istockphoto.com
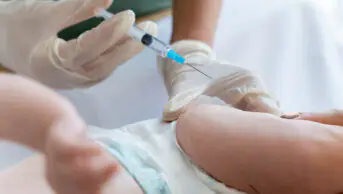
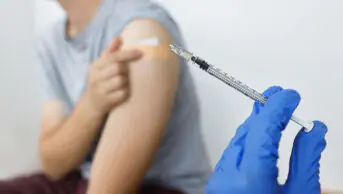
Community pharmacies in England have been commissioned to administer influenza vaccines for the upcoming 2015–2016 flu season. The deal between NHS England, NHS Employers and the Pharmaceutical Services Negotiating Committee (PSNC) means there will, for the first time, be a national plan to have pharmacy manage a vaccination service.
Some pharmacies in England already provide flu vaccines according to local agreements, and this deal builds on the success of those pharmacies in recruiting patients and providing a safe service. With certified training, pharmacists will provide the seasonal flu jabs to eligible adults according to the national flu immunisation programme, which is administered by the Department of Health in conjunction with Public Health England (PHE) and NHS England.
Pharmacists will need to keep records of any consultations for the purposes of clinical governance, claiming of payments and post-remuneration checks. According to the information available from the PSNC and NHS Employers, there will be a service specification and guidance will be provided; these need to be published as soon as possible to ensure that pharmacy owners, managers and staff have as much time as possible to train and prepare.
Flu vaccines are not always highly effective at preventing infection. Protection offered by the 2014–2015 season vaccine was as low as 3% overall in a UK analysis of 1,314 primary care patients, conducted by PHE. Usually, a 50% effectiveness figure is achieved.
The World Health Organization (WHO) advises on the strains it believes will be prevalent in the coming year in the northern and southern hemispheres. This advice informs the make-up for the vaccines to be manufactured. Sometimes the WHO’s assessment is not quite right, or there is genetic drift that renders the vaccine less effective, as was the case for one component in the past winter.
Nevertheless, vaccination remains an effective way of reducing the burden of flu among at-risk patients. Those adults eligible for the flu vaccine programme in England are people aged 65 years and over; younger adults in certain clinical risk groups, such as those with respiratory disease, diabetes or heart failure; people in long-term care settings; pregnant women; and carers.
It is easy to see how community pharmacy can be a one-stop setting for vaccination. Patients collecting prescriptions for any of the at-risk conditions are an obvious group for pharmacies to target. Medicines use reviews and the new medicine service may help pharmacists to identify opportunities to explain the value of flu vaccination. Over-the-counter medicines transactions provide further opportunities for pharmacy teams to connect with hard-to-reach groups. And many pharmacies have contact with nursing homes and carers of older patients who live at home.
In the 2012–2013 winter, PHE received reports of 904 people with confirmed influenza infection admitted to critical care wards, 98 of whom died. Many more cases of flu are neither recognised nor recorded, and on average around 8,000 deaths per year are attributable to flu.
Pharmacies are a good place to improve coverage of flu vaccination among hard-to-reach patients. But community pharmacy teams must be proactive in recruiting eligible patients to be vaccinated to safeguard their health.