The Board of Trustees of the Science Museum
A new exhibition at the Science Museum, London, which opened on 9 November, explores potential solutions to the “unprecedented global threat of antibiotic resistance”.
Superbugs: The Fight For Our Lives
interweaves human stories of “superbug” encounters with the latest research into diagnostics and the search for new antimicrobials.
Visitors are introduced to Geoffrey Pattie, a cancer patient, who describes his months spent in a hospital isolation unit after antibiotics failed to treat his kidney infection. We hear from Sarah Whitney, an infection prevention nurse at The Royal Marsden NHS Trust, London, who uses mapping tools to prevent bacterial spread across wards. And GP Imran Rafi discusses the challenges of reducing antimicrobial prescribing in the face of patient expectations.
A range of design solutions is presented, too, including door handles with built-in sanitisers and fluorescent bandages that glow in the presence of bacterial infection.
A separate display showcases, for the first time, four prototype diagnostic devices competing for the Longitude Prize, alongside some rather unusual sources of potential new antibiotics, including leafcutter ants and komodo dragons.
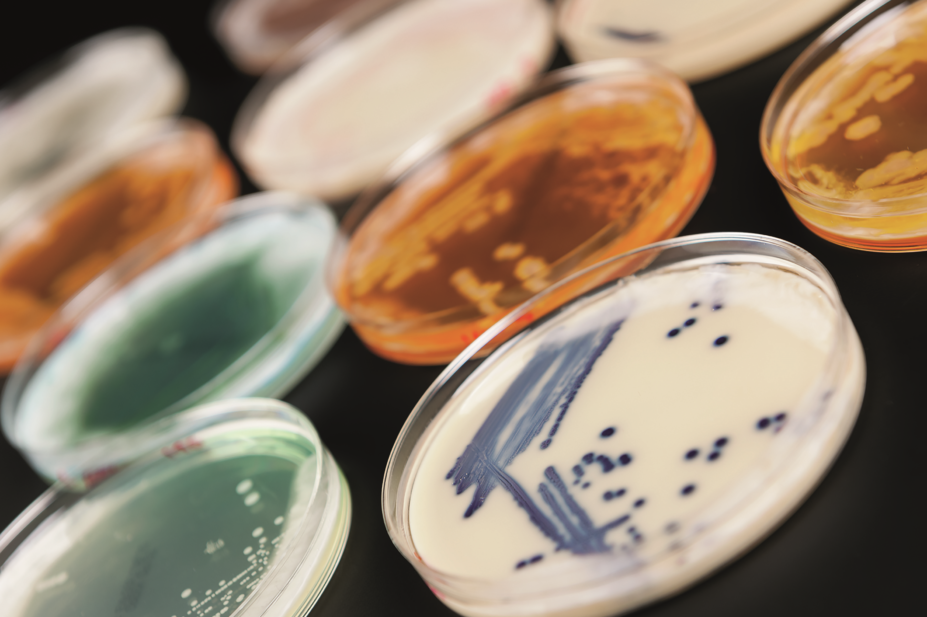
Visitors can also experience a close encounter with twelve real (albeit well-sealed) bacterial colonies, including nine bacteria that the World Health Organization (WHO) classifies as “a significant threat to human health”.

Source: Corrinne Burns / The Pharmaceutical Journal
A separate display showcases, for the first time, four prototype diagnostic devices competing for the Longitude Prize
Speaking at the exhibition launch, Lord Jim O’Neill, author of 2016’s
Review on Antimicrobial Resistance
, said that globally 750,000 people die each year as a consequence of antibiotic resistance. If we do nothing to address the matter, he added, this figure could rise to 10 million people by 2050. O’Neill imagined a future where doctors would not be allowed to prescribe antibiotics unless “state-of-the-art diagnostic tests” had been carried out on the patient: “Even if we find new and effective drugs, we need to stop treating antibiotics like sweets.”
There is no community or hospital pharmacist voice in the exhibition, and hence no exploration of how pharmacists’ work on antimicrobial stewardship aligns with that of their colleagues in primary and secondary care. However, Seema Patel, medical director at Pfizer Essential Health UK who is a qualified pharmacist, told The Pharmaceutical Journal that the exhibition is a good opportunity to “raise awareness with the public, and to get them to think a bit more about how they use antibiotics so they can then have a discussion with their doctor, nurse or pharmacist.
“It’s about getting the message lined up, so we’re all consistently advising the same thing to our patients.”

Source: Corrinne Burns / The Pharmaceutical Journal
The exhibition’s message will not be new to pharmacists, but it is certainly interesting to explore some of the more unusual avenues being investigated in the hunt for new antibiotics, diagnostic tests and interventions to prevent the spread of infection. And it is good to see the Science Museum giving such an accessible and engaging profile to antimicrobial stewardship efforts. The exhibition dovetails well with the awareness-raising efforts of other organisations, including the Royal Pharmaceutical Society’s antimicrobial stewardship campaign.
“Educating healthcare professionals, patients and governments about the problems and potential solutions in antimicrobial resistance is key,” Patel said.
“I think this exhibition can only be a good thing.”
Superbugs: The Fight for Our Lives is free and open daily from 9 November 2017 until spring 2019. The exhibition is sponsored by Pfizer (major sponsor) and Shionogi (associate sponsor) with additional support from UK Research and Innovation and the University of East Anglia.
RPS campaigns on antimicrobial stewardship
Antimicrobial stewardship has long been a policy and campaign focus of the Royal Pharmaceutical Society (RPS).
Responding to the UK Government’s Antimicrobial Resistance Strategy, published 13 September 2013, the RPS said that “Training of community pharmacists has the potential to reduce GP consultations by means of public education and symptomatic management of self-limiting infections”. In another response, to a 2014 NICE consultation on guidance for ‘Antimicrobial resistance: changing risk-related behaviours’ the Society said that the “use of minor ailment schemes whereby patients can receive symptomatic treatments for infections can decrease visits to a GP by 50% and reduce the number of prescribed antibiotics”.
In July 2014 the Society, together with the Royal College of General Practitioners (RCGP), the Royal College of Physicians (RCP), the Royal College of Nursing (RCN) and the UK Faculty of Public Health (FPH) published a Joint Statement on Antimicrobial Resistance. Among the recommendations of this statement was a call for antimicrobial prescribing data to be monitored, and for licensing requirements for new antimicrobials changed to include data on the minimum dosage required for clinical effectiveness.
In 2014, RPS Scotland collaborated with the Scottish Antimicrobial Prescribing Group (SAPG), Community Pharmacy Scotland and Pharmacy Voice to produce a European Antibiotic Awareness day resource pack for community pharmacists, which included a patient-directed self-care information leaflet for treating infectious ailments. The packs were distributed in November 2014.
Later that month, on European Antibiotic Awareness Day itself —18 November 2014 — RPS Scotland held a parliamentary reception and debate on antimicrobial resistance, sponsored by Jim Eadie MSP. The event led to a Scottish Parliamentary debate on the subject, held on 5 February 2015. Also on European Antibiotic Awareness Day, RPS Wales and the Royal College of General Practitioners (RCGP) held a lunchtime discussion with Welsh Assembly Members (AMs) on the use of antibiotics in primary care. During the summit, the two professional bodies called for Wales to commit to a public education campaign on the subject, and greater antimicrobial stewardship.
At the 2017 annual conference, the RPS launched its new GB-wide campaign on antimicrobial stewardship. The campaign aims to show how pharmacists are contributing to a targeted 50% reduction in inappropriate prescribing of antibiotics by 2020. As part of this campaign, the AMS portal— a hub for health professionals co-produced by the RPS and University College London — will be updated and relaunched.
Throughout all antimicrobial campaign and policy activity, the Antimicrobial Expert Advisory Group — chaired by antimicrobial pharmacist Harpal Dhillon — acts to advise the Society and shape policy on the subject.
Your Society working for you.
Not a member? Become a member now


