Science Photo Library
The majority of mouth ulcers are painful and can adversely affect eating and drinking. As such, patients with mouth ulcers often present in community pharmacies. Aphthous stomatitis (oral ulceration), which represents a full-thickness breach in the epithelium lining the soft tissues of the mouth, affects a high proportion of the population and can be the result of a wide range of conditions[1],[2]
(see Box 1).
Pharmacists can ask basic questions concerning the nature of the ulceration, which can help provide a good indication about the likely cause (see Box 2), as well as providing patients with symptomatic relief and immediate local treatment. However, a person suspected of having an oral squamous cell carcinoma (mouth cancer) must be instructed to urgently seek the opinion of a dental practitioner or their GP.
This article will cover different types of oral ulceration, how pharmacists can differentiate between the variety of causes and, therefore, advise on the treatment options available.
Box 1: Conditions that may present as oral ulceration
- Recurrent aphthous stomatitis;
- Physical trauma (e.g. bite, fractured tooth surfaces, hot foods);
- Chemical trauma (e.g. aspirin burn);
- Acute necrotising ulcerative gingivostomatitis;
- Lichen planus;
- Lichenoid drug reaction;
- Herpetic gingivostomatitis (e.g. herpes simplex virus);
- Hand, foot and mouth disease (e.g. Coxsackie virus);
- Squamous cell carcinoma (e.g. mouth cancer);
- Erythema multiforme (e.g. adverse drug reaction);
- Vesiculobullous disease (e.g. mucous membrane pemphigoid/pemphigus);
- Haematological malignancy (e.g. leukaemia);
- Inflammatory bowel disease (e.g. Crohn’s disease, coeliac disease);
- Haematinic deficiency (e.g. low iron, vitamin B12 or folic acid).
Box 2: Questions to ask an individual complaining of oral ulceration
- Is the ulceration painful?
- How many ulcers do you have?
- How long have you had the ulcer(s)?
- Which sites in your mouth are affected?
- Do you have any concurrent signs or symptoms?
- Have you recently started any new medicines?
- Have you had a similar episode of ulceration previously?
- If so, how long did the ulcers take to heal?
- Are you aware of any factors that predispose to your ulcers?
Traumatic oral ulceration
Aetiology and presentation
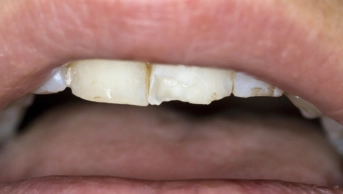
Usually presenting as a single, painful, irregular ulcer (see Figure 1), patients can often recall an incident that preceded the development of the ulcer, such as biting the lining of the mouth, or a thermal burn from hot food or drinks. Alternatively, it may be caused by a sharp surface on a tooth, restoration or denture.
Management
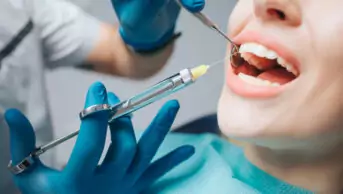
Patients experiencing toothache may place an aspirin tablet adjacent to the affected tooth in an attempt to relieve the pain. Dissolution of aspirin in saliva produces a low pH, which leads to a local chemical burn on the mucosa, referred to as an “aspirin burn” with little, if any, relief of the toothache[3]
. Patients should be advised against such use of aspirin.
Pharmacists should recommend an antiseptic or topical anti-inflammatory spray for the management of mouth ulcers (see Box 3). If the individual appears otherwise well, symptomatic treatment involving the use of a warm saline mouthwash or provision of topical chlorhexidine or benzydamine spray should help. Patients should be advised to visit a dental practitioner to remove any dental source of trauma.
The oral epithelium should recover within a few days of treatment. However, if the ulcer persists beyond three weeks, patients should be referred to their GP or dental practitioner to exclude the presence of cancer.
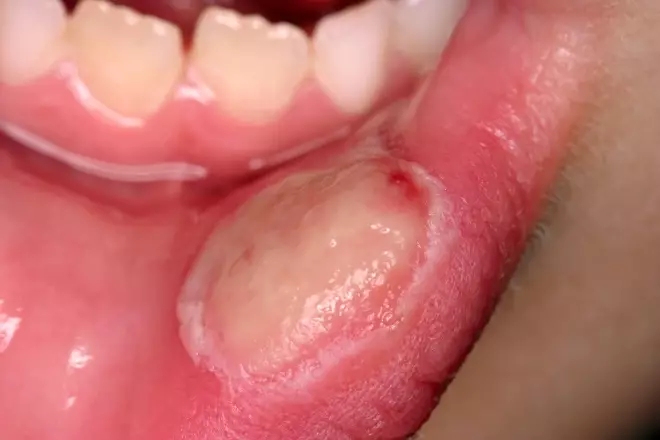
Figure 1: Traumatic ulcer
Source: Science Photo Library
Box 3: Topical preparations
Saline mouthwash
Salt water mouthwash, prepared by dissolving half a teaspoon of salt in glass of warm water, should be used as a rinse at frequent intervals until the discomfort and swelling subsides.
Antiseptic mouthwash or spray
Chlorhexidine gluconate 2mg/mL (0.2%) mouthwash or spray (sugar-free) used twice daily as instructed (10mL for one minute). It should not be used within 30 minutes of using toothpaste, owing to possible interaction (and it can cause an unpleasant taste in the mouth).
Non-steroidal anti-inflammatory mouthwash or spray
Benzydamine hydrochloride 1.5mg/mL (0.15%) as mouthwash or spray (sugar-free) used four times daily as instructed (15mL as rinse or four sprays every 1.5 hours as required).
Steroid aerosol inhalation or tablet
Beclometasone diproprionate aerosol inhalation, 50 micrograms/metered inhalation. Used as instructed (1–2 puffs directed on to ulcers twice daily). The use of this is unlicensed in oral ulceration.
Hydrocortisone sodium succinate muco-adhesive buccal tablet 2.5mg used as instructed (one tablet dissolved adjacent to ulcer four times daily). This is unlicensed for use in children aged under 12 years and should be given on medical advice only.
Source: BNF 76. London: Pharmaceutical Press; 2018
Recurrent oral ulceration
Ulcers may be a long-standing problem for some patients. Recurrent aphthous stomatitis (RAS) presents as painful round or oval ulcers that recur at different sites in the mouth[4]
. It has been categorised into three subtypes:
- Minor RAS:
- Occurs in groups of around five small ulcers;
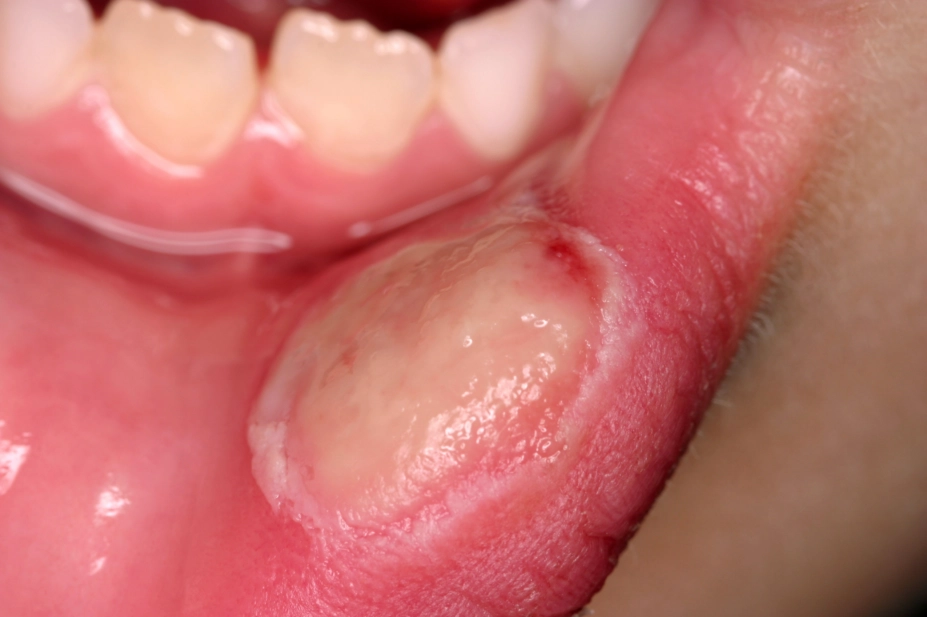
- Ulcers are each less than 1cm in diameter on the non-keratinised sites in the mouth, such as buccal mucosa, labial mucosa or the floor of the mouth (see Figure 2);
- Ulcers usually heal within 10–14 days.
- Major RAS:
- Occurs as one to three ulcers at any one time;
- Ulcers are greater than 1cm in diameter;
- Involve any oral sites;
- May take several weeks to heal.
- Herpetiform RAS:
- Involves between 10 and 50 small ulcers at non-keratinised sites that heal within 10–14 days.
Questions regarding the number of ulcers present at any one time, the sites of the mouth affected and length of healing time will inform the type of RAS present.
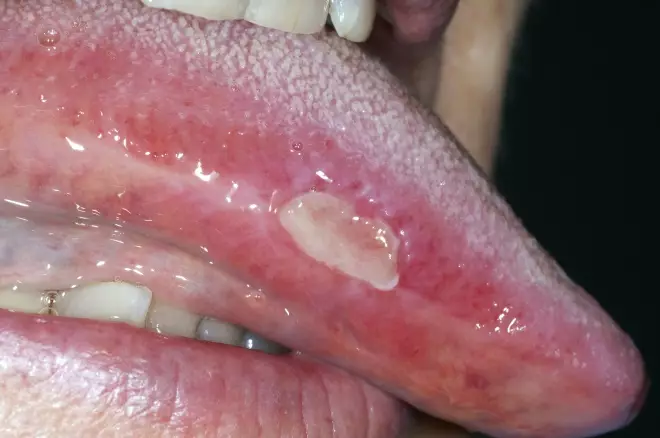
Figure 2: Recurrent aphthous stomatitis
Source: Science Photo Library
Aetiology and presentation
A range of aetiological factors have been implicated in RAS, including haematinic deficiency, hypersensitivity reactions and psychological stress[5],[6]
.
Vegetarians and vegans can develop iron deficiency anaemia, while some women experience iron deficiency owing to heavy menstrual bleeding. Pharmacists and healthcare professionals should question the patient about aspects of their diet and menstrual cycle to elucidate the cause of the ulcer. However, if abdominal symptoms are reported, patients should be referred to a medical practitioner for possible haematological assessment and exclusion of gastrointestinal disease.
Food preservatives, specifically benzoic acid and benzoates (E210–E219), chocolate and tomatoes have also been implicated in the causation of RAS, as well as toothpastes containing the foaming agent, sodium lauryl sulphate. Advice to avoid these substances should be given to those presenting with this condition.
It is generally accepted that RAS can develop during periods of psychological stress, and it is worth discussing this with patients.
The onset of RAS and RAS-like ulcers has also been reported as an adverse drug event[7]
, while some patients begin to experience mouth ulcers when they quit smoking (although the aetiological basis for this is unclear)[6]
.
Management
Management of all three types of RAS include the topical use of antiseptic, non-steroidal and steroid preparations (see Box 3). Fluticasone furoate nasal spray, fluticasone propionate nasal spray, fluocinolone gel and betamethasone sodium phosphate dispersible tablets are used as alternatives to steroid preparations in specialist practice.
A doxycycline (prescription-only medicine) mouthwash, prepared by breaking a 100mg capsule into 10mL of water and then used as a mouthwash for two minutes, three times daily, has been reported to be helpful in some cases of RAS and is included in the BNF
[8]
. However, this is not licensed for children aged under 12 years, and is contraindicated during pregnancy or for breastfeeding mothers, owing to the possibility of defects in developing teeth.
A range of topical preparations are advertised for mouth ulcers (e.g. choline salicylate, cetylpyridinium, chlorocresol, lignocaine [lidocaine], carbenoxolone). While some patients may find these products helpful, there is little scientific evidence to support their claimed efficacy.
Several systemic drugs have been reported to help in RAS that does not respond to topical therapy. These include thalidomide, dapsone and colchicines (LongoVital®; Orkla Care, Denmark), which is a herbal supplement with multivitamins[9]
. However, the use of systemic agents should only be initiated in specialist centres.
Geographic tongue
Aetiology and presentation
The condition (also known as benign migratory glossitis or erythema migrans) is extremely prevalent and can affect any age group, including young children. The aetiology of geographic tongue is unknown; however, histopathologically, it resembles psoriasis. It can be diagnosed from the characteristic clinical appearance and history of symptoms.
Individuals with geographic tongue characteristically complain of having ‘mouth ulcers’; however, geographic tongue is not true ulceration; it consists of irregular areas of loss of epithelial papillae on the dorsum and lateral margins of the tongue (see Figure 3).
Questioning the patient will reveal:
- The ‘ulcers’ are multiple;
- They are painful when eating hot or spicy foods;
- They are limited to the tongue;
- They change rapidly in appearance over a period of a few days.
Management
Individuals should be reassured about the benign and noninfectious nature of the condition. First-line treatment is a dispersible form of zinc sulphate (Solvazinc®; Galen Limited, Northern Ireland) at a dose of 125mg as a mouthwash for two minutes, three times daily over a period of three months. Symptomatic geographic tongue may also respond to topical agents (see Box 3).
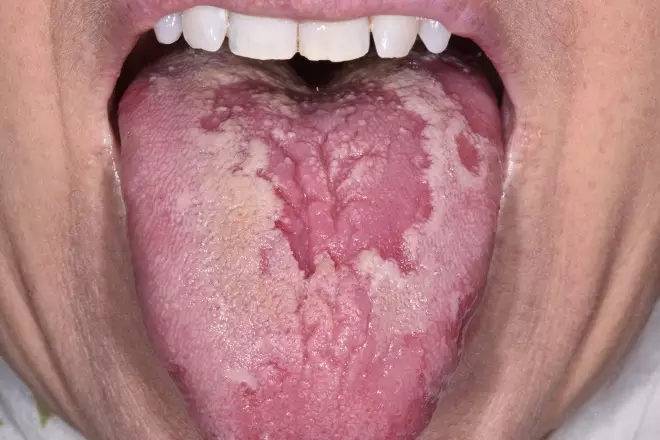
Figure 3: Geographic tongue
Source: Science Photo Library
Squamous cell carcinoma
Aetiology and presentation
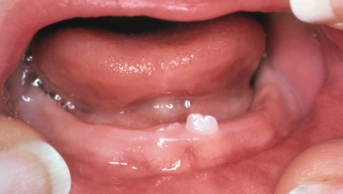
The clinical presentation of squamous cell carcinoma can vary greatly, but often involves a single, persistent ulcer. Although any site in the mouth can be involved, the majority of cases develop in the floor of the mouth, under the tongue (see Figure 4) or in the retromolar region (the space at the rear of the mandible). Mouth cancer is usually painless in its early stages; therefore, the majority of tumours are not detected until the individual seeks help with increasing discomfort or other problems in the mouth.
The aetiology of mouth cancer remains unknown, but presently, the two most important factors are believed to be tobacco use and the consumption of alcohol[10]
. Betel nut chewing — chewing the fruit of the areca palm for its stimulant effects — is popular in some ethnic groups[11]
. As betel nut chewing is also an important factor in the development of squamous cell carcinoma, it is something that should be considered to establish diagnosis. Suspicion of possible mouth cancer is heightened if the patient confirms any of the social habits mentioned, especially in combination.
The human papillomavirus can also infect the mouth and throat, and there is increasing evidence to support its role in oropharyngeal cancer[12]
.
Management
Almost 60% of people with oral cavity cancer survive for five years or more after diagnosis[13]
. However, diagnosis can only be made by biopsy; therefore, patients with suspected mouth cancer or a mouth ulcer that persists for more than three weeks, should be referred immediately to their GP or dental practitioner.
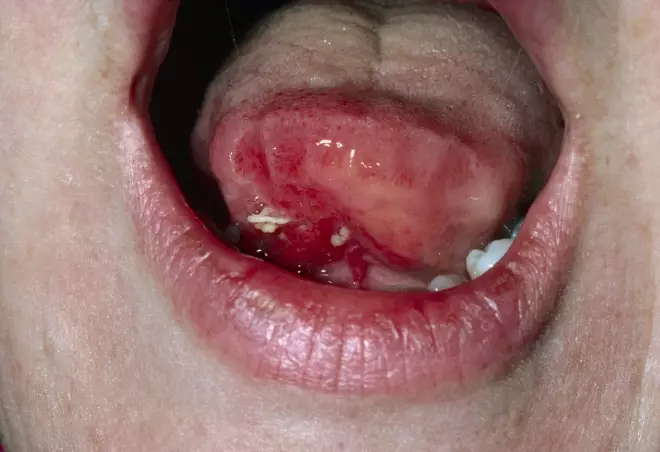
Figure 4: View of squamous cell carcinoma of the tongue
Source: Science Photo Library
Primary herpetic gingivostomatitis
Aetiology and presentation
Primary herpetic gingivostomatitis, as a result of infection with herpes simplex virus type 1 (HSV-1), is the most frequent viral infection of the mouth[14]
. It has been estimated that up to 90% of the population worldwide is seropositive for HSV-1 by the age of 40 years[15]
. The blisters of primary herpetic gingivostomatitis rupture rapidly to produce blood-crusted lips and widespread painful oral ulceration (see Figure 5). The ulceration is extremely painful, with multiple small ulcers affecting any site in the mouth. Concurrent symptoms include pyrexia, headache and cervical lymphadenopathy. It is important to bear in mind that the patient may be presenting with initial HSV-1 infection and, as such, there would not have been a previous episode of similar symptoms.
Management
Since the majority of cases develop in early childhood (and are often unnoticed or incorrectly dismissed as an episode of teething), parents of a child with suspected HSV-1 should be informed of the infectious nature of the condition. Instruction should be given to limit contact with the lips and mouth to reduce the risk of the spread of the virus to other sites.
Supportive symptomatic therapy should include the following:
- A chlorhexidine mouthwash;
- Analgesic therapy (e.g. paracetamol);
- Soft diet;
- Adequate fluid intake.
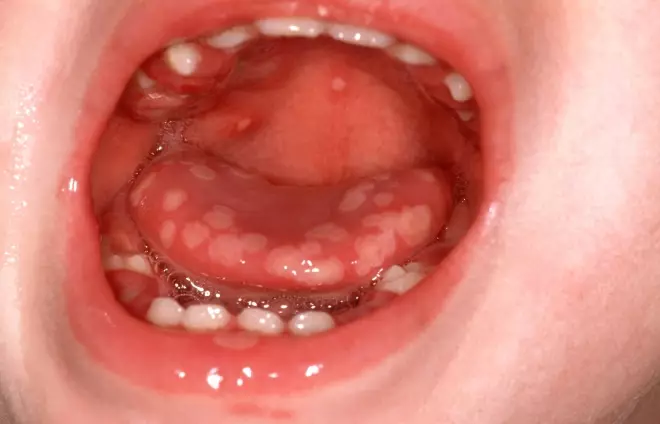
Figure 5: Primary herpetic gingivostomatitis
Source: Alamy
In otherwise healthy individuals, primary infection with HSV-1 will resolve within 7–10 days. Referral to a dentist or medical practitioner should be advised in immune-compromised patients, or in children with widespread severe symptoms, to consider the need for antiviral therapy. First-line treatment is aciclovir. The standard regimen is 200mg aciclovir as suspension (100mg/5mL) five times daily for five days. This dosage is halved in children under two years of age.
Lichen planus
Aetiology and presentation
This mucocutaneous, immune-mediated disorder has been reported to affect around 2% of the Western population, including the UK[16]
. The condition may be limited to the mouth or skin, although some patients have involvement at both these and other sites.
The intra-oral presentation is characterised by the presence of bilateral and symmetrical white patches, which principally affect the buccal mucosae, labial mucosa, tongue and attached gingivae.
Traditionally, lichen planus has been divided, based on clinical features, into a number of subtypes that include:
- Reticular;
- Erosive;
- Plaque-like;
- Atrophic;
- Bullous.
However, drawing a clear division between subtypes is often difficult. Many patients may show evidence of different subtypes of lichen planus, not only at different sites within the mouth, but also at different times in the duration of the condition (see Figure 6). Diagnosis can be made relatively easily on clinical symptoms alone, especially in patients who also have skin involvement.
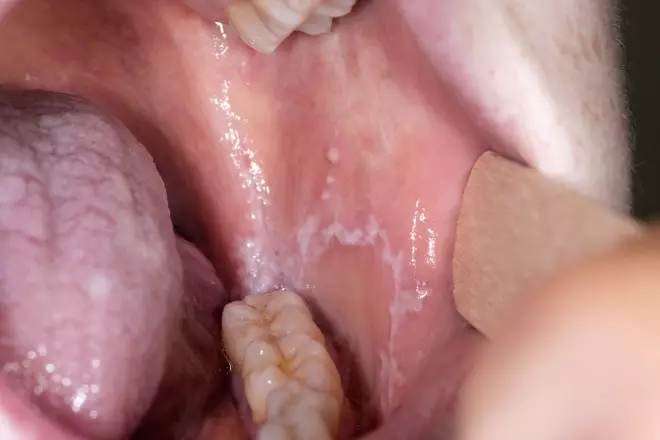
Figure 6: Lichen planus affecting the mucosal surface of the cheek
Source: Science Photo Library
Management
Pharmacists and healthcare professionals should advise patients that lichen planus is generally accepted to be a benign condition, although occasional cases of oral cancer arising in lichen planus have been reported. No active treatment is required in asymptomatic cases.
Symptomatic management involves the use of topical agents (see Box 3). Fluticasone furoate nasal spray, fluticasone propionate nasal spray, fluocinolone gel and betamethasone sodium phosphate dispersible tablets are used as alternative steroid preparations in specialist practice, along with the calcineurin inhibitor, tacrolimus. The use of systemic drug therapy for lichen planus includes prednisolone and a range of immunosuppressive agents[17]
.
It is worth asking patients with suspected lichen planus about their drug history, as a lichenoid drug reaction is a well-recognised adverse drug event to a number of widely used therapies, including non-steroid anti-inflammatory drugs, antihypertensives and oral hypoglycaemic agents. For example, oral ulceration has been reported following the introduction of the potassium-channel activator, nicorandil, for the prevention of angina[18]
. Adverse drug reactions should be reported using the Yellow Card Scheme.
When to refer
Referral to a dental practitioner is required when an ulcer is thought to be traumatic owing to contact with teeth or other structures in the mouth. If there is a suspicion of mouth cancer or atypical oral ulceration, patients should visit their dental practitioner or GP. Patients with RAS who also report abdominal symptoms or possible blood loss should be referred to their GP, as should patients with severe HSV-1 infection. Any cases where the onset of ulceration coincides with the initiation of a new systemic medicine should be reported as suspected adverse drug event and referral to a GP.
Useful resources
- Scottish Dental Clinical Effectiveness Programme Drug Prescribing For Dentistry. Free online app available at: www.sdcep.org.uk
- The British Society for Oral Medicine: www.bsom.org.uk
References
[1] Lewis MAO & Jordan RCK. Oral Medicine. London: CRC Press; 2012
[2] Lewis MAO & Lamey PJ. A Guide to Clinical Oral Medicine. 3rd edn. London: British Dental Association; 2011
[3] Holmes RG, Chan DC & Singh BB. Chemical burn of the buccal mucosa. Am J Dent 2004;17(3):219–220. PMID: 15301223
[4] Scully C. Aphthous ulceration. N Eng J Med 2006;355(2):165–172. doi: 10.1056/NEJMcp054630
[5] Scully C, Gorsky M & Lozada-Nur F. The diagnosis and management of recurrent aphthous stomatitis: a consensus approach. J Am Dent Assoc 2003;134(2):200–207. PMID: 12636124
[6] Gavic L, Cigic L, Lukenda DB et al. The role of anxiety, depression, and psychological stress on the clinical status of recurrent aphthous stomatitis and oral lichen planus. J Oral Pathol Med 2014;43(6):410–417. doi: 10.1111/jop.12148
[7] Yuan A & Woo SB. Adverse drug events in the oral cavity. Oral Surg Oral Med Oral Pathol Oral Radiol 2015;119(1):35–47. doi: 10.1016/j.oooo.2014.09.009
[8] Joint Formulary Committee. British National Formulary. 74th Edn. London: BNF Publications; 2018
[9] Brocklehurst P, Tickle M, Glenny AM et al. Systemic interventions for recurrent aphthous stomatitis (mouth ulcers). Cochrane Database Syst Rev 2012;(9):CD005411. doi: 10.1002/14651858.CD005411.pub2
[10] Hunter KD & Yeoman CM. An update on the clinical pathology of oral precancer and cancer. Dent Update 2013;40(2):120–122, 125–126. doi: 10.12968/denu.2013.40.2.120
[11] NHS. Mouth cancer. 2016. Available at: https://www.nhs.uk/conditions/mouth-cancer/causes/ (accessed March 2019)
[12] Centers for Disease Control and Prevention. HPV and oropharyngeal cancer. 2018. Available at: https://www.cdc.gov/cancer/hpv/basic_info/hpv_oropharyngeal.htm (accessed March 2019)
[13] Cancer Research UK. Mouth and oropharyngeal cancer: survival. 2018. Available at: https://www.cancerresearchuk.org/about-cancer/mouth-cancer/survival (accessed March 2019)
[14] Kolokotronis A & Doumas S. Herpes simplex virus infection, with particular reference to the progression and complications of primary herpetic gingivostomatitis. Clin Microbiol Infect 2006;12(3):202–211. doi: 10.1111/j.1469-0691.2005.01336.x
[15] National Institute for Health and Care Excellence. Clinical knowledge summaries: herpes simplex — oral. 2016. Available at: https://cks.nice.org.uk/herpes-simplex-oral (accessed March 2019)
[16] De Rossi SS & Ciarrocca K. Oral lichen planus and lichenoid mucositis. Dent Clin North Am 2014;58(2):299–313. doi: 10.1016/j.cden.2014.01.001
[17] Thongprason K, Carrozzo M, Furness S & Lodi G. Interventions for treating oral lichen planus. Cochrane Database of Syst Rev 2011;(7):CD001168. doi: 10.1002/14651858.CD001168.pub2
[18] Scully C, Azul A, Crighton A et al. Nicorandil can induce severe oral ulceration. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2001;91(2):189–193. doi: 10.1067/moe.2001.110306