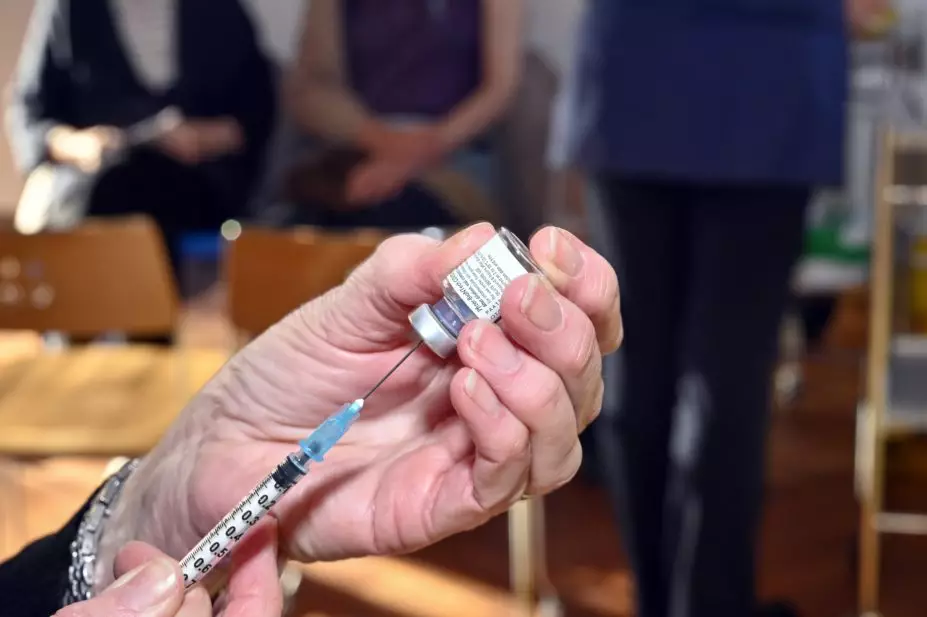
Science Photo Library
I was offered the Pfizer BioNTech COVID-19 vaccine and, to be frank, I was scared.
I called my parents, friends and colleagues. Is it safe? What are the long-term effects? I spent a day frantically learning as much as I could. I even read the 51-page public assessment report. I sought to understand the science behind the technology. I deep-dived into the conspiracy theories. After much nail biting, the internet did something it hasn’t done for a while: it reassured me.
So I booked my appointment and the very next day — Sunday 20 December — I received the vaccine at a vaccination hub at the Bloomsbury Surgery, London. I was welcomed by a multidisciplinary healthcare team donned in personal protective equipment. After completing my risk assessment and getting my temperature checked, I was ushered into a vaccination room and greeted by a nurse, who was professional and reassuring. She double-checked my risk assessment questions — such as whether I had a history of allergy or anaphylaxis, any recent vaccinations, any chance of pregnancy, and any anticoagulation medicines — and then she prepared my vaccine.
For me, the injection was painless, just like getting my annual flu jab (although, I must say, this felt just a tad more momentous). After the vaccination, I sat in a waiting room for 15 minutes while being monitored for any adverse reactions. I then booked my second dose: 21 days from the date of my first one.
I left the vaccination centre feeling optimistic, feeling lucky to receive the vaccine, and feeling extremely proud to work as a healthcare professional. If having a sore arm for the next two days was the price to pay, it seemed like a pretty good deal.
Are you anxious about the vaccine? Let me break it down for you:
Was the vaccine process ‘rushed’?
In short: no. Although the vaccine has been developed, tested and approved quickly, there has been no compromise on safety or efficacy. The research supporting the Pfizer vaccine is based on years of data we already had for coronaviruses, and uses well-established mRNA technology. Also, a public sense of urgency meant that we had more scientists, more money and more resources than ever before thrown at one issue — that brings down barriers.
Is the vaccine safe?
In short: yes. Before the Pfizer BioNTech vaccine was approved by the Medicines and Healthcare products Regulatory Agency (MHRA), it was studied in around 43,000 participants in an ongoing randomised placebo-controlled international trial. The side effects observed are much like those of other approved vaccines, including pain at injection site, tiredness, headaches — all textbook reactions. And it’s important to note that mRNA technology does not affect our body’s genetic material because it never goes inside our cells’ nucleus, where our DNA is stored. The body will degrade the mRNA once it has delivered the message to produce antibodies against COVID-19.
What are the long-term effects?
In short: we don’t know. What we do know is that COVID-19 is deadly: at the time of writing almost 70,000 people in the UK have died. We know that most side effects of vaccines occur very quickly. There are very few cases where problems have developed later down the line. And in the event that any problems develop, they’ll be continuously monitored under the MHRA’s yellow card scheme. The long-term impact was what concerned me most. I understand the hesitation, but we need to be driven by data, and not emotions. There are very few cases where vaccines have administered anything but protection.
I encourage all pharmacists and pharmacy teams to get the vaccine when it is offered to them. Pharmacies are located at the heart of communities. We are the most accessible healthcare professionals, with more than 400 million visits to community pharmacy every year, so we have to make sure we keep safe and reduce the transmission of the virus.
Many of our patients are elderly or have comorbidities, putting them at high risk of suffering poorer outcomes from COVID-19. Having the vaccine means protecting your patients, protecting your families, protecting your colleagues, and preventing our NHS from being overwhelmed, and it is one of the first steps in getting back to a life without lockdowns. Vaccines save lives.
Chaohui Wang, community pharmacist, Green Light Pharmacy; teacher practitioner, UCL School of Pharmacy. Tweet her at: @chaowangpharm
Find out more: ‘Ten things pharmacists should know about COVID-19 vaccines’


