
James Jones Jr/Shutterstock
A five-year integrated pharmacy degree, leading to pharmacist registration, is set to be introduced throughout Scotland in three years’ time. However, the detail of how the workplace learning will fit into the degree timetable and which model to adopt, has not yet been decided.
Shona Robison, the Scottish secretary for health and sport, is backing the proposal from the special advisory group that was set up to consider the reform of education and training and which published its report, ‘Five-year integrated initial education programme for pharmacists in Scotland’ on 5 May 2017.
The Scottish government had asked the chief pharmaceutical officer to set up the advisory group, which was called the Five Year Integrated Initial Education Programme for Pharmacists in Scotland.
Robison told The Pharmaceutical Journal: “I warmly welcome these proposals to strengthen the initial education of pharmacists in Scotland by moving to an integrated five-year programme.”
She adds: “Given our current focus on workforce planning and development and the extending role of pharmacists within multidisciplinary teams, this report provides a real opportunity to better prepare our new pharmacists for practice in Scotland by ensuring they are able to practice in the evolving NHS health and social care landscape.”
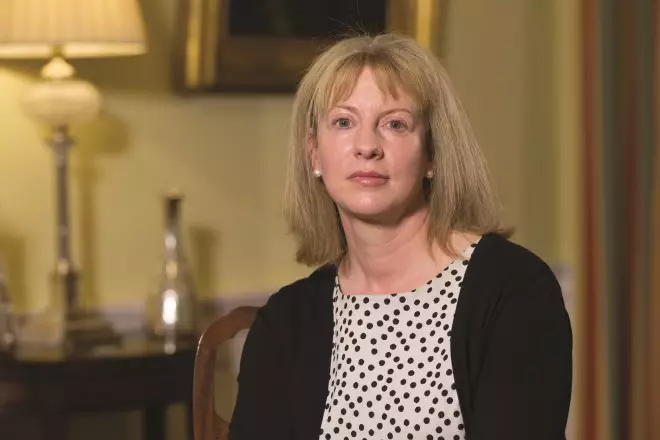
Source: Scottish government
Shona Robison, the Scottish secretary for health and sport, says that moving to an integrated five-year programme will strengthen the initial education of pharmacists in Scotland
In the report, the advisory group is recommending that the new five-year degree should be introduced in 2020 and replace the existing traditional four-year programme. At present, the initial education and training of a pharmacist comprises a four-year Master of Pharmacy (MPharm) degree and a one-year pre-registration training programme (4+1).
There is a need for a step change to create a more clinically focused, integrated degree to ensure that pharmacy graduates can meet the workforce demands of the profession in Scotland, the advisory group says.
Furthermore, there is also a need for more “enhanced experiential learning in clinical practice” and a recognition of the benefits of workplace learning which can reinforce confidence and professional competence.
The advisory group points out that a five-year integrated degree provides opportunities for earlier development and assessment of professionalism and holistic clinical decision-making. It will also permit better management of pharmacy trainee numbers to meet workforce demands.
The new degree also supports the Scottish government’s priorities to strengthen the primary care workforce and its desire for every GP practice to have access to a pharmacist with advanced skills.
However, the group backs away from proposing how a five-year degree would be delivered and whether the workplace learning would be offered as a 12-month block, for example, or in smaller blocks across the programme. That finer detail should be worked out as part of the implementation programme, the group recommends.
The change will make Scotland the first UK country to introduce a national integrated five-year degree and the proposed implementation could begin in 2020–2021.
“The first students achieving [the new] status could graduate and register in summer 2025,” says the report. This will require an alignment of the reaccreditation of the two schools of pharmacy in Scotland by the General Pharmaceutical Council so that they both occur within the same timescale (2019-2020), it adds. The two Scottish pharmacy schools are based at Robert Gordon University in Aberdeen (pictured above) and at Strathclyde University in Glasgow.
Currently, only the University of Nottingham and the University of East Anglia offer a five-year integrated route to professional qualifications and registration. The University of Bradford also has a five-year degree but its model is different as it offers “intercalated” periods of pre-registration training which means that workplace learning is not overseen by the institution. There are no similar five-year degrees in Northern Ireland or Wales.

Source: Royal Pharmaceutical Society
John McAnaw, chair of Royal Pharmaceutical Society Scottish Pharmacy Board, said he would also like to see the initial education of pharmacists become a clinically funded degree
Commenting on the report, John McAnaw, chair of Royal Pharmaceutical Society Scottish Pharmacy Board, said: “With an integrated degree programme, the opportunity to provide enhanced experiential learning in the different sectors of the profession will be a very positive step, and it aligns well with our manifesto statement which advocated a standardised approach to vocational training.”
However, McAnaw, said there were a number of issues to be worked through before it becomes reality, such as the funding and timing of clinical placements.
“But we are supportive of taking a staged approach and to evolving the model as outlined in the report. We would also like to see the initial education of pharmacists becoming a clinically funded degree, as this would provide greater scope for interdisciplinary learning and for the necessary clinical experience across the health professions to be in place for our students.”
The group’s report comes eight months after it was originally set up to explore whether there was support for an integrated degree.


