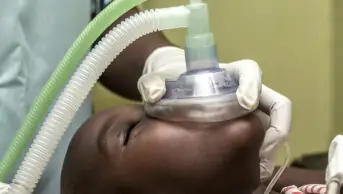
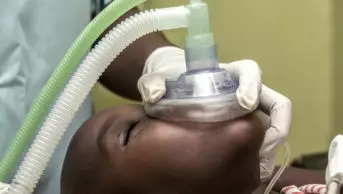
For more than 150 years, nitrous oxide has been used as an anaesthetic and anxiolytic in operating theatres, ambulance transport, dentistry, and during labour and delivery[1]. It is commonly used in the form of Entonox, a mixture of nitrous oxide and air (known as ‘gas and air’).
However, in the past 40 years, several studies have reported an increased incidence of adverse events in healthcare professionals who are regularly exposed to Entonox, in the absence of ventilation or scavenging systems, which collect and remove excess nitrous oxide and prevent it from being released back into the room[2].
The studies have highlighted three main risks. “The first one is inactivation of vitamin B12,” explains Laura Stevenson, associate chief pharmacist in aseptic services at King’s College Hospital NHS Foundation Trust, “it can cause the body to decide that vitamin B12 is a foreign particle.
“We get B12 in our food and [normally], when you eat B12 your body absorbs it, but essentially, after [Entonox exposure] it won’t get absorbed, so you become vitamin B12 deficient, which can lead to a range of issues.”
Nitrous oxide irreversibly oxidises cobalamin (AKA vitamin B12), which then inhibits the function of a crucial enzyme, methionine synthase.
Inhibition of this enzyme leads to the disruption of two vital cycles in the body — the methionine cycle and the folate cycle. Disrupting the methionine cycle can lead to a wide range of disorders, including spinal cord defects and neuropsychiatric disorders, while disruption of the folate cycle interferes with the production of blood cells in the bone marrow, resulting in megaloblastic anaemia.
As well as vitamin B12 deficiency, several epidemiological studies have linked prolonged exposure to nitrous oxide with miscarriage, congenital abnormalities and reduced rates of fertility[3].
In 1999, Bodin et al. found that babies born to women who had been exposed to Entonox at work were more likely to have a reduced birthweight and be at an increased risk of being small for their gestational age[4].
However, more research is needed to assess exactly how widespread the problems associated with prolonged Entonox exposure actually are and how long the effects could potentially last — some studies suggest that nitrous oxide is not cleared from the body as quickly as previously thought[5].
“There isn’t a huge amount of evidence to say how many cases they’ve found,” says Stevenson.
“I think that’s probably a lot to do with the fact that it’s not been tested for; until now, we haven’t been looking for it.”
The current limits
Currently, the Health and Safety Executive (HSE) — the UK workplace safety regulator — recommends that nitrous oxide concentrations averaged over eight hours (time-weighted average [TWA]) do not exceed 100 parts per million (ppm)[6]. This workplace exposure limit (WEL) is substantially higher than levels set in other parts of the world, including the United States, Australia, France and Denmark, where levels are all set at 25ppm.
“It’s an average calculated over eight hours. So, for example, you were exposed to an average of 780ppm, over eight hours — that would fall below the TWA of 100ppm,” says an expert in medical gases, who does not want to be named.
You could be exposed to quite high levels for a very short period of time and still be within the workplace exposure limit
Expert in medical gases
“So, you could be exposed to quite high levels for a very short period of time and still be within the WEL.”
In March 2023, NHS England published guidance on minimising exposure to nitrous oxide in healthcare settings in England. It outlines the mitigations that NHS trusts should “consider” to protect staff.
The guidance states that, if an NHS trust decides to use gas and air, following clinical review, [it should establish] staff risk of exposure to nitrous oxide through a clinically-led Control of Substances Hazardous to Health (COSHH) risk assessment of each space in which the gas is administered, and then introduce certain mitigations — including environmental ventilation, staff repositioning and training in the administration of gas and air — where appropriate.
Despite this, many trusts have reported levels that far exceed the WEL.
The Pharmaceutical Journal submitted a Freedom of Information (FOI) request to all NHS trusts in England to find out how many were carrying out personal sampling to assess occupational exposure to nitrous oxide and, of these, how many had returned a high result.
Overall, 130 trusts responded to the request, of which 67 (52%) had carried out personal sampling.
Of these, 26 (20%) said they had found a high result, exceeding that of the WEL. One trust said levels had been found to be 12 times in excess of the WEL and that 38 staff were affected. Four trusts said levels were more than six times the WEL, and a further nine trusts found levels that were over twice the WEL.
Reassuringly, all trusts said they had informed their staff of the results and many had taken remedial action, including hiring mobile destruction units, carrying out vitamin B12 screening and staff rotations, installing mechanical ventilation and scavenger units, and bringing in training on the use of Entonox and equipment.
Some eight trusts said they had decided to suspend Entonox — either temporarily or permanently — and others have ceased all piped supply of nitrous oxide (see Figure).
However, it is also important that trusts tackle the issue at its source.
Necessary action
Nitrous oxide is predominantly stored in manifolds. However, many hospital trusts have outdated manifolds with old piping, making the risk of leaks particularly high. Awareness of this has increased as trusts have carried out work in an effort to meet the NHS’s net zero emissions target.
Many NHS teams across the UK have recognised that their nitrous oxide manifolds are redundant or excessive, compared to actual need, and that they contribute significantly to emissions. Consequently, many manifolds have been decommissioned and the use of smaller cylinders has been explored[7].
Stevenson’s trust is based in an old Victorian hospital — with a manifold to match. As a result, a lot of effort has been put into fixing repeated leaks in the system. However, she says that, despite this, there are still breaches in levels of nitrous oxide, primarily because of the way that Entonox is used.
I’m not overly surprised that there are breaches because maternity wards were not set up to have that risk assessed
Laura Stevenson, associate chief pharmacist in aseptic services at King’s College Hospital NHS Foundation Trust
“Women are using this Entonox, the staff are in the area, and they breathe it out in the room.
“So, I’m not overly surprised that there are breaches because maternity wards were not set up to have that risk assessed until a lot of people started to figure out [the potential risks].”
The expert in medical gases says that a lot of it comes down to proper use of the Entonox devices. Some hospitals have switched from using mouthpieces to masks to limit leakages, but this has had varying success.
“I tested in two different delivery rooms where the labouring mothers were using facemasks as opposed to a bite piece to inhale Entonox,” they recall.
“In one room, the nitrous oxide levels were unexpectedly very low. Later, I spoke to the mother; it was her second baby, she’d used a bite piece in another hospital first time around and she said the facemask was absolutely fine to use.
“But the midwife explained that this woman was very concerned and did not want to cause any harm to the midwife by exhaling into the room … she made sure the mask was pressed to her face so that her breaths were exhaled via the scavenger. In the second room, where another mother was using a facemask, the personal nitrous oxide levels were higher. In this case, the partner was holding the facemask for her and I don’t think he had a good seal against the mouth, especially when she was exhaling.
“If the facemask is not used properly, then [the leakage] is far worse.”
But the solutions do not have to be complicated, or particularly expensive.
At Hull University Teaching Hospitals NHS Trust, staff replaced the seals on the Entonox system at both the bedhead panels and the demand valves, which are used when patients inhale the gas. In addition to this, they now only plug the valves into the Entonox supply when they are in use, rather than having them connected all of the time[8].
These small changes to reduce Entonox leaks enabled the trust to save gas to the value of £40,000 per year.
“We replicated that at King’s and we didn’t quite get the same results, which made us realise that we had other issues that we need to tackle,” explains Stevenson. However, she still feels it is something all trusts should be doing.
“I think it’s best practice; midwives have been so engaged and they’re happy taking [the Entonox tubes] out when they’re not using them and tying them up on the bed space; that just minimises leaks right away with absolutely no change in clinical use.”
As well as doing this, Stevenson believes that regular personal monitoring to test occupational exposure to nitrous oxide needs to included in guidance.
There are a few methods by which trusts can do this, including purchasing personal sampling tubes, which need to be sent back within two weeks, but only cost around £150 each, and G200 nitrous oxide analysers, which do not have a time pressure but are more expensive, at around £3,000 apiece.
Both can be worn by staff to measure their personal exposure to nitrous oxide, and can be used to assess their average exposure over eight hours and ensure that it is below 100ppm.
“For personal monitoring, you have to wear [the G200] in a carry case, either as a shoulder bag, or around the waist, the machine sucks air from near to the mouth via tubing,” the medical gases expert explains.
“In my view, it’s the best monitor because it displays in real time, so you can also detect leaking terminal units.”
“It should be written into guidance, to test every six months in every single room on labour ward areas,” says Stevenson.
“Then it gives [staff] peace of mind that they’ve done this, [and you can] identify [leaks] on a regular basis, [enabling] you to fix them.”
Direction is needed from the top
However, Stevenson says that, currently, trusts are not mandated to take action.
“Guidance came out from NHS England … and obviously that says you should be doing the testing.
“But [there isn’t] anything official from any governing bodies.”
The medical gases expert agrees that advice differs: “The [NHS] Health Technical Memorandum HTM 03 specifies ventilation requirements, high-level supply and low-level extract, with a minimum of 10 room air changes per hour. It does not specify a scavenger … the [Department of Health and Social Care] Health Building Note HBN09-02 recommends 15 air changes and a proprietary scavenger system.”
Responses to The Pharmaceutical Journal’s FOI request highlighted that almost a third (29%) of trusts had not carried out any personal sampling to assess individual exposure to nitrous oxide. Without testing, it is not possible to know if staff are being exposed to levels of Entonox that could be potentially harmful.
“Every employer has a legal responsibility to ensure that any hazardous materials are controlled under COSHH,” the medical gases expert says.
“And to have confidence that your staff are not exposed to levels higher than the limits specified under COSHH, you need to monitor. So, trusts are not compliant with COSHH if they haven’t actually measured these levels.
“In my experience, to comply with COSHH, delivery rooms need to have appropriate ventilation systems and scavengers.”
A spokesperson for the HSE told The Pharmaceutical Journal that its expectation from “an enforcement viewpoint” was to ensure adequate control — i.e. exposure levels that do not exceed the WEL.
“In the case of maternity, a scavenging system [that is] either integral with or in close proximity to the patient is an effective way to ensure the attending midwife is not exposed to significant levels of nitrous oxide.”
The spokesperson added that, as the likely exposure periods are not continuous throughout any given day, or likely to occur every day, significantly more data were required to make a suitable and sufficient assessment of risk.
“One way of doing this could be to start by logging exposure times each day over a period of a few weeks. When this is determined, a competent individual should be able to advise on appropriate methods of personal exposure monitoring for those personnel attending expectant mothers, who are using Entonox.”
When you speak to the midwives, they have never heard that this is a worry
Laura Stevenson, associate chief pharmacist in aseptic services at King’s College Hospital NHS Foundation Trust
Part of the problem, Stevenson says, is that many members of staff are still not aware that occupational exposure to Entonox is an issue.
“When you speak to the midwives, they have never heard that this is a worry,” says Stevenson.
“It’s not something that’s done on their induction, it’s not something that health and safety even really knew about … that’s the biggest concern on my end … that people aren’t [being] told about it.
“People are starting to realise more how dangerous it is for the environment, but not necessarily how dangerous it is for people.”
The medical gases expert says that, as a standard, if trusts want to make sure that their staff are always protected, they need to have a scavenger and they need to have the compliant ventilation and low-level extraction.
“Even in the most compliant hospitals delivery rooms, with suitable ventilation and scavenger systems, there will be Entonox present in the room — I’ve seen it happen, especially in the second stage of labour when the mother is pushing, they’ll breath in, hold it, brace and push and then exhale into the room.
“And depending on where [the midwife] is standing and how the room is set out … if the labouring mother exhales into the room, the midwife may well inhale exhaled breath before it is extracted.”
Responding to the FOI figures, a spokesperson for HSE told The Pharmaceutical Journal it was “vital” that exposure risks to staff at maternity wards were “properly managed”.
“We are aware that there have been issues with controlling exposure to nitrous oxide at a number of NHS maternity units and any specific complaints about this have been followed up, as will any others.
“Where it is necessary to use nitrous oxide, employers are required to ensure that exposure does not exceed the WEL and that compliance with COSHH is achieved.”
NHS England declined to comment.
- 1van Amsterdam J, van den Brink W. Nitrous oxide–induced reproductive risks: Should recreational nitrous oxide users worry? J Psychopharmacol. 2022;36:951–5. doi:10.1177/02698811221077194
- 2Pickles J. Guide to scavenging of nitrous oxide. Dental Nursing. 2016.https://ramedical.com/wp-content/uploads/2016/08/DN-Guide-to-Scavenging.pdf (accessed May 2023).
- 3Nitrous oxide: updated harms assessment. Advisory Council on the Misuse of Drugs. 2023.https://www.gov.uk/government/publications/nitrous-oxide-updated-harms-assessment/nitrous-oxide-updated-harms-assessment-accessible (accessed May 2023).
- 4Bodin L, Axelsson G, Ahlborg, Jr G. The Association of Shift Work and Nitrous Oxide Exposure in Pregnancy with Birth Weight and Gestational Age. JSTOR. 1999.https://www.jstor.org/stable/3703564 (accessed May 2023).
- 5Henderson KA. Occupational exposure of midwives to nitrous oxide on delivery suites. Occupational and Environmental Medicine. 2003;60:958–61. doi:10.1136/oem.60.12.958
- 6EH40/2005 Workplace exposure limits. Health and Safety Executive. 2020.https://www.hse.gov.uk/pubns/priced/eh40.pdf (accessed May 2023).
- 7Morrison A. Interim protocol for decommissioning of nitrous oxide manifolds DL (2021) 41 . Scottish government. 2021.https://www.sehd.scot.nhs.uk/dl/DL(2021)41.pdf (accessed May 2023).
- 8Hospital gas emissions slashed at Women and Children’s Hospital. NHS Hull University Teaching Hospitals. 2022.https://www.hey.nhs.uk/news/2022/05/17/hospital-gas-emissions-slashed-at-women-and-childrens-hospital/ (accessed May 2023).