Since it was first made available on the NHS in 1961, there is no doubt that ‘the pill’ has been a stalwart of contraception.
More than 99% effective at preventing pregnancy — when taken correctly — the combined hormonal contraceptive pill provided women with the first reliable, biological form of contraception.
In 2017/2018, more than 3.1 million people were taking the combined or mini pill1.
However, the picture has shifted over the past decade. NHS data on sexual and reproductive health services in England, published in 2025, show a 63% decrease in usage of oral contraceptives over the past ten years — from 426,800 users in 2014/2015 to 159,800 users in 2024/20252.
The data also reveal a 49% increase in natural family planning over the same period — from 7,700 in 2014/2015 to 11,500 in 2024/20252.
Figure 1: Oral contraceptives and natural family planning data from 2014/2015 to 2024/2025
Simultaneously, the abortion rate has hit a record high. According to Department of Health and Social Care data for 2023 — the latest available — there were almost 278,000 abortions in England and Wales, which is an 11% increase compared with 2022 and the highest rate since the Abortion Act was introduced in 19673.
The shift away from hormonal contraceptives has been termed ‘hormone hesitancy’ and sparked a study, published in BMJ Sexual and Reproductive Health in 2025, which compared self-reported contraceptive methods among 33,495 patients who presented for abortion to the British Pregnancy Advisory Service in 2018, with 55,055 patients presenting for abortion to the service in 20234.
The researchers found that self-reported use of fertility awareness-based methods of contraception around the time of conception among patients increased from 0.4% in 2018 (n=129/33,495) to 2.5% in 2023 (n=1,364/55,055), while use of hormonal methods of contraception decreased from 18.8% in 2018 (n=6,289/33,495) to 11.3% in 2023 (n=6,215/55,055)4.
In addition, those reporting using no contraception at the time of conception increased by 14%, from 55.8% in 2018 (n=18,703/34,495) to 69.6% in 2023 (n=38,336/55,055)4, the study results revealed.
It is therefore undeniable that women are moving away from traditional methods of contraception, but what is behind these climbing rates of women’s rejection of hormonal contraception?
Role of social media
“I think one of the main culprits has got to be social media and the misrepresentation of hormonal contraception on social media,” says Zara Haider, president of the College of Sexual and Reproductive Healthcare, and sexual and reproductive health consultant.
“I know that hormonal contraception doesn’t suit everybody, but there are some people that it would absolutely suit but they are seeing and hearing stuff on social media. It’s totally unregulated, no evidence base, but they are absolutely taking it to heart and thinking that’s what’s going to happen to them,” she adds.
“And then they tell their friends, and then they tell their family, and it’s a snowball effect.”
Haider says TikTok and Instagram are the likely offenders. “People like short, snappy, bite-sized bits of information, that’s entertaining as well. And I think TikTok and Instagram really have that kind of market,” she explains.
Maryam Nasri, a consultant in sexual and reproductive health at Central Middlesex Hospital, says patients frequently cite these apps when voicing their concerns. “[Patients] mention TikTok a lot and sometimes they’re afraid to tell us where they’ve heard it so they’ll say, ‘I’ve just read it online’.”
She says patients’ main concern is that hormonal contraception will affect their fertility. “They always say ‘It’s going to affect my fertility, isn’t it? Am I going to be as fertile as I was before?’”
Nasri adds that patients are also concerned about its effect on their libido. “In some people, hormones do decrease libido, but it’s not a universal effect,” she says.
“In the most worrying cases, they think that it’s carcinogenic. Now we know of its role in breast cancer, but actually, obesity and alcohol have got a much higher risk of affecting your future cancer risk.”
The Pharmaceutical Journal searched ‘the pill’ and ‘birth control’ on TikTok. Among the top videos under the search terms was a clip of psychologist Sarah Hill on the Diary of a CEO podcast — which has 4.5 million followers on TikTok — claiming that the pill “changes who a woman is” by changing her hormones, along with impacting a woman’s ability to handle stress, mental health and libido.
In another video from influencer account Rosie and Harry, which has 5.6 million followers, Rosie Daniels says the pill “ruined my body and covered me in psoriasis”, while another video claims that gynaecologists are not “telling their patients how bad birth control is” and goes on to list “blood clots, high cholesterol, increased risk of heart disease”.
Some women are also increasingly concerned about whether hormonal contraception may be contributing to fatigue, brain fog or a general sense of ‘hormonal imbalance’, even if blood tests are normal
Deborah Evans, clinic director and superintendent pharmacist at Remedi Health in Winchester, Hampshire
Figure 2: Screenshots from TikTok
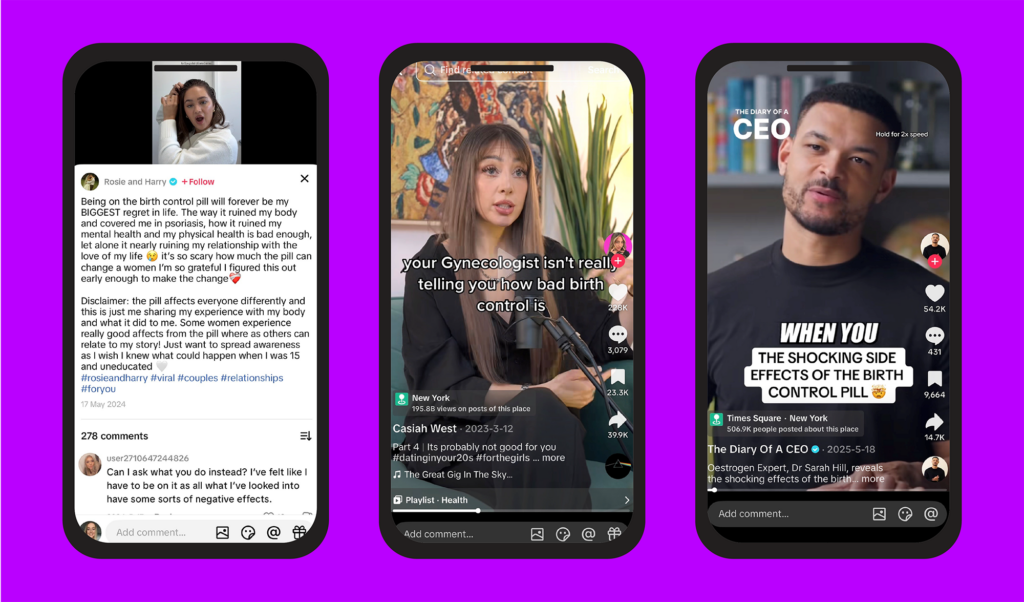
TikTok / The Pharmaceutical Journal
The NHS lists side effects and risks associated with use of the combined pill, including the potential risk of a blood clot in the lung or leg, a blood clot causing heart disease, a blood clot causing a stroke and elevated risks of breast and cervical cancer while taking and for ten years after stopping the pill. These risks are also included in patient information leaflets for the pill.
However, no direct cause has been found between the pill and its effect on mental health, libido or skin conditions.
Deborah Evans, clinic director and superintendent pharmacist at Remedi Health in Winchester, Hampshire — which provides a private contraception service — says women commonly raise concerns about hormonal contraception, which has increased in recent years.
“The most frequent worries relate to mood changes (including anxiety, low mood and irritability), weight gain, reduced libido, skin changes such as acne, and irregular bleeding patterns, particularly with progestogen-only methods,” she explains.
“Some women are also increasingly concerned about whether hormonal contraception may be contributing to fatigue, brain fog or a general sense of ‘hormonal imbalance’, even if blood tests are normal,” she says.
“Many women refer directly to social media, particularly TikTok, Instagram and podcasts, and they often mention content about ‘coming off the pill’, cycle tracking, or claims that hormonal contraception disrupts natural hormones or fertility.”
“This can be helpful in prompting engagement, but it can also increase anxiety when risks are presented by people who are not necessarily medically qualified and out of context.”
Women are using apps that are actually meant for menstrual tracking as something to stop getting pregnant — they’re not meant for that
Zara Haider, president of the College of Sexual and Reproductive Healthcare and sexual and reproductive health consultant
Fertility awareness apps
Alongside this deluge of content on the supposed harms of the pill and other hormonal contraceptives is content promoting the use of fertility-awareness apps.
These apps primarily track women’s menstrual cycles, through women inputting when their period begins and ends and logging symptoms throughout their cycle to predict when ovulation and menstruation will occur.
One of the most popular cycle-tracking apps ‘Natural Cycles’ is the only app to be certified as a contraceptive in the UK and internationally. It was certified in the EU in 2017 and in the United States in 2018.
Users input their basal temperature daily — either by using a thermometer or syncing the app with a wearable device, such as an Apple Watch — along with their symptoms. The app then analyses the data to determine where a woman is in her menstrual cycle and predicts her fertility on the given day — either categorising it as a green ‘not fertile’ day or red ‘fertile’ day. This can be switched for women who are planning to become pregnant.
Natural Cycles is claimed to be 93% effective with typical use and 98% effective with perfect use.
However, it has faced backlash over unintended pregnancies and, 2018, advertising of the app was banned in the UK by the Advertising Standards Agency over inaccuracy claims.
At the time of going to press, Natural Cycles claimed it had 4 million registered users.
“There is definitely a place for Natural Cycles, but we always ask patients, ‘What happens if you fall pregnant?’” Nasri says.
“There’s a high risk associated with fertility awareness methods that they can fall pregnant. If they’re going to welcome it, that’s fine, but if it’s going to cause anxiety and other consequences of an unplanned pregnancy, then they should find a more reliable contraceptive method.”
Haider agrees. “Women are using apps that are actually meant for menstrual tracking as something to stop getting pregnant — they’re not meant for that.”
“They are fantastic in the clinic, but for the right purpose. I fit a lot of coils in my service and one of the questions you ask somebody before you fit a coil to make sure there’s no pregnancy risk is, when was the first day of your last period?” she adds.
“Back in the day, before these apps, people used to look up to the sky to find inspiration and have no clue; nowadays, they reach into their back pocket, they pull out their phone, and they produce one of these clever apps, and it will absolutely tell you when every last period was.”
She says that they’re “brilliant for allowing women to get in touch with their bodies and work out what’s going on, but they’re not meant to be used, by and large, for preventing pregnancies”.
Evans acknowledges a shift in women seeking fertility awareness approaches but says this is “balanced by many still actively seeking hormonal solutions for symptom control”.
“What has changed more noticeably is a reluctance to commit to long-acting methods, such as implants or coils without very detailed discussion. Many women express a preference for methods they perceive as more easily reversible, such as the pill, as it feels within their control and simpler to stop if side effects occur.”
NHS data on sexual and reproductive health services show that, in 2014/2015, 346,100 women were using long-acting reversible contraceptives, compared with 263,200 in 2024/2025, which represents a 24% decrease2.
We’re trying to counter [misinformation] with the right information, with evidence-based, interesting information
Zara Haider, president of the College of Sexual and Reproductive Healthcare and sexual and reproductive health consultant
Lack of education
While these apps may be increasing women’s knowledge about their bodies, Nasri highlights a lack of education around contraceptives, starting in schools.
“We don’t have the best sex education. It might talk about condoms, but it doesn’t talk about other contraception.”
Haider also agrees education needs to begin at school. “I know work is going on to try and improve what’s out there, improve signposting to sexual health clinics, improve signposting to information about sexual health and contraception, but I think there is room for improvement, and it’s about getting that basic education starting young.”
Government guidance on sex education for the 2026 curriculum says this should include “the facts about the full range of contraceptive choices, efficacy and options available, including male and female condoms, and signposting towards medically accurate online information about sexual and reproductive health to support contraceptive decision-making”.
Of course, young people are likely to come across inaccurate, unregulated information online.
Haider says better regulation on apps would help, “but how you do that would be quite tricky”.
“We’re trying to counter [misinformation] with the right information, with evidence-based, interesting information.”
However, she says it’s not just young people lacking in education. “I think it’s across the board. We’ve got women coming out of long-term, stable relationships entering new relationships, who were quite in the dark about sexual health, maybe never having used contraception, never having used barrier methods before. We’ve certainly got a rise in sexually transmitted infections in the older age group.”
She adds that there is also a lack of education around the non-contraceptive benefits of contraception. “So, helping to control those heavy periods, helping to control that pelvic pain, that cyclical pain, and other cyclical symptoms. Hormonal contraception could have a big part to play in that, but people read stuff on social media, and they’re totally put off even engaging in those conversations”.
Nasri echoes this. “For example, the Mirena coil — you can use it for contraception, but you can also use it to reduce heavy menstrual bleeding. It has actually reduced the rate of hysterectomy for heavy menstrual bleeding.”
The coil can also be used as part of hormone replacement therapy in women, as it provides progesterone and protects the lining of the womb against oestrogen.
What else could it be?
There may be other factors at play in the decline of hormonal contraception.
“We know that over time, a lot of the contraception services have closed down, so it’s becoming less and less easy for people to access the services that they want in a timely way closer to home,” says Haider.
Experts have attributed the closure and reduction of contraception services in England to a combination of chronic underfunding of public health, fragmented commissioning responsibilities and the lasting impact of the COVID-19 pandemic5.
At an evidence session held in 2025, the Health and Social Care Committee heard how the “training pathway for sexual and reproductive healthcare specialists is six years post-foundation, with intense competition” and that “a 2023 workforce survey suggested one-third of the sexual health workforce was expected to retire by 2028”6.
A report by HIV charity Terence Higgins Trust also found that in 2023, waiting times for face-to-face appointments available to book via telephone averaged 13 days, which rose to 19 days in rural parts of England7.
There is also the fact that a woman taking the pill is taking the same pill that was available 60 years ago and contending with the same side effects, giving rise to the argument: why should they still put up with that? Particularly in the context of trials for the long-awaited male contraception being halted over the same “undesirable side effects” that women experience, such as weight gain, acne and mood changes8.
This refusal to tolerate side effects that were once dismissed as the cost of prevention, alongside the growing influence of social media and overstretched sexual health services, suggest the fall in use of hormonal contraception is not the product of a single cause but a collision of cultural, structural and personal shifts.
The result? A generation rethinking what control over their own fertility should look like.
- 1.Davis N, McIntyre N. Revealed: pill still most popular prescribed contraceptive in England. The Guardian . 2019. https://www.theguardian.com/uk-news/2019/mar/07/revealed-pill-still-most-popular-prescribed-contraceptive-in-england
- 2.Sexual and Reproductive Health Services, England (Contraception), 2024-25. NHS England. 2025. https://digital.nhs.uk/data-and-information/publications/statistical/sexual-and-reproductive-health-services/2024-25/methods-of-contraception#uptake-of-user-dependant-contraceptives
- 3.Abortion statistics commentary, England and Wales: 2023. Department of Health and Social Care . 2026. https://www.gov.uk/government/statistics/abortion-statistics-for-england-and-wales-2023/abortion-statistics-commentary-england-and-wales-2023
- 4.McNee R, McCulloch H, Lohr PA, Glasier A. Self-reported contraceptive method use at conception among patients presenting for abortion in England: a cross-sectional analysis comparing 2018 and 2023. BMJ Sex Reprod Health. 2025;51(3):186-190. doi:10.1136/bmjsrh-2024-202573
- 5.Hall R. Access to contraception has got harder in England, top doctor says. The Guardian. 2023. https://www.theguardian.com/society/2023/jun/05/access-to-contraception-has-got-harder-in-england-lesley-regan-davina-mccall
- 6.Sexual health services undervalued and under-resourced after a decade of being overlooked. UK Parliament . 2025. https://committees.parliament.uk/committee/81/health-and-social-care-committee/news/210106/sexual-health-services-undervalued-and-underresourced-after-a-decade-of-being-overlooked/
- 7.Over-stretched and under strain: A Mystery Shopper Approach to Access to Sexual Health Services in England, Scotland and Wales. Terrence Higgins Trust. 2023. https://tht.org.uk/sites/default/files/2023-07/Mystery%20shopper%20report%20(28%20july%202023%20update).pdf
- 8.Gorvett Z. Many side-effects deemed unacceptable in the male pill have been plaguing women for decades. Is there a double standard? BBC. 2023. https://www.bbc.co.uk/future/article/20230216-the-weird-reasons-male-birth-control-pills-are-scorned
2 comments
You must be logged in to post a comment.



What about EHC?
The Natural Cycles app is a CE-marked digital contraceptive, clinically validated through peer-reviewed studies to prevent pregnancy. Unlike general period-tracking apps, our algorithm analyses multiple data inputs and is specifically designed to account for cycle variability. As a regulated medical device, we're required to continuously monitor real-world effectiveness, and our data consistently meets or exceeds our published rates – 93% effective with typical use and 98% effective with perfect use. We understand that, as a relatively new contraceptive method, there's confusion in the medical community about the differences between the Natural Cycles app and period trackers, and we're actively working to change that.