Science Photo Library
After reading this article, you should be able to:
- Recognise the common signs and symptoms caused by benign prostatic hyperplasia (BPH);
- Be familiar with the various pharmacological treatments for BPH and their associated side effects;
- Have an understanding of non-pharmacological treatment options and self-care advice for patients.
Benign prostatic hyperplasia (BPH) is one of the most common urological conditions among males, with an estimated 3 million affected in the UK. The incidence of BPH is approximately 50% in males aged 60–70 years, increasing to 90% in males aged over 80 years[1,2].
BPH is characterised by the non-malignant proliferation of glandular epithelial tissue and stromal components of the prostate. The main clinical manifestations of BPH are lower urinary tract symptoms, which considerably reduce men’s quality of life[3,4]. Patients with BPH commonly present in primary care to their GP or community pharmacist, but more complex cases can present in a hospital setting if red flag symptoms are present.
The role of the pharmacist is inextricably linked to the management of BPH, from initial presentation and diagnosis, to pharmacological management. The various treatment options available makes pharmacist involvement crucial to optimising treatment, ensuring positive outcomes and minimising adverse effects.
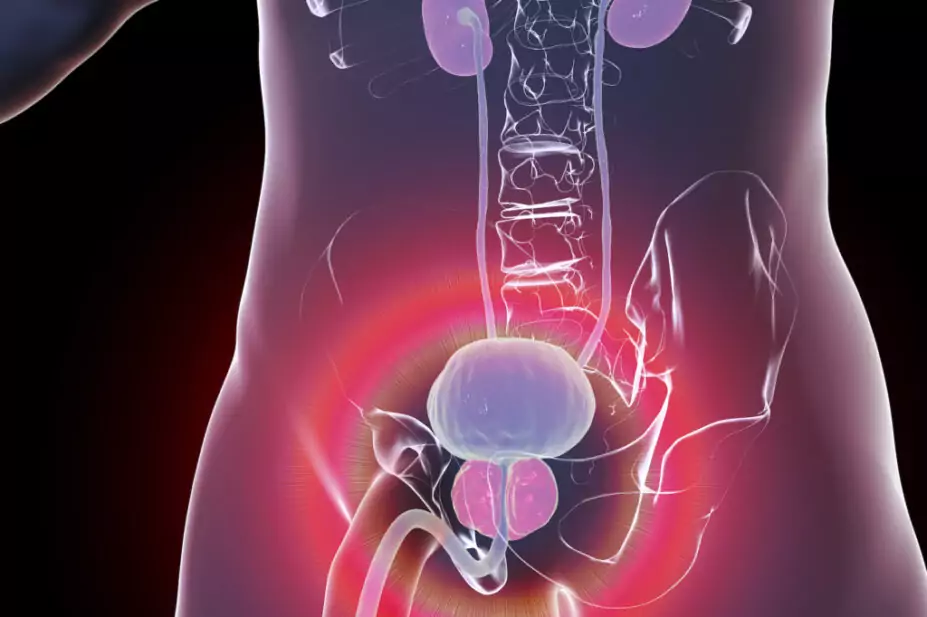
The prostate is a small, walnut-sized organ located under the bladder, through which the urethra runs. It is composed of epithelial cells, which are secretory, and stromal cells, which include smooth-muscle cells and connective tissue. The prostate’s main function is to produce prostatic fluid, which is combined with sperm to make semen[5].
The prostate is intricately linked to the endocrine system and relies on androgens, such as testosterone, to maintain its secretory functions. Testosterone is converted to dihydrotestosterone (DHT) by the enzyme 5α-reductase[5,6]. DHT is ten times more potent than testosterone and, through intracellular effects on DNA transcription, is responsible for the normal development of the prostate. It is also thought to be responsible for the abnormal growth seen in BPH[4,5]. The aetiology of BPH also has a dynamic component owing to increased smooth muscle tone in the prostate[4].
Symptoms
BPH is often asymptomatic but can lead to benign prostate enlargement. This causes the prostate to compress on the urethra and neck of the bladder, leading to lower urinary tract symptoms and bladder outflow obstruction[3]. However, not all males with lower urinary tract symptoms will have BPH, nor will all males with BPH have bladder outflow obstruction.
Lower urinary tract symptoms are divided into three categories: voiding symptoms, storage symptoms and post-micturition symptoms (see Table 1)[3,5,6]. Other symptoms of BPH include both acute and chronic urinary retention, renal impairment, haematuria (blood in urine) and frequent urinary tract infections (UTIs)[6].
Red-flag symptoms that require referral or further investigation include[1,7]:
- Haematuria;
- Cloudy, foul-smelling urine;
- Associated symptoms of infection, such as fever or flank pain;
- Associated symptoms of cancer, such as night sweats and weight loss.
Risk factors
There are two main risk factors for developing BPH: age and the presence of circulating androgens[8]. Increasing age is the most significant risk factor. It is hypothesised that, as circulating levels of testosterone decrease with age, the enzymatic conversion of testosterone to DHT is upregulated [8]. Studies have shown that castrated patients do not develop the condition, indicating that circulating androgens are necessary to the development of BPH[9]. There is a genetic predisposition to developing BPH; there is a greater risk of developing the condition if there is a known family history[5,10]. Modifiable risk factors, such as poor diet, obesity and decreased physical activity, can substantially influence the development of BPH[10]. A link between BPH and erectile dysfunction has been observed, but it is unclear if one precedes the other[10].
Diagnosis
BPH is diagnosed using a combination of clinical examinations and investigations. A digital rectal exam should be carried out to gauge the size of the prostate. A thorough clinical history will be taken and an international prostate symptom score (IPSS) calculated[3]. The IPSS questionnaire comprises eight questions and is used to assess clinical severity and record lower urinary tract symptoms; 0–7 is mild, 8–19 is moderate and 20–35 is severe. Urinalysis is used to exclude infection and identify haematuria. A full blood count, urea and electrolyte panel are used to establish renal function and exclude differential diagnoses[3,11]. A prostate specific antibody (PSA) test can be useful for identifying elevated PSA levels (common in BPH) and estimating the size of the prostate.
The main differential diagnosis to consider when suspecting BPH is prostate cancer, which can present with overlapping symptoms. Other prostate cancer symptoms to be aware of are painless haematuria, lower back pain, weight loss and reduced appetite[12]. PSA is also raised in patients with prostate cancer; however, PSA levels naturally increase with age and false positive rates are as high as 75%[12,13].
Lifestyle advice
For many patients, lifestyle modifications can improve symptoms without the need for further intervention[14]:
- Regularly practise pelvic floor exercises to strength the muscles that control urine flow[15];
- Stop smoking to reduce the incidence of coughing, which can strain the pelvic floor muscles[16];
- Reduce caffeine intake to limit irritation to the bladder[17];
- Decrease alcohol consumption as alcohol acts as a diuretic[18];
- Drink six to eight glasses of water per day. Limiting fluid intake can reduce bladder capacity and make incontinence worse[18];
- Avoid constipation to prevent straining[19];
- Lose excess weight to lessen pressure on the bladder[19];
- Avoid heavy lifting. This can put pressure on the pelvic floor muscles, increasing the risk of leaks[16].
Cognitive behavioural therapy and bladder training both include techniques to increase the time between feeling the urge to urinate and passing urine. For instance, in bladder training, patients learn to suppress the urgency for urination by contracting their pelvic muscles, hopping from one foot to another and distracting themselves. Evidence has shown the impact of bladder training on both incontinence and an overactive bladder, with up to 87% of patients demonstrating improvement[20].
Pharmacological management
The aim of pharmacological treatment is to manage symptoms based on patient-related goals focusing on issues prioritised by the individual[14].
Medication should be offered to patients with bothersome symptoms, as described in Table 1, for whom lifestyle changes have not been successful[3]. Symptoms, comorbidities, age, concurrent medication and recent observations (such as blood pressure) should be taken into consideration before starting treatment[3].
Alpha blockers
An alpha blocker should be offered as first-line treatment for patients with moderate-to-severe symptoms[14]. By relaxing smooth muscle, they improve symptoms and urinary flow rates but do not reduce the risk of requiring subsequent surgery[21]. Dizziness, orthostatic hypotension, nasal congestion and retrograde ejaculation are common side effects[22]. The lower urinary tract is largely mediated by alpha-1A-adrenergic receptors. As a result, alpha-1A-selective alpha blockers, such as tamsulosin, have fewer systemic adverse effects[23].
Tamsulosin has been classified as a pharmacy-only medicine since 2009[24]. See Table 2 for dosing information. It can be purchased over the counter by patients who meet stringent eligibility criteria (see Box). Eligible patients can be offered an initial two-week supply, followed by a further four-week supply if improvements in urinary symptoms are seen[24]. After six weeks, patients must be assessed by a doctor to determine suitability for further treatment or if additional investigations are needed[24]. Referral criteria is detailed in the box below[24].
Box: Referral criteria for patients requesting tamsulosin over the counter
- Aged under 45 years or over 75 years;
- Symptoms for less than 3 months;
- Red-flag symptoms (e.g. haematuria, foul-smelling urine, fever, pain, night sweats, weight loss);
- Patients on strong CYP3A4 inhibitors;
- Patients already taking alpha blockers for another indication;
- Problems with their liver, kidney or heart;
- Diagnosed or suspected uncontrolled diabetes;
- Previous prostate surgery;
- Already taking medication for lower urinary tract symptoms;
- Surgery for glaucoma or cataract surgery scheduled;
- Hypersensitivity to tamsulosin if taken previously.
5α-reductase inhibitors
Men with symptoms of BPH who have prostates estimated to be greater than 30g or a PSA level more than 1.4ng/mL, and are deemed to be at high risk of progression, should be given a 5α-reductase inhibitor, such as finasteride or dutasteride[3]. By blocking the conversion of testosterone to dihydrotestosterone, finasteride and dutasteride reduce serum PSA, prostate volume, urinary symptoms and the need for surgery[25]. Although usually well tolerated, the side effects can be distressing for patients and can include impotence, gynecomastia and decreased libido[24]. Head-to-head comparison studies have not shown any significant difference between finasteride and dutasteride[26].
Anticholinergics
Anticholinergics can be offered to patients with symptoms of an overactive bladder[3]. Muscarinic M3 receptors initiate bladder contraction and, therefore, antagonising these receptors causes relaxation. Traditional side effects include dry mouth, dizziness, constipation and blurred vision[22]. Furthermore, increasing focus on the long-term cognitive impact of anticholinergics has demonstrated an increased risk of dementia[27]. Anticholinergic burden is a scoring system describing the risk of adverse drug reactions and dementia with a higher score indicating a higher risk[28]. All anticholinergics used for the treatment of urinary symptoms have an anticholinergic burden of 3 — the highest possible individual score[27].
Mirabegron
Mirabegron is a novel, specific β3-adrenoceptor agonist with proven efficacy in the treatment of an overactive bladder[29]. Meta-analysis has shown similar efficacy in comparison with antimuscarinics (a subtype of anticholinergic drugs), but with fewer inconvenient side effects[30]. This is reflected by patients having greater adherence with mirabegron than more traditional therapies[31]. Blood pressure should be monitored and dose reductions are recommended for patients on concurrent enzymatic inhibitors or in the presence of renal and hepatic impairment[22]. It provides a valuable alternative for patients who cannot tolerate, or have a clinical contraindication to, anticholinergics; however, it is a relatively new drug with few long-term studies in this cohort and is significantly more expensive than anticholinergics.
Other
A loop diuretic, taken in the afternoon, can be offered for patients with nocturnal polyuria; however, this is an unlicensed indication[3,22]. Desmopressin can be considered for the treatment of nocturnal polyuria after other medical causes have been rigorously excluded and patients have not benefitted from other treatments[3]. Phosphodiesterase-5 inhibitors should not be offered to males solely experiencing urinary symptoms[3].
Herbal supplements
Herbal supplements have been proposed for the treatment of BPH[32]. The most widely used is saw palmetto (serena repens) extract, potentially owing to its mechanism as a mild 5α-reductase inhibitor; however, trials have demonstrated no benefit compared with placebo for improving symptoms or urinary flow rate[33–35].
Botulinum toxin
Botulinum toxin is a neurotoxin that inhibits the release of acetylcholine[36]. A recent meta-analysis demonstrated that botulinum toxin did not differ from placebo in terms of efficacy or procedure-related side effects[37]. Clear recommendations for its use cannot be made owing to insufficient proof of clinical benefit[38].
Non-pharmacological management
Surgery
Surgery can be offered to patients who have not responded adequately to medical management[3]. Transurethral resection of the prostate (TURP) is considered the gold standard and involves removing a section of the gland using a heated metal wire[39]. In severe cases, complete removal may be necessary — known as a prostatectomy[40]. Given the typical age of presenting patients, surgery poses significant risks of mortality and morbidity. For example, retrograde ejaculation and erectile dysfunction can occur in up to 75% and 10% of men, respectively[41].
Devices
Devices are increasingly being used to avoid the risks associated with medication and surgery[42]. Transurethral microwave thermotherapy, transurethral needle ablation, transrectal high-intensity focused ultrasound (HIFU) and use of the UroLift system are simple procedures that are often performed in an outpatient setting[42]. In March 2023, UroLift was recommended by the National Institute for Health and Care Excellence (NICE) as a cost-effective alternative to TURP[43]. Fewer side effects have been reported using these methods; however, concerns have been raised over their long-term efficacy[42]. For instance, 44% of patients treated with HIFU required BPH-related surgery within four years[44].
Catheters
Urinary catheterisation, either intermittent or indwelling, is recommended by NICE for select patients[3]. It can be conducted by patients, carers or healthcare professionals. Intermittent catheterisation can give patients control over their symptoms but requires training and dexterity to complete successfully[14]. Indwelling catheters can be offered to patients for whom medical management or surgery has failed and who are not able to manage intermittent self-catheterisation[14]. However, they increase the risk of urinary tract infection and can cause local trauma to the urethral area if placed incorrectly[45].
Other
Incontinence products can be used at any stage of management. They include pads, pants, sheaths and drainage systems. Toilet aids and containment products are occasionally available on the NHS, depending on local policy[46].
Best practice
- Pharmacists should be able to recognise the most common lower urinary tract symptoms and the red-flag symptoms that require further investigation;
- Advise and review the most appropriate medication for each patient group, optimising where suitable;
- Be aware of the potential adverse effects associated with medications used to manage benign prostatic hyperplasia;
- Have knowledge of alternate methods, besides medication, to manage symptoms;
- Clinicians should make every contact count and advise patients on lifestyle changes to manage their symptoms.
- This article was amended on 20 September 2023 to correct an error in the description of botulinum toxin
- 1Lee SWH, Chan EMC, Lai YK. The global burden of lower urinary tract symptoms suggestive of benign prostatic hyperplasia: A systematic review and meta-analysis. Sci Rep. 2017;7. doi:10.1038/s41598-017-06628-8
- 2Prostate-Related Statistics. The Urology Foundation. https://www.theurologyfoundation.org/professionals/healthcare-resources-and-reports/urology-resources/facts-and-figures/prostate-related-statistics (accessed Aug 2023).
- 3Lower Urinary Tract Symptoms in Men: Recommendations [CG97]. National Institute for Health and Care Excellence. 2015.https://www.nice.org.uk/Guidance/CG97 (accessed Aug 2023).
- 4Lerner LB, McVary KT, Barry MJ, et al. Management of Lower Urinary Tract Symptoms Attributed to Benign Prostatic Hyperplasia: AUA GUIDELINE PART I—Initial Work-up and Medical Management. Journal of Urology. 2021;206:806–17. doi:10.1097/ju.0000000000002183
- 5Lawrentschuk N, Ptasznik G, Ong S. Benign Prostate Disorders. Endotext. 2000.https://www.ncbi.nlm.nih.gov/books/NBK279008/ (accessed Aug 2023).
- 6Ng M, Baradhi KM. Benign Prostatic Hyperplasia. StatPearls. 2023.https://www.ncbi.nlm.nih.gov/books/NBK558920/ (accessed Aug 2023).
- 7Rutter P. Community Pharmacy. 5th ed. Elsevier 2020. https://shop.elsevier.com/books/community-pharmacy/rutter/978-0-7020-8020-3#full-description (accessed Aug 2023).
- 8Bartsch G, Rittmaster R, Klocker H. Dihydrotestosterone and the concept of 5α-reductase inhibition in human benign prostatic hyperplasia. World J Urol. 2002;19:413–25. doi:10.1007/s00345-002-0248-5
- 9Wilson JD, Roehrborn C. Long-Term Consequences of Castration in Men: Lessons from the Skoptzy and the Eunuchs of the Chinese and Ottoman Courts. The Journal of Clinical Endocrinology & Metabolism. 1999;84:4324–31. doi:10.1210/jcem.84.12.6206
- 10Lim KB. Epidemiology of clinical benign prostatic hyperplasia. Asian Journal of Urology. 2017;4:148–51. doi:10.1016/j.ajur.2017.06.004
- 11Benign Prostatic Hyperplasia. BMJ Best Practice. 2022.https://bestpractice.bmj.com/topics/en-gb/208 (accessed Aug 2023).
- 12Prostate Cancer: Diagnosis and Management [NG131]. National Institute for Health and Care Excellence. 2021.https://www.nice.org.uk/guidance/ng131/chapter/Recommendations#assessment-and-diagnosis (accessed Aug 2023).
- 13Prostate Cancer: How Should I Assess a Person with Suspected Prostate Cancer? National Institute for Health and Care Excellence. 2022.https://cks.nice.org.uk/topics/prostate-cancer/diagnosis/assessment/ (accessed Aug 2023).
- 14Firth J, Conlon C, Cox T, editors. Oxford Textbook of Medicine. Oxford University PressOxford 2020. doi:10.1093/med/9780198746690.001.0001
- 15Non-Surgical Treatment: Urinary Incontinence. NHS. 2023.https://www.nhs.uk/conditions/urinary-incontinence/treatment (accessed Aug 2023).
- 1610 Ways to Stop Leaks: Urinary Incontinence. NHS. 2023.https://www.nhs.uk/conditions/urinary-incontinence/10-ways-to-stop-leaks (accessed Aug 2023).
- 17Lohsiriwat S, Hirunsai M, Chaiyaprasithi B. Effect of caffeine on bladder function in patients with overactive bladder symptoms. Urol Ann. 2011;3:14. doi:10.4103/0974-7796.75862
- 18Bradley CS, Erickson BA, Messersmith EE, et al. Evidence of the Impact of Diet, Fluid Intake, Caffeine, Alcohol and Tobacco on Lower Urinary Tract Symptoms: A Systematic Review. Journal of Urology. 2017;198:1010–20. doi:10.1016/j.juro.2017.04.097
- 19Parsons JK, Sarma AV, McVary K, et al. Obesity and Benign Prostatic Hyperplasia: Clinical Connections, Emerging Etiological Paradigms and Future Directions. Journal of Urology. 2013;189. doi:10.1016/j.juro.2012.11.029
- 20Booth J, Bliss D. Consensus statement on bladder training and bowel training. Neurourology and Urodynamics. 2020;39:1234–54. doi:10.1002/nau.24345
- 21Chapple C, Wyndaele J, Nordling J, et al. Tamsulosin, the first prostate-selective alpha 1A-adrenoceptor antagonist. A meta-analysis of two randomized, placebo-controlled, multicentre studies in patients with benign prostatic obstruction (symptomatic BPH). European Tamsulosin Study Group. Eur Urol 1996;29:155–67.https://www.ncbi.nlm.nih.gov/pubmed/8647141
- 22British National Formulary. BMJ and Pharmaceutical Press. 2023.http://www.medicinescomplete.com (accessed Aug 2023).
- 23Beduschi MC, Beduschi R, Oesterling JE. Alpha-Blockade Therapy for Benign Prostatic Hyperplasia: from a Nonselective to a More Selective Alpha1A-Adrenergic Antagonist. Urology. 1998;51:861–72. doi:10.1016/s0090-4295(98)00140-x
- 24OTC Tamsulosin – A Quick Reference Guide. Royal Pharmaceutical Society. 2010.https://www.rpharms.com/publications/member-resources (accessed Aug 2023).
- 25ROEHRBORN CG, BRUSKEWITZ R, NICKEL JC, et al. Sustained Decrease in Incidence of Acute Urinary Retention and Surgery With Finasteride for 6 Years in Men With Benign Prostatic Hyperplasia. Journal of Urology. 2004;171:1194–8. doi:10.1097/01.ju.0000112918.74410.94
- 26Nickel JC, Gilling P, Tammela TL, et al. Comparison of dutasteride and finasteride for treating benign prostatic hyperplasia: the Enlarged Prostate International Comparator Study (EPICS). BJU International. 2011;108:388–94. doi:10.1111/j.1464-410x.2011.10195.x
- 27Kay GG, Abou-Donia MB, Messer WS Jr, et al. Antimuscarinic Drugs for Overactive Bladder and Their Potential Effects on Cognitive Function in Older Patients. Journal of the American Geriatrics Society. 2005;53:2195–201. doi:10.1111/j.1532-5415.2005.00537.x
- 28King R, Rabino S. ACB Calculator . ACB Calculator . https://www.acbcalc.com/medicines (accessed Aug 2023).
- 29Kang TW, Kim SJ, Kim MH, et al. Beta 3 Adrenoreceptor Agonist for the Management of Lower Urinary Tract Symptoms in Men With Benign Prostatic Hyperplasia: A Systematic Review. Int Neurourol J. 2021;25:182–91. doi:10.5213/inj.2142068.034
- 30Kelleher C, Hakimi Z, Zur R, et al. Efficacy and Tolerability of Mirabegron Compared with Antimuscarinic Monotherapy or Combination Therapies for Overactive Bladder: A Systematic Review and Network Meta-analysis. European Urology. 2018;74:324–33. doi:10.1016/j.eururo.2018.03.020
- 31Yeowell G, Smith P, Nazir J, et al. Real-world persistence and adherence to oral antimuscarinics and mirabegron in patients with overactive bladder (OAB): a systematic literature review. BMJ Open. 2018;8:e021889. doi:10.1136/bmjopen-2018-021889
- 32Bowker LK, Price JD, Shah KS, et al. Oxford Handbook of Geriatric Medicine. 3rd ed. Oxford, UK: : Oxford University Press 2018. https://global.oup.com/academic/product/oxford-handbook-of-geriatric-medicine-3e-9780198738381?cc=us&lang=en& (accessed Aug 2023).
- 33Suzuki M, Ito Y, Fujino T, et al. Pharmacological effects of saw palmetto extract in the lower urinary tract. Acta Pharmacol Sin. 2009;30:271–81. doi:10.1038/aps.2009.1
- 34Bent S, Kane C, Shinohara K, et al. Saw Palmetto for Benign Prostatic Hyperplasia. N Engl J Med. 2006;354:557–66. doi:10.1056/nejmoa053085
- 35Barry MJ. Effect of Increasing Doses of Saw Palmetto Extract on Lower Urinary Tract Symptoms. JAMA. 2011;306:1344. doi:10.1001/jama.2011.1364
- 36Rusnack S, Kaplan S. The use of botulinum toxin in men with benign prostatic hyperplasia. Rev Urol 2005;7:234–6.https://www.ncbi.nlm.nih.gov/pubmed/16985836
- 37Shim SR, Cho YJ, Shin I-S, et al. Efficacy and safety of botulinum toxin injection for benign prostatic hyperplasia: a systematic review and meta-analysis. Int Urol Nephrol. 2015;48:19–30. doi:10.1007/s11255-015-1153-3
- 38Chung ASJ, Woo HH. Update on minimally invasive surgery and benign prostatic hyperplasia. Asian Journal of Urology. 2018;5:22–7. doi:10.1016/j.ajur.2017.06.001
- 39Knight GM, Talwar A, Salem R, et al. Systematic Review and Meta-analysis Comparing Prostatic Artery Embolization to Gold-Standard Transurethral Resection of the Prostate for Benign Prostatic Hyperplasia. Cardiovasc Intervent Radiol. 2020;44:183–93. doi:10.1007/s00270-020-02657-5
- 40Alternatives: Transurethral Resection of the Prostate (TURP). NHS. 2021.https://www.nhs.uk/conditions/transurethral-resection-of-the-prostate-turp/alternatives (accessed Aug 2023).
- 41Risks: Transurethral Resection of the Prostate (TURP). . NHS. 2021.https://www.nhs.uk/conditions/transurethral-resection-of-the-prostate-turp/risks (accessed Aug 2023).
- 42Kim EH, Larson JA, Andriole GL. Management of Benign Prostatic Hyperplasia. Annu. Rev. Med. 2016;67:137–51. doi:10.1146/annurev-med-063014-123902
- 43UroLift for Treating Lower Urinary Tract Symptoms of Benign Prostatic Hyperplasia [MTG58]. National Institute for Health and Care Excellence. 2021.https://www.nice.org.uk/guidance/mtg58 (accessed Aug 2023).
- 44Madersbacher S, Schatzl G, Djavan B, et al. Long–Term Outcome of Transrectal High– Intensity Focused Ultrasound Therapy for Benign Prostatic Hyperplasia. European Urology. 2000;37:687–94. doi:10.1159/000020219
- 45Dybowski BA, Zapała P, Bres-Niewada E, et al. Catheter-associated bacterial flora in patients with benign prostatic hyperplasia: shift in antimicrobial susceptibility pattern. BMC Infect Dis. 2018;18. doi:10.1186/s12879-018-3507-9
- 46Incontinence Products: Urinary Incontinence. NHS. 2023.https://www.nhs.uk/conditions/urinary-incontinence/incontinence-products (accessed Aug 2023).
2 comments
You must be logged in to post a comment.


Is there a typo in this article? "Botulinum toxin is a neurotoxin that inhibits the release of acetylcysteine[36]." - should this read "acetylcholine" instead??
Many thanks for your comment. I am Senior Editor for Research & Learning at the PJ. We are currently investigating this with the author and will confirm if a correction to the article is necessary shortly.