Shutterstock.com
Open access article
The Royal Pharmaceutical Society has made this article free to access in order to help healthcare professionals stay informed about an issue of national importance.
To learn more about coronavirus, please visit: https://www.rpharms.com/resources/pharmacy-guides/wuhan-novel-coronavirus
Source: Shutterstock.com
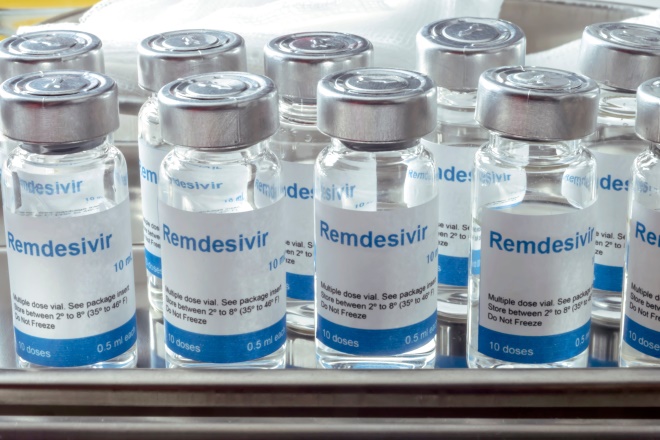
The researchers noted that the study was not a test of the efficacy of remdesivir in treating COVID-19, owing to the lack of a placebo
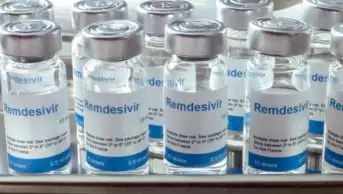
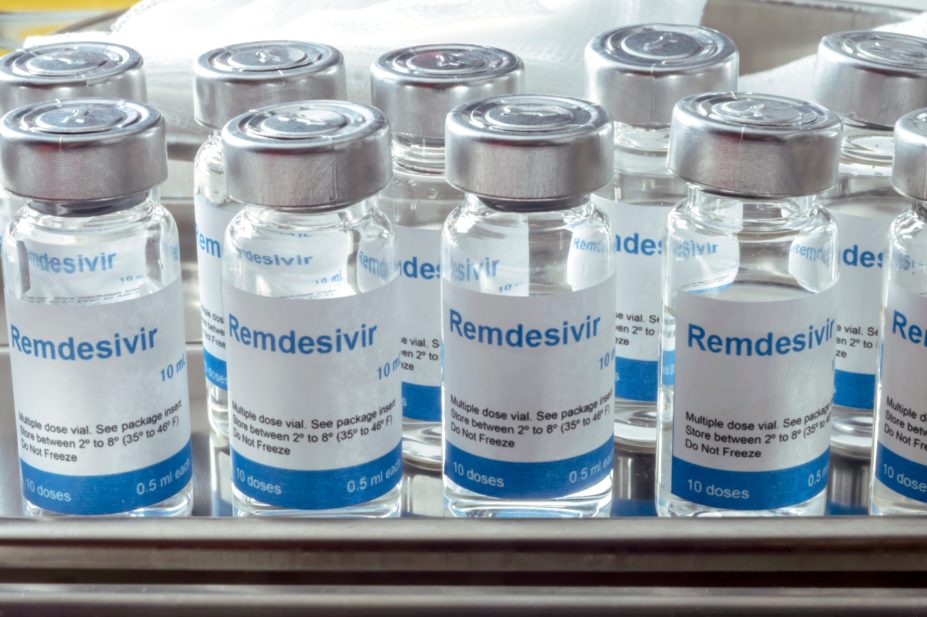
There is no significant difference in efficacy between five-day and ten-day courses of the antiviral remdesivir for patients with severe COVID-19 not requiring ventilation, research published in The New England Journal of Medicine has shown (27 May 2020)[1]
.
In an open-label, multicentre, phase III trial, 200 patients were randomised to receive treatment for five days and 197 were randomised to receive treatment for ten days. At baseline, those assigned to the ten-day group had a significantly worse clinical status than the other group.
By day 14, a clinical improvement of 2 points or more on a 7-point ordinal scale was observed in 64% of the five-day patients and 54% of the ten-day patients. After adjusting for the baseline clinical status, the researchers concluded that patients in both groups had a similar distribution in clinical status.
Owing to the lack of a placebo, the researchers pointed out that the study was not a test of the efficacy of remdesivir in treating COVID-19. However, they said that the results suggested that, if remdesivir was an active agent, supplies that are likely to be limited could be conserved with shorter durations of therapy.
“Patients who progress to mechanical ventilation may benefit from ten days of remdesivir treatment; further evaluation of this subgroup and of other high-risk groups … is needed to determine the shortest effective duration of therapy,” they added.
References
[1] Goldman J, Lye D, Hui D et al. NEJM 2020. doi: 10.1056/NEJMoa2015301
You may also be interested in
Paxlovid speeds COVID-19 recovery but does not reduce hospital admissions

Antivirals have little effect on mortality in patients hospitalised with COVID-19, suggest WHO trial interim results