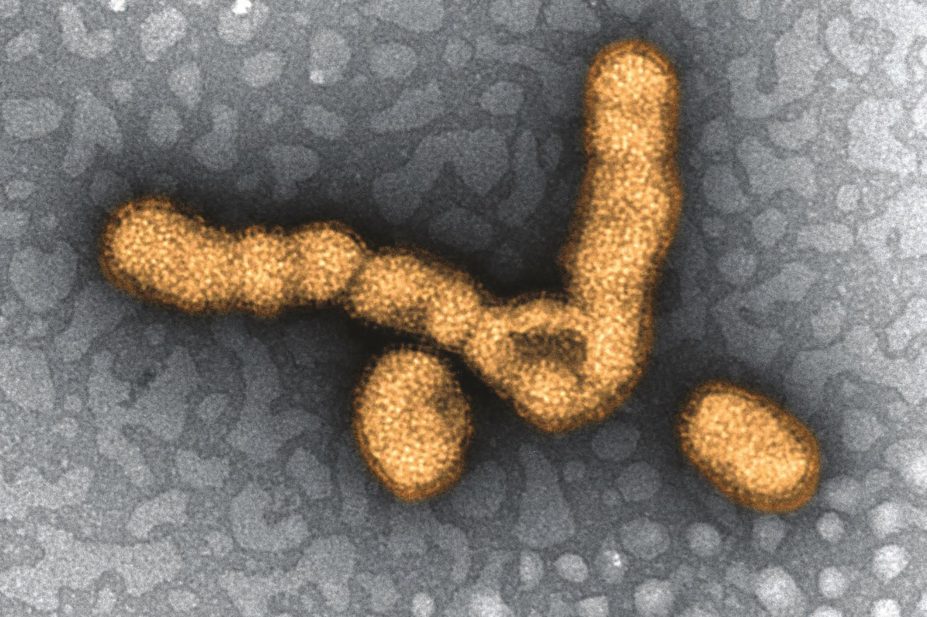
National Institute of Allergy and Infectious Diseases (NIAID)
The evidence base for influenza drugs such as oseltamivir (Tamiflu) and zanamivir (Relenza) must be strengthened, says a report from the Wellcome Trust and the Academy of Medical Sciences.
However, the report, initiated in response to a request from the Department of Health, says “the government will always have to make difficult policy decisions based on incomplete evidence and in the face of competing priorities”.
Neuraminidase inhibitors (NAIs) have been the subject of much controversy, especially after a 2014 Cochrane review concluded that Tamiflu did not reduce flu admissions to hospital, and it was questioned whether the UK government was justified in stockpiling these drugs. The review followed a long battle to gain access to the clinical trial data.
The report, ‘Use of neuraminidase inhibitors in influenza’, states that randomised control trials on the drugs are a “high priority”, despite the difficulties of conducting such research in the event of an influenza pandemic. However, it adds that pre-existing evidence from observational studies are not to be dismissed. It is “essential” that pre-agreed protocols are now put in place to collect high quality evidence for the drug’s effectiveness, the report says.
Richard Pebody, head of flu surveillance for Public Health England, acknowledges that the report highlights areas where the evidence base is more limited.
“We will carefully consider the findings of the report, but it is important to note that the UK remains one of the best prepared countries for future flu pandemics and antivirals remain a core part of our strategy,” he says.
The report suggests that in the event of a pandemic, or a particularly virulent strain of seasonal influenza, routine use of the drugs may be “advisable”. Pebody says “the UK maintains stockpile of NAIs to respond to a flu pandemic – with enough stock to treat 50% of the population”.
For patients hospitalised with severe influenza, the drugs can reduce the number of deaths, the report says. Therefore, it recommends that oseltamivir and zanamivir should only be used in cases where the patient requires hospitalisation.
But for the majority of patients, flu is a self-limiting disease and the report reiterates the findings from the Cochrane review that the use of NAIs has been found to reduce the duration of illness by only 14–17 hours. Pebody says that the findings are largely in line with current UK government policy.
In addition, the data indicate that for the medicines to be effective, they should be initiated within 48 hours of the onset of symptoms, in line with current UK recommendations. However, as use of the drugs is only recommended in severe disease, identifying these patients within 48 hours can be a difficult clinical judgement, the report says.
In the case of high-risk patients, the report says the evidence is clear that pregnant women hospitalised with flu should be given NAIs. But for other high-risk groups, such as children, there is a lack of evidence to guide decisions on NAI treatment.
John Ashton, president of the Faculty of Public Health, says: “The report shows there is good evidence for using antivirals in some cases, although they have no place in treating seasonal flu. People in at risk groups are more vulnerable, while there may be circumstances in which giving antivirals to large parts of the wider population is necessary.”
He says: “We agree with the authors that it is difficult to decide about whether stockpiling of antiviral drugs is necessary, because the evidence for this is patchy and the nature of future pandemics uncertain.”
The faculty supports the call for further research about what makes antivirals effective in treating influenza. “We also need to provide the public with clear messages about how we best provide the right coverage to whole populations when required,” Ashton adds.
You may also be interested in

Antivirals have little effect on mortality in patients hospitalised with COVID-19, suggest WHO trial interim results
Government tightens availability of remdesivir treatment for COVID-19 patients as supplies shrink