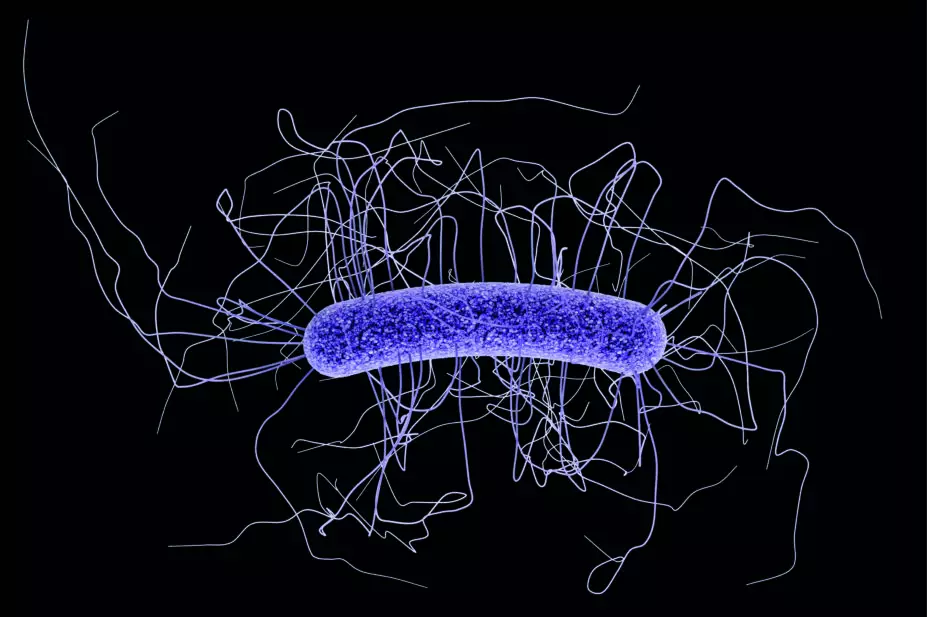
CDC / James Archer
A new antibiotic to target Clostridium difficile is to enter phase III clinical trials, it has been announced.
Ridinilazole, which was developed by Oxfordshire biotechnology company Summit Therapeutics, is a narrow-spectrum antibiotic which, in preclinical efficacy studies, was found to have a potent bactericidal effect against all clinical isolates of C. difficile tested.
In phase II clinical trials, it was found to be well tolerated and demonstrated potent bactericidal activity against C. difficile with a minimal effect on the bacteria that naturally reside in the gut, thereby reducing the risk of recurrent infection.
According to government figures, C. difficile is the biggest cause of infectious diarrhoea in hospitalised patients and can, in the most serious cases, be fatal.
The phase III clinical trial programme is expected to comprise two large global trials of around 700 patients each to evaluate ridinilazole compared with the current standard of care, vancomycin, to see which is superior in terms of sustained clinical response (SCR). SCR is defined as clinical cure at the end of treatment and no recurrence of infection within 30 days.
Ideal treatment
Richard Vickers, chief scientific officer for antimicrobials at Summit Therapeutics, said: “As evidenced by our growing body of clinical and preclinical data, we believe ridinilazole has the ideal profile to become a single therapeutic approach capable of both treating the initial C. difficile infection and reducing the high rates of recurrent disease.”
C. difficile occurs naturally in the intestines and, in healthy people, causes no symptoms. Infection arises when the normal bacteria in the gut are compromised, typically following the use of broad-spectrum antibiotics that can cause widespread damage to the natural flora in the gut, enabling the overgrowth of C. difficile bacteria, of which some strains are now resistant to certain antibiotics.
For decades[1]
, the only treatments for C. difficile have been broad-spectrum antibiotics, specifically, vancomycin and metronidazole, which, while effective, also damage the gut, leaving patients vulnerable to further infection.
According to the Summit Therapeutics, within the first 30 days there is a 25–30% chance of having a second C. difficile infection and each additional episode of C. difficile infection is associated with greater disease severity, higher mortality rates and, consequently, an increased burden on the healthcare system.
An urgent issue
In a 2013 report, the Centers for Disease Control and Prevention (CDC), stated C. difficile to be one of three urgent threats that require urgent public health attention.
“Despite a 77% reduction since 2007 in cases of C. difficile infection, it is still a major problem in the UK. Last year, there were almost 13,000 cases reported in England and more than 2,000 deaths,” explains Phil Howard, consultant antimicrobial pharmacist at Leeds Teaching Hospitals NHS Trust and a member of the Royal Pharmaceutical Society (RPS) Antimicrobial Expert Advisory Group.

Source: Royal Pharmaceutical Society
Phil Howard, consultant antimicrobial pharmacist at Leeds Teaching Hospitals NHS Trust and a member of the Royal Pharmaceutical Society (RPS) Antimicrobial Expert Advisory Group, points out that there was a 9.3% drop in C. difficile cases in England last year
However, as he points out, there was a 9.3% drop in C. difficile cases in England last year, which he attributes, not to new treatments, but to the reduction in broad-spectrum antibiotic use in response to the primary care quality premium and hospital CQUIN clinical improvement schemes.
“Prevention of C. difficile through good antimicrobial stewardship is probably the best strategy, though improved treatments of those who develop C. difficile is always welcome,” he says.
Fast-track designation
In July 2015, ridinilazole was granted fast-track designation by the US Food and Drug Administration, which also designated the antibiotic as a Qualified Infectious Disease Product (QIDP). This means that its marketing exclusivity is extended for an additional five years upon FDA approval.
A review by Lord Jim O’Neill, ’Tackling drug-resistant infections globally’[2]
, published in 2016, predicted that AMR will cause 10 million deaths a year by 2050, an effect on the world economy of $100 trillion and the potential end of modern medicine as we know it today.

Source: AMR Review
The Review on Antimicrobial Resistance, which was formerly chaired by Lord Jim O’Neill, pictured, predicted that AMR will cause 10 million deaths a year by 2050
In May 2017, G20 health ministers made a commitment to tackle antibiotic usage and begin implementing national action plans by the end of 2018. In further efforts to tackle antimicrobial resistance (AMR), the European Medicines Agency, recommended changes to the prescribing information for vancomycin, for example changes to the way infusion dosages of the antibiotic are calculated so that they are based on a patient’s age and weight. The recommendations supported the oral use of vancomycin for C. difficile infections.
The results of the ridinilazole phase III trial are expected in 2020.
References
[1] Goldenberg, S. Expanding the armamentarium for the treatment of Clostridium difficile infection. Lancet Infect Dis 2017. doi.org/10.1016/ S1473-3099(17)30237-2
[2] O’Neill, J. The review on antimicrobial resistance: Tackling drug-resistant infections globally. May 2016. Available at: https://amr-review.org/sites/default/files/160518_Final%20paper_with%20cover.pdf