Shutterstock.com
Personalised telephone advice from a pharmacist can improve medication adherence in patients with long-term conditions, research shows.
The study is thought to be the first of its kind to measure the impact of telephone-based pharmacy interventions by a mail order pharmacy on patients taking medication for chronic conditions. The report, published in BMJ Quality and Safety
[1]
, is the result of a three-year, randomised controlled trial.
“People want [to have] a conversation with their pharmacist, but often don’t get it,” says Theo Raynor, professor of pharmacy practice at the University of Leeds and a co-supervisor of the study. The research has shown that telephone support is feasible, he adds.
Researchers recruited 677 patients taking medication for type 2 diabetes or high cholesterol. Around half (340) of the patients were offered the intervention: two tailored telephone conversations with a pharmacist, four to six weeks apart, with a written summary of the discussion alongside a medicines reminder chart. The control group were offered their existing dispensing service from Pharmacy2U: ordering prescribed medication online or by phone and having prescriptions delivered by post.
The researchers found that the intervention group were significantly more likely than the control group to be adherent to their medication: 36 out of the 340 patients (10.6%) in the intervention group were non-adherent (less than 90% of medication taken in the past week) at six months compared with 66 out of 337 patients (19.6%) in the control group.
The improved adherence was also evident six months after the pharmacist intervention was completed.

By talking to patients, pharmacists can help alleviate concerns over side effects, says Theo Raynor, professor of pharmacy practice at the University of Leeds
“There is more research to be done on clinical outcomes, but I don’t think we should wait for that,” says Raynor. “It’s time we actually starting doing this across the country as a matter of course.”
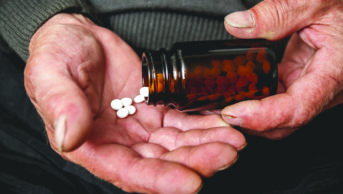
He says the first consultation takes about 15 minutes on average, with follow up being around five minutes, adding that innovators can get “bogged down” in the use of apps and smartphones at the expense of the telephone. “This is a good and simple tool and one that works especially well with elderly patients, who are more likely to need help with their multiple medications but less likely to have access to apps.”
Raynor concedes that pharmacists cannot solve all the problems of non-adherence. “What this study shows is that by talking to patients we can help alleviate concerns over side effects or administration, as well as just helping them to remember. What we can do is minimise the problem – and this tailored conversation is an ideal way of doing that.”
Carmel Hughes, professor of primary care pharmacy at Queen’s University in Belfast, who was not involved in the study, agrees that simple interventions such as telephone support are “a real advantage”.
“The value of a conversation should not be underestimated,” she says. “[The trial] has also used more than one measure of adherence (i.e. not just relied on self-report, which is subject to bias), and there are some positive clinical trends. It would be interesting to know if this intervention is transferable to other conditions.”
The study was co-funded by Pharmacy2U – the UK’s largest online pharmacy – and the UCL School of Pharmacy.
References
[1] Lyons I, Barber N, Raynor DK et al. The Medicines Advice Service Evaluation (MASE): a randomised controlled trial of a pharmacist-led telephone based intervention designed to improve medication adherence. BMJ Qual Saf 2016. doi: 10.1136/bmjqs-2015-004670