This content was published in 2009. We do not recommend that you take any clinical decisions based on this information without first ensuring you have checked the latest guidance.
Summary
MRSA skin and soft tissue infections are an increasing management challenge. Health care associated MRSA, affecting older compromised patients presents in both the community and hospital contrasts with the rarer true community associated MRSA which affects healthy young people. Newly licensed agents are now in use in many UK hospitals and other agents are in the advanced stages of development. How these new agents should be optimally deployed is uncertain but prudent use to safe guard future treatment options seems wise at the present time.
In hospitals S.aureus, dominates as the cause of surgical site infection with rates of MRSA. in the UK of between 30 and 40% of S. aureus blood stream isolates. 1 Health care associated MRSA (HA-MRSA) SSTIs are recognised in both hospitalised patients as well as in patients presenting from the community or from long term care facilities. Such patients usually will have an identifiable risk history (see below). Community associated MRSA (CA-MRSA) is an emerging entity, more akin to CA-MSSA and characterised by lack of healthcare-associated risk factors.
Clinical features of MRSA SSTI
Clinical differences between HA-MRSA and CA-MRSA (box 1) can largely be explained by the production of the Panton Valentine leucocidin (PVL) toxin in CA-MRSA. This characteristic virulence factor in S. aureus, recognised since the 1950s and prior to the emergence of MRSA, kills peripheral mononuclear cells in vitro and is associated with intense localised tissue destruction. PVL has not been a prominent feature of HA-MRSA.

Healthcare-associated MRSA
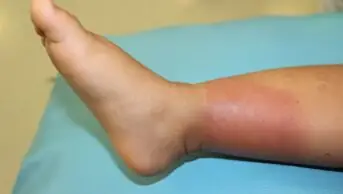
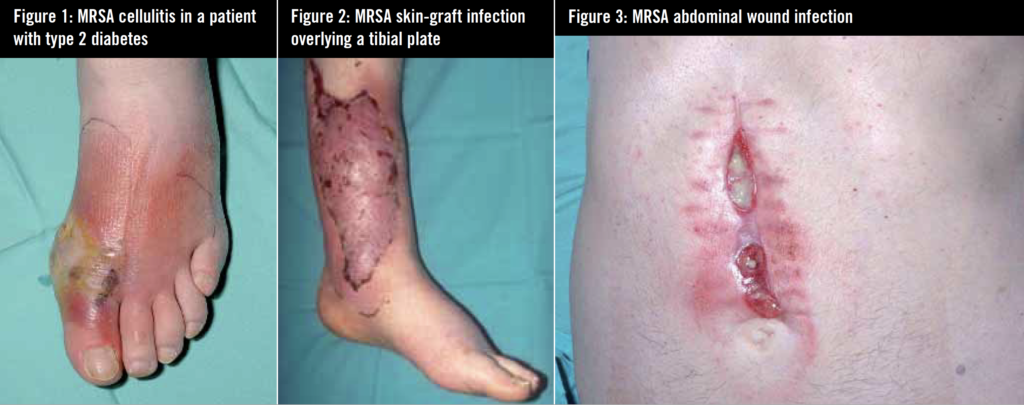
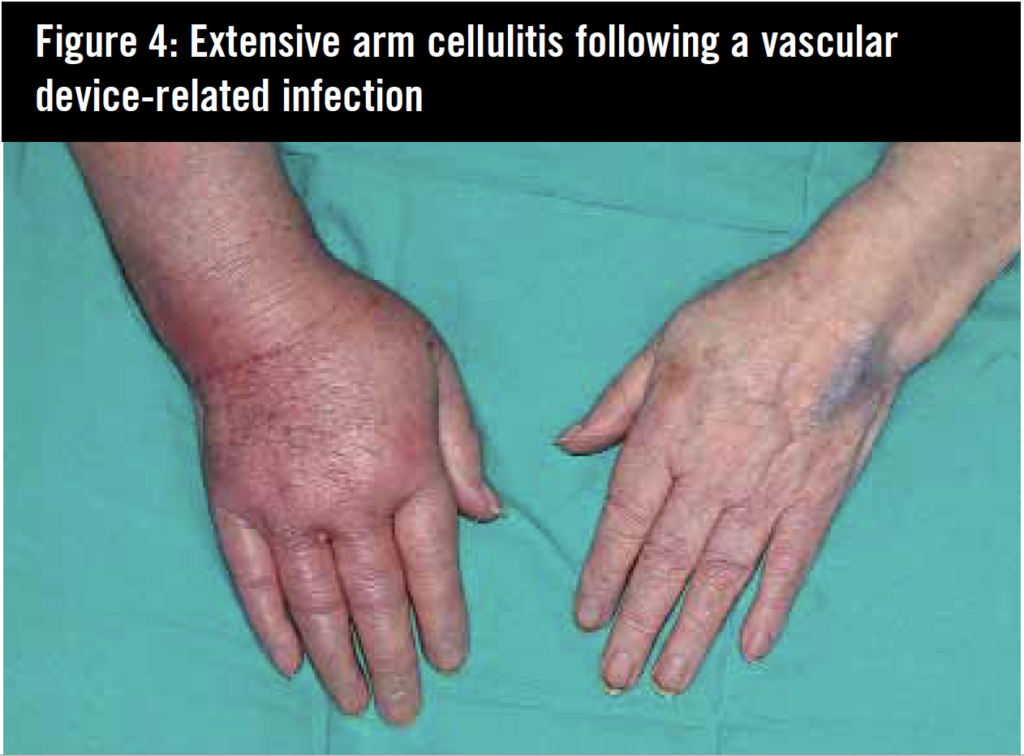
HA-MRSA affects predominantly elderly or compromised patients. Co-morbidity is usual. Diabetes mellitus (figure 1), vascular disease and recurrent hospital admissions, indwelling urinary catheters and vascular devices are important risk factors.2 Prior antibiotic therapy with fluoroquinolones, cephalosporins and macrolides are important risk factors predisposing to MRSA colonisation. 3 Prior colonisation or infection itself is an independent risk factor for subsequent infection. 4 Presentation is with surgical site infection (figure 2 and 3), vascular device–related infection (figure 4), primary bacteraemia or deep-seated infection.
Management of HA-MRSA SSTI
In superficial surgical site infection, deeper infection and blood stream infection should be considered and excluded, particularly if foreign material is present. Clinical assessment for systemic inflammatory response and potential other foci of infection (septic arthritis, endocarditis etc) and blood cultures are mandatory. Response to antibiotics is unlikely without removal or debridement of associated devices or collections. This may be difficult when maintenance of vascular access is essential or prosthetic material is deeply embedded. Management must be discussed with the appropriate surgical specialist. Parenteral therapy is usually required initially (see below). In mild infections combination therapy with two “old” antibiotics is usually effective. Monotherapy is discouraged as is associated with rapid development of resistance. Agents that can be used in combination include doxycycline 100mg 12 hourly, fusidic acid 500mg 8 hourly, trimethoprim 200mg 12 hourly and rifampicin 300mg-600mg 12 hourly. Trimethoprim-sulphamethozazole (co-trimoxazole) is another alternative. Linezolid 600mg bd (see below) is an option for use under expert guidance, but should be reserved for patients who are unable to tolerate above regimens.
Community-associated MRSA
CA-MRSA causes a broad range of SSTI from furunculosis, carbuncles and simple abscesses to cellulitis and necrotising infections in a number of patient populations predominantly in North America and Australia. Its role and extent in community acquired SSTI in Europe is not well defined. .In contrast to HA-MRSA infections, CA-MRSA affects healthy young adults with notable reported outbreaks in contact sports teams, prisons and men who have sex with men reflecting spread in crowded environments.5 CA-MRSA is associated with increased transmission, recurrence, complications and hospitalisation. In some US areas significant proportions of serious S. aureus presenting in community practice are due to CA-MRSA. 6
Management of CA-MRSA SSTI
Incision and drainage should be performed when a collection is evident. Localised infections may require no further therapy although short course oral therapy as above is recommended. In contrast to HA-MRSA, CA-MRSA may be sensitive to clindamycin and so may be an additional option. Management of severe and progressive SSTIs are discussed below.
Antibiotic treatment of severe MRSA SSTIs
Current UK MRSA management guidance does not specify a particular agent for MRSA SSTI, but indicates that when local meticillin resistance in S. aureus, exceeds 10%, then empirical anti-Staphylococcal therapy should incorporate activity against MRSA. 7 This would apply to most suspected healthcare-associated S. aureus infection in the UK. Empirical therapy versus CA-MRSA in SSTI is currently not justified in the UK. Parenteral therapy should be used in any severe SSTI as defined in the accompanying article.
Vancomycin
Glycopeptides have been the agents of choice for MRSA since the discovery of the Streptomyces product, vancomycin.. Initially a rapidly bacteriocidal agent in all S. aureus, binding of vancomycin to D-alanine, a component of peptide-glycan in Gram positive organism cell wall leads to inhibition of cell wall synthesis and bacterial death. Initial used in penicillin-resistant Staphylococci in the 1950s, use increased in the 1980s when MRSA was recognised. Epidemic strains of MRSA in the 1990s in UK hospitals lead to an explosion in vancomycin usage. Despite widespread use resistance has been slow to develop and resistance has only been recorded in the USA in <10 patients.8 More troubling is the emergence of heterozygous resistance to vancomycin where small populations of intermediate-resistant organisms may amplify under selection pressure following glycopeptide exposure resulting in treatment failure.9 A slow but steady “creep” in the mean inhibitory concentration (MIC) over time has been observed. Thickening of the MRSA cell wall is associated with loss of cidality and treatment failure. This is of particular concern as cell wall thickening may also confer partial resistance to newer agents such as daptomycin.
Despite these concerns for the majority of MRSA SSTIs vancomycin remains an entirely appropriate choice of agent. Dosing regimens and target trough concentrations vary between institutions and currently there is no national or international consensus on targets. Loading dose is weight dependent and subsequent dose and interval is dependent on weight and creatinine clearance. Higher trough concentrations should be considered in deep seated or serious MRSA infections (target trough concentrations of between 10-25mg/kg). Some favour continuous intravenous infusion (cIVI) of vancomycin over 24 hours to avoid unnecessary peaks in concentration following a standard, weight adjusted loading dose (see www.glasgowformulary.com). This is well tolerated and gives a constant high concentration above the MIC for the entire 24 hours. Although not demonstrated to be superior to standard bolus IV dosing cIVI does deliver higher concentrations of vancomycin, avoiding very high peak concentrations.
Side-effects of vancomycin have been over-estimated. The “red man syndrome” due to impurities in the original formulation of vancomycin is no longer seen due to purification. Infused too quickly, vancomycin is associated with flushing due to histamine release. Renal dysfunction is a rarity if cIVI is used but may be associated with high peak concentrations when high dose bolus IVI regimen used.10 Glycopeptide-associated thrombocytopenia, is a rare complication of usually prolonged therapy and usually will resolve on discontinuation.
Teicoplanin
The other glycopeptide in widespread use in the UK and Europe is teicoplanin. Despite having been used in Europe since the late 1980s it remains an “investigational drug” in USA. It is more highly protein bound than vancomycin and as a consequence has a much longer t1/2 but lower free drug concentration. This allows for once daily dosing 400mg (after initial loading) although in severe infections higher unlicensed doses are commonly used (600-1000mg /day). Therapeutic drug monitoring is not routinely available and therefore most dosing regimens are “guesstimates”. In general for MRSA SSTI one would aim for a trough concentration of 10-20mg/l but higher if bacteraemia was likely. High dose, weight based intermittent dosing (10-15mg/kg three times per week following a daily loading regimen for 3 days) may be used in MRSA SSTI in the OPAT setting. Hetero-resistance in MRSA is also described with teicoplanin and the same question marks regarding declining efficacy are true for teicoplanin as they are for vancomycin. There is no evidence to support superiority of teicoplanin over vancomycin (or vice-versa) in SSTI and teicoplanin is currently more expensive than generic vancomycin, Teicoplanin use in hospitals is therefore a balance between convenience (of once daily bolus IV) and cost.
Quinupristin with dalfopristin
Two naturally occurring streptogramin antibiotics are combined in this bacteriocidal compound. Although only IV formulated, the oral streptogrammin, pristinamycin is available in mainland Europe and can be used in the UK on a named patient basis following import. The streptogramins maintain excellent activity against MRSA and have been shown to be non-inferior to vancomycin in complicated SSTI. 11 Use of the IV agent has been hampered by troublesome thrombophlebitis and thrice daily administration. Use of this agent has been limited in the UK and it is currently reserved for severe MRSA infections where treatment with other conventional licensed products has failed.
Linezolid
The oxazolidanone, linezolid, licensed in 2001 is bacteriostatic against S. aureus. It binds to the 50S ribosomal subunit, preventing production of the 70S subunit. Dose is 600mg (IV or oral) 12 hourly, it is not highly protein bound, is widely distributed and has excellent oral bioavailability allowing oral switch and potentially early hospital discharge without the need for continuation of IV therapy. Clinical trials have shown non-inferiority to the glycopeptides in SSTI although a sub set analysis showed greater cure rate in MRSA infected patients.12 Economic advantages have also been demonstrated in earlier oral switch and hospital discharge. Side-effects are well described, including marrow (notably thrombocytopenia and anaemia) and mitochondrial toxicity (with peripheral neuropathy and optic neuritis). Linezolid is a weak mono-amine oxidase inhibitor, so concomitant use with anti-depressants is cautioned. For most SSTIs linezolid is an acceptable option and can be considered in patients with poor IV access, in those in whom it is advantageous to discharge early on oral therapy and in failure or intolerance with glycopeptides. Caution should be exercised with respect to toxicity and use beyond 4 weeks is not recommended. Resistance in MRSA is described, although usually in patients with deep-seated infections associated with irremovable foci of infection.
Tigecycline
Tigecycline is a novel glycycline that binds to the 30S subunit of the ribosome of Gram-positive and negative organisms. Bacteriostatic, with a broad spectrum (excluding Pseudomonas) and rapid and wide volume of distribution, it has demonstrated non-inferiority in complicated SSTIs in clinical trials compared with vancomycin plus aztreonam.13 Dosing is twice daily 50mg IV although a once daily regimen is being evaluated. No oral formulation is available and main side-effect is nausea. Use should generally be restricted for those SSTIs where polymicrobial infection is suspected and other conventional formulary agents have failed or are contra-indicated.
Daptomycin
Daptomycin, a cyclic lipopeptide was licensed in Europe in 2006. Mode of action in Gram-positive organisms is calcium-dependent efflux of potassium following insertion of its lipophilic tail into the cell membrane leading to cell death. Concentration dependent bacteriocidal activity against MRSA is irrespective of growth phase. Protein binding is high with renal tract excretion. Dosing in SSTI is 4mg/kg although there is a trend toward higher dosing at 6mg/kg if the SSTI is severe, bacteraemia or deep sepsis is suspected or the patient is an intravenous drug user or suffering from burns when a wider volume of distribution is anticipated.14 Dosing interval increase to 48 hours when creatinine clearance < 30mls/min and following dialysis in renal replacement therapy. In obese patients dosing should be based on actual total body weight.
Daptomycin was non-inferior to vancomycin or penicillinase-resistant penicillins in complicated SSTI, although rapid cidality was suggested; 63% of daptomycin-treated patients received 4-7 days of therapy compared with 33% in the comparators.15 In phase 4 studies overall success in SSTI has been observed in >90% and in the sub groups of microbiologically evaluable patients with S. aureus infection (including a high proportion of MRSA infection) success rates were high comparing favourably with other studies. Sepsis, ICU stay, and Creatinine clearance <30 ml /min are associated with clinical failure in daptomycin-treated patients with SSTI. 14 Reduced daptomycin susceptibility in isolates exposed to vancomycin in some deep seated infections has questioned the utility of daptomycin in glycopeptide treatment failure although this has yet to be substantiated.
Daptomycin treatment-limiting skeletal muscle side-effects at 4mg/kg occur in 0.4%. These manifest as asymptomatic increase in creatinine phosphokinase, muscle pain, weakness, myositis or rarely rhabdomyolysis. Although not a true adverse event, daptomycin may lead to a spurious rise in the measured prothrombin time due to a test reagent reaction. This is of relevance when receiving concomitant warfarin or with sepsis-associated coagulopathy and may lead to prematurely discontinuation of daptomycin or confusion with anti-coagulation therapy.
Daptomycin’s once daily administration, efficacy in SSTI, low and predictable toxicity profile and activity versus MRSA make it ideal for outpatient administration.
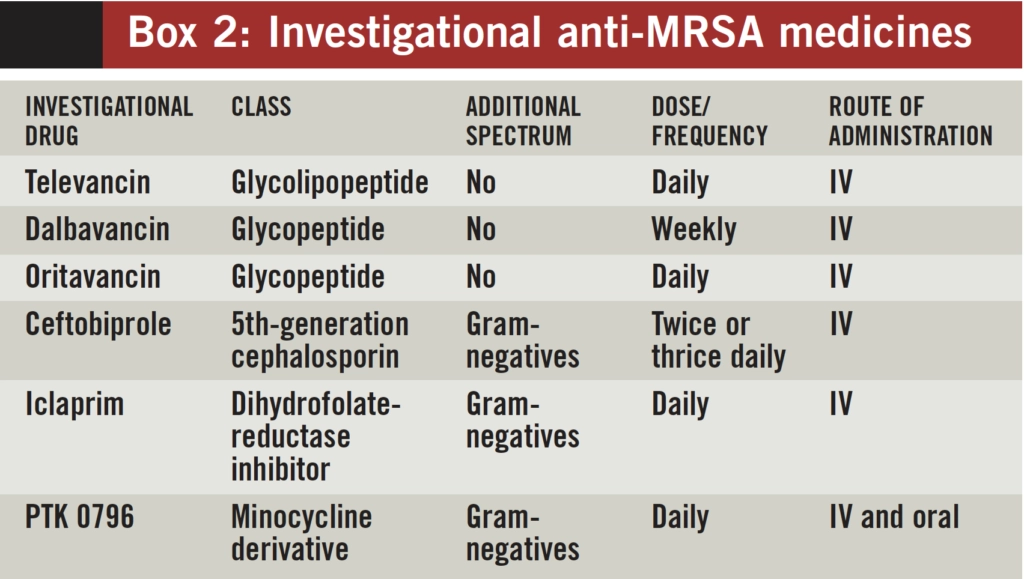
New medicines in the pipeline
There are a number of new agents close to approval (box 2). These represent re-engineering of existing drug groups including the glycopeptides (televancin,16 dalbavancin 17 and oritavancin 18), dihyrofolate reductase inhibitors (iclaprim), tetracyclines and cephalosporins (ceftobiprole 19). Some may prove useful as resistance to the currently available anti-MRSA agents emerges. Others, particularly the glycopeptide-derived agents may struggle for a market share given potential cross resistance. Dalbavancin, derived from teicoplanin, has an ultra-long half life allowing for weekly dosing and may prove useful in OPAT. 16 Ceftobiprole is the first beta-lactam agent to be engineered to overcome MRSA resistance. 17 Immediate concerns are the risk of promotion of Clostridium difficile and extended spectrum beta lactamase inhibitors. It may prove useful in polymicrobial, pulmonary or central nervous system infection.
Anti-MRSA drugs and hospital formularies
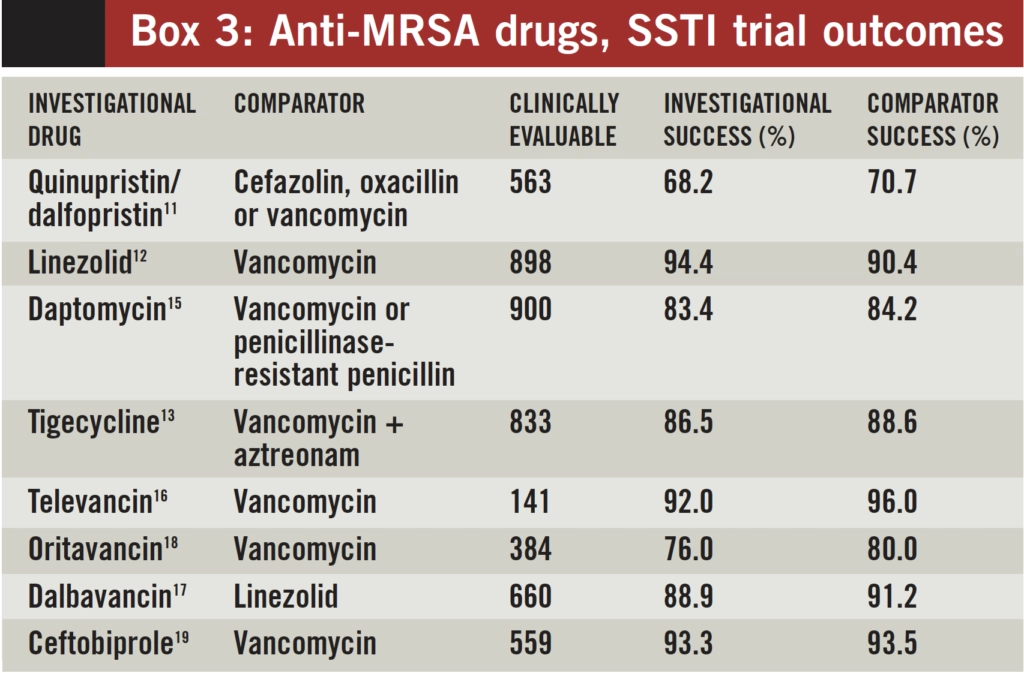
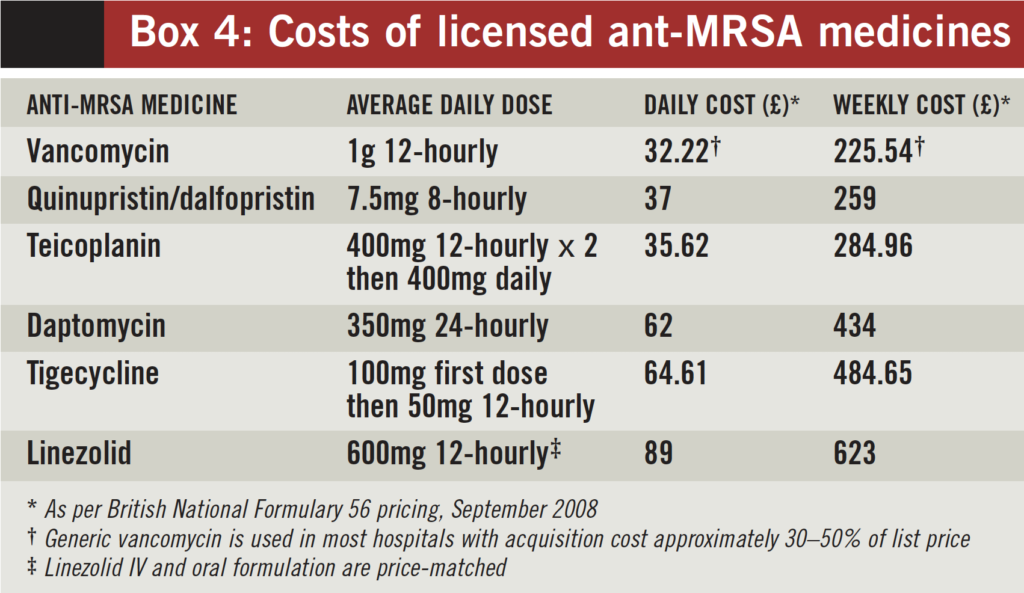
As in other areas of therapeutics, balancing cost with the promotion of the most efficacious agents can sometimes be difficult. Clinical trials have not demonstrated superiority of the newer agents over vancomycin in SSTI (box 3). Superiority of linezolid in a sub set analysis of a single trial requires substantiation before routine use is advocated. Widespread linezolid use will promote resistance and potentially unmask toxicity. Costs vary markedly between the different agents and generic vancomycin is considerably cheaper than all anti-MRSA alternatives (box 4). On balance therefore vancomycin remains the preferred antibiotic for HA-MRSA SSTI and other agents should be restricted to the advice of an infection specialist. To facilitate early discharge, teicoplanin (in OPAT) or linezolid can be considered although if oral therapy is possible then combination therapy with the older agents should be considered first. Until there is a powerful cost-benefit analysis produced (evidence of earlier hospital discharge or shorter duration of therapy), daptomycin should be reserved for those intolerant, allergic or failing on glycopeptide therapy and in view of its cidality, considered in severe and rapidly progressive SSTI where MRSA is either proven or strongly suspected or bacteraemia is likely. Optimal therapy of serious SSTI with CA-MRSA is not known but both inezolid and Daptomycin may have a role. Tigecycline should be reserved for those with polymicrobial SSTI where MRSA is implicated.
References
- European Antimicrobial Resistance Surveillance System. Susceptibility results for S. aureus isolates in 2005: http//www.rivm.nl/ears/database/
- Graffunder EM, Venezia RA. Risk factors associated with nosocomial methicillin-resistant Staphylococcus aureus (MRSA) infection including previous use of antimicrobials. J Antimicrob Chemother 2002; 49: 999-1005
- Taconelli E, De Angelis G, Cataldo M A, Pozzi E, Cauda R. Does antibiotic exposure increase the risk of methicillin-resistant Staphylococcus aureus (MRSA) isolation? A systematic review and meta-analysis. J Antimicrob Chemother 2008; 61: 26-38
- Huang SS, Platt R. Risk of methicillin-resistant Staphylococcus aureus infection after previous infection or colonization. Clin Infect Dis2003; 36: 281-285.
- Fridkin SK, Hageman, Morrison M, Sanza LT, Como-Sabetti K, Jernigan JA, Harriman K, Harrison LH, Lynfield R, Farley MM. Methicillin-resistant Staphylococcus aureus in three communities. N Eng J Med 2005; 352: 1436-1447
- Morgan GJ, Krishnadasan A, Gorwitz RJ, Fosheim GE, McDougal LK, Carey RB, Talan DA et al. Methicillin-resistant S. aureus infections among patients in the emergency department. N Eng J Med 2006; 355: 666-674
- Gemmel CG, Edwards DI, Fraise EP, et al. Guidelines for the prophylaxis and treatment of methicillin-resistant Staphylococcus aureus (MRSA) infections in the UK. J Antimicrob Chemother2006, 57:589-608.
- Sievert DM, Rudrik JT, Patel JB, McDonald LC, Wilkins MJ, Hageman JC. Vancomycin-resistant Staphylococcus aureus in the United States, 2002-2006 Clin Infect Dis 2008; 46: 668-674
- Sakoulas G, Moise-Broder PA, Schentag J et al. Relationship of MIC and bactericidal activity to efficacy of Vancomycin for treatment of methicillin-resistant Staphylococcus aureus bacteremia. J Clin Microbiol 2004; 42: 2398–402.
- Hidayat LK, Hsu DI, Quist R et al. High-dose vancomycin therapy for methicillin-resistant Staphylococcus aureus infections: efficacy and toxicity. Arch Intern Med 2006; 166: 2138–44.
- Nichols R L, Graham D R, Barriere S L, Rodgers A, Wilson S E, Zervos M et al Treatment of hospitalised patients with compliocated Gram-positive skin and skin structure infections: two randomised, multicentre studies of quinupristin/dalfopristin versus cefazolin, oxacillin or vancomycin. J Antimicrob Chemother 1999; 44: 263-273
- Weigelt J, Itani K, Stevens D et al. Linezolid versus vancomycin in treatmet of complicated skin and soft tissue infection. Antimicro Ag Chemother 2005; 49: 2260-2266
- Ellis-Grosse E J, Babinchak T, Dartois N, Rose G, Loh E. The efficacy and safety of tigecycline in the treatment of skin and skin structure infections: results of a double blind phase 3 comparison studies with vancomycin-aztreonam. Clin Infect Dis 2005; 41 suppl 5: S341-53
- Seaton R A. Daptomycin: rationale and role in the management of skin and soft tissue infection. J Antimicrob Chemother 2008; 62 Supp; 3 iii15-iii23
- Arbeit R D, Maki D, Tally F, Campanaro E, Eisenstein B I. The safety and efficacy of daptomycin for the treatment of complicated skin and skin structure infections. Clin Infec Dis 2004; 38: 1673-1681
- Stryiewski M E, O’Riordan W D, Lau W K, Pien F D, Dunbar L M, Vallee M, Fowler V G et al. Televancin versus standard therapy for treatment of complicated skin and soft tissue infections due to Gram-positive bacteria. Clin Infect Dis 2005; 40: 1601-1607
- Jauregui L E, Babazadeh S, Seltzer E, Goldberg L, Krievins D, Frederick M et al. Randomized double blind comparison of once weekly dalbavancin versus twice-daily linezolid therapy for the treatment of complicated skin and skin structure infections. Clin Infect Dis 2005; 41: 1407-1415
- Wasilewski M M, Disch D P, McGill J M, Harris H W, O’Riordan W, Zeckel M L. Equivalence of shorter course therapy with oritavancin vs vancomycin/cephalexin in complicated skin/ skin structure infections. Abstr Intersci Conf Antimicrob Agents Chemother 2001; Dec 16-19: 41: abstract no UL-18
- Noel G J, Strauss R S, Amsler K, Heep M, Pypstra R, Solomkin J S. Results of a double blind, randomised trial of ceftobiprole treatment of complicated skin and skin structure infections caused by Gram-positive bacteria. Antimicrob Agents Chemother 2008; 52: 37-44