Abstract
Aim
To assess the current level of service offered to clients for smoking cessation and to identify opportunities for improvement.
Design
Cross sectional survey.
Setting and sample
Community pharmacies located in five PCTs in north London (n=298).
Outcome measures
Pharmacist and pharmacy characteristics, smoking-cessation knowledge and training, current provision of a smoking cessation service, content of advice, attitudes and potential barriers to the provision of a service.
Results
Responses were received from 80 pharmacists. Half of the respondents always proactively offer brief advice when selling or dispensing nicotine replacement therapy (NRT) and bupropion, but less often when selling OTC medicine and other prescriptions. The most common advice is to suggest the use of NRT and 71.3% offer a smoking cessation service with follow-up clinic. Training has a clear influence on whether a proactive role is adopted and in offering a smoking-cessation service. Respondents have excellent knowledge in the use of NRT in smoking cessation but poorer knowledge of behavioural change techniques.
Discussion
A large proportion of respondents provide a smoking-cessation service, but there are gaps and deficiencies in knowledge and services, suggesting opportunities for improvement. Training programmes should focus on behavioural and cognitive techniques as well as pharmacotherapies. A system of offering smoking cessation advice in a more consistent and structured way by using a computer program should be explored.
Pharmacists are a highly credible source of health information, accorded with a high level of trust.1 Despite long recognition by the Royal Pharmaceutical Society of health promotion and health education as core activities for pharmacists,2 they are still “a major untapped resource for health improvement”.3
Recent proposals are for community pharmacists to develop a much wider role in public health.3 As the first point of contact for purchases of pharmacotherapies for smoking cessation, community pharmacists are in an optimal position to provide advice and encouragement to smokers, and can sometimes be the first and only health professional with whom smokers interact. It is fitting then, as part of this public health role, that pharmacists should be a major provider of smoking-cessation services.
Under the new contractual framework for community pharmacy in England (2005),4 the provision of opportunistic advice became an essential service, obligatory for all pharmacists. In addition, pharmacists were offered the opportunity to develop a more intensive smoking-cessation service as an enhanced service, with level 2 training to provide one-to-one smoking-cessation advice as part of the Department of Health-funded NHS smoking-cessation services.5 However, barriers to the service, such as lack of time, insufficient remuneration and a lack of counselling skills,1, 6, 7 can prevent pharmacists from making full use of opportunities to communicate with patients, and factors affecting their likelihood and propensity to do so are unknown. It is likely that practice will vary, and there will be a gap between pharmacists’ knowledge and attitudes and provision of service.8, 9
The aim of this survey was to assess the current level of service offered to clients for smoking cessation in community pharmacies in the primary care trusts of Camden, Islington, Haringey, Barnet and Enfield. It is important to assess the willingness of pharmacists to assume a proactive role in the promotion of cessation; to understand the factors that affect the way they offer advice in order to develop strategies to increase the proportion offering smoking-cessation advice, and to improve the quality of that advice.
Method
Setting and sample
Community pharmacies located in the five PCTs in north London identified from the local health authority list10 (n=298) were mailed a questionnaire, adapted from previous surveys,7,8,11 to elicit information about pharmacist and
pharmacy characteristics, smoking-cessation knowledge and training, current provision of a smoking-cessation service, content of advice, attitudes towards the provision of a service, and potential barriers and factors that facilitate the provision of a service, together with a Freepost envelope for return.
The questionnaire was piloted with a group of 20 pharmacists outside the area for content, format, relevance and clarity, and subsequently revised. The cover letter was addressed to the pharmacist-in-charge to obtain the most reliable information about the practice and activity of the pharmacy. The first mailing was in March 2006, follow-up reminders were mailed a month later with a duplicate questionnaire.
Analysis
Data were analysed descriptively using frequency measures and means for smoking-cessation activities, knowledge, attitudes and perceptions. Scores on knowledge and skills, effectiveness and importance of resources were dichotomised into high (above the median) and low (at or below the median) scores, and incorporated into a univariate analysis using chi-squared and t-tests to explore possible determinants of assuming a proactive role in offering brief advice and providing a service.
An exploratory factor analysis was conducted to examine relationships and reduce the dimensions of attitudes and perceptions of the role of pharmacists as advisers.
Results
Pharmacist and pharmacy characteristics
Responses were received from 80 pharmacists (26.9 per cent), 15.1 per cent responded only after a reminder was sent. Response rates varied by PCT. The mean age of respondents was 40.9 (standard deviation 11.9) and 58.8 per cent were male. The highest degree for 92.5 per cent of respondents was a first degree (BSc or MPharm). The mean number of years in practice was 16.8, ranging from 0.5 to 45 years. Just one respondent reported being a current smoker and 73.8 per cent had never smoked.
Almost half of the questionnaires (45 per cent) were completed by owners, 55 per cent came from pharmacists working in independent pharmacies, and 11 (13.8 per cent) were located in a food store or health centre. Independence of the pharmacy was associated with owner status. More women respondents were working in large chains, while 63.8 per cent of owners and 70 per cent of respondents from independent pharmacies were male (P=0.001). There was no difference in status by PCT.
Smoking cessation activity in community pharmacy
A large majority of pharmacists agreed with the role in health promotion and healthy lifestyle information required under the terms of the new contractual framework. Most pharmacies (90 per cent) reported displaying posters and leaflets advertising services for smoking cessation. The provision of a counselling area was common, 51.3 per cent reported having a private, and 25 per cent a semi-private, counselling area.
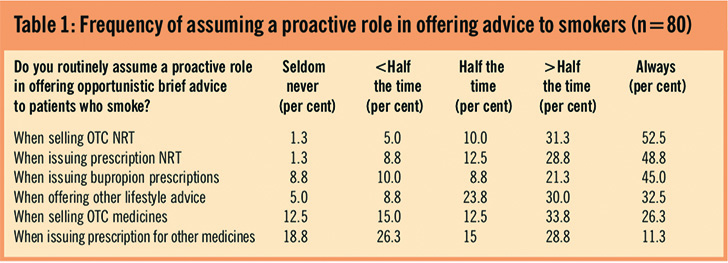
Thirty-five per cent of respondents routinely record the smoking status of patients. Although approximately half of the respondents reported always proactively offering brief advice when selling or dispensing nicotine replacement therapy (NRT) and bupropion, pharmacists less often take the opportunity to offer advice to smokers when selling over-the-counter medicines, and when dispensing other prescriptions (Table 1).
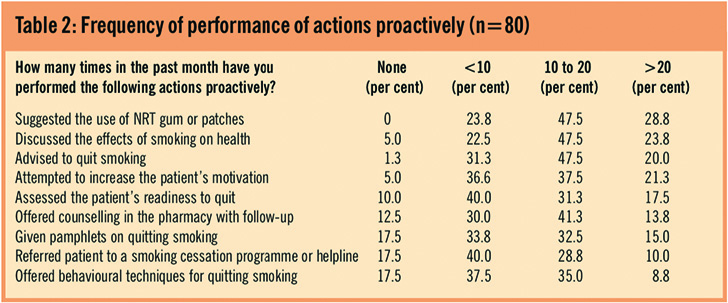
The most common brief advice offered on a proactive basis is to suggest the use of NRT, with fewer offers of programme referrals and behavioural help (Table 2).
Of the total respondents, 57 (71.3 per cent) offer a smoking cessation service and follow-up clinic on a regular or ad hoc basis, 10 (12.5 per cent) offer a service with no appointment system or follow-up, and 13 (16.3 per cent) do not offer a service. Most clinics offer six 10- to 20-minute appointments, (ranging from one to 12 appointments and five to 45 minutes).
Of the 55 respondents who gave information about the content of their counselling, over 80 per cent always address reasons for quitting, reasons for smoking and motivation, and include information-giving in the counselling session (Table 3).
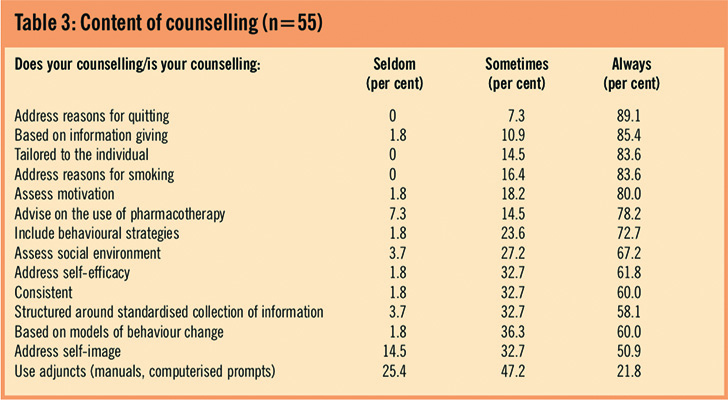
The use of pharmacotherapy and behavioural strategies are always included by a majority, but the important topics of social environment and self-efficacy are included only sometimes by one-third of pharmacists. Self-image and the use of adjuncts to help the client are not addressed or used by the majority. Most pharmacists use other materials, particularly the NHS stop smoking guide,12 and the “Helping smokers stop” guide produced by the Royal Pharmaceutical Society and the National Institute for Health and Clinical Excellence.13
Smoking cessation knowledge and training
Only 10 respondents (12.5 per cent) reported having had no training in smoking cessation, 55 (68.8 per cent) receiving training on a continuing education course, 12 (16.25 per cent) trained at university and in continuing education, and two (2.5 per cent) only at university; 80.8 per cent of those trained in continuing education received their training from the PCT.
A relatively large proportion of respondents claimed to have excellent knowledge in the use of NRT in smoking cessation (48.8 per cent) and about the effects of smoking on health (45 per cent), but few rated their knowledge of behavioural techniques as excellent (Table 4).
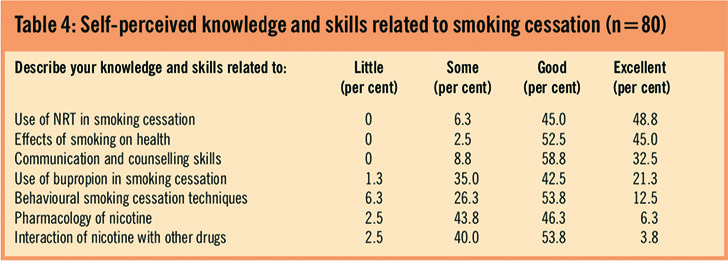
Training in smoking cessation both at university and in continuing education is weakly related to a higher total knowledge score. However, pharmacists receiving training from the PCT are more likely to highly rate their knowledge of behavioural techniques (P=0.021).
A high proportion of respondents thought that NRT, together with professional help, is very effective in helping patients to quit (82.5 per cent). Although the effectiveness of smoking-cessation programmes is also highly rated (67.5 per cent), only 32.5 per cent believe that behavioural counselling is very effective in helping patients to quit. NRT alone without professional help was considered to be very effective by fewer respondents, but pharmacists appeared to be unaware of the effectiveness of bupropion (Table 5).

Attitudes towards the provision of a smoking-cessation service
Pharmacists were asked to indicate their agreement or disagreement with 18 statements about the acceptability and effectiveness of a smoking-cessation service offered by them. A factor analysis with varimax rotation was performed as an exploratory measure to examine relationships and reduce these items to fewer subscales. Four factor scales were identified, where no item loaded less than 0.58 on only one factor (Table 6).
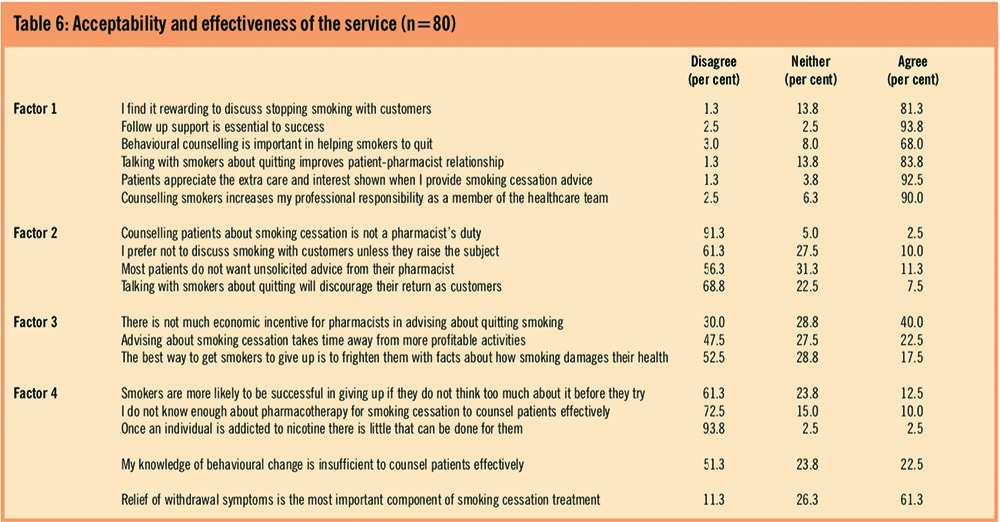
Cronbach’s alpha was used to assess reliability for each of the factors. They can be represented as:
- Positive attitudes towards service provision (19 per cent variance explained, Cronbach’s alpha=0.85), suggesting a confident and forward-looking approach to the changing role of pharmacists; high proportions of pharmacists indicated strong agreement with these statements
- Negative attitude (15.5 per cent variance explained, Cronbach’s alpha=0.75), suggesting worries about service provision, reaction from customers, and the role of pharmacists as advisers and counsellors; pharmacists generally disagreed with these statements, but responses suggested some ambivalence about being involved
- Business-oriented factors (10.1 per cent variance explained, Cronbach’s alpha=0.61), statements referring to economic incentives and taking time away from more profitable activities, which, perhaps unsurprisingly, were more salient for independent pharmacies and owners
- Methods of advising smokers (10 per cent variance explained, Cronbach’s alpha=0.68), referring more to the nature of the problem. The degree of ambivalence in responses suggests a lack of confidence in knowledge and ability to counsel successfully
Two statements relating to whether the relief of withdrawal is the most important component of treatment and knowledge of behavioural change did not fit easily into any of these dimensions. However, responses to these also suggest a lack of understanding in many pharmacists of the role of behaviour in smoking cessation. Factor scores were used as independent variables to examine predictors of the service.
Resources and barriers to the provision of a smoking cessation service
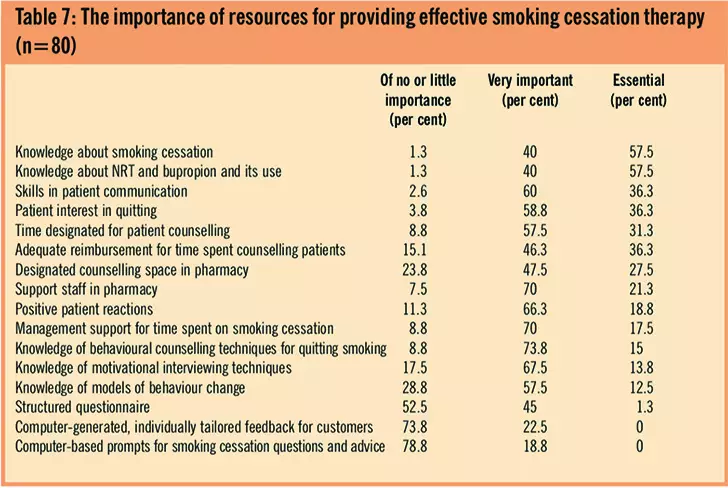
To assess perceived needs and aids to good practice as well as perceived barriers to offering a smoking-cessation service in the pharmacy, pharmacists were asked to rate the importance of certain resources for providing effective smoking-cessation therapy. General knowledge about smoking cessation and about NRT and bupropion were rated as an essential resource for providing smoking-cessation therapy by the highest number (57.5 per cent).
Communication skills, patient interest in quitting, and practical considerations, such as adequate reimbursement, time designated and designated counselling space, were high on the list, and there was a group of resources, including positive patient reactions, behavioural counselling techniques and knowledge of motivational interviewing techniques that pharmacists thought were important but not essential. Knowledge of behavioural models, structured questionnaires and computer-based prompts and feedback, which can add consistency and reliability to the advice, were considered of little importance (Table 7).

Associations and predictors of proactivity and service provision
Scores for routinely assuming a proactive role in offering opportunistic brief advice to patients who smoke were totalled and dichotomised at or below the median (total score 4-24, m=16.25, med=17.5). The number of times proactive actions were performed in the past month were totalled and dichotomised at or below the median (total score 2–27, m=14.5, med=15.5). The summary scores were used to examine the data for predictors of proactivity.
No significant associations were found between pharmacy or pharmacist characteristics and taking a more proactive role. However, pharmacists were more likely to assume a proactive role in offering advice to patients if they received training in smoking cessation while at university (P=0.04), if they considered their knowledge of communication skills and of the use of bupropion to be above the median (P=0.004, P=0.014), if their belief in the effectiveness of programmes and of behavioural counselling was above the median (P=0.006, P=0.013), and if they had a more positive attitude towards the provision of a service (P=0.002). Pharmacists were less likely to be proactive if they scored above the median on the importance of patient interest (P=0.013).
Respondents were dichotomised into service providers and non-service providers, and chi-square and t-tests carried out to examine the data for relationships and predictors of service provision.
No relationships were found between service provision and counselling area, PCT, or gender, but pharmacists were more likely to offer a service if they had over 24 years of practice (P=0.019). Training also has a clear influence on offering a service; pharmacists trained in continuing education were significantly more likely to offer a service than those not trained or trained elsewhere. However, most of this influence is accounted for by PCT training (P<0.0001).
Provision of a service is also associated with above the median knowledge of NRT (P=0.0009), with considering NRT together with professional help to be very effective (P=0.002), with scoring highly on the importance of adequate reimbursement (P=0.016), scoring significantly higher on positive attitudes (P=0.012), and having confidence in their knowledge of behavioural change to counsel patients effectively (ie, they disagree that their knowledge of behaviour change is insufficient to counsel patients effectively) (P=0.025).
Discussion
Responses from this sample of pharmacists indicate that interest in promoting a healthy lifestyle is high, and indicators of activity show that a large proportion of respondents are already providing a smoking-cessation service. Pharmacists perceived their knowledge on smoking cessation topics to be good and most pharmacists were aware which treatments are most effective. Attitudes towards the provision of a smoking-cessation service and the role of pharmacists in that provision are positive, and pharmacists appreciate the necessity for certain resources, such as knowledge of pharmacotherapy, communication and counselling skills.
Although the picture presented is positive, there are gaps and deficiencies in knowledge and services, suggesting opportunities for improvement. First, it is not common practice to identify and approach smokers, and few pharmacists document the status of patients. This is consistent with other studies.7,8,11,14 The results also suggest that many pharmacists are not comfortable with a proactive approach. Approximately half do not consistently offer brief advice when selling NRT either OTC or on prescription or when dispensing bupropion, and a smaller proportion take the opportunity to offer advice when selling or dispensing other medicines.
The second issue, and consistent with previous findings, is the deficiency in the knowledge and awareness of the role of behavioural counselling in smoking cessation. Although most respondents rate themselves highly on knowledge of the effects of smoking on health and on the use of NRT, they show less understanding of the behavioural side of the smoking habit and appeared to underrate the value of behavioural counselling as part of the treatment, showing little appreciation of the fact that behavioural counselling is an integral part of the treatment in cessation programmes. Attitude scores, although encouragingly positive about the role of the pharmacist in smoking cessation, also suggest a high emphasis on pharmacotherapy and withdrawal relief, reiterating the need for more knowledge and training in the use of behavioural and cognitive techniques to strengthen the pharmacotherapy advice given.
Thirdly, pharmacists show gaps in their application of effective advice. Too few include the important components of self-efficacy, self-image and social environment in their counselling, which are essential elements for understanding the habit for both the counsellor and the patient.
Although training, particularly when received from the PCT, is strongly associated with the provision of a service, it is weakly associated with knowledge. This suggests that either training courses do not routinely include the necessary components or that some pharmacists have an unrealistic perception of their knowledge and ability to offer effective counselling.
A World Health Organization European survey15 found that 83 per cent of pharmacists consider their knowledge to be sufficient to advise patients. However, no definition of how much knowledge is sufficient and the content of such knowledge is offered. The current data suggest a mismatch between perceived knowledge, an awareness of what constitutes sufficient knowledge, and the content of such knowledge.
Pharmacists with no training perceive their knowledge to be high, although their belief in the effectiveness of some methods contradict this claim. It is important that pharmacists are trained in theory and evidence to ensure that advice is standardised and reliably delivered. Training programmes that focus on the importance of the use of behavioural and cognitive techniques using a theoretical model of behaviour change rather than the more traditional information-giving “pharmacist as expert” model16 would improve the content of pharmacy advice programmes.
Organisational factors are also important in ensuring that smoking-cessation messages are reliably delivered. Adjuncts that facilitate the intervention, such as manuals or computerised reminders to provide advice on smoking, can help, and should form part of the strategies.17 However, the advantage of such adjuncts is not fully appreciated by pharmacists. Computer-based prompts and structured-assessment questionnaires can facilitate an intervention, provide support and give more structure to advice. Computer-based programs also enable the structuring of advice to include behaviour change based on theoretical models, and can have an empowering effect on pharmacists who may have less confidence in their ability to use these behavioural techniques.
Adequate reimbursement and negative patient reactions can be a concern. However, although provision of a service may vary according to how much control the pharmacist has over the decision, negative attitudes towards economic issues did not appear to have a negative influence on service provision. The system of reimbursement from the PCT may be instrumental in moderating and overcoming these barriers, and is, therefore, essential to prevent economic issues becoming an impediment to the provision of a service.
Limitations
It is important to note that the response rate to this survey was low. The views represented are those of a small sample of pharmacists, and we cannot assume that these respondents are representative of the target population, or of the general attitudes and concerns of pharmacists in the UK.
Data on training from Camden PCT suggest that pharmacy personnel were more likely to return the completed questionnaire if they had received recent training (within two years) from the PCT. Thus a selection bias may be operating where those pharmacists offering a smoking-cessation service were more likely to return the questionnaire, and this self-selected sample represents the best possible picture of pharmacists’ services in smoking cessation.
If we conservatively assume that the non-responders were not offering a service, the proportion of active pharmacists would reduce to 19.1 per cent, presenting a rather different picture. Similar surveys elsewhere have shown low response rates,7 and these other studies suggest that pharmacists are not routinely involved in smoking-cessation activities.
Conclusions
Pharmacists are willing to assume a health-promotion role, and opportunities offered by the front-line availability of high-street pharmacies and by PCT involvement should be exploited to the full to offer a reliable and standardised service. A system offering smoking-cessation advice in a more consistent and structured way by using a computer program to standardise and make current services more efficient should be explored. As Lancaster and colleagues stated “there is unlikely to be significant change in knowledge from new studies of training based around existing methods for smoking cessation. The development of novel approaches to smoking cessation may have implications for training studies in the future.”18
Acknowledgements
This study was funded by the North Central London Research Network (NoCLoR), and reviewed by the Camden and Islington Community Health Services Local Research Ethics Committee. I thank Neesha Patel for her help with the mailing, and the entry and analysis of data, and also the pharmacists in north London who took part. A copy of the questionnaire used is available from the author: hazel.gilbert @ucl.ac.uk.
About the author
Hazel Gilbert, PhD, C Psychol, is senior research fellow, Research Department of Primary Care and Population Health, UCL Medical School, Royal Free Campus, Rowland Hill Street, London NW3 2PF (e-mail hazel.gilbert@ucl.ac.uk).
References
- Vitale F. Professional intervention for smoking cessation: thecontribution of the pharmacist. European Journal of PublicHealth 2000;10(Suppl):21–4.
- Royal Pharmaceutical Society. Medicines ethics andpractice: a guide for pharmacists. London: RoyalPharmaceutical Society; 1995.
- Department of Health. Choosing health through pharmacy: aprogramme for pharmaceutical public health 2005–2015.London: DoH; 2005.
- Department of Health. The new contractual framework forcommunity pharmacy. London: DoH; 2004.
- Health Development Agency. Standard for training in smoking cessation treatments. London: HAD; 2003.
- Maguire TA, McElnay JC, Drummond A. A randomized controlled trial of a smoking cessation intervention based in community pharmacies. Addiction 2001;96:325–31.
- Williams DM, Newsom JF, Brock TP. An evaluation of smoking-cessation-related activities by pharmacists. Journal of American Pharmaceutical Association 2000;40:366–70.
- Aquilino ML, Farris KB, Zillich AJ, Lowe JB. Smoking-cessation services in Iowa community pharmacies. Pharmacotherapy 2003;23:666–73.
- Sinclair HK, Bond CM, Lennox AS. The long-term learning effect of training in stage of change for smoking cessation: a three-year follow up of community pharmacy staff’s knowledge and attitudes. International Journal of Pharmacy Practice 1999;7:1–11.
- Authorities and trusts. Available at www.nhs.uk (accessed 17/07/09).
- Brewster JM, Ashley MJ, Laurier C, Dioso R, Victor C, Ferrence R et al. On the front-line of smoking cessation: pharmacists’ practices and self-perception. Canadian Pharmacy Journal 2005;138:3.
- Department of Health. Stop smoking start living. London: DoH; 2007.
- McRobbie H, McEwen A. Helping smokers to stop: advice for pharmacists in England. National Institute for Health and Clinical Excellence, Royal Pharmaceutical Society and Pharmacy Health Link; 2005.
- Hudman KS, Prokhorov AV, Corelli R. Tobacco cessation counselling: pharmacists’ opinions and practices. Patient Education and Counseling 2006;61:152–60.
- Teräsalmi E, Gustafsen I, Juncher V, Djerf K. Smoking habits of community pharmacists in 12 European countries and their attitudes towards non-smoking work. Research report: pharmacists against smoking. EuroPharm Forum. Copenhagen: World Health Organization; 2001.
- Blenkinsopp A, Anderson C, Armstrong M. Systematic review of the effectiveness of community pharmacy-based interventions to reduce risk behaviours and risk factors for coronary heart disease. Journal of Public Health Medicine 2003;25:144–53.
- Lichtenstein E, Hollis JF, Severson HH, Stevens VJ, Vogt TM, Glasgow RE et al. Tobacco cessation interventions in health care settings: rationale, model, outcomes. Addictive Behaviors 1996;21:709–20.
- Lancaster T, Silagy C, Fowler G. Training health professionals in smoking cessation (review). In: The Cochrane Library, 3. Oxford: Update Software; 2003.


