McLean
Ever since the Shipman inquiry in 2002, which found former GP Harold Shipman to be guilty of the murder of more than 250 of his patients, UK regulations around controlled drugs (CDs) have noticeably tightened.
Just over a decade later, in 2013, healthcare organisations were mandated to appoint a controlled drug accountable officer (CDAO) to monitor CDs across their local communities, and CDs local intelligence networks were set up for the reporting of CD concerns.
Reports of “unaccounted for losses” of controlled drugs are now on the rise. Figures obtained by The Pharmaceutical Journal under the Freedom of Information Act have revealed that 1,387 controlled drugs were reported as being lost, stolen, or missing in England in 2018/2019. This is a rise of 19% on the previous year.
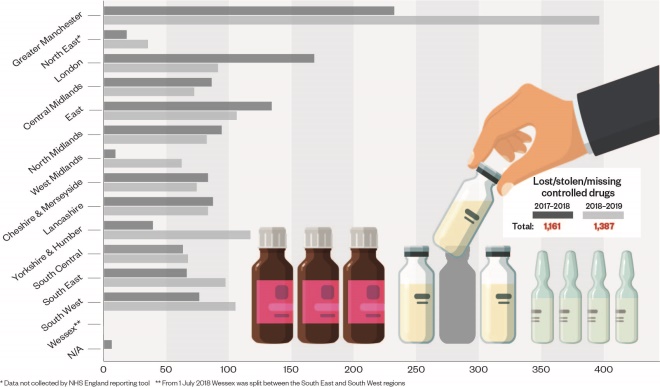
There are complex reasons behind this increase in the number of reports — not least that the rollout of NHS England’s reporting tool was only completed in 2018. It is also not clear what proportion of these missing CDs result in diversion and illicit use and/or sale on the black market.
However, this does not excuse the fact that there are serious concerns that the UK’s CD system is being undermined by naivety, tardy reporting and a lack of resources. In its latest report on the subject, published in July 2019, the Care Quality Commission (CQC) said that diversion of ‘lower schedule’ controlled drugs — such as those in Schedule 4 and Schedule 5 — was becoming “increasingly sophisticated” and that monitoring of incidents was “insufficient”.
No system is foolproof, but again this is no excuse — we should not be in a situation where CDs are being grabbed from pharmacy shelves.
Indeed, perhaps it is not the regions that have reported the highest numbers that we should be looking at, but those that are reporting the fewest incidents. For example, 396 incidents of CDs being lost, stolen or missing were reported in Greater Manchester in 2018/2019, whereas only 62 incidents were reported in the West Midlands during the same period.
There may be good reason for this, but, in many cases, these variations come down to reporting culture. CDAOs say that, too often, incidents of possible diversion are deemed insignificant and remain unreported, or are reported too late for them to be developed properly.
The whole system rests on healthcare professionals reporting incidents to their CDAO in good time, so that the circumstances around the loss can be investigated. Healthcare professionals need to let go of the fear of reporting these incidents and instead consider carefully the dangers of not reporting them.
Only then can trends be identified, gaps in management plugged and national policy be adjusted to ensure that these dangerous drugs do not end up in the wrong hands. It should not need stating that there is the huge potential for harm here: these drugs fuel addiction, cause significant harm and can lead to death.
Pharmacists are vital to this. Both in hospital dispensaries and the community, pharmacists should be looking at their processes to ensure they are capable of spotting any signs of CD diversion at the earliest opportunity, and improving and standardising their management of CDs where they can.
CDAOs have also told The Pharmaceutical Journal that, too often, their teams were too small to be able to respond appropriately to concerns being raised. There is certainly a case to be made that there are too many national bodies involved — the police, the Medicines Healthcare products Regulatory Agency and the CQC — and too few on the ground making sure the system remains robust.
This is no time to be complacent about the management of CDs in the UK. Only with consistent reporting and a strong commitment to prioritising this issue can we gain a clear picture of the scale of abuse and diversion of CDs — and then hope to tackle it.


