Shutterstock.om / JL
Its launch was delayed by the political wrangling over Brexit, but what is a few months’ wait when the health service in England now has a ten-year plan for its future? Running at nearly 140 pages, the ‘NHS Long-Term Plan’ is a major milestone for a service that has — at times over the past few years — appeared to be drifting rudderless.
NHS England claims that the plan will save almost half a million lives, harness the power of technology to make the health service fit for the future, and provide the biggest ever national investment in mental health services. And it is excellent news for the status of pharmacy, with the profession mentioned frequently as a solution to boosting primary care workforce capacity and improving the use of medicines in the NHS.
But it comes with some major health warnings. It outlines how the service will spend the extra £20.5bn per year promised by the government over the next five years, but no further funding is promised after that.
The most radical idea contained in the document suggests that around a third of outpatient hospital appointments will be avoided through digital GP appointments and redesigned hospital support, and pharmacists are allocated a significant role in improving primary care in particular. But the plan makes little mention of community pharmacy at all.
Indeed, the biggest omission is any specific proposal on how the planned transformation of primary care and prevention in the health service will be staffed. There is mention of a plan to “substantially expand the number of clinical pharmacists” and a workforce plan is promised later in 2019.
But deep cuts have since been announced in hospital pharmacy training, and pharmacy schools are struggling to fill their places. The plan promises “to make greater use of community pharmacists’ skills” and in the same breath says it will be “exploring further efficiencies through reform of reimbursement and wider supply arrangements”.

Source: Nic Bunce / The Pharmaceutical Journal
Sandra Gidley, chair of the Royal Pharmaceutical Society English Pharmacy Board, welcomes pharmacist recognition in the NHS plan, but says more detail is required
On the whole, the plan has been welcomed across pharmacy. Sandra Gidley, chair of the Royal Pharmaceutical Society English Pharmacy Board, gives a qualified response: “This is the first document [in which] there have been consistent mentions of the role of pharmacists and we have to take encouragement from that,” she says. “But we need to see more detail of what is planned — the devil is in the detail.”
Primary care networks
Keith Ridge, chief pharmaceutical officer at NHS England, says the plan is “full of fantastic opportunities for pharmacy professionals working together across all sectors”. And the long-term plan highlights the “essential role” of pharmacists in delivering the schemes and initiatives that it proposes.
There is heavy mention of pharmacist involvement in one of the plan’s central ideas — plans for so-called “primary care networks” to be implemented across the country (see Box 1).
Box 1:
What is a primary care network?
A primary care network is a group of GP practices working together with community services, pharmacy, the voluntary sector, social care and even hospitals to provide effective, joined-up care for that area.
The government’s ‘Refreshing NHS plans for 2018/2019’ report set a goal for clinical commissioning groups (CCGs) to encourage each GP practice in England to become part of a primary care network.
The ‘NHS Long-Term Plan’ says £4.5bn will fund the expansion of community multidisciplinary teams and outlines that GP practices in a local area would enter into a “network contract” with a “designated single fund, through which all network resources will flow”.
One of the earliest and most widespread forms of the network is the primary care home project, which launched in October 2015, with 15 pilot regions chosen in December 2015.
The model brings together a range of healthcare professionals, including pharmacists, to look after a population of between 30,000 and 50,000 patients.
According to the National Association of Primary Care (NAPC), a “mature” primary care home operates “like a mutual organisation or society with strong social values”. It could involve establishing a “company in which clinicians and managers can become directors”, who may wish to employ other healthcare workers such as pharmacists. Alternatively, providers, including community pharmacies, could work together through “an alliance contract”. Primary care homes also operate under a single, whole population-based budget.
Pharmacy is already involved in more than 200 established primary care homes. In a document jointly published by several pharmaceutical bodies, including the NAPC, the Royal Pharmaceutical Society and the Pharmaceutical Services Negotiating Committee, pharmacists are said to be “conducting medication reviews, helping reduce unnecessary medications and supporting patients who are taking multiple medications regularly”.
The ‘NHS operational planning and contracting guidance for 2019/2020’ report required CCGs to commit “£1.50/head recurrently to developing and maintaining primary care networks so that the target of 100% coverage is achieved as soon as is possible and by 30 June 2019 at the latest”.
According to the plan, networks of GP practices will be offered a share of £4.5bn of extra funding allocated to setting up bodies covering populations of up to 50,000 patients, with multidisciplinary community teams staffed by “pharmacists, district nurses, community geriatricians [and] dementia workers” equipped to carry out a wider range of care outside hospital (see Box 2).
Within these networks, pharmacists will be supported to “find and treat people with high-risk conditions”, such as atrial fibrillation and cardiovascular disease, and will “undertake a range of medicine reviews, including educating patients [with asthma] on the correct use of inhalers”. They will also deliver enhanced support for people in care homes, working with colleagues in the acute sector and in community pharmacy.
Gidley warned that pharmacy involvement with the new primary care networks will “probably will need some further thought”. This is because some of the models of joint primary care working that are most similar to the proposed networks “are very GP-centric”.
She added: “It’s our job to ensure that pharmacists have a high-profile role in those networks and that their skills are used.” Speaking in a personal capacity as a community pharmacist, Gidley explained: “I would want to ensure that, for example, these asthma reviews are undertaken by pharmacists in the community, as well as in a doctor’s surgery, because there are many pharmacists with great expertise.”
What we’re trying to do in the primary care home is not move the pharmacist out of where they are historically and sometimes best placed — the community pharmacy
Pioneers of the primary care network idea say that community pharmacy will continue to have a role (see Figure 1). James Kingsland, president of the National Association of Primary Care, which founded the first primary care home — a type of network praised by NHS England chief executive Simon Stevens — suggests community pharmacy is “best placed” to provide certain community services.
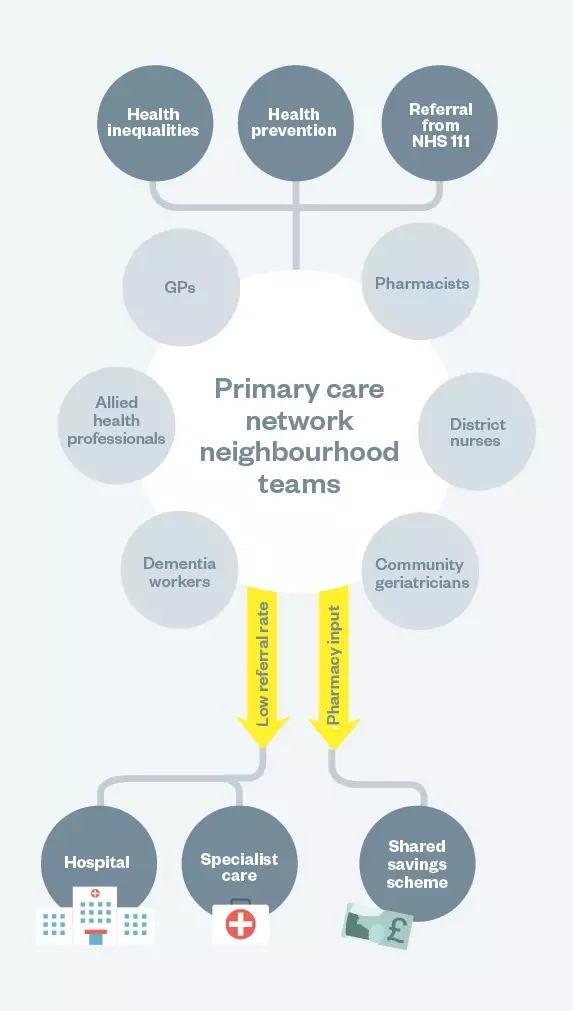
How a primary care network might work
Source: JL The Pharmaceutical Journal
This diagram illustrates how a primary care network could be implemented, based on information from the ‘NHS Long-Term Plan’

Source: National Association of Primary Care
James Kingsland, president of the National Association of Primary Care, says community pharmacists are best placed to provide many services
“It’s the community pharmacist working as part of a multidisciplinary team, and what we’re trying to do in the primary care home is not move the pharmacist out of where they are historically and sometimes best placed — the community pharmacy — where they have their own interactions with patients,” says Kingsland.
When employed in general practice, pharmacists “quickly become part of a one-team approach”, he says, which has “rapid benefits” initially, but without recurring funding some GPs are having to “shed the cost” of their employed pharmacist after funding has run out.
“The primary care home is a longer outlook where the community pharmacy starts to gain more confidence about being part of a collaborative network,” explains Kingsland. “You’ve got to have a team-based approach where community pharmacy feels part of the developmental process of the primary care home, and as part of that team rather than just another agency giving [a] service to an individual patient.”
Box 2: View from a pharmacist working as part of a primary care network
As a pharmacist working at the Beacon Medical Group primary care home in Devon, Robin Conibere says plans to expand primary care networks nationally with heavy involvement from pharmacy is “a really good move”.
“From the pharmacist in general practice pilot so far, we’re obviously proving that we’ve got a valuable contribution to make and the more pharmacists in practices the better,” he says.
On a day-to-day basis, Conibere, who is directly employed by the Beacon Medical Group, which was formed as a merger of three existing GP practices and covers around 33,000 patients, says he spends “roughly 50% [of his time] doing back-office audits and medication safety reviews, and dealing with [other] tasks” and the rest doing patient-facing care — “either seeing patients in clinics [or] doing medication reviews”.
He adds: “I also help out with our urgent care team, which is a multidisciplinary [team] where I will see patients with acute conditions and manage them within my competence, and if there’s anything that [I can’t do], I’ve got a paramedic next to me on one side, I’ve got an advance nurse practitioner on the other side and we’ve got a team of GPs who rotate through the urgent care team as well.
“Sometimes when you’re in community [pharmacy], you come across things that are frustrating and trying to get hold of a prescriber or a GP to sort them out is nigh on impossible.
“But by having us here in the practice, pharmacists normally have a solution to their problems pretty quickly.”
The Beacon Medical Group was one of the first 15 primary care homes to be set up and since then, Conibere says the centre has seen “savings on the medicines spend”.
“As a profession, we are very savvy to the cost-effective prescribing of medicines and if we can see an opportunity to do something that can save the system money then we’ll do it — as long as it’s in the best interest for the patient,” he says.
Digital future
There are some new opportunities for community pharmacy announced in the plan (see Box 3). NHS England told The Pharmaceutical Journal that it is now working with GP practices, community pharmacies and commissioners on establishing a GP-to-community pharmacy referral pilot programme, described as “pharmacy connection schemes for patients who don’t need primary medical services”. This is expected to begin later in 2019 at sites across England before a wider rollout.
It will be important to ensure sufficient numbers of patients are referred to community pharmacies and for front-line pharmacists to excel in providing assessment, advice and management of those patients
And although it has not been confirmed yet, a national rollout of the Digital Minor Illness Referral Service (DMIRS), under which NHS 111 refers patients to community pharmacy after they have been assessed by a call adviser, is likely. Andre Yeung, pharmacy local professional network chair for Cumbria and the north east of England — where the service was first piloted in December 2017 — says it represents “a fantastic opportunity” for community pharmacy to demonstrate how it can support patients to manage acute minor illness.
He adds: “It will be important to ensure sufficient numbers of patients are referred to community pharmacies and for front-line pharmacists to excel in providing assessment, advice and management of those patients.”
The long-term plan may also mark a return for plans to increase “hub-and-spoke dispensing” in community pharmacy, as part of the search for “further efficiencies”.
NHS England told The Pharmaceutical Journal that it intends to use new technology and automation to increase the efficiency of dispensing while freeing up clinical time for pharmacists to spend caring for patients. To achieve this, it confirmed it was looking into changes to some government regulations, including around hub-and-spoke dispensing — a model that the government considered reforming in 2016 before abandoning proposals after pharmacy representative bodies raised questions over whether the model was safe and how it would comply with the Falsified Medicines Directive (FMD).
The model involves sending prescriptions to a dedicated ‘hub’ for assembling, dispensing and labelling before being transferred to a local ‘spoke’ pharmacy for a patient to pick up or for delivery to a patient’s home.
No further details on this have been provided, but this could create an opportunity for online pharmacies to become increasingly involved in the dispensing model for high street pharmacies. Now Healthcare Group, an online pharmacy that dispenses around 20,000 prescriptions per month, believes this opens the door for the company to act as “a hub for community pharmacies, bridging a gap and meeting the aims set out by the NHS to free up time for community pharmacists to spend with patients”.
It remains to be seen if this is what NHS England has in mind. The Pharmaceutical Services Negotiating Committee says it still has concerns over the hub-and-spoke system that it needs to discuss with the government, including how it would comply with the FMD, which is due to go live in February 2019, and what the model “would mean for professional liability”.
Bolstering the workforce
An analysis of the NHS Long-Term Plan by The King’s Fund, an independent think tank, indicates that the workforce is one of the biggest risks to the entire plan. “Whether the plan can be delivered relies critically on tackling workforce shortages,” it says.
A workforce implementation plan, which was promised in the long-term plan and is due to be published in 2019, will include input from chief professional officers, including Ridge.
But pharmacists have already raised concerns over workforce shortages, with contractors telling the General Pharmaceutical Council in December 2018 that community pharmacies have had to “limit” services to maintain safe staffing levels.
And the plan was undermined by a subsequent announcement a few days later from Health Education England saying it would be cutting support funding for NHS preregistration training places across England to 75% from September 2020.
Further criticism comes from the Pharmacists’ Defence Association (PDA), which says it is “dismayed” that the document refers to “clinical pharmacists” rather than community pharmacists.
We believe the workload will be unmanageable without the appropriate use of the whole pharmacy workforce
“There are several activities which the paper ascribes to ‘clinical’ pharmacists in primary care networks but which we believe could (and should) also be provided by pharmacists in the community pharmacy network to spread the load,” says a spokesperson for the PDA.
“Indeed, we believe the workload will be unmanageable without the appropriate use of the whole pharmacy workforce.”
Gidley echoes the PDA’s points, calling for “these ambitious plans … to be underpinned with a comprehensive strategic approach to educating and training the workforce for the future, especially by investment in foundation training and professional development for pharmacists”.
Exactly what the long-tem plan will mean for the NHS — and pharmacy in particular — will only be known after a decade, but for some, the NHS has to get these changes right.
Kingsland suggests the NHS “may never recover” from a failure to deliver. “If new leaders in NHS England or the Department of Health and Social Care decide on a different tack, I don’t think they’ve got the support of the service or the morale in the service to think of something different,” he says. “If someone comes along with a new plan in two years’ time, I think it could be a fatal wound to the NHS.”
Box 3: What else does the ‘NHS Long-Term Plan’ propose for pharmacy?
- Primary care networks will be linked with care homes over the coming decade, and residents will be given “pharmacist-led medicine reviews where needed”;
- The initiative to stop overmedication of people with a learning disability, autism or both will be expanded in an effort to curb the number of people inappropriately prescribed psychotropic medicine;
- The NHS will set up a “shared savings scheme” that will see primary care networks benefit from actions such as reducing overmedication through pharmacist reviews;
- All providers will be expected to implement electronic prescribing in an effort to reduce errors by up to 30%;
- From 2019, the NHS will start offering whole-genome sequencing to all children with cancer for a more precise diagnosis and more personalised treatments;
- Community pharmacists will provide NHS Health Checks while pharmacists in primary care networks will be supported to “find and treat people with high-risk conditions”.