Shutterstock.com
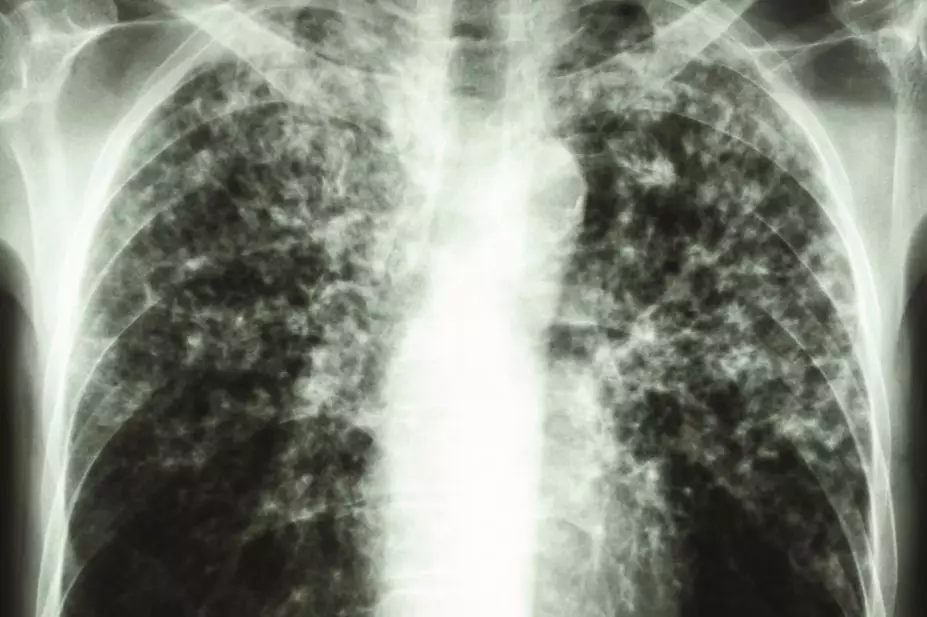
The challenges associated with access to paediatric medicines for tuberculosis (TB) were highlighted by Lisa Hedman, from the Department of Essential Medicines and Health Products at the World Health Organization (WHO), who gave a presentation on 3 September 2014 at the 74th International Pharmaceutical Federation Congress in Bangkok.
There are around 8.6 million cases of TB globally, with paediatric cases representing an estimated 6% of these in 2012, equal to approximately 530,000 children. However, accurate figures for paediatric disease prevalence are difficult to ascertain. One of the reasons for this is the challenge of acquiring suitable sputum samples from children to enable a diagnosis to be made. Multidrug resistant TB accounts for about 3.6% of cases. The majority of patients are in South East Asia, specifically in China and India, and a quarter of cases are found in Africa.
When TB recently re-emerged as a global problem, drugs went back on the market based on authorisations that had been given in the 1950s and 1960s. However, the appropriateness of the paediatric dosing had not been established, Hedman told delegates. In 2010, following a US study that indicated that doses for children required a higher dose per kilogram of body weight, WHO changed paediatric treatment guidelines. However, manufacturers did not respond by developing corresponding first-line formulations for children. This led to first- and second-line treatments that were not adapted for paediatric requirements.
There are at least four drugs for first-line therapy and more for second-line therapy. A large proportion of children are co-infected with HIV. To minimise the number of tablets that children are required to take and increase compliance, TB drugs should be formulated as fixed dose combination preparations. Such products are available for adults, but the ratios of ingredients are not appropriate for children, who require higher doses of isoniazid per kilogram of body weight. Therefore, ad hoc extemporaneous dosing using adult preparations, by splitting tablets not designed for this purpose — for example, into thirds or sixths — is common practice. This will affect both compliance and the accuracy of dosing, Hedman pointed out. Paediatric treatment guidelines have now been in place for four years, but there is currently no drug available that corresponds to them. The clinical consequences of this are likely to be the development of multidrug resistant strains of TB but this is difficult to quantify, especially when basic data, such as the number of children requiring treatment, is lacking.
Each country affected will require access to drugs to treat TB, thus there is not so much a global market as lots of national markets. As a result, markets for paediatric formulations are often small and fragmented across many countries, making them difficult to sustain. In the case of paediatric TB, the lack of treatment options is acute and could ultimately be contributing to cases of drug resistant TB, she said. The goal of the Speeding treatments to end paediatric tuberculosis (STEP–TB) initiative is to increase global access to safe, properly dosed, child-friendly formulations of current first-line TB drugs. The project was initiated in July 2013 by the TB alliance and WHO, with funding from UNITAID and USAID. Other similar programmes will be needed to ensure sustainable access to paediatric formulations, Hedman concluded.
