
BSIP SA / Alamy Stock Photo
This article was originally published in June 2019 and updated in March 2026.
Meningitis is one of the leading infection-related causes of death in children in the world, second only to pneumonia1. It is responsible for more deaths than malaria, AIDS, measles and tetanus combined1. The disease is more prevalent in children aged under four years and in teenagers.
In England, there has been a sustained decline in confirmed cases of invasive meningococcal disease over the past two decades, from 2,595 cases in 1999/2000 to fewer than 400 cases annually in recent years2. UK Health Security Agency data indicate that 378 cases were confirmed in 2024/2025, compared with 340 cases in 2023/2024 and 396 cases in 2022/2023, reflecting some year-to-year variation following a marked reduction during the COVID-19 pandemic2,3. However, a localised outbreak of serogroup B meningococcal disease in Kent in 2026 — which has been associated with fatalities and multiple hospitalisations — has prompted a targeted public health response, including antibiotic prophylaxis and vaccination of close contacts, highlighting the ongoing risk of disease despite overall low incidence4.
Pharmacists have a vital role in raising awareness of the signs and symptoms of meningitis, while also maximising the benefit of the national immunisation programme to reduce the incidence of the disease. This article will cover initial management options, with a focus on children and neonates.
Causes
Meningitis is the inflammation of the membranes covering the brain and spinal cord (i.e. meninges). It can be caused by viruses, bacteria or fungi.
Meningococcal disease encompasses meningococcal septicaemia, meningococcal meningitis or a combination of the two5.
The overall annual incidence of invasive meningococcal disease in the UK is low, at fewer than 1 case per 100,000 population6. With prompt antimicrobial treatment and supportive care, outcomes are generally favourable; however, the disease remains associated with significant morbidity and mortality6. In England, the case-fatality ratio for invasive meningococcal disease was 2.3% in 2023/20246. Complications are more common following pneumococcal meningitis, occurring in about 30% of people compared with 7% with meningococcal meningitis6.
Bacterial meningitis is most commonly caused by Neisseria meningitidis (also known as meningococcus), although the main pathogens alter with age. As such, N. meningitidis, Streptococcus pneumoniae (also known as pneumococcus) and Haemophilus influenzae type B are the leading causes of meningitis in children older than three months; however, Streptococcus agalactiae, Escherichia coli, S. pneumoniae and Listeria monocytogenes are more common in children younger than three months5,6.
The bacteria that cause meningitis are very common — they are present in the nasopharynx in around one in ten people who may not ever show any symptoms of disease. The reasons why some people develop meningitis, while others do not, are not yet fully understood. It is thought that genetic variations in the genes for Factor H and Factor H-related proteins may have a role to play7. These proteins regulate a part of the body’s immune system called the complement system, which recognises and kills invading bacteria.
Risk factors
In general, young children are at the highest risk of bacterial meningitis and septicaemia, but other age groups, including older people, can also be vulnerable to specific types. One study found that meningococcal meningitis was less frequent in older patients, whereas pneumococcal, listerial and meningitis of unknown origin were more frequent5,8. People with low immunity may also be at an increased risk, such as those with HIV or undergoing chemotherapy treatment.
Individual countries show seasonal patterns of bacterial meningitis. Increased cases have been observed between the months of December and March in the United States, France and the UK9. There is also evidence that mass gatherings and exposure to cigarette and wood smoke can make people more susceptible to certain causes of meningitis and septicaemia, potentially from interference with mucosal immunity10.
This is reflected in reports of a localised outbreak of meningococcal disease in Kent in March 2026, which has predominantly affected adolescents and young adults in settings involving close contact, including communal living and high-density social events. Factors such as crowding and close interpersonal contact combined with behaviours such as sharing drinks may facilitate transmission. The MenB vaccine was only included in the routine infant vaccination programme in 2015, so many of the affected individuals will not have received it, reflecting gaps in population-level protection in adolescents and young adults.
Depending on the cause, cases of meningitis may be isolated; however, those who have been in close contact with someone with bacterial meningitis may be at increased risk of disease.
Pathophysiology
Infection occurs through transmission of contaminated respiratory droplets or saliva. Pili on the bacterial surface are thought to disrupt endothelial cell junctions in the blood–brain barrier, allowing the pathogens to penetrate it11. Once they have entered the subarachnoid space (i.e. the area of the brain between the arachnoid membrane and the pia mater), the pathogens replicate rapidly. This causes the production of several inflammatory mediators, including lymphocytes and inflammatory cytokines, as well as local immunoglobulin production by plasma cells. This enhances the influx of leukocytes into the normal cerebrospinal fluid (CSF), which releases toxic substances that contribute to the production of cyctotoxic oedema and increased intracranial pressure. It is this process that can contribute to neurological damage and potential death12,13.
Signs, symptoms and immediate management
Symptoms typically occur within three to seven days after transmission5. Early, non-specific symptoms of meningitis include:
- Irritability;
- Ill appearance;
- Lethargy;
- Refusing food/drink;
- Headache;
- Other aches and respiratory symptoms;
- Vomiting/nausea;
- Fever.
Suspected meningitis is a medical emergency. Pharmacy professionals should ensure immediate referral for urgent medical assessment and must not delay escalation.
In infants, healthcare professionals should be aware that classic signs of meningitis, including neck stiffness, bulging fontanelle and high-pitched cry, are often absent with bacterial meningitis5,14. Less common early symptoms include shivering, diarrhoea, abdominal pain and distention, coryza and other ear, nose and throat symptoms5.
General features of meningitis include a non-blanching rash that can appear anywhere on the body, altered mental state, shock, unconsciousness and toxic or moribund state. If a patient presents with these symptoms, the glass test (also known as the ‘Tumbler test’, see Figure) may be used to aid diagnosis, where the side of a clear glass should be firmly pressed against the rash – if it does not fade under pressure, the patient may have septicaemia and needs urgent medical attention5,15. However, it should be noted that the National Institute for Health and Care Excellence’s Clinical Knowledge Summary states that the glass test should not be used solely for diagnosing bacterial meningitis and meningococcal septicaemia6.
Figure: Glass or ‘tumbler’ test
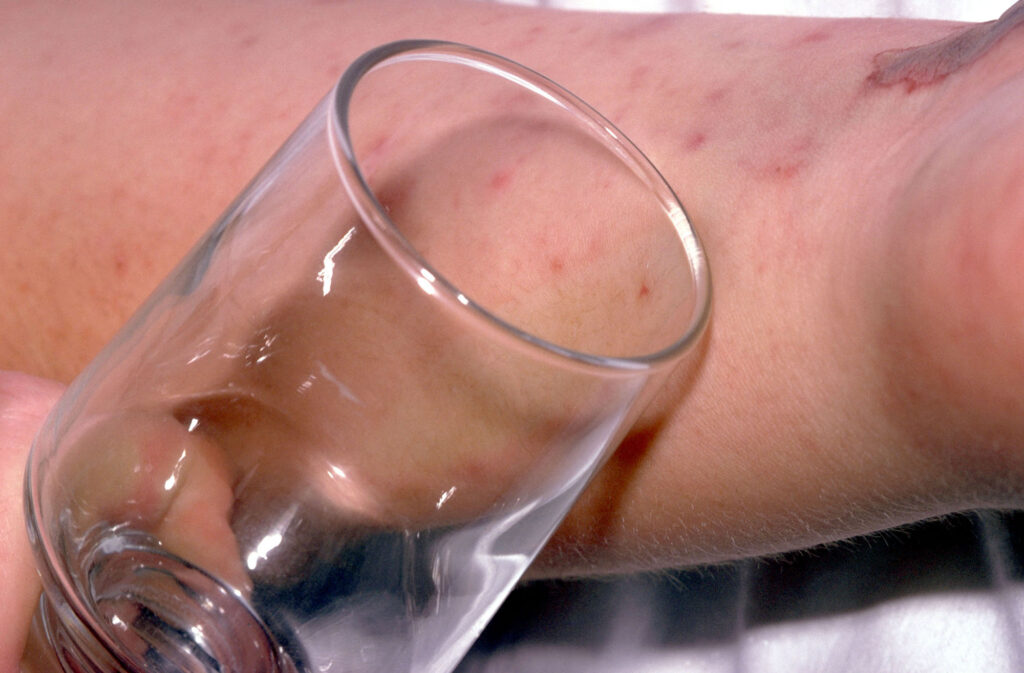
Mediscan / Alamy Stock Photo
The classic rash associated with meningitis usually looks like small, red pin pricks that spreads quickly over the body and turns into red or purple blotches. However, a rash is not always present with meningitis and may be less visible in darker skin tones. It is, therefore, important to also check the soles of the feet, palms of the hands and eyelids in the patient with suspected meningitis5.
Furthermore, if the patient is a child or young person, it is important for healthcare professionals to consider other non-specific features of their presentation, such as the level of parental or carer concern (particularly compared with previous illness in the child or young person or their family), how quickly the illness is progressing and clinical judgement of the overall severity of the illness5.
Prevention and vaccination
As meningitis can be caused by several different pathogens, there are several vaccinations available that can offer some protection against the disease (see Table)13,16–23.
Table: Vaccinations available for meningitis and infections linked with meningitis
Case studies
Several case studies show how assessment and treatment of meningitis varies by patient. All patients, events and incidents in these case studies are fictitious and should only be used as examples in the clinical setting.
Case study one: a toddler with mild meningitis
Eva, aged three years, is on holiday with her grandparents. She is unusually tired and is complaining that her legs are aching. This morning, Eva’s grandparents noticed a very small purple rash on her leg, so they have to come to the pharmacy for advice. Eva has no fever or any other symptoms, but her grandmother has a cold sore.
Assessment and diagnosis
The rash does not fade under pressure when a glass is pressed against it.
Petechiae and purpura are significantly more common with invasive meningococcal infection than with pneumococcal meningitis, which rarely presents with a rash6. However, although the glass test is widely promoted in patient information leaflets, the National Institute for Health and Care Excellence (NICE) has found no evidence on its use and the test is not promoted in its guidelines. Consequently, NICE advises that the glass test should not be used as the only test for diagnosing the condition15. The local health protection team is informed that Eva may have meningitis and an ambulance is called.
Treatment options
On arrival at hospital, Eva is showing signs of shock — she is tachycardic with increased drowsiness and cold peripheries. After having initial tests, she is treated for shock with a fluid bolus of 20mL/kg sodium chloride 0.9% for over ten minutes. A lumbar puncture is contraindicated in shock and, therefore, Eva is empirically started on IV ceftriaxone and steroids. She is also started on IV aciclovir, owing to her history of contact with the herpes simplex virus.
Advice and recommendations
Eva is treated with antibiotics for ten days and her grandparents are both prescribed rifampicin as chemoprophylaxis. Antibiotic prophylaxis should be given as soon as possible (ideally within 24 hours) after the diagnosis of the index case15.
Case study two: a baby with meningitis
Katherine — a mother of Jacob and Esme, aged six weeks and four years, respectively — comes into the pharmacy seeking advice about Jacob’s blocked nose and fever. She explains that Esme had gastroenteritis with cold symptoms and fever one week ago, but no rash. Katherine is worried about Jacob and asks for advice.
Assessment and diagnosis
Katherine brings her children into the consultation room for further assessment. Jacob has been more unsettled than usual and does not want to feed as much as normal. Upon examination, Jacob has a rash on his stomach and back, which his mother says was not present this morning. His rash looks like red blotches and does not fade with the glass test. Owing to his age, Jacob is too young to have received any vaccinations, including MenB.
Katherine is warned that Jacob may have meningitis, as he has the characteristic rash, as well as other known symptoms. He needs to be taken to hospital for emergency assessment and an ambulance is called.
Treatment options
On arrival at the hospital, Jacob has blood tests taken and a lumbar puncture. He is started on IV ceftriaxone with amoxicillin (owing to presence of risk factors for Listeria monocytogenes) with full-volume maintenance fluids and enteral feeds as tolerated[5]. Corticosteroids must not be used in children aged under three months with suspected or confirmed bacterial meningitis.
Jacob has hourly observations initially for heart rate, blood pressure, respiratory rate, oxygen saturation, fluid balance and Glasgow Coma Scale (GCS). The GCS is a neurological scale used to describe the level of consciousness in a person following a traumatic brain injury — the lower the number, the more severe the brain injury. The local health protection team is also informed that Jacob may have meningitis.
Cefotaxmine may be used as an alternative if ceftriaxone is contraindicated (it should not be given to premature babies or in babies with jaundice, hypoalbuminaemia or acidosis, as it may exacerbate hyperbilirubinaemia)24.
The microbiology consultant calls the ward to confirm that Jacob has group B streptococcal meningitis. Amoxicillin is stopped. As per the National Institute for Health and Care Excellence’s guidelines, antibiotics should be stopped after 14 days if Jacob has recovered5. If he is still unwell at that stage, advice from an infection specialist will be required5.
Advice and recommendations
Before discharge, Katherine is given the contact details of several patient support organisations, including meningitis charities that can offer support and written information to signpost her to further help. Jacob has an audiology appointment booked in two weeks and will be seen by a paediatrician after this. At this appointment, the following morbidities will be considered:
- Hearing loss;
- Orthopaedic complications;
- Skin complications (including scarring from necrosis);
- Psychosocial problems;
- Neurological and developmental problems;
- Kidney failure.
Outcome
Jacob makes a full recovery from his meningitis with no lasting effects.
Case study three: an adult with suspected meningitis
Jane is a paediatric haematology nurse who comes into the pharmacy asking to buy paracetamol. She says she has a terrible headache and upset stomach. She seems confused and disorientated; talking to her further highlights that something is not right.
Jane explains that she has not felt well since last night and has spent most of the day in bed, as she feels like she has no energy. However, some of what Jane also says does not make sense and she is finding it hard to follow the conversation. She has no fever or rash.
Assessment and diagnosis
Vomiting, severe headache and confusion are all symptoms of meningitis. The pharmacist uses a symptom checker, such as the one by the Meningitis Research Foundation, to help with decision-making.
Upon further questioning, it is clear that Jane must go to a hospital immediately and an ambulance is called. Jane presented with confusion and disorientation, which might indicate a stroke; however, bacterial meningitis can cause stroke.
Treatment options
When the paramedics arrive at the pharmacy, they find Jane has a Glasgow Coma Scale of 4/15. Once Jane arrives in hospital, they follow the stroke pathway, but she is now also febrile. Jane has a lumbar puncture and the results show she has bacterial meningitis. She also has a CT scan that shows an infarct on her right temporal lobe. Jane is treated in hospital with antibiotics and steroids, and eventually discharged to go home after three weeks.
Jane was working in the paediatric intensive care unit the week preceding the symptoms. She was looking after a child with Haemophilus influenzae type b (Hib). The patient was in a neutral pressure side room with a positive pressure lobby — this is an infection control measure to prevent the spread of microbial contaminants outside the patient’s side room. The lobby had been used to store an apheresis machine; however, the door between the side room and lobby had been left open, inadvertently leading to the exposure of Hib.
Outcome
Although Jane has now fully recovered, she has to wear glasses owing to damage to her optical nerve. She also has tinnitus and occasionally suffers from severe headaches.
Recovering from meningitis/complications
Some of the most common complications associated with meningitis are13:
- Hearing loss, which may be partial or total — people who have had meningitis will usually have a hearing test after a few weeks to check for any problems;
- Recurrent seizures;
- Problems with memory and concentration;
- Problems with coordination, movement and balance;
- Learning difficulties and behavioural problems;
- Vision loss, which may be partial or total;
- Loss of limbs — amputation is sometimes necessary to stop the infection spreading through the body and remove damaged tissue;
- Bone and joint problems, such as arthritis;
- Kidney problems.
Useful resources
- 1.Levels and Trends in Child Mortality Report 2017. UNICEF. October 2017. Accessed March 2026. https://www.unicef.org/reports/levels-and-trends-child-mortality-report-2017
- 2.Invasive meningococcal disease in England: annual laboratory confirmed reports for epidemiological year 2017 to 2018. Public Health England. October 2018. Accessed March 2026. https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/751821/hpr3818_IMD.pdf
- 3.Invasive meningococcal disease in England: annual laboratory-confirmed reports for epidemiological year 2024 to 2025. UK Health and Security Agency. November 2025. Accessed March 2026. https://www.gov.uk/government/publications/meningococcal-disease-laboratory-confirmed-cases-in-england-2024-to-2025/invasive-meningococcal-disease-in-england-annual-laboratory-confirmed-reports-for-epidemiological-year-2024-to-2025
- 4.Wise J. Meningitis in Kent: Two young people dead and 11 seriously ill in outbreak. BMJ. 2026;392:s503. doi:10.1136/bmj.s503
- 5.Meningitis (bacterial) and meningococcal disease: recognition, diagnosis and management. NICE guideline NG240. National Institute for Health and Care Excellence. March 2024. Accessed March 2026. https://www.nice.org.uk/guidance/ng240
- 6.Meningitis – bacterial meningitis and meningococcal disease. National Institute for Health and Care Excellence. August 2025. Accessed March 2026. https://cks.nice.org.uk/topics/meningitis-bacterial-meningitis-meningococcal-disease/
- 7.Genome-wide association study identifies variants in the CFH region associated with host susceptibility to meningococcal disease. Nat Genet. 2010;42(9):772-776. doi:10.1038/ng.640
- 8.Domingo P, Pomar V, de Benito N, Coll P. The spectrum of acute bacterial meningitis in elderly patients. BMC Infect Dis. 2013;13(1). doi:10.1186/1471-2334-13-108
- 9.Paireau J, Chen A, Broutin H, Grenfell B, Basta NE. Seasonal dynamics of bacterial meningitis: a time-series analysis. The Lancet Global Health. 2016;4(6):e370-e377. doi:10.1016/s2214-109x(16)30064-x
- 10.Cooper LV, Robson A, Trotter CL, et al. Risk factors for acquisition of meningococcal carriage in the African meningitis belt. Tropical Med Int Health. 2019;24(4):392-400. doi:10.1111/tmi.13203
- 11.Kolappan S, Coureuil M, Yu X, Nassif X, Egelman EH, Craig L. Structure of the Neisseria meningitidis Type IV pilus. Nat Commun. 2016;7(1). doi:10.1038/ncomms13015
- 12.Tunkel AR, Scheld WM. Pathogenesis and pathophysiology of bacterial meningitis. Clin Microbiol Rev. 1993;6(2):118-136. doi:10.1128/cmr.6.2.118
- 13.Sáez-Llorens X, McCracken GH Jr. Bacterial meningitis in children. The Lancet. 2003;361(9375):2139-2148. doi:10.1016/s0140-6736(03)13693-8
- 14.Meningitis. NHS. March 2026. Accessed March 2026. https://www.nhs.uk/conditions/meningitis/
- 15.Baines P, Reilly N, Gill A. Paediatric meningitis: clinical features and diagnosis. . Clin Pharm. 2009;1:307-310. https://www.researchgate.net/publication/289624043_Paediatric_meningitis_Clinical_features_and_diagnosis
- 16.NHS vaccinations and when to have them. NHS . 2023. Accessed March 2026. https://www.nhs.uk/vaccinations/nhs-vaccinations-and-when-to-have-them/
- 17.6-in-1 vaccine. NHS. June 2023. Accessed March 2026. https://www.nhs.uk/vaccinations/6-in-1-vaccine/
- 18.MenB vaccine for children. NHS. 2024. Accessed March 2026. https://www.nhs.uk/vaccinations/menb-vaccine-for-children/
- 19.Pneumococcal vaccine. NHS. 2023. Accessed March 2026. https://www.nhs.uk/vaccinations/pneumococcal-vaccine/
- 20.MMRV (measles, mumps, rubella and chickenpox) vaccine. NHS. 2025. Accessed March 2026. https://www.nhs.uk/vaccinations/mmrv-vaccine/
- 21.MenACWY. NHS. 2024. Accessed March 2026. https://www.nhs.uk/vaccinations/menacwy-vaccine/
- 22.Bexsero Meningococcal Group B vaccine for injection in pre-filled syringe. Electronic Medicines Compendium. 2025. Accessed March 2026. https://www.medicines.org.uk/emc/product/5168/smpc#gref
- 23.Complete routine immunisation schedule from 1 January 2026. UK Health Security Agency. 2026. Accessed March 2026. https://www.gov.uk/government/publications/the-complete-routine-immunisation-schedule/complete-routine-immunisation-schedule-from-1-january-2026
- 24.Ceftriaxone: Contraindications. BNFC. Accessed March 2026. https://bnfc.nice.org.uk/drugs/ceftriaxone/#contra-indications
You might also be interested in…

Recognition and management of whooping cough
Everything you need to know about meningitis B
