CJ Hutchinson / Alamy Stock Photo
The use of pill organisers by older people could increase the risk of drug-related adverse events, say researchers.
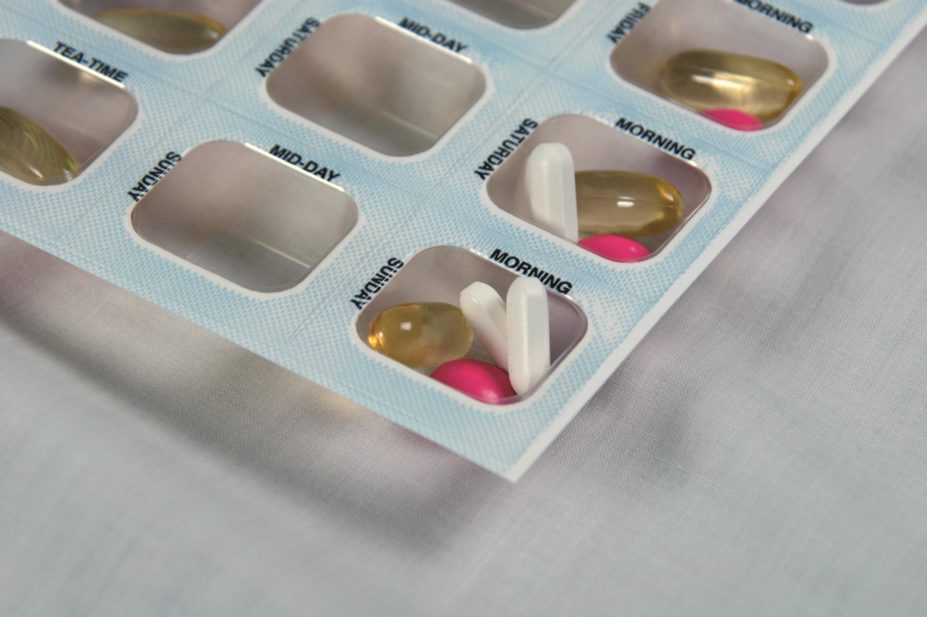
Following a feasibility study looking at the efficacy of pill organisers, also known as monitored dosage systems (MDS) or multi-compartment compliance aids (MCAs), researchers observed adverse events, particularly falls, among patients assigned to an MCA that were not seen in patients who continued with usual care.
The research was intended to explore the ideal trial design for establishing the efficacy of the devices, which includes Dosset and Nomad boxes, as well as other designs that allow multiple medications to be placed into compartments according to when they should be taken.
In addition to a systematic review and focus groups, the researchers carried out a randomised trial involving 29 patients aged 75 years and over who were selected based on certain requirements: they had to be taking at least three solid-form, oral medications, at least two of which were from a defined list of 11 drugs (including simvastatin, levothyroxine, omeprazole and metformin); and treatment had to be expected to continue for at least 12 months.
The participants were also identified as unintentionally non-adherent to their medication, which was confirmed during a three-week adherence-monitoring period, as part of the selection process. They were then randomly assigned to a weekly or monthly MCA or usual care for eight weeks.
Of the 25 patients who completed the trial, there were five adverse events or serious adverse events, all of which were among patients assigned to an MCA, the researchers found.
Reporting their findings in the July 2016 issue of Health Technology Assessment
[1]
, the researchers say the results could be a consequence of doctors increasing medication dosages for patients who were poorly adherent to their treatment before using an MCA.
“They are now taking significantly more medication than they were prior to MCA initiation,” explains lead author Debi Bhattacharya, from the University of East Anglia. “This can therefore result in dose-related side effects, such as hypoglycaemia from oral antidiabetics and hypotension from antihypertensives.”
Three of the adverse events were falls, which the researchers concluded could have been a result of drug-induced hypotension. They also recorded one incident of hypoglycaemia and one incident where a patient was incapacitated for at least 12 hours.
Bhattacharya says it is intuitive that improving medicine adherence could lead to dose-related adverse events. “When recommending initiation of an MCA, it may be prudent to review the prescribed dose of any medication with a high risk of dose-related adverse events (e.g. antihypertensives, hypoglycaemics, anticoagulants and anticonvulsants) before introduction of an MCA, and to monitor after its introduction to ensure treatment is optimised,” she suggests.
Theo Raynor, professor of pharmacy practice at the University of Leeds, says the NHS spends around £23m on MCAs each year, despite a lack of evidence for their efficacy. “If these were medicines, we simply wouldn’t be using them,” he says.
Raynor adds that prescribers and pharmacists should take other steps before suggesting an MCA to patients, including reducing the number of medicines patients are taking, where possible, and/or simplifying dosing regimes. He also suggests that a reminder chart, which doctors and pharmacists can print for patients, can act like an MCA but is much easier to initiate.
Raynor agrees that the study lays the groundwork for establishing the efficacy of MCAs in future research, but says: “Let’s try and do other things first before we use something that we really don’t know the impact of.”
Lelly Oboh, consultant pharmacist at Guy’s & St Thomas’ NHS Trust and NHS Specialist Pharmacy Services, says that social care services are a major driver of MCA use, particularly when patients come out of hospital, because some care providers will not give medications unless they are in an MCA.
She adds that using MCAs has become the norm, but says the focus for pharmacists should be on finding out why people are not taking their medicines. She adds that MCAs are just one method to try to improve adherence; other actions such as coaching patients on the value of their medicines, using a diary, changing formulations, or enlisting the help of family or carers may also be effective.
“We can’t say this is the one thing that’s going to work, so we always need to find out for that particular patient what their needs are and the reasons they’re not taking their medicines. And then we have to decide what’s the best way [to help them],” Oboh concludes.“That’s exactly what we knew before and I think that’s what this [study] is still saying.”
References
[1] Bhattacharya D, Aldus CF, Barton G et al. The feasibility of determining the effectiveness and cost-effectiveness of medication organisation devices compared with usual care for older people in a community setting: systematic review, stakeholder focus groups and feasibility randomised controlled trial. Health Technology Assessment 2016. doi: 10.3310/hta20500
You may also be interested in

‘Moving the goalposts’: the worrying rise of testosterone replacement therapy

Coroner flags lack of clarity around expanded role of community pharmacists under Pharmacy First
