This content was published in 2011. We do not recommend that you make any clinical decisions based on this information without first ensuring you have checked the latest guidance.
An updated version of this article was published in 2018 and can be found here.
Slurred speech, facial droop and arm weakness — it is critical that all healthcare professionals are alert for these signs of stroke to ensure that patients displaying them receive treatment quickly
Stroke is the third most common cause of death globally.1 In the UK it is a major health problem — the incidence of first ischaemic stroke is about 98,000 people each year and approximately 2% of people in England and Wales have had a stroke. About 23% of people die within 30 days of having a stroke and, of the people who survive, 60–70% die within three years.2
In terms of morbidity, stroke can cause hospital admissions, reduced quality of life and long-term disability.2 Stroke is the leading cause of disability in the UK and it is thought that more than 900,000 people in England are living with the effects of stroke, with about half of these dependent on others for support with everyday activities. In England, stroke is estimated to cost the economy around £7bn per year. This comprises direct costs to the NHS of £2.8bn, costs of informal care of £2.4bn and costs because of lost productivity and disability of £1.8bn.3
Summary
Stroke is a major cause of morbidity and mortality in the UK, yet about 80% of strokes are preventable. Factors that are known to increase the risk of stroke include age, gender, hypertension, atrial fibrillation, diabetes and cigarette smoking.
Broadly, a stroke can be classified as either ischaemic (caused by a thrombus) or haemorrhagic (caused by the rupture of blood vessels). Stroke is a medical emergency and the sooner that it is diagnosed and treated the better the outcome.
What is stroke?
Stroke is defined by the World Health Organization as a clinical syndrome consisting of “rapidly developing clinical signs of focal (at times global) disturbance of cerebral function, lasting more than 24 hours or leading to death with no apparent cause other than that of vascular origin”. A transient ischaemic attack (TIA) is defined as stroke symptoms and signs that resolve within 24 hours.3
However, these definitions have limitations. One example is that they are based on clinical features, not those seen with imaging.4 Also, the symptoms of a TIA usually resolve within minutes, or a few hours at most, and anyone with continuing neurological signs when first assessed should be presumed to have had a stroke.
Classification
Broadly, a stroke can be classified as either ischaemic or haemorrhagic. An ischaemic stroke is caused by an in situ thrombosis or distal embolism as a result of cardioembolic or atherosclerotic arterial disease. About 70% of strokes are ischaemic.
Haemorrhagic stroke can be further subdivided into intracerebral haemorrhage (usually caused by rupture of small penetrating vessels in the brain) and subarachnoid haemorrhage (caused by rupture of intracranial aneurysms contained within the subarachnoid space surrounding the brain).5
Strokes can be further classified according to the underlying cause or the affected region of the brain.
Risk factors
The American Stroke Association estimates that 80% of strokes are preventable. Medical knowledge about the risk factors for stroke is based on epidemiological studies. Most of these risk factors are associated with cerebral infarction and not cerebral haemorrhage. Risk factors can be divided into modifiable and non-modifiable, as below. Some rare risk factors are listed in Box 1.
Non-modifiable risk factors
Age
The chance of stroke approximately doubles with each decade of life after the age of 55 years. Stroke in younger patients (15–45 years) is rare and accounts for about 10% of all strokes.6
Gender
Stroke is more common in men than in women. In most age groups, more men than women will have a stroke in a given year. However, more than half of total stroke deaths occur in women. At all ages, more women than men die of stroke.
Other risk factors
Other risk factors for stroke include a family history of stroke, ethnicity (eg, Afro-Caribbean people are at higher risk) and genetic conditions, such as Fabry’s disease (see Box 1).
Box 1: Less common risk factors for stroke
- Cervical artery dissection
- Drugs (eg, oral contraceptive pill, hormone replacement therapy, illicit drug use)
- Fabry’s disease
- Fibromuscular dysplasia
- Haematological disorders
- Homocystinuria
- Infections
- Inflammatory vascular disorders
- Mitochondrial disorders
- Moyamoya syndrome
- Migraine
- Paradoxical embolism
- Pregnancy
- Sleep apnoea
- Sneddon’s syndrome
- Trauma
Modifiable risk factors
Hypertension
Hypertension is the single most important modifiable risk factor for stroke. In clinical trials, antihypertensive therapy has been associated with reductions in stroke incidence averaging 35–40%.7 Hypertension increases the risk of ischaemic stroke by promoting both large vessel atherogenesis and intracranial small vessel disease.
Atrial fibrillation
Atrial fibrillation (AF) is an important risk factor for stroke and is increasingly common with advancing age. AF is associated with about 15% of all strokes; treatment of AF (eg, rhythm control) can reduce the overall stroke risk by 10%. Anticoagulation reduces the risk of stroke for patients with AF by approximately 70%.
Diabetes
People with diabetes have a 2–2.5 times greater risk of stroke than non-diabetic people.
Hyperlipidaemia
Various trials in patients with ischaemic heart disease have shown that statins significantly reduce the incidence of stroke (in association with lowering cholesterol).
Smoking
The risk of stroke for males and females who smoke cigarettes is double that for non-smokers.
Others
Other modifiable risk factors include ischaemic heart disease, peripheral arterial disease, carotid or other artery disease. Minor modifiable risk factors include poor diet and obesity.
Clinical features
Stroke is a medical emergency and the sooner it is diagnosed and treated, the better the outcome. It is vital to distinguish between a stroke and conditions that may present as a stroke (see Box 2).
Box 2: Conditions that can mimic stroke8
The following are examples of conditions that can present with clinical features that mimic stroke:
- Seizure
- Sepsis
- Delirium
- Toxic or metabolic conditions (including hypoxia and drug overdose)
- Space-occupying lesion (eg, tumour)
- Vestibular disorders
- Dementia
- Migraine
- Spinal cord lesion
Generally, if a patient presents with a gradual onset of symptoms, without focal symptoms and with a history that suggests a non-vascular basis for the event (eg, migraine or seizure), a stroke might be excluded. However, there can be exceptions to this.
Validated formal screening tools are used to assist with the rapid diagnosis of a stroke. The two most commonly used are FAST (an acronym for face, arm, speech, time)9 and ROSIER (Recognition of stroke in emergency room).10 The FAST tool is quick and easy to use (see Box 3, p202). It lists the common clinical features of stroke — facial weakness or droop, arm (or leg) weakness and inability to speak clearly or comprehend speech. Recent media campaigns have aimed to highlight this checklist to the public so that they are able easily to recognise the signs and symptoms of stroke and call for the emergency services as soon as possible.
Box 3: Recognising stroke
FAST The Stroke Association urges people to recognise stroke symptoms FAST. FAST is an acronym for:9
- Facial weakness — Can the person smile? Has their mouth or eye drooped?
- Arm (or leg) weakness — Can the person raise both arms?
- Speech — Can the person speak clearly and understand what you say?
- Time to call 999
A stroke should be suspected if a person exhibits any of these symptoms.
ROSIER Another scale that can be used is the “Recognition of stroke in emergency room” (ROSIER) scale.10 Using the ROSIER scale, points are allocated based on the symptoms described below:
- Loss of consciousness or syncope? (−1 point)
- Seizure activity? (−1 point)
- New acute onset:
- Asymmetric facial weakness? (+1 point)
- Asymmetric arm weakness? (+1 point)
- Asymmetric leg weakness? (+1 point)
- Speech disturbance? (+1 point)
- Visual field defect? (+1 point)
A stroke is likely if a person scores >0 in the absence of hypoglycaemia.
The ROSIER scale is designed for use in emergency departments and is more in-depth than the FAST tool (although it can be completed in less than five minutes). This scale also includes screening for common conditions that can mimic stroke (see Box 3).10
Diagnostic investigations
Imaging and other investigations are required to diagnose stroke and to determine its cause.
Computed tomography
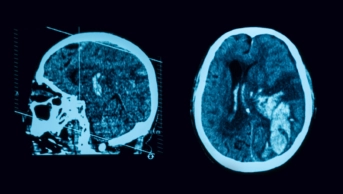
The diagnosis of stroke is confirmed with the help of brain imaging. Non-contrast computed tomography (CT) scanning is quick and safe. In the acute phase, haemorrhage is clearly visible as areas of high attenuation (ie, areas that look brighter than normal tissue — see Figure, p202). This appearance remains reliable for about 72 hours but, by day 10, the area of haemorrhage will become hypodense (ie, look darker than normal tissue).
In ischaemic stroke, a demarcated zone of hypodensity appears, which reflects the arterial territory involved and, by determining both its location and its size, may guide further investigations and management, and predict outcome. However, in some cases, hypodensity may be difficult to detect due to the limited spatial resolution of CT and bony artefacts (causing distortion of the image). Over the first few hours, ischaemic stroke may produce only subtle abnormalities, reflecting early oedema. CT perfusion and angiography are more advanced techniques and are more likely to be used in the future.
Magnetic resonance imaging
Magnetic resonance imaging (MRI) is the brain imaging method of choice in stroke because it is more sensitive in detecting early ischaemia and it allows for differentiation between old and new ischaemia. However, MRI is more time-consuming than CT scanning and is therefore not appropriate for the initial assessment of patients who may be eligible for thrombolysis (see accompanying article, p205). MRI is preferred for the investigation of TIA.3
Carotid duplex ultrasonography
Stenosis of the carotid artery can cause stroke. It is often suspected when patients present with symptoms that indicate occlusion of the middle or anterior cerebral arteries. The most common way to diagnose carotid stenosis is using carotid duplex ultrasonography, which is a well-tolerated and non- invasive procedure. Magnetic resonance angiography and CT angiography can also be used in the screening and assessment of carotid stenosis.
Additional assessments
In addition to general assessments — which include blood pressure, electrocardiogram (ECG), urea and electrolytes, blood glucose, cholesterol, full blood count, erythrocyte sedimentation rate, thyroid function and inflammatory markers — specific investigations are required to define the type and cause of the stroke, informed by the patient’s age.
ECG abnormalities may suggest a cardiac origin for a thrombus. If brain imaging and the clinical presentation fit with embolic stroke, or if clinical findings suggest cardiac disease, cardiac imaging is indicated, as is a 24-hour Holter monitor (to detect arrhythmias, such as AF).
Urinalysis may reveal abnormalities in patients with diabetes, vasculitis or infective endocarditis. In young patients with stroke of no obvious cause, a drug screen (eg, for amphetamines, cocaine, ecstasy) should be considered.
The acute treatment of stroke is discussed in the accompanying article (p205).
References
1 Brown MM, Markus H, Oppenheimer S. Stroke Medicine (1st ed). United Kingdom: Taylor & Francis group; 2006.
2 National Institute for Health and Clinical Excellence. Clopidogrel and modified-release dipyridamole for the prevention of occlusive vascular events. December 2010. www.nice.org.uk/ta210 (accessed 3 May 2011).
3 National Institute for Health and Clinical Excellence. Diagnosis and initial management of acute stroke and transient ischaemic attack. July 2008. www.nice.org.uk/cg68 (accessed 3 May 2011).
4 Rudd A, Wolfe C. Aetiology and pathology of stroke. Hospital Pharmacist 2002;9:32–6.
5 Donnan G. What are the mechanisms of stroke? Dialogues in Cardiovascular Medicine 2003;8:15–21.
6 Putcala J, Metso AJ, Metso TM, et al. Analysis of 1008 Consecutive Patients aged 15–49 with first-ever ischaemic stroke: the Helsinki young stroke registry. Stroke 2009;40:1195–1203.
7 US Department of Health and Human Services. The seventh report of the Joint National Committee on prevention, detection, evaluation and treatment of high blood pressure. December 2003. www.nhlbi.nih.gov/guidelines/hypertension (accessed 3 May 2011).
8 Hand PJ, Kwan J, Lindley RI, et al. Distinguishing between stroke and mimic at the bedside: the Brain Attack Study. Stroke 2006;37:769–75.
9 Stroke Association. Suspect a stroke? Act FAST. www.stroke.org.uk/ campaigns/raising_awareness/act_fast.html (accessed 3 May 2011).
10 Nor AM, Davis J, Sen B, et al. The recognition of stroke in the emergency room (ROSIER) scale: development and validation of a stroke recognition instrument. Lancet Neurology 2005;4:727–34.