I was clinically screening a prescription chart in the treatment room on a ward, when a newly qualified nurse came in crying. Asking what the matter was, she confided that she had made an administration error, and self-reported the incident to the ward manager. The junior nurse is now frightened of doing drug administration rounds, and takes a long time to complete her round.
This incident reminded me of my first error as a newly qualified pharmacist, and how petrified I felt about making the error. Are healthcare professionals entering the workplace prepared for the emotional impact of an error occurring, and are we supported in our learning post errors?
Evidence suggests that improving staff experience in turn improves patient experience.[1] Do hospital trusts support the emotional, and psychological well-being of staff who have made errors?
I conducted a study that aimed to evaluate the extent to which pharmacy staff, doctors, and nurses are supported in their learning from medication errors. It was a qualitative study that used focus groups to explore participants’ views on five topics related to the study aim. These included the emotional component of errors, barriers to learning from errors, support and feedback given after an error is made, learning activities undertaken, and improvement strategies.
Emotional response to an error
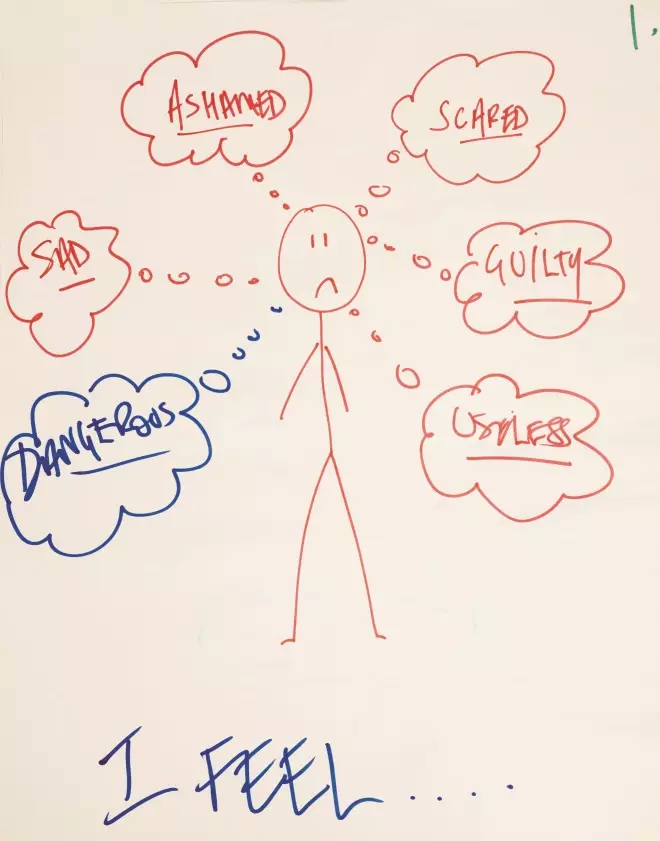
Drawing from a pharmacist who had made a medication error.
Participants said they experienced powerful emotional responses after making medication errors. All professional groups and grades report feeling worried, scared, ashamed, upset, angry, stressed and guilty after making an error. Participants reported loss of sleep, feeling sick (nauseous), and crying as reactions to errors.
Statements such as “I could have killed myself” and “till today, I have not got over it” raised concern about the psychological well-being of the participants concerned. Students and junior participants reported feeling like a hindrance and nuisance and explained that as a newly registered practitioner every error is huge to you.
Participants reported loss of confidence in performing the same task and stated that time and support to rebuild that confidence was not offered.
Additionally, participants reported fear due to realising they could cause harm to the patients, fear of disciplinary action, and disappointment because they believed they had let the patients down. Doctors in particular reported that they felt isolated and empty inside.
Support from colleagues

Drawing from a doctor, illustrating a lack of support for staff following a medication error.
A few participants reported good support by senior staff in terms of reassurance and encouragement to reflect and learn from the experience. However, a large proportion of participants reported lack of support and feedback, suggesting: “nobody has got the time, so we don’t get support post errors”. The participants raised a strong concern about their well-being in relation to patient safety, and said the result of an error was “unhappy, worried, and scared staff, who as a result cannot be 100% effective in patient care”.
I have been involved in the introduction of an NHS trust training session on human factors and what it is to be human; setting up a confidential error support link accessible via the Datix error reporting system; and writing a ‘learning from errors’ help sheet which has been published by confidential care.[2]
Nobody wants to make an error, especially when that error could have serious consequences for patients. Perhaps we need to do more research into how we can facilitate a working environment where support is given to those who make mistakes and constructive feedback is given to help people learn from them.
References
[1]
Boorman, S. NHS Health and Well-being Review: Final Report. London: Central Office, 2009
[2] Confidential Care line (CiC) (Trust subscription) www.well-online.co.uk


