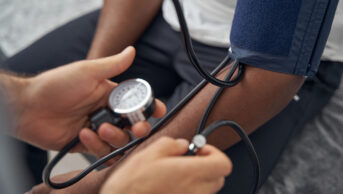
Alamy stock photo
The launch of one of the biggest campaigns to encourage greater use of community pharmacy and pharmacists as a frontline clinical service didn’t go entirely as planned.
The most cited reports on the Stay Well Pharmacy campaign, according to Google news, were a story in The Times suggesting that taking unwell small children to a pharmacy, rather than a doctor’s surgery, risked cases of sepsis being missed; and a meningitis survivor told their local paper they would take the pharmacy-first advice with caution.
But it would be churlish to criticise NHS England’s marketing exercise too heavily. It has ploughed a significant sum of money into this campaign, which includes a slick TV advertisement, and full social media push, to encourage millions of people, emphasising parents with children under the age of 5 years, to consult a pharmacist initially for minor illnesses.
This can only benefit community pharmacy. And if the drive is as successful as hoped, the NHS will be £850m better off and pharmacists will be firmly installed at the forefront of the public’s mind as the go-to clinician for self-limiting conditions.
But while such efforts are to be welcomed, the question has to be asked whether an equally effective route to establishing the pharmacy profession as a trusted clinical service would be to ensure that pharmacists are used in expanded clinical roles, and in big numbers.
If patients are treated by pharmacists who can manage their long-term condition when they call NHS 111 or present at their GP surgery, or by pharmacists who successfully stop them from smoking, would this not produce the anecdotal evidence among the general public that a pharmacist can be consulted just as readily as a doctor in many instances?
In 2016, a Royal Pharmaceutical Society report found that introducing a named pharmacist policy giving pharmacists overall responsibility for medicines in care homes across Great Britain could significantly improve quality of care and save £135m for the NHS every year.
An announcement of hundreds of pharmacist roles being created in care homes had been expected for some time; but in the end, news of the government’s intention to fund 180 pharmacy and 60 pharmacy technician posts to help improve medicines optimisation in care homes dribbled out this month, buried away on page 26 of NHS England and NHS Improvement’s ‘Refreshing NHS plans for 2018/19’.
These new posts will be paid for by the controversial Pharmacy Integration Fund, which the government admitted shortly before Christmas, had spent only just over a third of the budget pledged for 2016–2018.
So 180 pharmacists in care homes is a start. And pharmacists have been funded to do exceptional work in the NHS Urgent Medicine Supply Advanced Service, while money has been provided to
embed 1,100 pharmacists in general practices
. Health Education England is also developing new pharmacy training programmes, including independent prescribing qualifications for up to 2,000 pharmacists working in primary care.
So the work to increase pharmacy’s clinical heft in the NHS does seem to be bearing fruit, albeit slowly. But with greater consistency in the government’s recognition of the pharmacists’ role in the wider healthcare arena, the need for glossy marketing campaigns may be lessened in the future, and first-hand evidence of pharmacy’s achievements may be more abundant.