This content was published in 2011. We do not recommend that you take any clinical decisions based on this information without first ensuring you have checked the latest guidance.
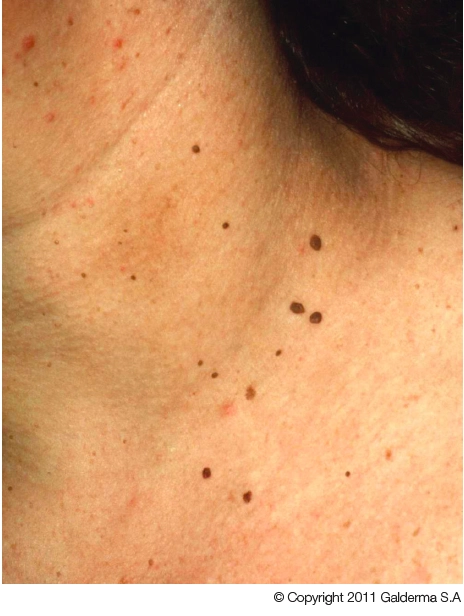
A: These look like skin tags, also known as acrochorda, cutaneous papilloma, fibroepithelial polyps, fibroma molluscum, soft fibroma and fibroma pendulum.
Skin tags are small, stalk-like outgrowths of epidermal and dermal tissue, which can grow up to 5cm but are normally much smaller. They are usually seen in skin fold areas of the body, such as the neck, groin and armpits.
They can also occur on the eye lids, abdomen, back and in the anal and vulvo-vaginal areas.
The vast majority of skin tags are benign tumours but one study of 1,335 lesions found that four were basal cell carcinomas and one was a squamous cell carcinoma. Nevertheless, the authors suggest that the malignancy potential of skin tags is low. Patients experience few, if any, problems with skin tags although pruritus and discomfort can occur if the lesions are snagged by jewellery.
Sometimes skin tags can change colour and become black and this is usually when a lesion becomes thrombosed — it will drop off after a few days.
Other common skin lesions that can be mistaken for skin tags are neurofibromas, seborrhoeic warts, viral warts and molluscum contagiosum.
Causes
Skin tags are thought to affect up to 46 per cent of the population. Prevalence rises with age such that as much as 59 per cent of the population has skin tags by the age of 70 years.
There appears to be an association between the incidence of skin tags and obesity as well as insulin resistance and atherosclerosis.
The causes of skin tags are not entirely clear but their presence in skin fold areas suggests that friction or frequent irritation is a potential cause. The condition appears to have a genetic component (there is a tendency for skin tags to occur in families) but other potential causes include hormonal imbalances. For example, skin tags are associated with agromegaly, the growth hormone disorder.
The presence of oestrogen and androgen in skin tag biopsies (and the fact that skin tags are often seen in pregnancy), suggests that sex hormones have a potential role in the development of these lesions.
Studies have found some types of human papilloma virus in skin tag biopsies, suggesting the virus is involved. Skin tags are also a cutaneous feature of Birt-Hogg-Dubè syndrome, a rare genetic disorder that leads to the development of renal and colonic cancers.
Treatment
Skin tags themselves are generally harmless and require no treatment but many patients want them removed for cosmetic reasons. There are no specifically licensed over-the-counter remedies and patients should be advised not to use salicylic acid based wart treatments on skin tags because these can damage the skin, causing scarring.
(Although unlicensed for the treatment of skin tags, some patients have used Wartner in an effort to remove them.)
Self-treatment by ligating the skin tag base with dental floss or fine thread and waiting for the tag to drop off is a home remedy that has been recommended.
Products based on essential oils (including tea-tree and castor oil) are advertised on the internet but none is licensed and there is little evidence of efficacy.
If patients have a large number of skin tags or if the lesions are bothersome, then GP treatments include cryotherapy (with liquid nitrogen), surgical excision or burning off the skin tag with a Hyfrecator (an electrosurgical device). Both surgical excision and hyfrecation give instant results. With cryotherapy patients will often need a few treatments before the lesions completely clear.
You might also be interested in…
How to select the right mouthwash

Thalassaemia and iron supplements