ‘feeling better’ as each infection and each patients’ response to infection, is different.
“If we take a simple urinary tract infection as an example, a three-day course will achieve microbiological cure if the causative organism is susceptible, but symptoms can take up to seven days to resolve due to an aseptic inflammatory response, so in this case, stopping when feeling better would result in seven days treatment, four of which were unnecessary,” he said.
Instead he said that the message that needed to be emphasised was that under treatment leaded to treatment failure, but over or unnecessary treatment leaded to resistance.
“Rather than trying to change patient perceptions around completing the course … more work is required around defining appropriate minimum course lengths, and this can then be used to inform prescribers,” he added.
World Health Organization advice, published in 2016, advised patients to “always complete the full prescription, even if you feel better, because stopping treatment early promotes the growth of drug-resistant bacteria”.
The authors of the BMJ paper say that research is needed to determine the most appropriate messages to give patients when prescribing them antibiotics but that, above all, antibiotics should be recognised as “a precious and finite nature resource that should be conserved”.
Helen Stokes-Lampard, chair of the Royal College of GPs said it was important that patients did not change their behaviour on the basis of one study.
“Resistance to antibiotics is one of the biggest health challenges we face globally,” she said.
“It’s important that we take on board new evidence around how to curb this — but we cannot advocate widespread behaviour change on the results of just one study.
“GPs and our teams are playing a huge part in curbing the trend for overuse of antibiotics, and will prescribe in accordance with clinical guidelines, and act in the best interests of the patient in front of us,” she said
In primary care, strategies such as point-of-care tests and delayed prescriptions have been developed to help avoid unnecessary antibiotic courses being started. In secondary care, strategies to reduce overuse involve changing or stopping antibiotics 48–72 hours after they have been started. However, as the analysis points out, this is challenging to implement owing to diagnostic uncertainty and concerns around the risk of incomplete treatments.
References
[1] Llewelyn M, Fitzpatrick J, Darwin E et al. The antibiotic course has had its day. BMJ 2017;358:j3418. doi: 10.1136/bmj.j3418